COVID-19 Group Testing Method Delivers Results 13 Times Faster than Individual Testing of Each Sample
|
By LabMedica International staff writers Posted on 30 Mar 2021 |
Illustration
A new group method of testing for COVID-19 allows results to be obtained 13 times faster as compared to individual testing of each sample.
The new method developed by researchers from the HSE Laboratory of Algorithms and Technologies for Networks Analysis (Nizhny Novgorod, Russia) and Vilnius University (Vilnius, Lithuania) can be used for asymptomatic populations with seemingly low incidence of coronavirus cases, where it will help detect the infected individuals at a maximum speed with a minimum number of tests, and timely apply the quarantine measures in order to prevent spreading of the disease.
Present COVID-19 testing solutions are based on the extraction of RNA from patients using oropharyngeal and nasopharyngeal swabs, and then testing with real-time PCR for the presence of specific RNA filaments identifying the virus. The speed of this approach is limited by the availability of reactants, trained technicians and laboratories. One way to speed up the testing procedures is group testing, where the swabs of multiple patients are grouped together and tested. The swabs from groups that return a positive result are then tested individually in order to detect specific COVID-19 positive patients. This approach helps decrease the number of tests twofold or more (depending on the spread of the disease) as compared to individual testing of each swab.
For example, suppose 96 samples should be tested and pools of up to 12 samples are possible. In individual testing, 96 tests are necessary. In pool testing, 8 pools of 12 samples are taken and testing is performed. If the result of one pool is positive, then additional 12 individual tests are needed. If two or three groups return a positive result, 24 or 36 additional tests are required, which, together with the first eight tests, will mean a decrease in the number of tests from two to five times as compared to individual testing. The researchers believe that the number of tests can be decreased by optimizing the size of groups that takes into account the total number of swabs and the forecasted number of infected individuals. As the number of infected individuals increases, the possibility of saving swabs decreases but is still about 40% in the event of an incidence of 100 positive samples per 1,000, and 18% for an incidence of 200 per 1,000.
There are ways to optimize group testing, such as choosing the optimal group size based on the total number of swabs and the projected level of disease spreading. Another is the binary splitting method, in which a positive group is split into halves and is tested again, until individual positive swabs are detected. The second method, however, is very time-consuming, which decreases its attractiveness during a pandemic. In addition, to optimize group testing, transposition-based replication is used: after grouping the swabs, researchers form additional control groups from the same swabs and test them together with the main groups. This helps further cut the number of tests, and if the disease levels are low, it also helps to detect positive swabs in one step, which speeds up the testing considerably.
However, this method does not allow for experimenting with group sizes to detect the optimal group size under specific conditions. Researchers from HSE University and Vilnius University suggested OptReplica technology, which uses a more complicated algorithm of swab grouping in key and control groups and helps decrease the number of control groups. In addition, the algorithm helps calculate the optimal group size for the present number of swabs and the forecasted level of disease spreading. The researchers conducted experimental research on samples of 96 and 384 swabs, carrying out 100 randomized tests for each sample size, and compared the effectiveness of transposition-based replication and OptReplica method for different levels of disease incidence. The studies have shown that if the optimal size of groups is chosen, OptReplica is more effective than transposition-based replication. In cases with low incidence, the use of OptReplica, a 13x average reduction of tests can be achieved compared to individual testing without time delay.
“Our simulations are actually proving that using this optimization replication strategy is always advantageous and, even in case of high spread of the disease (10% or 20% of positives in the population), we are still competitive with individual testing strategy,” explained Mario Guarracino, Chief Research Fellow of the Laboratory of Algorithms and Technologies for Networks Analysis.
Related Links:
HSE Laboratory of Algorithms and Technologies for Networks Analysis
Vilnius University
The new method developed by researchers from the HSE Laboratory of Algorithms and Technologies for Networks Analysis (Nizhny Novgorod, Russia) and Vilnius University (Vilnius, Lithuania) can be used for asymptomatic populations with seemingly low incidence of coronavirus cases, where it will help detect the infected individuals at a maximum speed with a minimum number of tests, and timely apply the quarantine measures in order to prevent spreading of the disease.
