Asparagine Metabolism Empowers Group A Streptococcus Infection
|
By LabMedica International staff writers Posted on 30 Jan 2014 |
![Image: Photomicrograph (900x) of Streptococcus pyogenes bacteria, viewed using Pappenheim\'s stain (Photo courtesy of the CDC - [US] Centers for Disease Control and Prevention). Image: Photomicrograph (900x) of Streptococcus pyogenes bacteria, viewed using Pappenheim\'s stain (Photo courtesy of the CDC - [US] Centers for Disease Control and Prevention).](https://globetechcdn.com/mobile_labmedica/images/stories/articles/article_images/2014-01-30/GMS-020a.gif)
Image: Photomicrograph (900x) of Streptococcus pyogenes bacteria, viewed using Pappenheim\'s stain (Photo courtesy of the CDC - [US] Centers for Disease Control and Prevention).
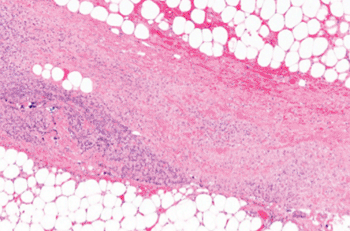
Image: Micrograph (H&E stain) of necrotizing fasciitis, showing necrosis (center of image) of the dense connective tissue, i.e., fascia, interposed between fat lobules (top-right and bottom-left of image) (Photo courtesy of Wikimedia Commons).
The bacteria that cause the frightening syndrome called "flesh-eating disease" have been found to be stimulated by the amino acid asparagine and inhibited by the chemotherapeutic enzyme asparaginase, which destroys asparagine.
Necrotizing fasciitis or NF, commonly known as "flesh-eating disease" is a rare infection of the deeper layers of skin and subcutaneous tissues, which quickly spreads across the fascial plane within the subcutaneous tissue. Individuals having compromised immune systems (due to conditions like diabetes, cancer, etc.) have greater risk of developing NF. It is a severe disease of sudden onset and is usually treated immediately with high doses of intravenous antibiotics. "Flesh-eating disease" is a misnomer, as the bacteria involved—most frequently Streptococcus pyogenes, or Group A Streptococcus (GAS)—do not actually "eat" the tissue. They cause the destruction of skin and muscle by releasing toxins, which include streptococcal pyogenic exotoxins.
Investigators at the Hebrew University of Jerusalem (Israel) reported in the January 16, 2014, issue of the journal Cell that during adherence to host cells, GAS releases streptolysin toxins, which create endoplasmic reticulum stress in the host cells. This stress causes an increase in the expression of the enzyme asparagine synthetase and the production of asparagine. The released asparagine is sensed by the bacteria, which induces altered expression of about 17% of the bacterial genes.
Asparaginase, a widely used chemotherapeutic agent, was found to block GAS growth in human blood and prevented GAS proliferation in a mouse model. To date asparaginase has not been used to treat GAS infections.
The Yissum Research Development Company (Jerusalem, Israel), the technology transfer arm of the Hebrew University of Jerusalem, has registered a patent for this discovery and is seeking commercial partners to help develop effective therapies against invasive Streptococcus infections.
Related Links:
Hebrew University of Jerusalem
Yissum Research Development Company
Necrotizing fasciitis or NF, commonly known as "flesh-eating disease" is a rare infection of the deeper layers of skin and subcutaneous tissues, which quickly spreads across the fascial plane within the subcutaneous tissue. Individuals having compromised immune systems (due to conditions like diabetes, cancer, etc.) have greater risk of developing NF. It is a severe disease of sudden onset and is usually treated immediately with high doses of intravenous antibiotics. "Flesh-eating disease" is a misnomer, as the bacteria involved—most frequently Streptococcus pyogenes, or Group A Streptococcus (GAS)—do not actually "eat" the tissue. They cause the destruction of skin and muscle by releasing toxins, which include streptococcal pyogenic exotoxins.
Investigators at the Hebrew University of Jerusalem (Israel) reported in the January 16, 2014, issue of the journal Cell that during adherence to host cells, GAS releases streptolysin toxins, which create endoplasmic reticulum stress in the host cells. This stress causes an increase in the expression of the enzyme asparagine synthetase and the production of asparagine. The released asparagine is sensed by the bacteria, which induces altered expression of about 17% of the bacterial genes.
