Histone Deacetylase Inhibitors Boost Parvovirus Cancer Killing Action
|
By LabMedica International staff writers Posted on 28 Oct 2013 |
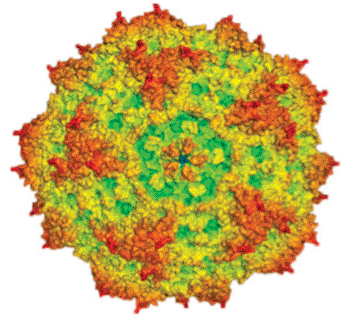
Image: Computer-generated representation of parvovirus H-1 (H-1PV) (Photo courtesy of Dr. Antonio Marchini, German Cancer Research Center).
The anticancer action of parvoviruses can be dramatically improved by co-treating cancer cells with parvovirus and histone deacetylase inhibitors (HDACIs) such as valproic acid.
The rat parvovirus H-1PV has oncolytic and tumor-suppressive properties potentially exploitable in cancer therapy. This possibility is being explored by cancer researchers, and while results have been encouraging, they have found that it is necessary to improve the cancer-killing capability of the virus.
Towards this end, investigators at the German Cancer Research Center (Heidelberg) have sought drugs or drug combinations that would improve the ability of parvoviruses to kill cancer cells. In a paper published in the September 17, 2013, online edition of the journal EMBO Molecular Medicine they described the effect of the histone deacetylase inhibitor valproic acid (VPA) on the interaction between H-1PV and human cervical carcinoma and pancreatic carcinoma cell lines.
The investigators showed that co-treatment of cultures with the parvovirus and VPA boosted the ability of the virus to kill a range of human cervical carcinoma and pancreatic carcinoma cell lines by inducing oxidative stress, DNA damage, and apoptosis. Furthermore, in rat and mouse xenograft models, H-1PV/VPA co-treatment strongly inhibited tumor growth promoting complete tumor remission in all co-treated animals. In contrast, animals treated with the same virus dose without the drug displayed no regression, not even when a 20-times higher dose of viruses was administered.
At the molecular level, the investigators found that the parvovirus nonstructural protein NS1 modulated viral transcription and cytotoxicity, both of which were enhanced by VPA treatment. NS1 was acetylated at residues K85 and K257 and addition of VPA correlated with an enhanced rate of NS1 acetylation. In contrast, amino-acid substitution of the two acetylation sites strongly impaired NS1-mediated viral gene transcription, viral replication, and cytotoxicity. VPA induced hyper-acetylation of NS1, which converted the protein into a more active polypeptide.
"The synergistic effect of a combination of parvoviruses and valproic acid enables us to deliver both the viruses and the drug at low doses, which prevents severe side effects," said senior author Dr. Antonio Marchini, a principle investigator in virology at the German Cancer Research Center. "The results are encouraging us to carry out further tests of this combination therapy. We believe it has the potential to arrest tumor growth in severe cases of cancer. We obtained impressive results in preclinical trials with parvovirus H-1 in brain tumors. However, the oncolytic effect of the viruses is weaker in other cancers. Therefore, we are searching for ways to increase the therapeutic potential of the viruses."
Related Links:
German Cancer Research Center
The rat parvovirus H-1PV has oncolytic and tumor-suppressive properties potentially exploitable in cancer therapy. This possibility is being explored by cancer researchers, and while results have been encouraging, they have found that it is necessary to improve the cancer-killing capability of the virus.
Towards this end, investigators at the German Cancer Research Center (Heidelberg) have sought drugs or drug combinations that would improve the ability of parvoviruses to kill cancer cells. In a paper published in the September 17, 2013, online edition of the journal EMBO Molecular Medicine they described the effect of the histone deacetylase inhibitor valproic acid (VPA) on the interaction between H-1PV and human cervical carcinoma and pancreatic carcinoma cell lines.
The investigators showed that co-treatment of cultures with the parvovirus and VPA boosted the ability of the virus to kill a range of human cervical carcinoma and pancreatic carcinoma cell lines by inducing oxidative stress, DNA damage, and apoptosis. Furthermore, in rat and mouse xenograft models, H-1PV/VPA co-treatment strongly inhibited tumor growth promoting complete tumor remission in all co-treated animals. In contrast, animals treated with the same virus dose without the drug displayed no regression, not even when a 20-times higher dose of viruses was administered.
At the molecular level, the investigators found that the parvovirus nonstructural protein NS1 modulated viral transcription and cytotoxicity, both of which were enhanced by VPA treatment. NS1 was acetylated at residues K85 and K257 and addition of VPA correlated with an enhanced rate of NS1 acetylation. In contrast, amino-acid substitution of the two acetylation sites strongly impaired NS1-mediated viral gene transcription, viral replication, and cytotoxicity. VPA induced hyper-acetylation of NS1, which converted the protein into a more active polypeptide.
