Photochemical Internalization Cancer Treatment with Minor Side Effects Closer to Reality
|
By LabMedica International staff writers Posted on 24 Jan 2012 |
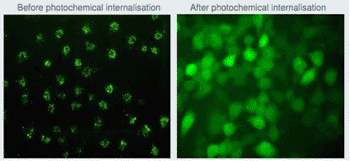
Image: Light-sensitive molecules (orange) before and after photochemical internalization (PCI) treatment. At left, the molecules are trapped within membranes inside the cancer cell. At right, the molecules have been released and can spread--along with the cytotoxic drugs--throughout the entire cancer cell (Photo courtesy of Pål K. Selbo/PCI Biotech).
Side effects are currently the biggest drawback with any cancer treatment. A Norwegian biotech company is getting closer to creating a treatment that destroys only cancer cells, leaving other cells unaffected.
It is not hard to find a drug that destroys cancer cells. The problem lies in the fact that a drug’s active compounds kill indiscriminately, not only diseased cells die but also other cells in the body. This is why the side effects associated with conventional cancer treatment are frequently so severe.
The hope of any cancer researcher is to develop a drug that works only against a cancerous tumor--without adversely affecting the rest of the body. This objective can be attained in two ways: one is to produce targeted drugs that affect only the cancer cells; the other is to design smarter way of delivering a drug to its target without affecting other parts of the body.
A biotech company, PCI Biotech Holding, ASA (Lysaker, Norway), has been focusing on the latter approach since 2000. Researchers working on the project Fotokjemisk internalisering for Cellegiftterapi av Kreft (Photochemical Internalization of Chemotherapy) have steadily been getting closer to a solution. Headed by chief scientific officer Dr. Anders Høgset, the project has received funding under the Program for User-driven Research-based Innovation (BIA) at the Research Council of Norway.
The technology is based on light and is called photochemical internalization (PCI). It was discovered in 1994 at the Norwegian Radium Hospital in Oslo (now part of Oslo University Hospital). PCI Biotech uses the technology to direct a red laser to the area of the body where the drug is to have its effect. The light significantly enhances drug delivery to specific locations inside the diseased cells.
“But in order to achieve the desired effect from the light, we need to give the patient a photosensitizing compound,” explained Dr. Høgset. “This is a chemical substance increasing cells’ sensitivity to light. We have created and patented a molecule [Amphinex] that we inject into a patient and let circulate for a few days. Then we give the patient the desired drug. After a short while, we shine the laser on the tumor where both Amphinex and the medication are now present. When light is applied, Amphinex triggers processes within the cancer cells, substantially enhancing the effect of the drug.”
The challenge of effectively transporting molecules to a targeted area inside a cell has long stumped cancer researchers. For pharmaceutical companies, it has created a logjam, slowing down further development of a number of molecules with great therapeutic possibilities.
Patients have often had to receive higher doses of a drug than what would otherwise be necessary had there existed a way to target drug delivery to the right location inside a cell. Because of these higher doses, the side effects patients experience are commensurately more severe. “Now we have finally succeeded in finding a way to deliver cancer medications inside the malignant cells, destroying them effectively,” noted Dr. Høgset.
These cancer-killing medications pass through cancer cell membranes much more easily, which considerably increases their accuracy. It follows that doses can be reduced substantially with side effects becoming correspondingly less severe. “In the laboratory, we have managed to enhance the effect of some cytotoxic drugs by a full 50 times. We did so by administering Amphinex and directing light to the cancer cell,” explained Dr. Høgset.
PCI Biotech, together with University College London Hospital, began performing research on human subjects two years ago. “All patients involved in the study experienced a considerable effect from the light treatment and, in most cases, the treated tumors disappeared altogether. No serious side effects were observed,” said Dr. Høgset.
PCI Biotech is now going to follow-up with additional clinical research. Up to the present, PCI Biotech has focused on localized cancer treatment, for example, for mouth cancer, breast cancer, and facial skin cancer. Many cancer patients stand to benefit greatly from localized treatment, but a great number also require treatment that can attack cancer that has metastasized to other areas of the body.
As part of a future project, PCI Biotech intends to extend its technology to treatment of metastatic cancer. The project will evaluate whether the technology can activate a person’s immune system, enabling it to attack cancer cells in more than one part of the body.