Asparaginase, a widely used chemotherapeutic agent, was found to block GAS growth in human blood and prevented GAS proliferation in a mouse model. To date asparaginase has not been used to treat GAS infections.
The Yissum Research Development Company (Jerusalem, Israel), the technology transfer arm of the Hebrew University of Jerusalem, has registered a patent for this discovery and is seeking commercial partners to help develop effective therapies against invasive Streptococcus infections.
Related Links:
Hebrew University of Jerusalem
Yissum Research Development Company
Latest BioResearch News
- Biomarker Signals Chemotherapy Resistance in Relapsed Small Cell Lung Cancer
- Inflammatory Gene Signature Links Metabolic Disease to Pancreatic Cancer Recurrence
- Study Links Abnormal Gene Splicing to Treatment Response in Metastatic Kidney Cancer
- Research Reveals How Some Aplastic Anemia Patients Recover Bone Marrow Function
- New Molecular Insights Support Diagnosis of Hodgkin Lymphoma
- Epigenetic Signals and Blood Markers Aid Chronic Fatigue Syndrome Diagnosis
- Microenvironment Biomarkers Could Enable Early Lung Cancer Detection
- Study Identifies Protein Changes Driving Immunotherapy Resistance in Multiple Myeloma
- Genetic Analysis Identifies BRCA-Linked Risks Across Multiple Cancers
- Study Identifies Hidden B-Cell Mutations in Autoimmune Disease
- Single-Cell Method Measures RNA and Proteins to Reveal Immune Responses
