Breakthrough Drug May Help to Reverse Spinal Damage
|
By LabMedica International staff writers Posted on 15 Dec 2014 |
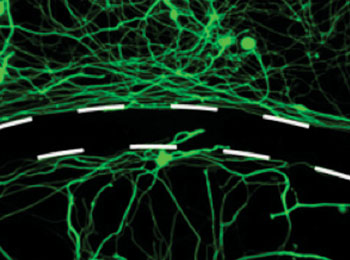
Image: Scientists have created a drug that helps nerve fibers cross scar tissue barriers after spinal cord injury (Photo courtesy of the NIH).
Injections of a new drug may partially relieve paralyzing spinal cord injuries, based on new findings from experiments performed in lab rats.
The new study, which was partly funded by the US National Institutes of Health (NIH; Bethesda, MD, USA), demonstrated how basic laboratory research can lead to new therapy options. “We’re very excited at the possibility that millions of people could, one day, regain movements lost during spinal cord injuries,” said Jerry Silver, PhD, professor of neurosciences, Case Western Reserve University School of Medicine (Cleveland, OH, USA), and a senior investigator of the study published December 3, 2014, in the journal Nature.
Every year, tens of thousands of people are paralyzed by spinal cord injuries. The injuries press and sever the long axons of spinal cord nerve cells, blocking communication between the brain and the body and resulting in paralysis below the injury. Using intuition, Bradley Lang, PhD, the lead author of the study and a graduate student in Dr. Silver’s lab, came up with the strategy of designing a drug that would help axons regenerate without having to touch the healing spinal cord, as current treatments may require. “Originally this was just a side project we brainstormed in the lab,” said Dr. Lang.
After spinal cord injury, axons try to cross the injury site and reconnect with other cells but are stymied by scarring that forms after the injury. Earlier research suggested their movements are blocked when the protein tyrosine phosphatase sigma (PTP sigma), an enzyme found in axons, interacts with chondroitin sulfate proteoglycans, a family of sugary proteins that fill the scars.
Dr. Lang and his colleagues designed a drug called intracellular sigma peptide (ISP) to block the enzyme and facilitate the drug’s entry into the brain and spinal cord. Injections of the drug under the skin of paralyzed rats close to the damaged site partially restored axon growth and improved movements and bladder functions. “There are currently no drug therapies available that improve the very limited natural recovery from spinal cord injuries that patients experience,” said Lyn Jakeman, PhD, a program director at the NIH’s National Institute of Neurological Disorders and Stroke (Bethesda, MD, USA). “This is a great step towards identifying a novel agent for helping people recover.”
At first, the objective of the research was to determine precisely how interactions between PTP sigma and chondroitin sulfate proteoglycans prevent axon growth. Drugs were designed to mimic the shape of a key part of PTP sigma, called the wedge. Different designs were evaluated on neurons grown in petri dishes alongside impenetrable barriers of proteoglycans. Treatment with ISP freed axon growth. “It was amazing. The axons kept growing and growing,” said Dr. Silver.
The scientists next tested the potential of the drug on a rat model of spinal cord injury. For seven weeks they injected rats with the drug or a placebo near the site of injury. A few weeks later the rats that received the drug showed improvements in walking and urinating while the placebo treatments had no effect. The findings suggested the drug passed into the brain and spinal cord.
When the researchers looked at the spinal cords under a microscope they found that the drug triggered sprouting of axons that use the neurochemical serotonin to communicate. The sprouting axons were seen below the injury site. Treating some of the lab rats with a blocker of serotonin communication partially reversed the advantageous effects of ISP injections, suggesting the newly growing axons helped the rats recover.
The ISP drug did not cause spinal cord axons known to control movements to cross the scar and reconnect with brain neurons above the injury site. Dr. Silver and his colleagues think this means the ISP-induced sprouting helped the rats recover by increasing the signal sent by the few remaining intact axons. “This is very promising. We now have an agent that may work alone or in combination with other treatments to improve the lives of many,” concluded Dr. Silver. He and his colleagues are looking to evaluate the ISP drug in preclinical trials.