Related Links:
PCI Biotech Holding
It is not hard to find a drug that destroys cancer cells. The problem lies in the fact that a drug’s active compounds kill indiscriminately, not only diseased cells die but also other cells in the body. This is why the side effects associated with conventional cancer treatment are frequently so severe.
The hope of any cancer researcher is to develop a drug that works only against a cancerous tumor--without adversely affecting the rest of the body. This objective can be attained in two ways: one is to produce targeted drugs that affect only the cancer cells; the other is to design smarter way of delivering a drug to its target without affecting other parts of the body.
A biotech company, PCI Biotech Holding, ASA (Lysaker, Norway), has been focusing on the latter approach since 2000. Researchers working on the project Fotokjemisk internalisering for Cellegiftterapi av Kreft (Photochemical Internalization of Chemotherapy) have steadily been getting closer to a solution. Headed by chief scientific officer Dr. Anders Høgset, the project has received funding under the Program for User-driven Research-based Innovation (BIA) at the Research Council of Norway.
The technology is based on light and is called photochemical internalization (PCI). It was discovered in 1994 at the Norwegian Radium Hospital in Oslo (now part of Oslo University Hospital). PCI Biotech uses the technology to direct a red laser to the area of the body where the drug is to have its effect. The light significantly enhances drug delivery to specific locations inside the diseased cells.
“But in order to achieve the desired effect from the light, we need to give the patient a photosensitizing compound,” explained Dr. Høgset. “This is a chemical substance increasing cells’ sensitivity to light. We have created and patented a molecule [Amphinex] that we inject into a patient and let circulate for a few days. Then we give the patient the desired drug. After a short while, we shine the laser on the tumor where both Amphinex and the medication are now present. When light is applied, Amphinex triggers processes within the cancer cells, substantially enhancing the effect of the drug.”
The challenge of effectively transporting molecules to a targeted area inside a cell has long stumped cancer researchers. For pharmaceutical companies, it has created a logjam, slowing down further development of a number of molecules with great therapeutic possibilities.
Patients have often had to receive higher doses of a drug than what would otherwise be necessary had there existed a way to target drug delivery to the right location inside a cell. Because of these higher doses, the side effects patients experience are commensurately more severe. “Now we have finally succeeded in finding a way to deliver cancer medications inside the malignant cells, destroying them effectively,” noted Dr. Høgset.
These cancer-killing medications pass through cancer cell membranes much more easily, which considerably increases their accuracy. It follows that doses can be reduced substantially with side effects becoming correspondingly less severe. “In the laboratory, we have managed to enhance the effect of some cytotoxic drugs by a full 50 times. We did so by administering Amphinex and directing light to the cancer cell,” explained Dr. Høgset.
PCI Biotech, together with University College London Hospital, began performing research on human subjects two years ago. “All patients involved in the study experienced a considerable effect from the light treatment and, in most cases, the treated tumors disappeared altogether. No serious side effects were observed,” said Dr. Høgset.
PCI Biotech is now going to follow-up with additional clinical research. Up to the present, PCI Biotech has focused on localized cancer treatment, for example, for mouth cancer, breast cancer, and facial skin cancer. Many cancer patients stand to benefit greatly from localized treatment, but a great number also require treatment that can attack cancer that has metastasized to other areas of the body.
As part of a future project, PCI Biotech intends to extend its technology to treatment of metastatic cancer. The project will evaluate whether the technology can activate a person’s immune system, enabling it to attack cancer cells in more than one part of the body.