- Study Links Midlife Vitamin D to Lower Tau in Alzheimer's
- International Consensus Standardizes Tumor Microbiota Detection and Reporting
- Common Metablolic Enzyme Could Predict Response to Cancer Immunotherapy
- Newly Identfied Genetic Variants in MND Support Prognosis and Family Testing
- Innate Immunity Variants Associated With Earlier Breast Cancer in BRCA1 Carriers
Channels
Clinical Chemistry
view channel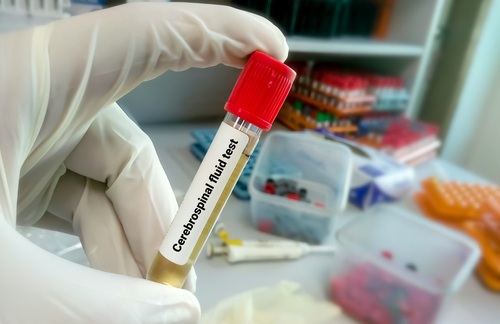
Ultrasensitive Test Detects Key Biomarker of Frontotemporal Dementia Subtype
Dementia affects more than 57 million people worldwide and is projected to nearly double within two decades, straining health systems and families. While biomarkers now enable accurate identification of... Read more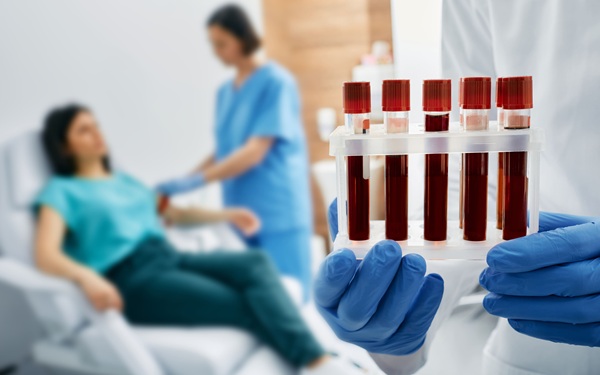
Routine Blood Tests Years Before Pregnancy Could Identify Preeclampsia Risk
High blood pressure during pregnancy is common and can progress to pre-eclampsia, making close monitoring at antenatal visits essential. However, most risk assessment begins only after pregnancy has started.... Read moreMolecular Diagnostics
view channel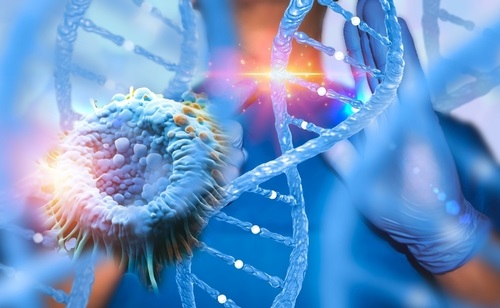
Liquid Biopsy Biomarkers Distinguish Inflammatory Breast Cancer and Support Monitoring
