A Potential Point-of-Care Method for the Diagnosis of Sepsis
|
By LabMedica International staff writers Posted on 21 Nov 2019 |
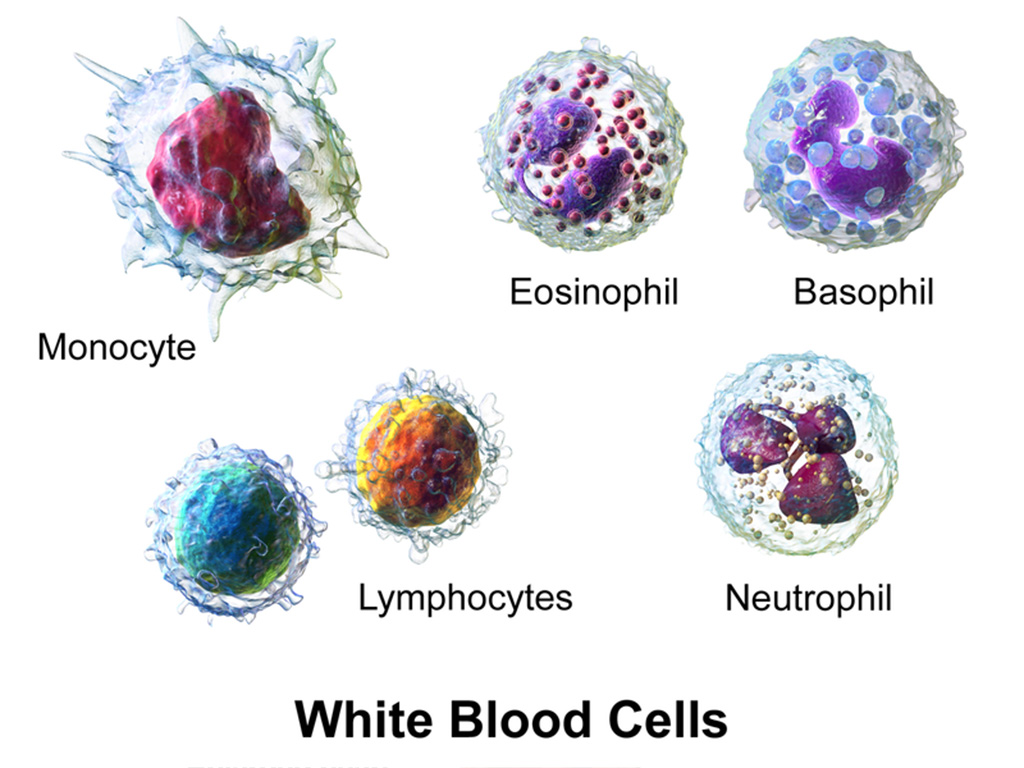
Image: Three-dimensional rendering of various types of white blood cells (Photo courtesy of Wikimedia Commons)
As part of the effort to create better methods to detect and treat sepsis, researchers developed a technique that enables measurement of the activation and function of white blood cells.
Sepsis is caused by an inflammatory immune response triggered by an infection. It is a life-threatening condition that arises when the body's response to infection causes injury to its own tissues and organs. Common signs and symptoms include fever, increased heart rate, increased breathing rate, and confusion. There may also be symptoms related to a specific infection, such as a cough with pneumonia, or painful urination with a kidney infection. In the very young, old, and people with a weakened immune system, there may be no symptoms of a specific infection and the body temperature may be low or normal, rather than high.
Current testing and diagnostic approaches fail to provide the precise and timely information needed to treat sepsis. To correct this, investigators at Brigham and Women's Hospital (Boston, MA, USA) designed a new method, based on microfluidics, which relies on minute channels to separate 50 microliter samples of peripheral blood into fractions comprising either the larger white blood cells or the smaller red blood cells and other elements of the blood.
The size-based microfluidic method was combined with novel isodielectric separation technology - developed by colleagues at the Massachusetts Institute of Technology (Cambridge, MA) - which measured cellular electrical activity. This method detected changes that occurred when white blood cells became activated and could distinguish patients with and without inflammation, such as in sepsis.
The investigators used the system to assess leukocyte phenotype and function over a period of seven days in serial samples from 18 hospitalized patients with sepsis and 10 healthy subjects.
Results revealed that the sepsis samples had significantly higher levels of CD16dim and CD16− neutrophils and CD16+ “intermediate” monocytes, as well as significantly lower levels of neutrophil-elastase release, O2 production, and phagolysosome formation. Repeated sampling of sepsis patients over seven days showed that leukocyte activation (measured by isodielectric separation) and leukocyte phenotype and function were significantly more predictive of the clinical course than complete-blood-count parameters.
"Our idea was to develop a point-of-care diagnostic test that, instead of focusing on the white blood cell count, would inform us about white blood cell activation state and function," said senior author Dr. Bruce Levy, chief of the division of pulmonary and critical care medicine at Brigham and Women's Hospital. "It has been exciting for us, as translational scientists, to work on a solution with outstanding bioengineer colleagues. Together, we are able to address a truly important clinical problem."
The potential use of the leukocyte function test to diagnose sepsis was described in the November 11, 2019, online edition of the journal Nature Biomedical Engineering.
