Prostate Cancer Detected in Blood Using Flow Cytometry
|
By LabMedica International staff writers Posted on 22 Feb 2016 |

Image: The Apogee Flow Cytometer used for detecting microparticles of prostate cancer (Photo courtesy of Schulich School of Medicine and Dentistry).
Current methods of detecting prostate cancer, such as the prostate-specific antigen (PSA) test and biopsies, have limitations. PSA tests are based on measuring a specific protein released by the prostate gland, but do not provide a definitive diagnosis.
A physical exam and biopsy are needed if PSA levels are elevated; however, even the painful biopsy procedure has a 15% error rate. During biopsies, a painful and invasive procedure, 12 needles are inserted into the rectum, with the hope of extracting material from an area with a tumor.
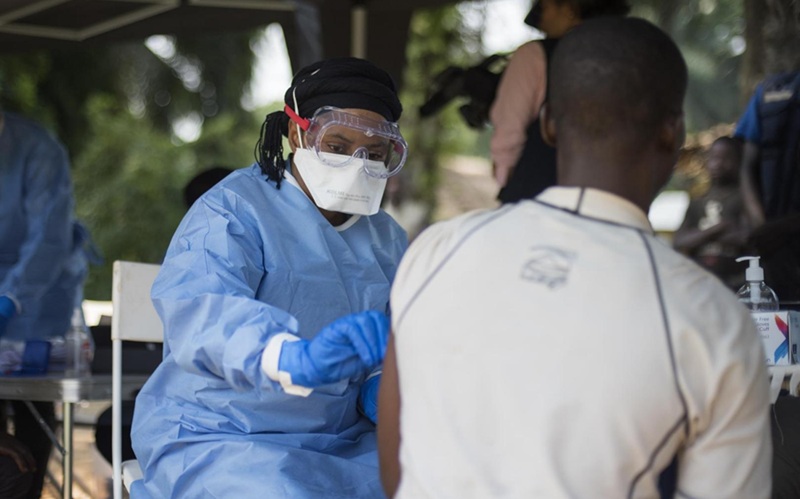
A team of scientists at the Western University's Schulich School of Medicine and Dentistry (London, ON, Canada) and at Lawson Health Research Institute (London, ON, Canada) have repurposed a machine once used to detect airborne pathogens in the second Gulf War. The machine is now used for fluid biopsies, a noninvasive way to detect prostate microparticles in the blood in a matter of minutes. Microparticles are essentially refuse released by prostate cells that circulate throughout the bloodstream.
The machine was used in the Gulf War, and more commonly to test water purity and the machine uses flow cytometry (Apogee Flow Systems; Hemel Hempstead, UK) to detect microparticles. Flow cytometry measures the specific characteristics of a fluid, such as blood, as it passes through a laser. Most men, who are more than 40 years old, regardless of their health, have detectable levels of prostate microparticles in their bloodstream. The scientists have conducted the first clinical cancer project to correlate the number of microparticles in the blood to the risk of having prostate cancer in that the more microparticles, the higher the risk.
The study provides a more accurate and less invasive testing method for patients suspected of having prostate cancer, and helps to identify patients who are at a higher risk of dying from prostate cancer. Hon Leong, PhD, an assistant professor and team leader, said, “Our findings point to a new direction in how we can better identify patients who actually have prostate cancer. With this test, we can improve the clinical outcomes for patients, reducing costs for unnecessary procedures and reducing errors in diagnosis.”
Related Links:
Western University's Schulich School of Medicine and Dentistry
Lawson Health Research Institute
Apogee Flow Systems
A physical exam and biopsy are needed if PSA levels are elevated; however, even the painful biopsy procedure has a 15% error rate. During biopsies, a painful and invasive procedure, 12 needles are inserted into the rectum, with the hope of extracting material from an area with a tumor.
A team of scientists at the Western University's Schulich School of Medicine and Dentistry (London, ON, Canada) and at Lawson Health Research Institute (London, ON, Canada) have repurposed a machine once used to detect airborne pathogens in the second Gulf War. The machine is now used for fluid biopsies, a noninvasive way to detect prostate microparticles in the blood in a matter of minutes. Microparticles are essentially refuse released by prostate cells that circulate throughout the bloodstream.
The machine was used in the Gulf War, and more commonly to test water purity and the machine uses flow cytometry (Apogee Flow Systems; Hemel Hempstead, UK) to detect microparticles. Flow cytometry measures the specific characteristics of a fluid, such as blood, as it passes through a laser. Most men, who are more than 40 years old, regardless of their health, have detectable levels of prostate microparticles in their bloodstream. The scientists have conducted the first clinical cancer project to correlate the number of microparticles in the blood to the risk of having prostate cancer in that the more microparticles, the higher the risk.