Present COVID-19 testing solutions are based on the extraction of RNA from patients using oropharyngeal and nasopharyngeal swabs, and then testing with real-time PCR for the presence of specific RNA filaments identifying the virus. The speed of this approach is limited by the availability of reactants, trained technicians and laboratories. One way to speed up the testing procedures is group testing, where the swabs of multiple patients are grouped together and tested. The swabs from groups that return a positive result are then tested individually in order to detect specific COVID-19 positive patients. This approach helps decrease the number of tests twofold or more (depending on the spread of the disease) as compared to individual testing of each swab.
For example, suppose 96 samples should be tested and pools of up to 12 samples are possible. In individual testing, 96 tests are necessary. In pool testing, 8 pools of 12 samples are taken and testing is performed. If the result of one pool is positive, then additional 12 individual tests are needed. If two or three groups return a positive result, 24 or 36 additional tests are required, which, together with the first eight tests, will mean a decrease in the number of tests from two to five times as compared to individual testing. The researchers believe that the number of tests can be decreased by optimizing the size of groups that takes into account the total number of swabs and the forecasted number of infected individuals. As the number of infected individuals increases, the possibility of saving swabs decreases but is still about 40% in the event of an incidence of 100 positive samples per 1,000, and 18% for an incidence of 200 per 1,000.
There are ways to optimize group testing, such as choosing the optimal group size based on the total number of swabs and the projected level of disease spreading. Another is the binary splitting method, in which a positive group is split into halves and is tested again, until individual positive swabs are detected. The second method, however, is very time-consuming, which decreases its attractiveness during a pandemic. In addition, to optimize group testing, transposition-based replication is used: after grouping the swabs, researchers form additional control groups from the same swabs and test them together with the main groups. This helps further cut the number of tests, and if the disease levels are low, it also helps to detect positive swabs in one step, which speeds up the testing considerably.
However, this method does not allow for experimenting with group sizes to detect the optimal group size under specific conditions. Researchers from HSE University and Vilnius University suggested OptReplica technology, which uses a more complicated algorithm of swab grouping in key and control groups and helps decrease the number of control groups. In addition, the algorithm helps calculate the optimal group size for the present number of swabs and the forecasted level of disease spreading. The researchers conducted experimental research on samples of 96 and 384 swabs, carrying out 100 randomized tests for each sample size, and compared the effectiveness of transposition-based replication and OptReplica method for different levels of disease incidence. The studies have shown that if the optimal size of groups is chosen, OptReplica is more effective than transposition-based replication. In cases with low incidence, the use of OptReplica, a 13x average reduction of tests can be achieved compared to individual testing without time delay.
“Our simulations are actually proving that using this optimization replication strategy is always advantageous and, even in case of high spread of the disease (10% or 20% of positives in the population), we are still competitive with individual testing strategy,” explained Mario Guarracino, Chief Research Fellow of the Laboratory of Algorithms and Technologies for Networks Analysis.