Inflammatory breast cancer is among the most aggressive forms of breast malignancy and remains challenging to diagnose and monitor. Obtaining tumor tissue can be difficult, and standard genome and RNA... Read more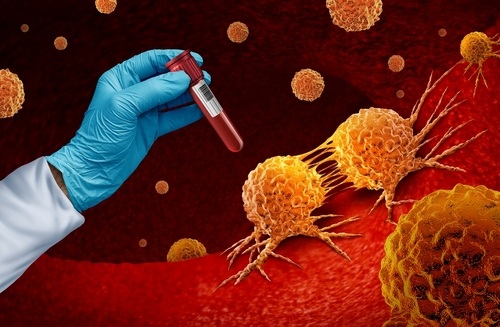
Blood Test Maps Tumor Microenvironment to Predict Immunotherapy Response
Immunotherapy has transformed cancer care, yet durable benefit remains limited to a subset of patients, and clinicians still lack reliable tools to predict response before treatment begins.... Read more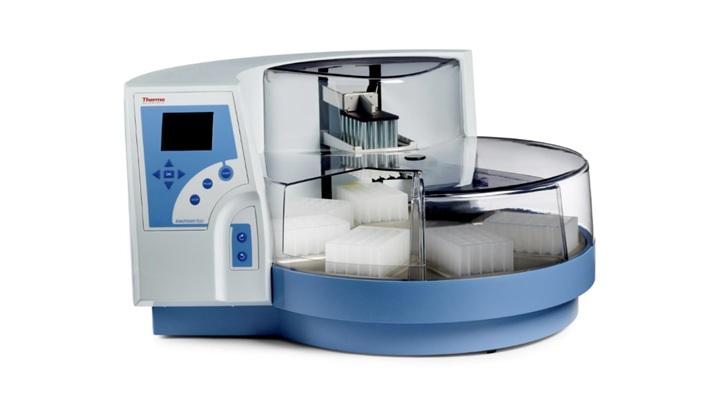
Multiplex Respiratory Panel Integrates Automated Extraction to Streamline High-Volume Testing
Respiratory infections drive heavy testing volumes in clinical laboratories, where accurate, timely results across multiple pathogens are essential. Many labs are seeking to streamline workflows and increase... Read moreHematology
view channel
Advanced CBC-Derived Indices Integrated into Hematology Platforms
Diatron, a STRATEC brand, has introduced six advanced hematological indices on its Aquila, Aquarius 3, and Abacus 5 hematology analyzers. The new Research Use Only (RUO) indices include Neutrophil-to-Lymphocyte... Read more
Blood Test Enables Early Detection of Multiple Myeloma Relapse
Bone marrow biopsies remain central to diagnosing and monitoring multiple myeloma, yet the procedure is painful, invasive, and often repeated over time. Older patients—who represent most new cases—can... Read moreImmunology
view channel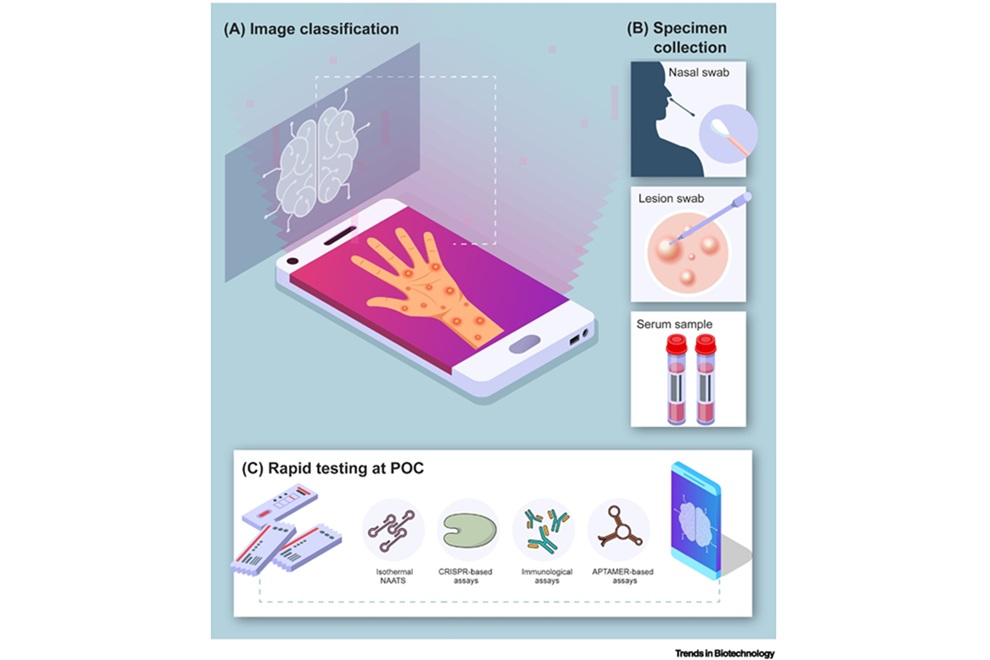
