Next Generation Sequencing Testing Protocol for SARS-CoV-2 Can Process Tens of Thousands of Samples in Less Than 48 Hours
|
By LabMedica International staff writers Posted on 26 May 2021 |

Image: Next Generation Sequencing Testing Protocol for SARS-CoV-2 Can Process Tens of Thousands of Samples in Less Than 48 Hours (Photo courtesy of Peter Duchek)
A new testing protocol for SARS-CoV-2 can process tens of thousands of samples in less than 48 hours and could also be adapted to many more pathogens.
The method, called SARSeq, has been developed by researchers at the Vienna BioCenter (Vienna, Austria) by combining their expertise in genomics, RNA biochemistry and data analysis.
Molecular tests that detect the presence of SARS-CoV-2 have become the best way to isolate positive cases and contain the spread of the virus. Several methods have come forward, some that detect viral proteins from nasopharyngeal swabs (such as antigen tests), and some that detect the presence of viral RNA from swabs, gargle samples, or saliva samples (such as reverse transcription and polymerase chain reaction tests, or RT-PCR).
Although antigen tests facilitate some logistical aspects of mass testing, their detection power is relatively weak – infected individuals carrying low amounts of virus remain undetected and can continue to infect other people. PCR tests, on the other hand, are more sensitive because they multiply fragments of the viral genome before scanning samples for the virus. However, they rely on the detection of fluorescent labels that tag viral sequences, which means that pooling samples coming from different people makes the process rather inefficient: if a pool tests positive, all the samples within the pool must be tested again individually to identify the source of the fluorescent signal. Too many machines needed, too expensive, too slow.
The new method developed by scientists at the Vienna BioCenter could enable large groups to be tested for SARS-CoV-2 with the same sensitivity as regular PCR tests. SARSeq, or ‘Saliva Analysis by RNA sequencing’, achieves high sensitivity, specificity, and the power to process up to 36,000 samples in less than 48 hours. The testing principle is conceptually simple: individual patient samples are collected into the wells of a testing plate - one well for each sample. Then, a fragment of viral RNA unique to SARS-CoV-2 - the nucleocapsid gene - is selectively converted to DNA and PCR-amplified in any well that contains it.
What distinguishes this first step to the usual PCR test is that each sample receives a unique set of short DNA sequences – or barcodes – that attach to the amplifying viral DNA. In a second amplification step, all the samples from one plate are pooled into one well, which receives a second set of unique DNA barcodes. The contents of multiple plates can be pooled once more, as the DNA molecules from each sample carry a unique combination of two sets of barcodes. This pooling and barcoding strategy makes SARSeq highly specific and scalable. Moreover, the NGS-based method allows to test several RNAs in parallel, including RNAs that control the sample quality or RNAs from other pathogens for differential diagnostics.
The testing procedure can run in parallel to existing diagnostics, while being independent of the bottlenecks in supply chains. Therefore, it does not compete with other testing methods for reagents or equipment. The principles behind SARSeq are simple and adaptable to any respiratory pathogen. As the world’s population skyrockets along with our proximity to animals, cutting-edge diagnostic methods like SARSeq will be crucial to prevent future diseases from spreading like wildfire.
“Amplifying the viral material from individual samples to a maximum homogenizes its quantity across positive samples, making SARSeq highly sensitive,” explained Luisa Cochella, group leader at the Research Institute of Molecular Pathology (IMP). “Within the thousands of samples that we could test simultaneously, some may contain up to 10 million times more coronavirus particles than others – if we pooled such samples before amplification, those with high amounts of viral material could mask other positive cases.”
“We combine the sensitivity of PCR with the high throughput of Next Generation Sequencing technology, or NGS, the same used to sequence the human genome. The NGS machine processes the pooled samples and tells us which samples contained any SARS-CoV-2 material. The barcodes allow us to distinguish each positive sample from the others, and trace it back to a patient,” added Ramesh Yelagandula, first author of the study.
Related Links:
Vienna BioCenter
The method, called SARSeq, has been developed by researchers at the Vienna BioCenter (Vienna, Austria) by combining their expertise in genomics, RNA biochemistry and data analysis.