Related Links:
HSE Laboratory of Algorithms and Technologies for Networks Analysis
Vilnius University
Latest COVID-19 News
- New Immunosensor Paves Way to Rapid POC Testing for COVID-19 and Emerging Infectious Diseases
- Long COVID Etiologies Found in Acute Infection Blood Samples
- Novel Device Detects COVID-19 Antibodies in Five Minutes
- CRISPR-Powered COVID-19 Test Detects SARS-CoV-2 in 30 Minutes Using Gene Scissors
- Gut Microbiome Dysbiosis Linked to COVID-19
- Novel SARS CoV-2 Rapid Antigen Test Validated for Diagnostic Accuracy
- New COVID + Flu + R.S.V. Test to Help Prepare for `Tripledemic`
- AI Takes Guesswork Out Of Lateral Flow Testing
- Fastest Ever SARS-CoV-2 Antigen Test Designed for Non-Invasive COVID-19 Testing in Any Setting
- Rapid Antigen Tests Detect Omicron, Delta SARS-CoV-2 Variants
- Health Care Professionals Showed Increased Interest in POC Technologies During Pandemic, Finds Study
- Set Up Reserve Lab Capacity Now for Faster Response to Next Pandemic, Say Researchers
- Blood Test Performed During Initial Infection Predicts Long COVID Risk
- Low-Cost COVID-19 Testing Platform Combines Sensitivity of PCR and Speed of Antigen Tests
- Finger-Prick Blood Test Identifies Immunity to COVID-19
- Quick Test Kit Determines Immunity Against COVID-19 and Its Variants
Channels
Clinical Chemistry
view channel
Urine-Based Nanosensor Tracks Lung Cancer and Fibrosis Noninvasively
Lung cancer remains difficult to monitor for early progression and treatment resistance, while pulmonary fibrosis continues to pose major challenges for early diagnosis. Clinicians need repeatable, noninvasive... Read more
Blood-Based Alzheimer’s Test Gains CE Mark for Amyloid Pathology Detection
Alzheimer’s disease is the most common cause of dementia, yet confirmatory testing remains invasive and hard to access. Diagnosis currently takes an average of 3.5 years, and about 75% of people with dementia... Read moreMolecular Diagnostics
view channel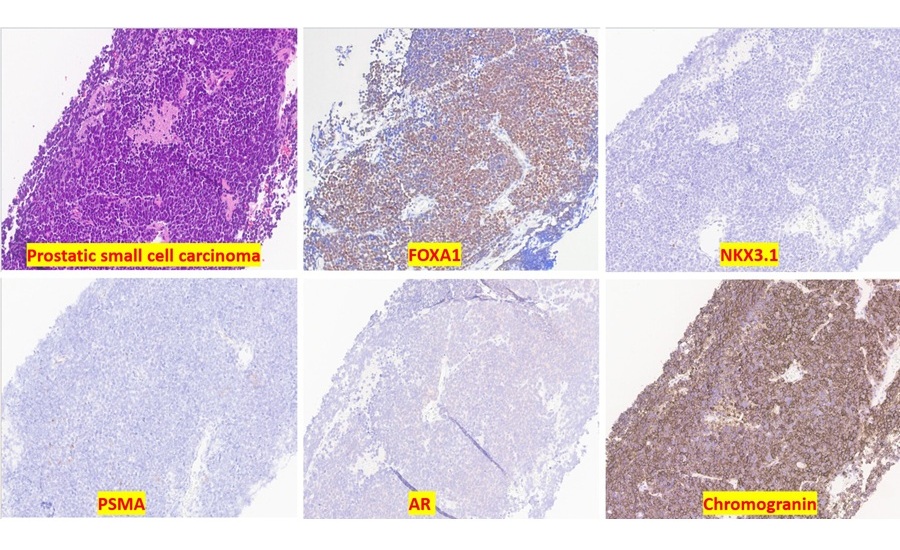
Sensitive Protein Marker Aids Diagnosis of Small Cell Prostate Cancer
Accurate identification of aggressive prostate cancer subtypes can be difficult when tumors lose expression of lineage markers used in routine pathology. Small cell carcinoma of the prostate, in particular,... Read more
Rapid Multiplex PCR Test Detects 11 Gastrointestinal Pathogens from Single Sample
Cepheid’s Xpert GI Panel has received CE marking under the In Vitro Diagnostic Medical Devices Regulation (IVDR) and is expected to begin shipping to countries that accept the CE mark in the coming weeks.... Read moreHematology
view channel
Stem Cell Biomarkers May Guide Precision Treatment in Acute Myeloid Leukemia
Acute myeloid leukemia (AML) is an aggressive blood cancer that most often affects older adults and still carries a poor prognosis despite therapeutic advances. Venetoclax-based regimens have improved... Read more
Advanced CBC-Derived Indices Integrated into Hematology Platforms
Diatron, a STRATEC brand, has introduced six advanced hematological indices on its Aquila, Aquarius 3, and Abacus 5 hematology analyzers. The new Research Use Only (RUO) indices include Neutrophil-to-Lymphocyte... Read moreImmunology