The study provides a more accurate and less invasive testing method for patients suspected of having prostate cancer, and helps to identify patients who are at a higher risk of dying from prostate cancer. Hon Leong, PhD, an assistant professor and team leader, said, “Our findings point to a new direction in how we can better identify patients who actually have prostate cancer. With this test, we can improve the clinical outcomes for patients, reducing costs for unnecessary procedures and reducing errors in diagnosis.”
Related Links:
Western University's Schulich School of Medicine and Dentistry
Lawson Health Research Institute
Apogee Flow Systems
Latest Technology News
- Algorithm Panel Aids Liver Fibrosis Assessment and Liver Cancer Surveillance
- Mailed Screening Kits Help Reduce Colorectal Cancer Screening Gaps
- AI-Enabled Assistant Unifies Molecular Workflow Planning and Support
- AI Tool Automates Validation of Laboratory Software Configuration Changes
- Point-of-Care Testing Enhances Health Literacy and Self-Management in Chronic Disease
- Fully Automated Sample-to-Insight Workflow Advances Latent TB Testing
- Tumor-on-a-Chip Platform Models Pancreatic Cancer Treatment Response
- New Platform Captures Extracellular Vesicles for Early Cancer Detection
- Microfluidic Single-Cell Assay Predicts Breast Cancer Risk
- AI Tool Predicts Non-Response to Targeted Therapy in Colorectal Cancer
- Integrated System Streamlines Pre-Analytical Workflow for Molecular Testing
- Noninvasive Sputum Test Detects Early Lung Cancer
- New AI Tool Enables Rapid Treatment Selection in Pediatric Leukemia
- Rapid Biosensor Detects Drug Sensitivity in Breast Tumors
- Breakthrough Mass Spectrometry Design Could Enable Ultra-Low Abundance Detection
- Online Tool Supports Family Screening for Inherited Cancer Risk
Channels
Clinical Chemistry
view channel
Urine-Based Test Shows Promise for Autism Screening in Children
Autism spectrum disorder (ASD) is commonly diagnosed through behavioral assessments, which can involve long waits that delay intervention. Earlier identification is linked to better developmental outcomes,... Read more
Liquid Biopsy Biomarkers May Improve Childhood Epilepsy Diagnosis
Childhood epilepsy remains a major neurological disorder with unmet needs for accurate, non-invasive biomarkers, as conventional tests such as electroencephalography and neuroimaging can have limited sensitivity... Read moreMolecular Diagnostics
view channel
Updated Guidance Prioritizes Stool-Based Colorectal Cancer Screening Tests
Colorectal cancer is the second-leading cause of cancer death in the United States and claimed an estimated 55,000 lives in 2026. Incidence is rising among adults younger than 50, even as overall mortality... Read more
Digital PCR Assays Support Surveillance of Bundibugyo Ebolavirus Outbreak
QIAGEN (Venlo, Netherlands) has introduced two custom-designed research-use-only (RUO) QIAcuity dPCR assays to support infectious disease research and surveillance connected to the Bundibugyo ebolavirus outbreak.... Read more
Blood-Based Proteomic Test May Predict Treatment Response in Non-Small Cell Lung Cancer
Lung cancer remains the leading cause of cancer death, with non-small cell lung cancer (NSCLC) accounting for most cases. Treatment decisions are often made without a clear indication of how a patient... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channel
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read more
Immune Enzyme Linked to Treatment-Resistant Inflammatory Bowel Disease
Inflammatory bowel disease (IBD) affects nearly 3 million people in the United States and its prevalence continues to rise. Medications that target tumor necrosis factor (TNF)-alpha are widely used, but... Read moreMicrobiology
view channel
Gut Microbiome Signatures Help Identify Risk of IBD Progression
Inflammatory bowel disease (IBD), encompassing Crohn’s disease and ulcerative colitis, is a chronic relapsing inflammatory disorder of the gastrointestinal tract with highly variable outcomes.... Read more
FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
Clinical guidelines support testing based on patient presentation in suspected gastrointestinal infections, yet available technologies have often forced laboratories to choose between panels that are too... Read morePathology
view channel
AI-Powered Atlas Maps Immune Structures Linked to Cancer Outcomes
Tertiary lymphoid structures are emerging as important indicators of antitumor immunity, but their heterogeneity and spatial context within tumors remain difficult to capture through routine diagnostics.... Read more
AI Tool Extracts Immune Signals from Biopsy to Inform Myeloma Therapy
Multiple myeloma is a bone marrow malignancy in which patients can respond very differently to the same treatments, making initial therapy decisions difficult. Clinicians must choose among options such... Read moreIndustry
view channelWerfen and Oxford Nanopore Collaborate on Transplant Assay Development
Werfen (Barcelona, Spain), a global specialized diagnostics company, has announced a strategic collaboration with Oxford Nanopore Technologies (Oxford, UK), which develops nanopore-based sequencing technology,... Read more