Molecular tests that detect the presence of SARS-CoV-2 have become the best way to isolate positive cases and contain the spread of the virus. Several methods have come forward, some that detect viral proteins from nasopharyngeal swabs (such as antigen tests), and some that detect the presence of viral RNA from swabs, gargle samples, or saliva samples (such as reverse transcription and polymerase chain reaction tests, or RT-PCR).
Although antigen tests facilitate some logistical aspects of mass testing, their detection power is relatively weak – infected individuals carrying low amounts of virus remain undetected and can continue to infect other people. PCR tests, on the other hand, are more sensitive because they multiply fragments of the viral genome before scanning samples for the virus. However, they rely on the detection of fluorescent labels that tag viral sequences, which means that pooling samples coming from different people makes the process rather inefficient: if a pool tests positive, all the samples within the pool must be tested again individually to identify the source of the fluorescent signal. Too many machines needed, too expensive, too slow.
The new method developed by scientists at the Vienna BioCenter could enable large groups to be tested for SARS-CoV-2 with the same sensitivity as regular PCR tests. SARSeq, or ‘Saliva Analysis by RNA sequencing’, achieves high sensitivity, specificity, and the power to process up to 36,000 samples in less than 48 hours. The testing principle is conceptually simple: individual patient samples are collected into the wells of a testing plate - one well for each sample. Then, a fragment of viral RNA unique to SARS-CoV-2 - the nucleocapsid gene - is selectively converted to DNA and PCR-amplified in any well that contains it.
What distinguishes this first step to the usual PCR test is that each sample receives a unique set of short DNA sequences – or barcodes – that attach to the amplifying viral DNA. In a second amplification step, all the samples from one plate are pooled into one well, which receives a second set of unique DNA barcodes. The contents of multiple plates can be pooled once more, as the DNA molecules from each sample carry a unique combination of two sets of barcodes. This pooling and barcoding strategy makes SARSeq highly specific and scalable. Moreover, the NGS-based method allows to test several RNAs in parallel, including RNAs that control the sample quality or RNAs from other pathogens for differential diagnostics.
The testing procedure can run in parallel to existing diagnostics, while being independent of the bottlenecks in supply chains. Therefore, it does not compete with other testing methods for reagents or equipment. The principles behind SARSeq are simple and adaptable to any respiratory pathogen. As the world’s population skyrockets along with our proximity to animals, cutting-edge diagnostic methods like SARSeq will be crucial to prevent future diseases from spreading like wildfire.
“Amplifying the viral material from individual samples to a maximum homogenizes its quantity across positive samples, making SARSeq highly sensitive,” explained Luisa Cochella, group leader at the Research Institute of Molecular Pathology (IMP). “Within the thousands of samples that we could test simultaneously, some may contain up to 10 million times more coronavirus particles than others – if we pooled such samples before amplification, those with high amounts of viral material could mask other positive cases.”
“We combine the sensitivity of PCR with the high throughput of Next Generation Sequencing technology, or NGS, the same used to sequence the human genome. The NGS machine processes the pooled samples and tells us which samples contained any SARS-CoV-2 material. The barcodes allow us to distinguish each positive sample from the others, and trace it back to a patient,” added Ramesh Yelagandula, first author of the study.
