Depressing Stress Signaling Increases Immune Activity
|
By LabMedica International staff writers Posted on 12 Sep 2017 |
Image: A ribbon model of the beta-2 adrenergic receptor (Photo courtesy of Wikimedia Commons).
Cancer researchers evaluating the immune status of the tumor microenvironment found that CD8+ T-cell frequency and functional orientation were regulated by beta-2-adrenergic receptor (beta-AR) signaling and suggested using clinically available beta-blockers in patients to improve responses to immunotherapy.
Anticancer therapies designed to block “checkpoints” within the immune system do not work for all patients, and their efficacy in controlling tumors is often short-lived. To better understand these phenomena and to improve the performance of check point inhibitors, investigators at Roswell Park Cancer Institute (Buffalo, NY, USA) used three strategies: physiologic (manipulation of ambient thermal environment), pharmacologic (beta-blockers), and genetic (beta-2-adrenergic receptor knockout mice) to reduce adrenergic stress signaling in two widely studied preclinical mouse tumor models.
They reported in the August 17, 2017, online edition of the journal Cancer Research that reducing beta-AR signaling facilitated conversion of tumors to an immunologically active tumor microenvironment. This immunologically enriched microenvironment displayed increased frequency of CD8+ T-cells with an effector phenotype and decreased expression of PD-1, in addition to an elevated effector CD8+ T-cell to CD4+ regulatory T-cell ratio. Moreover, this conversion significantly increased the efficacy of anti-PD-1 checkpoint blockade.
In short, manipulating beta-adrenergic receptor signaling to regulate the immune status of the tumor microenvironment supported the strategic use of clinically available beta-blockers in patients to improve responses to immunotherapy.
“Our bodies respond to certain types of stress - such as fear and anxiety, heat, cold, pain, depression, and even attack by cancer cells - in the same way. We jump into "fight or flight" mode, and the sympathetic nervous system dials up the release of norepinephrine,” said senior author Dr. Elizabeth Repasky, professor of immunology at Roswell Park Cancer Institute. “For reasons that we do not entirely understand yet, prolonged exposure to these stressors often makes our immune cells much less effective. But we demonstrate here that beta blockers, by reducing adrenergic signaling, allow anti-tumor immune cells to become much stronger, and give immunotherapies, and in particular checkpoint inhibitors, a much better chance to work.”
Related Links:
Roswell Park Cancer Institute
Anticancer therapies designed to block “checkpoints” within the immune system do not work for all patients, and their efficacy in controlling tumors is often short-lived. To better understand these phenomena and to improve the performance of check point inhibitors, investigators at Roswell Park Cancer Institute (Buffalo, NY, USA) used three strategies: physiologic (manipulation of ambient thermal environment), pharmacologic (beta-blockers), and genetic (beta-2-adrenergic receptor knockout mice) to reduce adrenergic stress signaling in two widely studied preclinical mouse tumor models.
They reported in the August 17, 2017, online edition of the journal Cancer Research that reducing beta-AR signaling facilitated conversion of tumors to an immunologically active tumor microenvironment. This immunologically enriched microenvironment displayed increased frequency of CD8+ T-cells with an effector phenotype and decreased expression of PD-1, in addition to an elevated effector CD8+ T-cell to CD4+ regulatory T-cell ratio. Moreover, this conversion significantly increased the efficacy of anti-PD-1 checkpoint blockade.
In short, manipulating beta-adrenergic receptor signaling to regulate the immune status of the tumor microenvironment supported the strategic use of clinically available beta-blockers in patients to improve responses to immunotherapy.
“Our bodies respond to certain types of stress - such as fear and anxiety, heat, cold, pain, depression, and even attack by cancer cells - in the same way. We jump into "fight or flight" mode, and the sympathetic nervous system dials up the release of norepinephrine,” said senior author Dr. Elizabeth Repasky, professor of immunology at Roswell Park Cancer Institute. “For reasons that we do not entirely understand yet, prolonged exposure to these stressors often makes our immune cells much less effective. But we demonstrate here that beta blockers, by reducing adrenergic signaling, allow anti-tumor immune cells to become much stronger, and give immunotherapies, and in particular checkpoint inhibitors, a much better chance to work.”