"The synergistic effect of a combination of parvoviruses and valproic acid enables us to deliver both the viruses and the drug at low doses, which prevents severe side effects," said senior author Dr. Antonio Marchini, a principle investigator in virology at the German Cancer Research Center. "The results are encouraging us to carry out further tests of this combination therapy. We believe it has the potential to arrest tumor growth in severe cases of cancer. We obtained impressive results in preclinical trials with parvovirus H-1 in brain tumors. However, the oncolytic effect of the viruses is weaker in other cancers. Therefore, we are searching for ways to increase the therapeutic potential of the viruses."
Related Links:
German Cancer Research Center
Latest BioResearch News
- Lung Cancer Study Reveals Cellular Program Behind Therapy Resistance
- Tumor Genome Marker May Predict Treatment Benefit in Pediatric Cancers
- Lysosomal Gene Defect Linked to Severe Childhood Brain Disorders
- Genetic Testing Identifies Greater Inherited Sudden Cardiac Arrest Risk in Younger Individuals
- Hidden 'Jumping Gene' Variant Linked to Higher Pancreatic Cancer Risk
- Common White Blood Cells Produce Schizophrenia-Linked Protein
- Nanopore Method Captures RNA Folding at Single-Molecule Resolution
- Tumor Microenvironment Marker Linked to Worse Survival in Solid Tumors
- Hidden Immune Gene Defect May Explain Kaposi Sarcoma Susceptibility
- Genetic Markers May Help Predict Amputation Risk in Peripheral Artery Disease
- Gene Signature Shows Promise for Depression Biomarker Testing
- AI-Driven Tumor Profiling Initiative Targets Precision Therapy Development
- Researchers Map Protein and Glycosylation Across 15 Human Body Fluids
- Telomere Length Abnormalities Linked to Lymphoma Development
- Biomarker Signals Chemotherapy Resistance in Relapsed Small Cell Lung Cancer
- Inflammatory Gene Signature Links Metabolic Disease to Pancreatic Cancer Recurrence
Channels
Clinical Chemistry
view channel
Alzheimer’s Blood Biomarkers Linked to Early Cognitive Differences Before Dementia
Blood-based screening for Alzheimer’s disease offers a noninvasive, lower-cost alternative to brain imaging or spinal fluid testing, yet its ability to flag the earliest cognitive changes has been unclear.... Read more
Urine-Based Test Shows Promise for Autism Screening in Children
Autism spectrum disorder (ASD) is commonly diagnosed through behavioral assessments, which can involve long waits that delay intervention. Earlier identification is linked to better developmental outcomes,... Read moreMolecular Diagnostics
view channel
Blood-Based Assay Enables Noninvasive Monitoring of Sarcoma Immunotherapy Response
Sarcomas remain difficult to monitor during immunotherapy, as low tumor mutation burden can limit traditional circulating tumor DNA approaches and repeat tissue biopsies are often impractical in advanced disease.... Read more
Tumor Mutation Marker Helps Refine Lung Cancer Prognosis and Guide Therapy Selection
Lung cancer remains the leading cause of cancer death worldwide, while heterogeneous tumor genetics continue to complicate treatment decisions. Although molecular testing is increasingly used to match... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channel
Study Points to Autoimmune Pathway Behind Long COVID Symptoms
Long COVID leaves many SARS-CoV-2 survivors with persistent fatigue, cognitive issues, palpitations, and musculoskeletal pain for months or years. Estimates cited in new research suggest 4%–20% of infected... Read more
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read moreMicrobiology
view channel
Gut Microbiome Signatures Help Identify Risk of IBD Progression
Inflammatory bowel disease (IBD), encompassing Crohn’s disease and ulcerative colitis, is a chronic relapsing inflammatory disorder of the gastrointestinal tract with highly variable outcomes.... Read more
FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
Clinical guidelines support testing based on patient presentation in suspected gastrointestinal infections, yet available technologies have often forced laboratories to choose between panels that are too... Read morePathology
view channel
AI-Powered Atlas Maps Immune Structures Linked to Cancer Outcomes
Tertiary lymphoid structures are emerging as important indicators of antitumor immunity, but their heterogeneity and spatial context within tumors remain difficult to capture through routine diagnostics.... Read more
AI Tool Extracts Immune Signals from Biopsy to Inform Myeloma Therapy
Multiple myeloma is a bone marrow malignancy in which patients can respond very differently to the same treatments, making initial therapy decisions difficult. Clinicians must choose among options such... Read moreTechnology
view channel
AI Platform Links Biomarker Results to Cancer Clinical Trials and Guidelines
Oncology teams must manage growing volumes of genomic data, rapidly evolving clinical trial options, and frequently updated care guidelines, all within tight clinic schedules. Translating complex tumor... Read more
Agentic AI Platform Supports Genomic Decision-Making in Oncology
Oncology care teams increasingly face the challenge of managing complex molecular diagnostics, evolving treatment options, and extensive electronic health record documentation. Translating multimodal data... Read moreIndustry
view channel