Related Links:
Vienna BioCenter
Latest COVID-19 News
- New Immunosensor Paves Way to Rapid POC Testing for COVID-19 and Emerging Infectious Diseases
- Long COVID Etiologies Found in Acute Infection Blood Samples
- Novel Device Detects COVID-19 Antibodies in Five Minutes
- CRISPR-Powered COVID-19 Test Detects SARS-CoV-2 in 30 Minutes Using Gene Scissors
- Gut Microbiome Dysbiosis Linked to COVID-19
- Novel SARS CoV-2 Rapid Antigen Test Validated for Diagnostic Accuracy
- New COVID + Flu + R.S.V. Test to Help Prepare for `Tripledemic`
- AI Takes Guesswork Out Of Lateral Flow Testing
- Fastest Ever SARS-CoV-2 Antigen Test Designed for Non-Invasive COVID-19 Testing in Any Setting
- Rapid Antigen Tests Detect Omicron, Delta SARS-CoV-2 Variants
- Health Care Professionals Showed Increased Interest in POC Technologies During Pandemic, Finds Study
- Set Up Reserve Lab Capacity Now for Faster Response to Next Pandemic, Say Researchers
- Blood Test Performed During Initial Infection Predicts Long COVID Risk
- Low-Cost COVID-19 Testing Platform Combines Sensitivity of PCR and Speed of Antigen Tests
- Finger-Prick Blood Test Identifies Immunity to COVID-19
- Quick Test Kit Determines Immunity Against COVID-19 and Its Variants
Channels
Clinical Chemistry
view channel
New PSA-Based Prognostic Model Improves Prostate Cancer Risk Assessment
Prostate cancer is the second-leading cause of cancer death among American men, and about one in eight will be diagnosed in their lifetime. Screening relies on blood levels of prostate-specific antigen... Read more
Extracellular Vesicles Linked to Heart Failure Risk in CKD Patients
Chronic kidney disease (CKD) affects more than 1 in 7 Americans and is strongly associated with cardiovascular complications, which account for more than half of deaths among people with CKD.... Read moreMolecular Diagnostics
view channel
Diagnostic Device Predicts Treatment Response for Brain Tumors Via Blood Test
Glioblastoma is one of the deadliest forms of brain cancer, largely because doctors have no reliable way to determine whether treatments are working in real time. Assessing therapeutic response currently... Read more
Blood Test Detects Early-Stage Cancers by Measuring Epigenetic Instability
Early-stage cancers are notoriously difficult to detect because molecular changes are subtle and often missed by existing screening tools. Many liquid biopsies rely on measuring absolute DNA methylation... Read more
“Lab-On-A-Disc” Device Paves Way for More Automated Liquid Biopsies
Extracellular vesicles (EVs) are tiny particles released by cells into the bloodstream that carry molecular information about a cell’s condition, including whether it is cancerous. However, EVs are highly... Read more
Blood Test Identifies Inflammatory Breast Cancer Patients at Increased Risk of Brain Metastasis
