Cell-Free DNA Identifies Liver Transplant Patients with Acute Rejection
|
By LabMedica International staff writers Posted on 04 Aug 2016 |
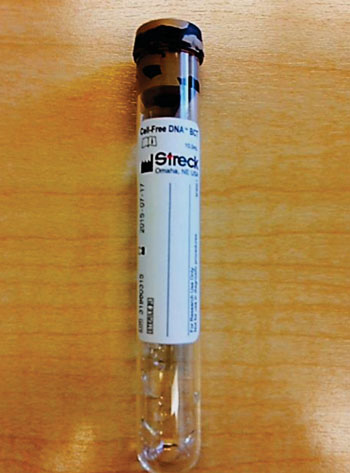
Image: A Cell-Free DNA BCT collection tube (Photo courtesy of Streck / Pathology Associates Medical Laboratory).
A cell-free DNA (cfDNA) test could help liver transplant patients receive crucial treatment for rejection faster, and has the potential to improve the prognosis of kidney and heart transplant patients as well.
Episodes of acute rejection, that is rejection that takes place in the first few months after an organ transplant, are relatively common. In liver transplant patients in particular, acute rejection develops in about 20% of those treated with standard immunosuppressive therapy. The gold standard for identifying rejection is biopsy, which is expensive and invasive, and at present there are no effective blood tests to take its place.
Scientists at Chronix Biomedical (Göttingen, Germany) and their associates determined whether a blood test for graft-derived cell-free DNA, which is cell-free DNA from a transplanted organ, could identify liver transplant patients with acute rejection. In a first-of-its-kind prospective multicenter trial, they monitored graft-derived cell-free DNA in the blood of 106 adult liver transplant recipients for at least one year post transplant. . Cell-free DNA was extracted from equal to or more than 1 mL EDTA plasma, obtained in Cell-free DNA-BCT tubes (Streck, Omaha, NE, USA). The turn-around time for an initial sample is about two days and one working day for any consecutive sample.
The teams found that in the 87 stable patients with no signs of graft injury and who were negative for hepatitis C virus infection, the median graft-derived cell-free DNA percentage decreased within the first week to a baseline level of less than 10% of total cell-free DNA concentrations. However, in the 20 patients with samples drawn during biopsy-proven acute rejection periods, graft-derived cell-free DNA levels were about 10-fold higher than those observed in the stable patients.
Overall they determined that by testing for graft-derived cell-free DNA levels of more than 10%, they were able to identify more than 90% of liver transplant patients with acute rejection, which was a substantially higher percentage than what conventional liver function tests can identify. They also believe that this test could detect heart and kidney transplant rejection, and are conducting additional studies to confirm this.
Ekkehard Schütz, MD, PhD, the senior author of the study, said, “This is really a universal test, you can use it for all kinds of solid organ transplantation since it’s just detecting the graft DNA, and it’s independent of what graft you are looking at. It will allow us to start treating these patients as early as possible, which not only impacts the acute situation that the patient is suffering at the time, but also impacts the long term survival of the graft. If we are able to diagnose rejection quickly enough, within a day or one and a half days, and the treating physician can react, then we can avoid really high-grade rejections further down the line.” The study was presented at the 68th American Association of Clinical Chemistry (AACC) Annual Scientific Meeting held July 31 to August 4, 2016, in Philadelphia, PA, USA.
Related Links:
Chronix Biomedical
Streck
American Association of Clinical Chemistry
Episodes of acute rejection, that is rejection that takes place in the first few months after an organ transplant, are relatively common. In liver transplant patients in particular, acute rejection develops in about 20% of those treated with standard immunosuppressive therapy. The gold standard for identifying rejection is biopsy, which is expensive and invasive, and at present there are no effective blood tests to take its place.
Scientists at Chronix Biomedical (Göttingen, Germany) and their associates determined whether a blood test for graft-derived cell-free DNA, which is cell-free DNA from a transplanted organ, could identify liver transplant patients with acute rejection. In a first-of-its-kind prospective multicenter trial, they monitored graft-derived cell-free DNA in the blood of 106 adult liver transplant recipients for at least one year post transplant. . Cell-free DNA was extracted from equal to or more than 1 mL EDTA plasma, obtained in Cell-free DNA-BCT tubes (Streck, Omaha, NE, USA). The turn-around time for an initial sample is about two days and one working day for any consecutive sample.
The teams found that in the 87 stable patients with no signs of graft injury and who were negative for hepatitis C virus infection, the median graft-derived cell-free DNA percentage decreased within the first week to a baseline level of less than 10% of total cell-free DNA concentrations. However, in the 20 patients with samples drawn during biopsy-proven acute rejection periods, graft-derived cell-free DNA levels were about 10-fold higher than those observed in the stable patients.