Related Links:
Roswell Park Cancer Institute
Latest BioResearch News
- Lung Cancer Study Reveals Cellular Program Behind Therapy Resistance
- Tumor Genome Marker May Predict Treatment Benefit in Pediatric Cancers
- Lysosomal Gene Defect Linked to Severe Childhood Brain Disorders
- Genetic Testing Identifies Greater Inherited Sudden Cardiac Arrest Risk in Younger Individuals
- Hidden 'Jumping Gene' Variant Linked to Higher Pancreatic Cancer Risk
- Common White Blood Cells Produce Schizophrenia-Linked Protein
- Nanopore Method Captures RNA Folding at Single-Molecule Resolution
- Tumor Microenvironment Marker Linked to Worse Survival in Solid Tumors
- Hidden Immune Gene Defect May Explain Kaposi Sarcoma Susceptibility
- Genetic Markers May Help Predict Amputation Risk in Peripheral Artery Disease
- Gene Signature Shows Promise for Depression Biomarker Testing
- AI-Driven Tumor Profiling Initiative Targets Precision Therapy Development
- Researchers Map Protein and Glycosylation Across 15 Human Body Fluids
- Telomere Length Abnormalities Linked to Lymphoma Development
- Biomarker Signals Chemotherapy Resistance in Relapsed Small Cell Lung Cancer
- Inflammatory Gene Signature Links Metabolic Disease to Pancreatic Cancer Recurrence
Channels
Clinical Chemistry
view channel
Urinary Biomarker Assay Predicts Kidney Disease Progression Beyond Standard Measures
Many patients with type 2 diabetes and chronic kidney disease continue to experience progressive renal decline, yet conventional markers such as albuminuria and estimated glomerular filtration rate (eGFR)... Read more
Saliva-Based Test Detects Biochemical Signs of Sleep Loss
Acute sleep loss impairs cognition and motor skills, raising safety risks that resemble alcohol intoxication. Clinicians currently lack an objective biochemical test to determine when someone is dangerously... Read more
Simple Dual-Tau Blood Test Detects and Stages Alzheimer’s Disease
Alzheimer’s disease is typically confirmed and staged with positron emission tomography scans and cerebrospinal fluid testing, procedures that are costly and invasive. Broader access to minimally invasive... Read more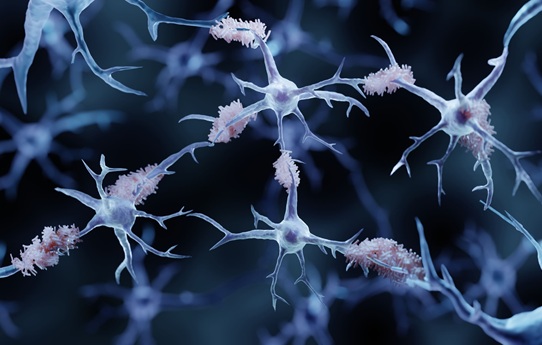
Alzheimer’s Blood Biomarkers Linked to Early Cognitive Differences Before Dementia
Blood-based screening for Alzheimer’s disease offers a noninvasive, lower-cost alternative to brain imaging or spinal fluid testing, yet its ability to flag the earliest cognitive changes has been unclear.... Read moreMolecular Diagnostics
view channel
Blood-Based RNA Test May Predict Chemotherapy Sensitivity in Lung Cancer
Lung cancer care increasingly relies on biomarker-guided patient stratification, but tissue biopsy can be impractical and treatment selection remains difficult for many patients. Blood-based assays that... Read more
Blood Test Predicts Immunotherapy Response in Head and Neck Cancer
Head and neck squamous cell carcinoma affects hundreds of thousands of people worldwide each year, yet response rates to immunotherapy remain low. Clinicians lack reliable, minimally invasive tools to... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channelAptamer-Based Biosensor Enables Mutation-Resilient SARS-CoV-2 Detection
Rapid evolution of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can undermine existing molecular diagnostics, especially when assays target small viral components. Double-antibody sandwich... Read more
Study Points to Autoimmune Pathway Behind Long COVID Symptoms
Long COVID leaves many SARS-CoV-2 survivors with persistent fatigue, cognitive issues, palpitations, and musculoskeletal pain for months or years. Estimates cited in new research suggest 4%–20% of infected... Read more
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read moreMicrobiology
view channel
New Culture Medium Speeds C. difficile Resistance Detection and Reduces Costs
Clostridioides difficile infections remain a persistent threat in hospitals and communities, affecting about 500,000 people in the United States each year. Severe cases can be fatal within 30 days of diagnosis,... Read more
Automated Blood Culture System Speeds Detection of Bloodstream Infections
Bloodstream infections and sepsis require rapid laboratory detection to guide targeted antimicrobial therapy and reduce mortality. Conventional blood culture workflows can delay actionable results by critical... Read morePathology
view channel
AI Pathology Tool Predicts Meningioma Recurrence from Routine Slides
Meningiomas are the most common primary brain tumors in adults, yet their course ranges from indolent to highly recurrent disease. Estimating an individual patient’s recurrence risk often requires advanced... Read more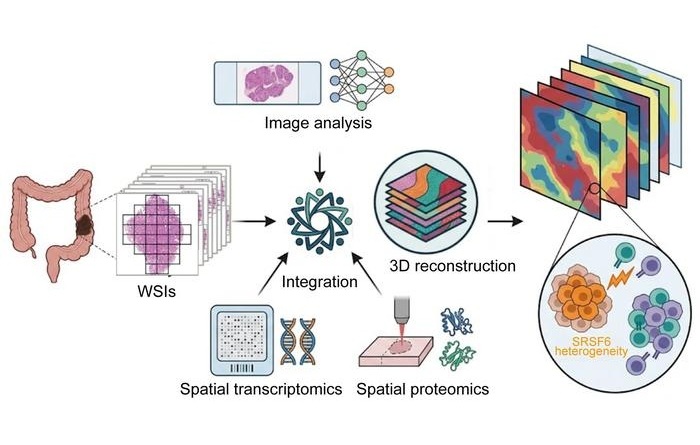
3D Spatial Multi-Omics Maps Intra-Tumor Diversity in Colorectal Cancer
Colorectal cancer remains a leading cause of cancer death, and clinical decision-making is complicated by marked intra-tumor heterogeneity. Conventional bulk sequencing averages molecular signals across... Read moreTechnology
view channel
AI Platform Links Biomarker Results to Cancer Clinical Trials and Guidelines
Oncology teams must manage growing volumes of genomic data, rapidly evolving clinical trial options, and frequently updated care guidelines, all within tight clinic schedules. Translating complex tumor... Read more
Agentic AI Platform Supports Genomic Decision-Making in Oncology
Oncology care teams increasingly face the challenge of managing complex molecular diagnostics, evolving treatment options, and extensive electronic health record documentation. Translating multimodal data... Read moreIndustry
view channel
Genetic Testing Program Expands Detection of Alpha-1 Antitrypsin Deficiency
Alpha-1 Antitrypsin Deficiency (AATD) is a progressive genetic condition, the leading known genetic risk factor for chronic obstructive pulmonary disease (COPD), and a cause of liver disease in both children... Read more




.jpg)