Brain metastasis is a frequent and devastating complication in patients with inflammatory breast cancer, an aggressive subtype with limited treatment options. Despite its high incidence, the biological... Read moreHematology
view channel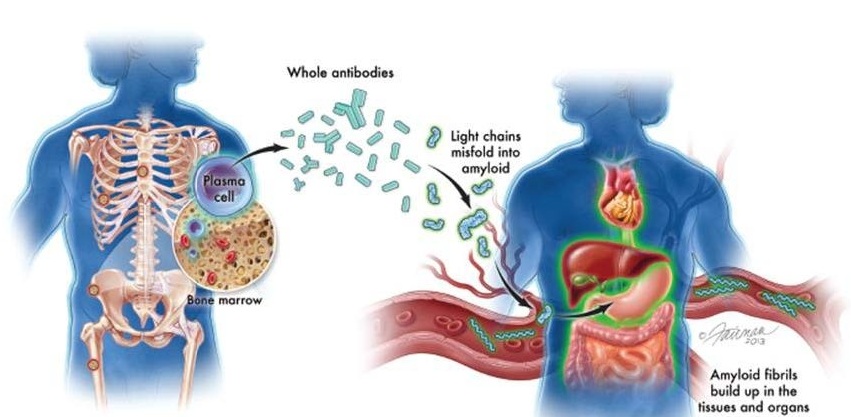
New Guidelines Aim to Improve AL Amyloidosis Diagnosis
Light chain (AL) amyloidosis is a rare, life-threatening bone marrow disorder in which abnormal amyloid proteins accumulate in organs. Approximately 3,260 people in the United States are diagnosed... Read more
Fast and Easy Test Could Revolutionize Blood Transfusions
Blood transfusions are a cornerstone of modern medicine, yet red blood cells can deteriorate quietly while sitting in cold storage for weeks. Although blood units have a fixed expiration date, cells from... Read more
Automated Hemostasis System Helps Labs of All Sizes Optimize Workflow
High-volume hemostasis sections must sustain rapid turnaround while managing reruns and reflex testing. Manual tube handling and preanalytical checks can strain staff time and increase opportunities for error.... Read more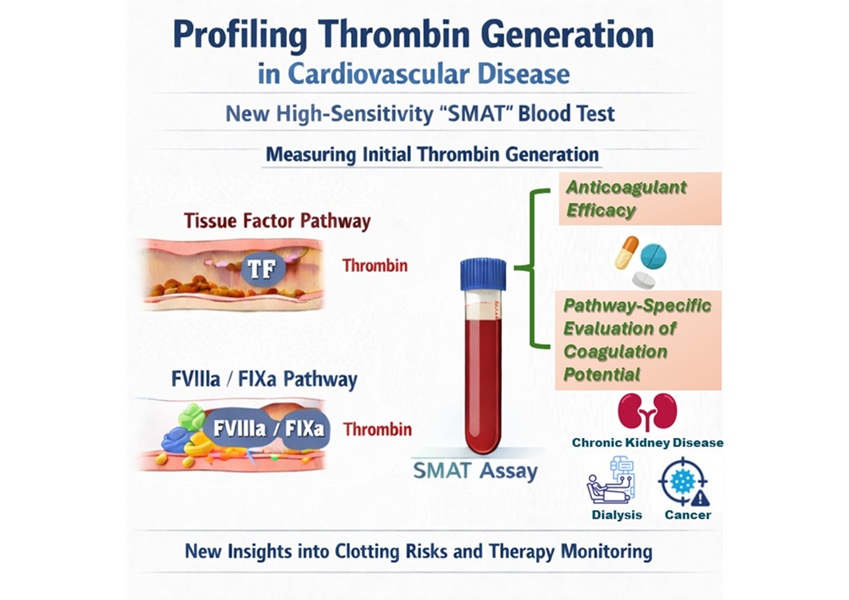
High-Sensitivity Blood Test Improves Assessment of Clotting Risk in Heart Disease Patients
Blood clotting is essential for preventing bleeding, but even small imbalances can lead to serious conditions such as thrombosis or dangerous hemorrhage. In cardiovascular disease, clinicians often struggle... Read moreImmunology
view channelBlood Test Identifies Lung Cancer Patients Who Can Benefit from Immunotherapy Drug
Small cell lung cancer (SCLC) is an aggressive disease with limited treatment options, and even newly approved immunotherapies do not benefit all patients. While immunotherapy can extend survival for some,... Read more
Whole-Genome Sequencing Approach Identifies Cancer Patients Benefitting From PARP-Inhibitor Treatment
Targeted cancer therapies such as PARP inhibitors can be highly effective, but only for patients whose tumors carry specific DNA repair defects. Identifying these patients accurately remains challenging,... Read more
Ultrasensitive Liquid Biopsy Demonstrates Efficacy in Predicting Immunotherapy Response
Immunotherapy has transformed cancer treatment, but only a small proportion of patients experience lasting benefit, with response rates often remaining between 10% and 20%. Clinicians currently lack reliable... Read moreMicrobiology
view channel
Comprehensive Review Identifies Gut Microbiome Signatures Associated With Alzheimer’s Disease
Alzheimer’s disease affects approximately 6.7 million people in the United States and nearly 50 million worldwide, yet early cognitive decline remains difficult to characterize. Increasing evidence suggests... Read moreAI-Powered Platform Enables Rapid Detection of Drug-Resistant C. Auris Pathogens