Point-of-Care Tests Could Expand Access to Mpox Diagnosis
Mpox outbreaks in non-endemic regions have underscored the need for rapid, accessible diagnostics to limit transmission. Polymerase chain reaction (PCR) remains the clinical reference, yet it depends on... Read more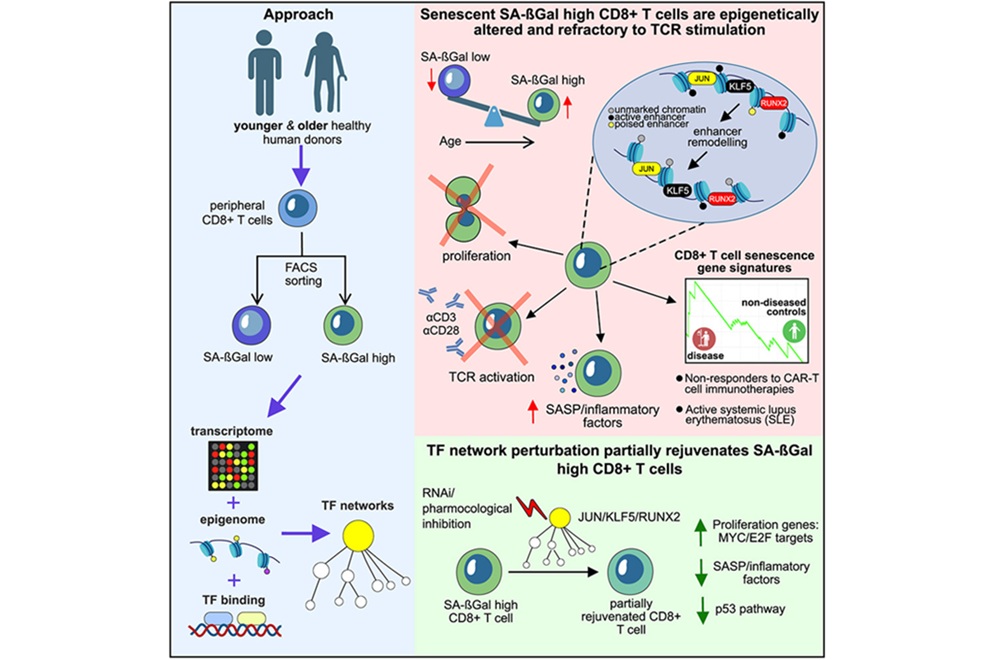
T-Cell Senescence Profiling May Predict CAR T Responses
Chimeric antigen receptor (CAR) T-cell therapy can deliver striking, durable remissions, yet many patients experience minimal or no benefit. The quality of patient-derived cytotoxic T lymphocytes used... Read moreMicrobiology
view channel
Rapid Antigen Biosensor Detects Active Tuberculosis in One Hour
Tuberculosis remains a major global health challenge and continues to drive significant morbidity and mortality. The World Health Organization’s 2024 global report cites it as the leading cause of death... Read more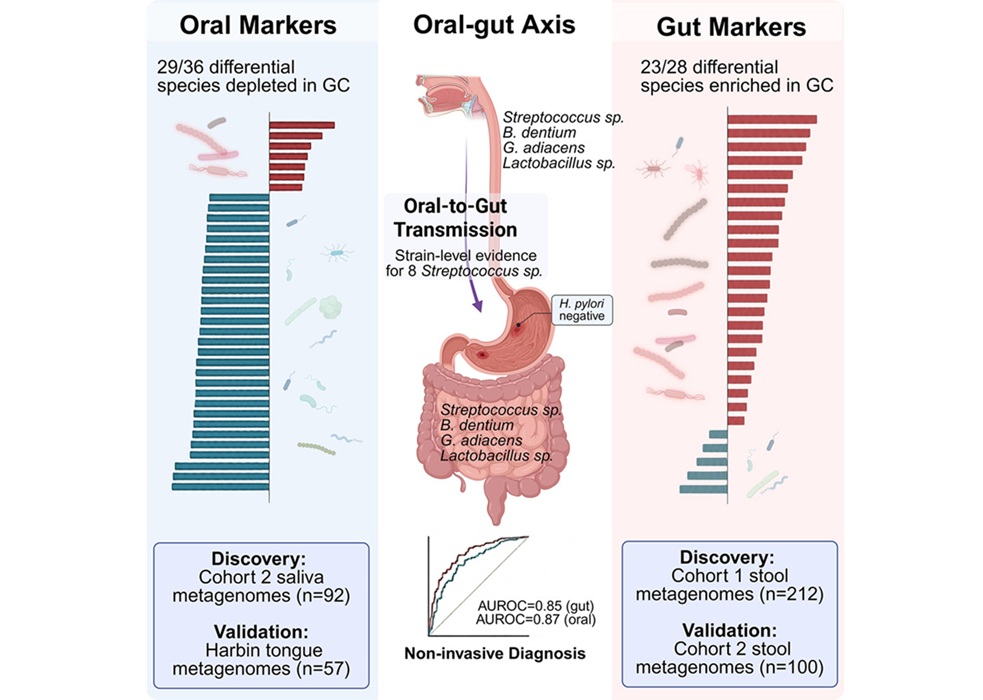
Oral–Gut Microbiome Signatures Identify Early Gastric Cancer
Early detection of gastric cancer could be advanced by scalable screening strategies using minimally invasive sampling. Saliva collection is noninvasive and cost-effective, supporting wider adoption... Read morePathology
view channel
FDA Clears AI Digital Pathology Tool for Breast Cancer Risk Stratification