Related Links:
PCI Biotech Holding
Latest BioResearch News
- Lung Cancer Study Reveals Cellular Program Behind Therapy Resistance
- Tumor Genome Marker May Predict Treatment Benefit in Pediatric Cancers
- Lysosomal Gene Defect Linked to Severe Childhood Brain Disorders
- Genetic Testing Identifies Greater Inherited Sudden Cardiac Arrest Risk in Younger Individuals
- Hidden 'Jumping Gene' Variant Linked to Higher Pancreatic Cancer Risk
- Common White Blood Cells Produce Schizophrenia-Linked Protein
- Nanopore Method Captures RNA Folding at Single-Molecule Resolution
- Tumor Microenvironment Marker Linked to Worse Survival in Solid Tumors
- Hidden Immune Gene Defect May Explain Kaposi Sarcoma Susceptibility
- Genetic Markers May Help Predict Amputation Risk in Peripheral Artery Disease
- Gene Signature Shows Promise for Depression Biomarker Testing
- AI-Driven Tumor Profiling Initiative Targets Precision Therapy Development
- Researchers Map Protein and Glycosylation Across 15 Human Body Fluids
- Telomere Length Abnormalities Linked to Lymphoma Development
- Biomarker Signals Chemotherapy Resistance in Relapsed Small Cell Lung Cancer
- Inflammatory Gene Signature Links Metabolic Disease to Pancreatic Cancer Recurrence
Channels
Clinical Chemistry
view channel
Saliva-Based Test Detects Biochemical Signs of Sleep Loss
Acute sleep loss impairs cognition and motor skills, raising safety risks that resemble alcohol intoxication. Clinicians currently lack an objective biochemical test to determine when someone is dangerously... Read more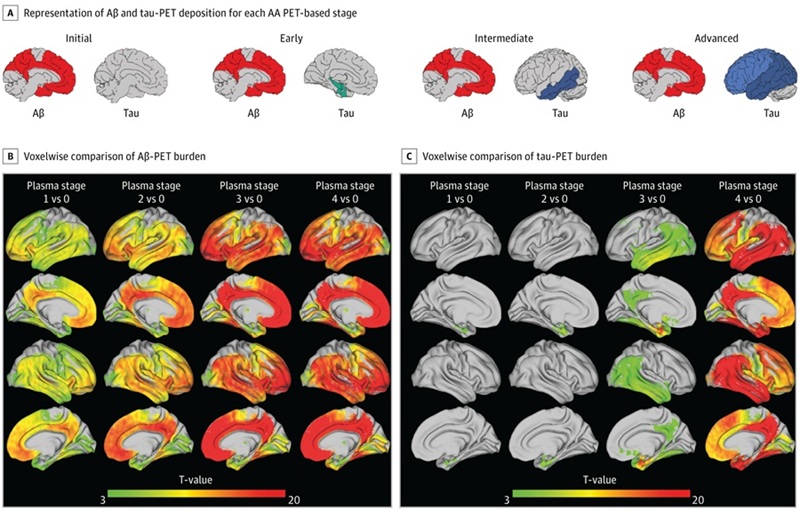
Simple Dual-Tau Blood Test Detects and Stages Alzheimer’s Disease
Alzheimer’s disease is typically confirmed and staged with positron emission tomography scans and cerebrospinal fluid testing, procedures that are costly and invasive. Broader access to minimally invasive... Read more
Alzheimer’s Blood Biomarkers Linked to Early Cognitive Differences Before Dementia
Blood-based screening for Alzheimer’s disease offers a noninvasive, lower-cost alternative to brain imaging or spinal fluid testing, yet its ability to flag the earliest cognitive changes has been unclear.... Read moreMolecular Diagnostics
view channel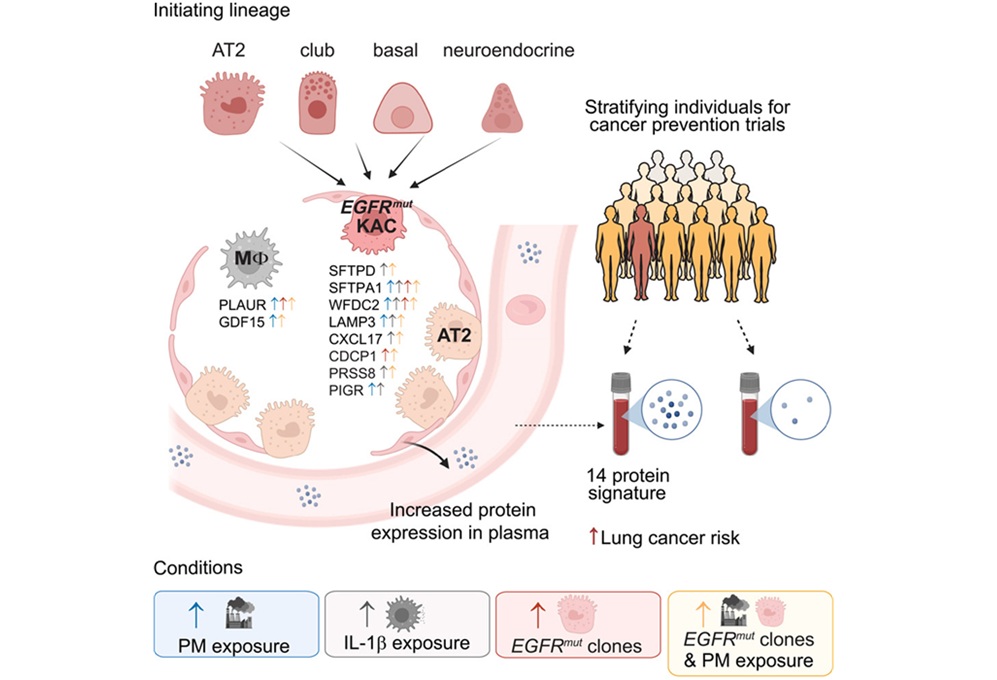
Plasma Protein Signature Predicts Lung Cancer Risk Up to Five Years Ahead
Lung cancer remains a leading cause of cancer death, and many cases are detected only after symptoms appear. Current screening programs largely target people with a history of smoking, leaving other at-risk... Read more
Circulating Tumor DNA Testing Guides Chemotherapy, Reduces Relapse in Colon Cancer