view channel
Routine TB Screening Test May Reveal Immune Aging and Mortality Risk
Immune aging is associated with weaker responses to vaccination, greater risks of infection, and higher levels of inflammation. Leveraging routinely ordered laboratory tests to quantify that responsiveness... Read more
Biomarkers and Molecular Testing Advance Precision Allergy Care
Allergic diseases often present with similar symptoms but can be driven by distinct biological mechanisms, making standardized care inefficient for many patients. Historically, individuals with pollen... Read moreMicrobiology
view channel
Study Finds Hidden Mpox Infections May Drive Ongoing Spread
Mpox continues to circulate despite vaccination, and many cases show no known link to a symptomatic partner. The role of people without symptoms has remained uncertain, limiting clarity on how transmission persists.... Read more
Large-Scale Genomic Surveillance Tracks Resistant Bacteria Across European Hospitals
Antimicrobial resistance (AMR) poses a growing threat to patient safety, with carbapenem-resistant Enterobacterales causing difficult-to-treat infections and leaving clinicians with limited therapeutic options.... Read more
Molecular Urine and Stool Tests Do Not Improve Early TB Treatment in Hospitalized HIV Patients
Tuberculosis is the leading cause of death among people living with HIV, and diagnosis in hospital settings remains difficult. Symptoms are often non-specific, disease can be extrapulmonary, and many patients... Read morePathology
view channel
FDA Clears AI Digital Pathology Tool for Breast Cancer Risk Stratification
Risk assessment at diagnosis is central to guiding therapy for early-stage, hormone receptor-positive, human epidermal growth factor receptor 2-negative (HR+/HER2-) invasive breast cancer, where overtreatment... Read more
New AI Tool Reveals Hidden Genetic Signals in Routine H&E Slides
Pathologists worldwide rely on hematoxylin and eosin (H&E) slides to examine tissue architecture, yet these stains do not reveal the underlying molecular activity that often drives disease.... Read moreTechnology
view channel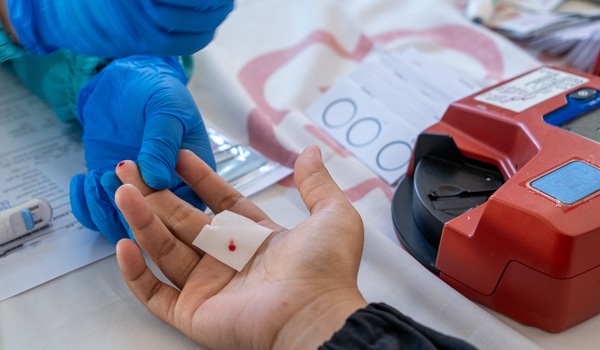
Point-of-Care Testing Enhances Health Literacy and Self-Management in Chronic Disease
Limited access to general practitioners and pathology services can delay diagnosis and monitoring for people in regional and remote communities. Rapid, on-the-spot testing can shorten turnaround times... Read more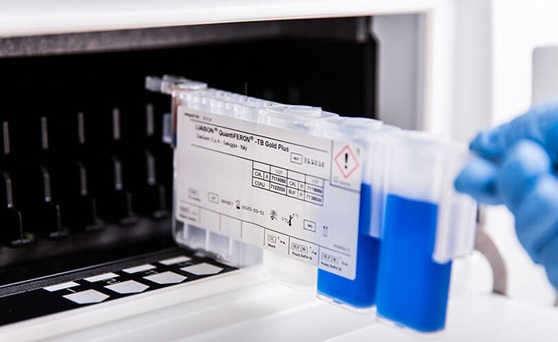
Fully Automated Sample-to-Insight Workflow Advances Latent TB Testing
Latent tuberculosis remains a substantial testing workload for clinical laboratories as screening programs expand. Despite this growth, only about 40% of testing has shifted from traditional skin tests... Read moreIndustry
view channel
AI-Powered Multi-Functional Analyzer Wins German Innovation Award
Hematology services are increasingly delivered across distributed care settings, where limited staffing and complex workflows can extend turnaround times. Advanced morphology review still often depends... Read more