Related Links:
Case Western Reserve University School of Medicine
National Institute of Neurological Disorders and Stroke
The new study, which was partly funded by the US National Institutes of Health (NIH; Bethesda, MD, USA), demonstrated how basic laboratory research can lead to new therapy options. “We’re very excited at the possibility that millions of people could, one day, regain movements lost during spinal cord injuries,” said Jerry Silver, PhD, professor of neurosciences, Case Western Reserve University School of Medicine (Cleveland, OH, USA), and a senior investigator of the study published December 3, 2014, in the journal Nature.
Every year, tens of thousands of people are paralyzed by spinal cord injuries. The injuries press and sever the long axons of spinal cord nerve cells, blocking communication between the brain and the body and resulting in paralysis below the injury. Using intuition, Bradley Lang, PhD, the lead author of the study and a graduate student in Dr. Silver’s lab, came up with the strategy of designing a drug that would help axons regenerate without having to touch the healing spinal cord, as current treatments may require. “Originally this was just a side project we brainstormed in the lab,” said Dr. Lang.
After spinal cord injury, axons try to cross the injury site and reconnect with other cells but are stymied by scarring that forms after the injury. Earlier research suggested their movements are blocked when the protein tyrosine phosphatase sigma (PTP sigma), an enzyme found in axons, interacts with chondroitin sulfate proteoglycans, a family of sugary proteins that fill the scars.
Dr. Lang and his colleagues designed a drug called intracellular sigma peptide (ISP) to block the enzyme and facilitate the drug’s entry into the brain and spinal cord. Injections of the drug under the skin of paralyzed rats close to the damaged site partially restored axon growth and improved movements and bladder functions. “There are currently no drug therapies available that improve the very limited natural recovery from spinal cord injuries that patients experience,” said Lyn Jakeman, PhD, a program director at the NIH’s National Institute of Neurological Disorders and Stroke (Bethesda, MD, USA). “This is a great step towards identifying a novel agent for helping people recover.”
At first, the objective of the research was to determine precisely how interactions between PTP sigma and chondroitin sulfate proteoglycans prevent axon growth. Drugs were designed to mimic the shape of a key part of PTP sigma, called the wedge. Different designs were evaluated on neurons grown in petri dishes alongside impenetrable barriers of proteoglycans. Treatment with ISP freed axon growth. “It was amazing. The axons kept growing and growing,” said Dr. Silver.
The scientists next tested the potential of the drug on a rat model of spinal cord injury. For seven weeks they injected rats with the drug or a placebo near the site of injury. A few weeks later the rats that received the drug showed improvements in walking and urinating while the placebo treatments had no effect. The findings suggested the drug passed into the brain and spinal cord.
When the researchers looked at the spinal cords under a microscope they found that the drug triggered sprouting of axons that use the neurochemical serotonin to communicate. The sprouting axons were seen below the injury site. Treating some of the lab rats with a blocker of serotonin communication partially reversed the advantageous effects of ISP injections, suggesting the newly growing axons helped the rats recover.
The ISP drug did not cause spinal cord axons known to control movements to cross the scar and reconnect with brain neurons above the injury site. Dr. Silver and his colleagues think this means the ISP-induced sprouting helped the rats recover by increasing the signal sent by the few remaining intact axons. “This is very promising. We now have an agent that may work alone or in combination with other treatments to improve the lives of many,” concluded Dr. Silver. He and his colleagues are looking to evaluate the ISP drug in preclinical trials.