Risk assessment at diagnosis is central to guiding therapy for early-stage, hormone receptor-positive, human epidermal growth factor receptor 2-negative (HR+/HER2-) invasive breast cancer, where overtreatment... Read more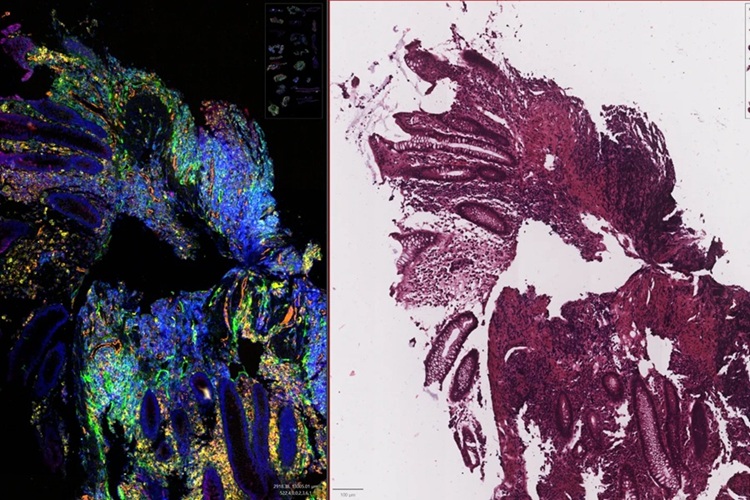
New AI Tool Reveals Hidden Genetic Signals in Routine H&E Slides
Pathologists worldwide rely on hematoxylin and eosin (H&E) slides to examine tissue architecture, yet these stains do not reveal the underlying molecular activity that often drives disease.... Read moreTechnology
view channel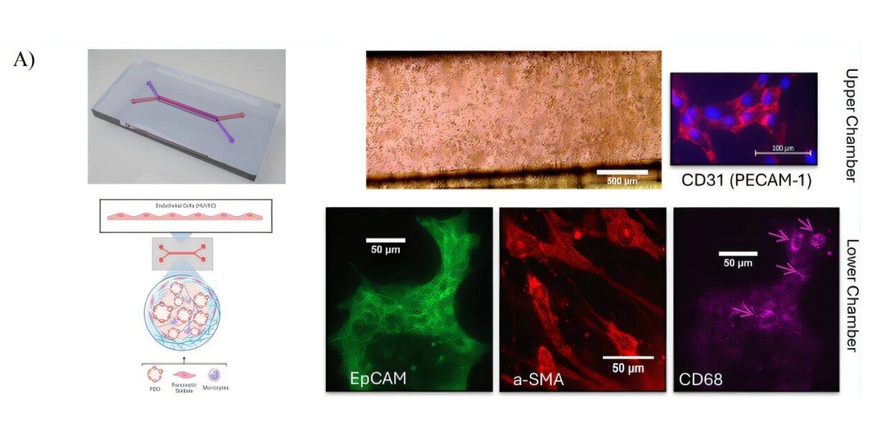
Tumor-on-a-Chip Platform Models Pancreatic Cancer Treatment Response
Pancreatic cancer remains one of the hardest malignancies to treat because tumors are embedded within a dense microenvironment that shapes growth and therapy response. Standard laboratory models often... Read more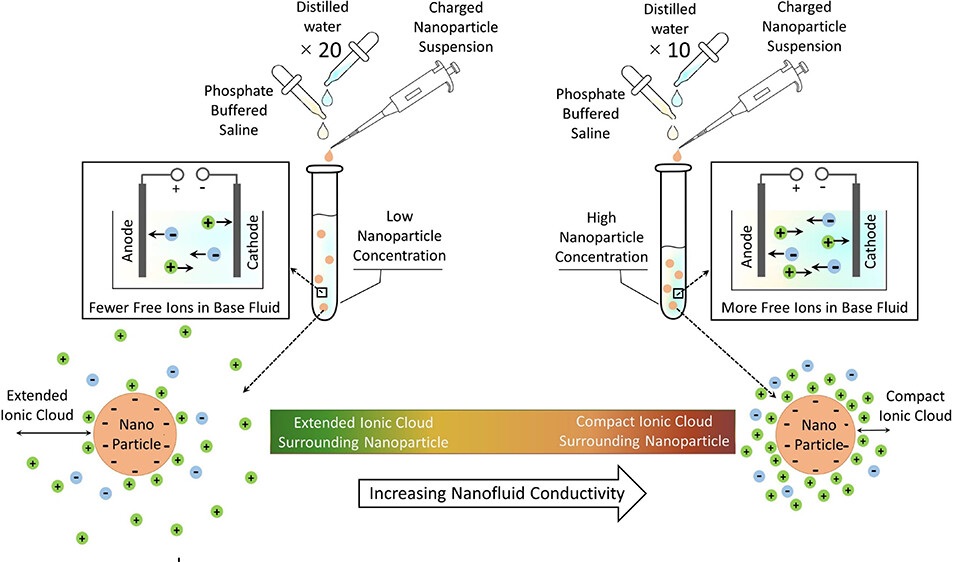
New Platform Captures Extracellular Vesicles for Early Cancer Detection
Early diagnosis remains the most effective way to reduce cancer mortality, yet many screening tools miss disease at its earliest stages. Biomarkers shed by tumors into blood and other fluids can be scarce... Read moreIndustry
view channel
Roche to Acquire PathAI for Up to $1.05 Billion to Strengthen AI Diagnostics Portfolio
Roche has entered into a definitive merger agreement to acquire PathAI, a company focused on digital pathology and artificial intelligence for pathology laboratories and the biopharma industry.... Read more