Overall they determined that by testing for graft-derived cell-free DNA levels of more than 10%, they were able to identify more than 90% of liver transplant patients with acute rejection, which was a substantially higher percentage than what conventional liver function tests can identify. They also believe that this test could detect heart and kidney transplant rejection, and are conducting additional studies to confirm this.
Ekkehard Schütz, MD, PhD, the senior author of the study, said, “This is really a universal test, you can use it for all kinds of solid organ transplantation since it’s just detecting the graft DNA, and it’s independent of what graft you are looking at. It will allow us to start treating these patients as early as possible, which not only impacts the acute situation that the patient is suffering at the time, but also impacts the long term survival of the graft. If we are able to diagnose rejection quickly enough, within a day or one and a half days, and the treating physician can react, then we can avoid really high-grade rejections further down the line.” The study was presented at the 68th American Association of Clinical Chemistry (AACC) Annual Scientific Meeting held July 31 to August 4, 2016, in Philadelphia, PA, USA.
Related Links:
Chronix Biomedical
Streck
American Association of Clinical Chemistry
Latest AACC 2016 News
- Molecular Test Detects Three Arboviruses in Plasma Samples
- Derived Exosomal Protein Biomarkers in Alzheimer’s Disease Diagnosis
- New Biochip Array Developed for ApoE4 Classification
- New Method Tested for Early Diagnosis Pediatric Diabetic Nephropathy
- FDA-Cleared Automated Cell Counter for CSF Launched at AACC 2016
- Semen Analysis Portfolio with Two New Products Featured at AACC 2016
- Automation Solutions for Clinical Diagnostic Equipment Showcased at AACC 2016
- New Tubes Designed for Medium Sample Volumes
- Multi Sample Osmometer Improves Testing Efficiency
- Innovative Information System Optimizes Laboratory Processes
- Innovative eLearning Interface Seamlessly Connects Competency Data
- Cloud-Based Connectivity Platform Advances Decentralized Healthcare
- Adhesives Research to Present Hydrophilic Adhesive Technologies
- Point-of-Care Immunoassay Analyzer on Display at AACC Annual Meeting
- Assay for Determination of 17-OH Progesterone to Be Featured at AACC Annual Meeting
- Fully Automated HbA1c Analyzer Available for Inspection at AACC Annual Meeting
Channels
Clinical Chemistry
view channel
Saliva-Based Test Detects Biochemical Signs of Sleep Loss
Acute sleep loss impairs cognition and motor skills, raising safety risks that resemble alcohol intoxication. Clinicians currently lack an objective biochemical test to determine when someone is dangerously... Read more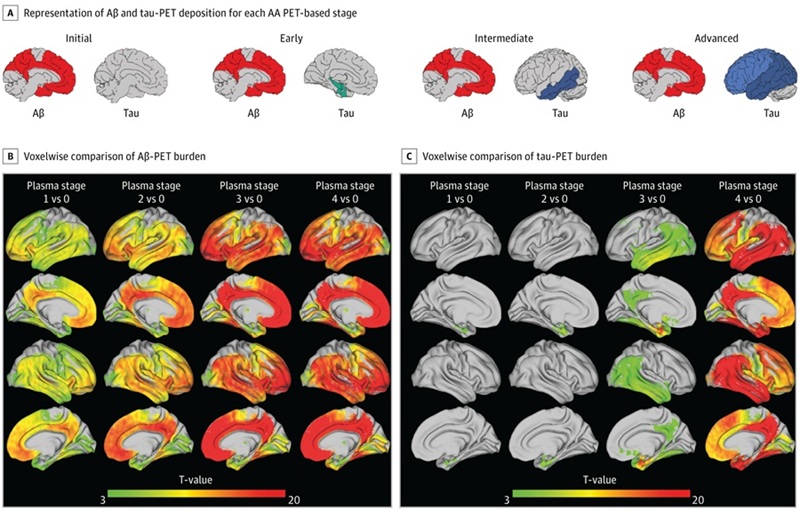
Simple Dual-Tau Blood Test Detects and Stages Alzheimer’s Disease
Alzheimer’s disease is typically confirmed and staged with positron emission tomography scans and cerebrospinal fluid testing, procedures that are costly and invasive. Broader access to minimally invasive... Read more
Alzheimer’s Blood Biomarkers Linked to Early Cognitive Differences Before Dementia