Related Links:
Case Western Reserve University School of Medicine
National Institute of Neurological Disorders and Stroke
Latest BioResearch News
- Lung Cancer Study Reveals Cellular Program Behind Therapy Resistance
- Tumor Genome Marker May Predict Treatment Benefit in Pediatric Cancers
- Lysosomal Gene Defect Linked to Severe Childhood Brain Disorders
- Genetic Testing Identifies Greater Inherited Sudden Cardiac Arrest Risk in Younger Individuals
- Hidden 'Jumping Gene' Variant Linked to Higher Pancreatic Cancer Risk
- Common White Blood Cells Produce Schizophrenia-Linked Protein
- Nanopore Method Captures RNA Folding at Single-Molecule Resolution
- Tumor Microenvironment Marker Linked to Worse Survival in Solid Tumors
- Hidden Immune Gene Defect May Explain Kaposi Sarcoma Susceptibility
- Genetic Markers May Help Predict Amputation Risk in Peripheral Artery Disease
- Gene Signature Shows Promise for Depression Biomarker Testing
- AI-Driven Tumor Profiling Initiative Targets Precision Therapy Development
- Researchers Map Protein and Glycosylation Across 15 Human Body Fluids
- Telomere Length Abnormalities Linked to Lymphoma Development
- Biomarker Signals Chemotherapy Resistance in Relapsed Small Cell Lung Cancer
- Inflammatory Gene Signature Links Metabolic Disease to Pancreatic Cancer Recurrence
Channels
Clinical Chemistry
view channel
Urine-Based Test Shows Promise for Autism Screening in Children
Autism spectrum disorder (ASD) is commonly diagnosed through behavioral assessments, which can involve long waits that delay intervention. Earlier identification is linked to better developmental outcomes,... Read more
Liquid Biopsy Biomarkers May Improve Childhood Epilepsy Diagnosis
Childhood epilepsy remains a major neurological disorder with unmet needs for accurate, non-invasive biomarkers, as conventional tests such as electroencephalography and neuroimaging can have limited sensitivity... Read moreMolecular Diagnostics
view channel
Updated Guidance Prioritizes Stool-Based Colorectal Cancer Screening Tests
Colorectal cancer is the second-leading cause of cancer death in the United States and claimed an estimated 55,000 lives in 2026. Incidence is rising among adults younger than 50, even as overall mortality... Read more
Digital PCR Assays Support Surveillance of Bundibugyo Ebolavirus Outbreak
QIAGEN (Venlo, Netherlands) has introduced two custom-designed research-use-only (RUO) QIAcuity dPCR assays to support infectious disease research and surveillance connected to the Bundibugyo ebolavirus outbreak.... Read more
Blood-Based Proteomic Test May Predict Treatment Response in Non-Small Cell Lung Cancer
Lung cancer remains the leading cause of cancer death, with non-small cell lung cancer (NSCLC) accounting for most cases. Treatment decisions are often made without a clear indication of how a patient... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channel
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read more
Immune Enzyme Linked to Treatment-Resistant Inflammatory Bowel Disease
Inflammatory bowel disease (IBD) affects nearly 3 million people in the United States and its prevalence continues to rise. Medications that target tumor necrosis factor (TNF)-alpha are widely used, but... Read moreMicrobiology
view channel
Gut Microbiome Signatures Help Identify Risk of IBD Progression
Inflammatory bowel disease (IBD), encompassing Crohn’s disease and ulcerative colitis, is a chronic relapsing inflammatory disorder of the gastrointestinal tract with highly variable outcomes.... Read more
FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
Clinical guidelines support testing based on patient presentation in suspected gastrointestinal infections, yet available technologies have often forced laboratories to choose between panels that are too... Read morePathology
view channel
AI-Powered Atlas Maps Immune Structures Linked to Cancer Outcomes
Tertiary lymphoid structures are emerging as important indicators of antitumor immunity, but their heterogeneity and spatial context within tumors remain difficult to capture through routine diagnostics.... Read more
AI Tool Extracts Immune Signals from Biopsy to Inform Myeloma Therapy
Multiple myeloma is a bone marrow malignancy in which patients can respond very differently to the same treatments, making initial therapy decisions difficult. Clinicians must choose among options such... Read moreTechnology
view channel
Mailed Screening Kits Help Reduce Colorectal Cancer Screening Gaps
Colorectal cancer screening is a longstanding preventive priority, yet participation and follow-up remain uneven across patient groups. Safety‑net primary care settings often face barriers that limit screening... Read more
Algorithm Panel Aids Liver Fibrosis Assessment and Liver Cancer Surveillance
Chronic liver disease is common and often progresses silently, increasing the risk of cirrhosis and hepatocellular carcinoma when not detected early. With an estimated 1.5 billion people affected worldwide... Read moreIndustry
view channelWerfen and Oxford Nanopore Collaborate on Transplant Assay Development
Werfen (Barcelona, Spain), a global specialized diagnostics company, has announced a strategic collaboration with Oxford Nanopore Technologies (Oxford, UK), which develops nanopore-based sequencing technology,... Read more