Infections caused by the pathogenic yeast Candida auris pose a significant threat to hospitalized patients, particularly those with weakened immune systems or those who have invasive medical devices.... Read morePathology
view channel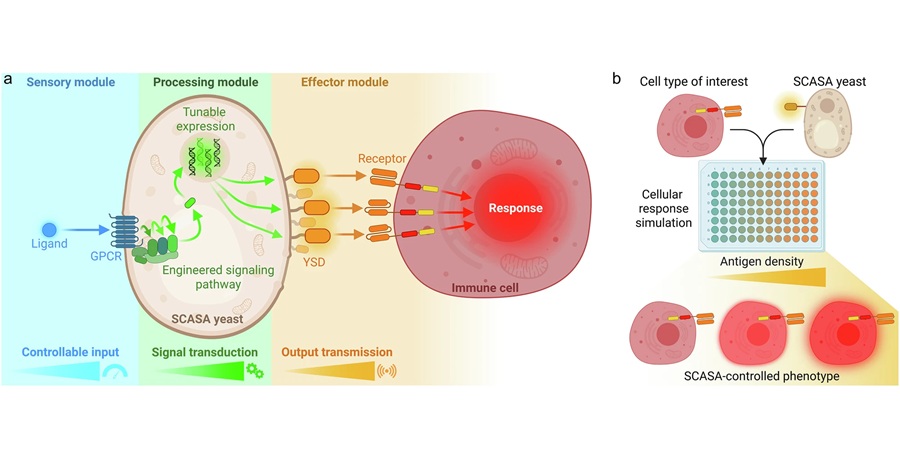
Engineered Yeast Cells Enable Rapid Testing of Cancer Immunotherapy
Developing new cancer immunotherapies is a slow, costly, and high-risk process, particularly for CAR T cell treatments that must precisely recognize cancer-specific antigens. Small differences in tumor... Read more
First-Of-Its-Kind Test Identifies Autism Risk at Birth
Autism spectrum disorder is treatable, and extensive research shows that early intervention can significantly improve cognitive, social, and behavioral outcomes. Yet in the United States, the average age... Read moreTechnology
view channel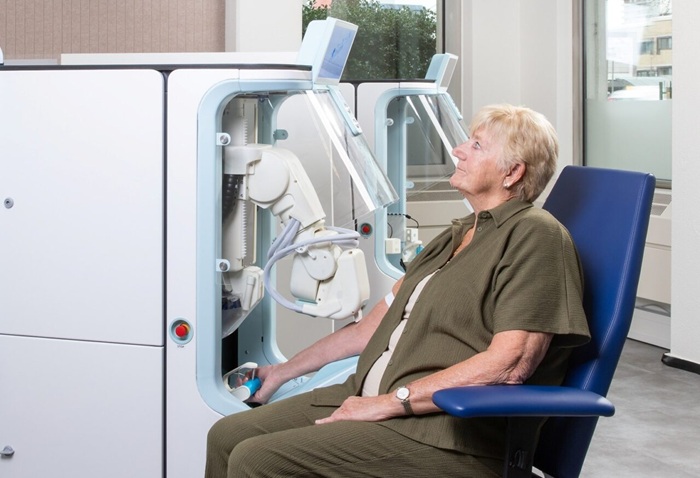
Robotic Technology Unveiled for Automated Diagnostic Blood Draws
Routine diagnostic blood collection is a high‑volume task that can strain staffing and introduce human‑dependent variability, with downstream implications for sample quality and patient experience.... Read more
ADLM Launches First-of-Its-Kind Data Science Program for Laboratory Medicine Professionals
Clinical laboratories generate billions of test results each year, creating a treasure trove of data with the potential to support more personalized testing, improve operational efficiency, and enhance patient care.... Read moreAptamer Biosensor Technology to Transform Virus Detection
Rapid and reliable virus detection is essential for controlling outbreaks, from seasonal influenza to global pandemics such as COVID-19. Conventional diagnostic methods, including cell culture, antigen... Read more
AI Models Could Predict Pre-Eclampsia and Anemia Earlier Using Routine Blood Tests
Pre-eclampsia and anemia are major contributors to maternal and child mortality worldwide, together accounting for more than half a million deaths each year and leaving millions with long-term health complications.... Read moreIndustry
view channelNew Collaboration Brings Automated Mass Spectrometry to Routine Laboratory Testing
Mass spectrometry is a powerful analytical technique that identifies and quantifies molecules based on their mass and electrical charge. Its high selectivity, sensitivity, and accuracy make it indispensable... Read more
AI-Powered Cervical Cancer Test Set for Major Rollout in Latin America
Noul Co., a Korean company specializing in AI-based blood and cancer diagnostics, announced it will supply its intelligence (AI)-based miLab CER cervical cancer diagnostic solution to Mexico under a multi‑year... Read more
Diasorin and Fisher Scientific Enter into US Distribution Agreement for Molecular POC Platform
Diasorin (Saluggia, Italy) has entered into an exclusive distribution agreement with Fisher Scientific, part of Thermo Fisher Scientific (Waltham, MA, USA), for the LIAISON NES molecular point-of-care... Read more