Blood-based screening for Alzheimer’s disease offers a noninvasive, lower-cost alternative to brain imaging or spinal fluid testing, yet its ability to flag the earliest cognitive changes has been unclear.... Read moreMolecular Diagnostics
view channel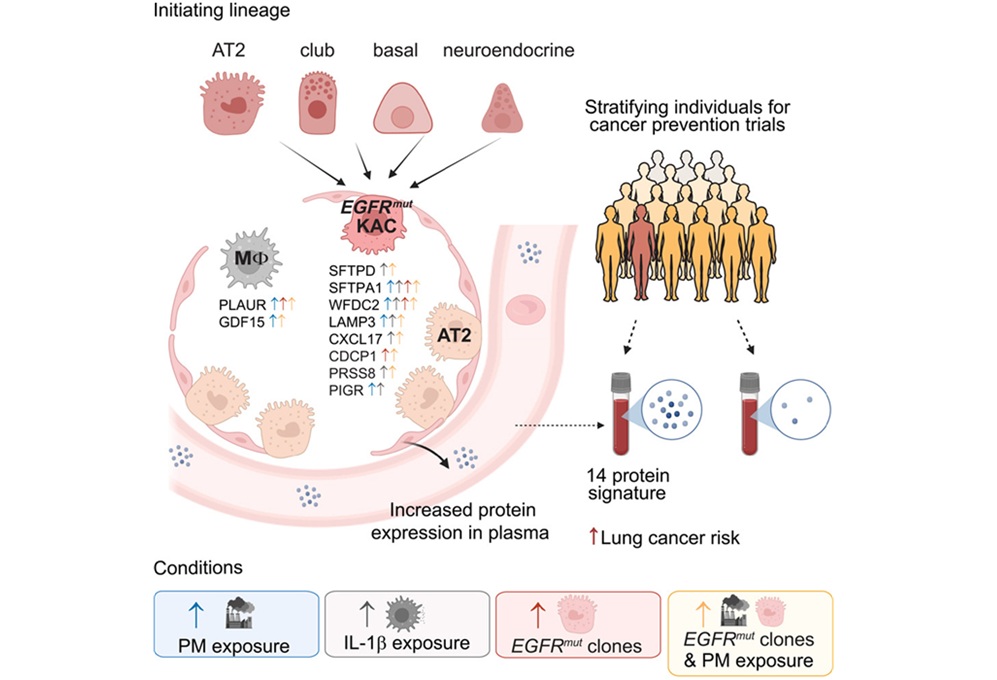
Plasma Protein Signature Predicts Lung Cancer Risk Up to Five Years Ahead
Lung cancer remains a leading cause of cancer death, and many cases are detected only after symptoms appear. Current screening programs largely target people with a history of smoking, leaving other at-risk... Read more
Circulating Tumor DNA Testing Guides Chemotherapy, Reduces Relapse in Colon Cancer
Adjuvant therapy decisions after curative surgery for colon cancer remain difficult, as conventional clinicopathologic factors often fail to capture residual disease risk. Liquid biopsy approaches that... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channelAptamer-Based Biosensor Enables Mutation-Resilient SARS-CoV-2 Detection
Rapid evolution of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can undermine existing molecular diagnostics, especially when assays target small viral components. Double-antibody sandwich... Read more
Study Points to Autoimmune Pathway Behind Long COVID Symptoms
Long COVID leaves many SARS-CoV-2 survivors with persistent fatigue, cognitive issues, palpitations, and musculoskeletal pain for months or years. Estimates cited in new research suggest 4%–20% of infected... Read more
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read moreMicrobiology
view channel
Gut Microbiome Signatures Help Identify Risk of IBD Progression
Inflammatory bowel disease (IBD), encompassing Crohn’s disease and ulcerative colitis, is a chronic relapsing inflammatory disorder of the gastrointestinal tract with highly variable outcomes.... Read more
FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
Clinical guidelines support testing based on patient presentation in suspected gastrointestinal infections, yet available technologies have often forced laboratories to choose between panels that are too... Read morePathology
view channel
Blood-Based Method Tracks Gene Activity in the Living Brain
Real-time measurement of gene activity in the brain has been limited by assays requiring destructive tissue sampling. Tracking active genes could reveal how the body responds to environmental factors,... Read more
FDA Approval Expands Automated PD-L1 Testing Across Solid Tumors
Clinical laboratories play a central role in guiding immunotherapy by reporting programmed death ligand-1 (PD‑L1) status across multiple solid tumors. Many sites are standardizing this work on fully automated... Read moreTechnology
view channel
AI Platform Links Biomarker Results to Cancer Clinical Trials and Guidelines
Oncology teams must manage growing volumes of genomic data, rapidly evolving clinical trial options, and frequently updated care guidelines, all within tight clinic schedules. Translating complex tumor... Read more
Agentic AI Platform Supports Genomic Decision-Making in Oncology
Oncology care teams increasingly face the challenge of managing complex molecular diagnostics, evolving treatment options, and extensive electronic health record documentation. Translating multimodal data... Read moreIndustry
view channel