Adjuvant therapy decisions after curative surgery for colon cancer remain difficult, as conventional clinicopathologic factors often fail to capture residual disease risk. Liquid biopsy approaches that... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channelAptamer-Based Biosensor Enables Mutation-Resilient SARS-CoV-2 Detection
Rapid evolution of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can undermine existing molecular diagnostics, especially when assays target small viral components. Double-antibody sandwich... Read more
Study Points to Autoimmune Pathway Behind Long COVID Symptoms
Long COVID leaves many SARS-CoV-2 survivors with persistent fatigue, cognitive issues, palpitations, and musculoskeletal pain for months or years. Estimates cited in new research suggest 4%–20% of infected... Read more
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read moreMicrobiology
view channel
Gut Microbiome Signatures Help Identify Risk of IBD Progression
Inflammatory bowel disease (IBD), encompassing Crohn’s disease and ulcerative colitis, is a chronic relapsing inflammatory disorder of the gastrointestinal tract with highly variable outcomes.... Read more
FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
Clinical guidelines support testing based on patient presentation in suspected gastrointestinal infections, yet available technologies have often forced laboratories to choose between panels that are too... Read morePathology
view channel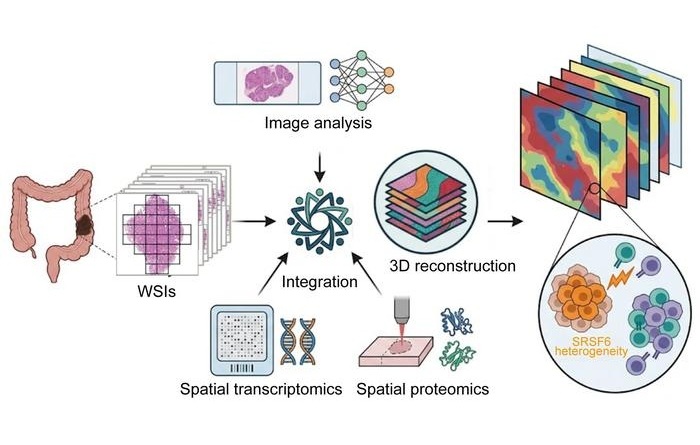
3D Spatial Multi-Omics Maps Intra-Tumor Diversity in Colorectal Cancer
Colorectal cancer remains a leading cause of cancer death, and clinical decision-making is complicated by marked intra-tumor heterogeneity. Conventional bulk sequencing averages molecular signals across... Read more
Blood-Based Method Tracks Gene Activity in the Living Brain
Real-time measurement of gene activity in the brain has been limited by assays requiring destructive tissue sampling. Tracking active genes could reveal how the body responds to environmental factors,... Read moreTechnology
view channel
AI Platform Links Biomarker Results to Cancer Clinical Trials and Guidelines
Oncology teams must manage growing volumes of genomic data, rapidly evolving clinical trial options, and frequently updated care guidelines, all within tight clinic schedules. Translating complex tumor... Read more
Agentic AI Platform Supports Genomic Decision-Making in Oncology
Oncology care teams increasingly face the challenge of managing complex molecular diagnostics, evolving treatment options, and extensive electronic health record documentation. Translating multimodal data... Read moreIndustry
view channel