Related Links:
Brigham and Women's Hospital
Massachusetts Institute of Technology
Sepsis is caused by an inflammatory immune response triggered by an infection. It is a life-threatening condition that arises when the body's response to infection causes injury to its own tissues and organs. Common signs and symptoms include fever, increased heart rate, increased breathing rate, and confusion. There may also be symptoms related to a specific infection, such as a cough with pneumonia, or painful urination with a kidney infection. In the very young, old, and people with a weakened immune system, there may be no symptoms of a specific infection and the body temperature may be low or normal, rather than high.
Current testing and diagnostic approaches fail to provide the precise and timely information needed to treat sepsis. To correct this, investigators at Brigham and Women's Hospital (Boston, MA, USA) designed a new method, based on microfluidics, which relies on minute channels to separate 50 microliter samples of peripheral blood into fractions comprising either the larger white blood cells or the smaller red blood cells and other elements of the blood.
The size-based microfluidic method was combined with novel isodielectric separation technology - developed by colleagues at the Massachusetts Institute of Technology (Cambridge, MA) - which measured cellular electrical activity. This method detected changes that occurred when white blood cells became activated and could distinguish patients with and without inflammation, such as in sepsis.
The investigators used the system to assess leukocyte phenotype and function over a period of seven days in serial samples from 18 hospitalized patients with sepsis and 10 healthy subjects.
Results revealed that the sepsis samples had significantly higher levels of CD16dim and CD16− neutrophils and CD16+ “intermediate” monocytes, as well as significantly lower levels of neutrophil-elastase release, O2 production, and phagolysosome formation. Repeated sampling of sepsis patients over seven days showed that leukocyte activation (measured by isodielectric separation) and leukocyte phenotype and function were significantly more predictive of the clinical course than complete-blood-count parameters.
"Our idea was to develop a point-of-care diagnostic test that, instead of focusing on the white blood cell count, would inform us about white blood cell activation state and function," said senior author Dr. Bruce Levy, chief of the division of pulmonary and critical care medicine at Brigham and Women's Hospital. "It has been exciting for us, as translational scientists, to work on a solution with outstanding bioengineer colleagues. Together, we are able to address a truly important clinical problem."
The potential use of the leukocyte function test to diagnose sepsis was described in the November 11, 2019, online edition of the journal Nature Biomedical Engineering.
Related Links:
Brigham and Women's Hospital
Massachusetts Institute of Technology
Latest Molecular Diagnostics News
- Plasma Protein Signature Predicts Lung Cancer Risk Up to Five Years Ahead
- Circulating Tumor DNA Testing Guides Chemotherapy, Reduces Relapse in Colon Cancer
- Researchers Uncover Distinct Chromosome Signature in Aggresive ALT Cancers
- Simple Cytogenetic Method Could Improve Classification of ALL Subtypes
- Blood-Based Assay Enables Noninvasive Monitoring of Sarcoma Immunotherapy Response
- Genomic Test Guides Chemotherapy Decisions in Early-Stage Breast Cancer
- Tumor Mutation Marker Helps Refine Lung Cancer Prognosis and Guide Therapy Selection
- Multi-Cancer Test Boosts Detection When Added to Standard Screening
- Blood-Based MRD Monitoring Supports Relapse Prevention in Leukemia
- Genomic Test Predicts Chemotherapy Benefit in Metastatic Prostate Cancer
- Blood Protein Markers Flag Multiple Sclerosis Risk Years Before Diagnosis
- Digital PCR Assays Support Surveillance of Bundibugyo Ebolavirus Outbreak
- Updated Guidance Prioritizes Stool-Based Colorectal Cancer Screening Tests
- Blood-Based Proteomic Test May Predict Treatment Response in Non-Small Cell Lung Cancer
- Position Statements Outline Evidence Standards for Multi-Cancer Detection Tests
- Ultrasensitive MRD Blood Test Detects Early Breast Cancer Recurrence
Channels
Clinical Chemistry
view channel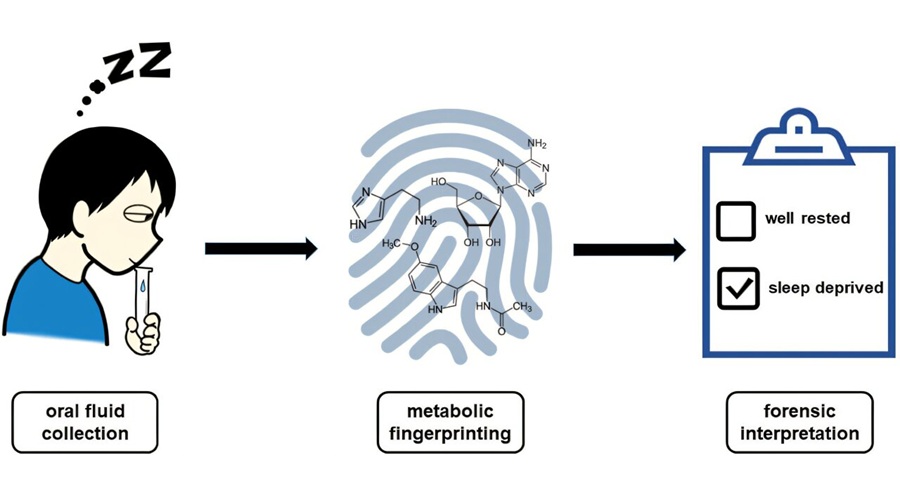
Saliva-Based Test Detects Biochemical Signs of Sleep Loss
Acute sleep loss impairs cognition and motor skills, raising safety risks that resemble alcohol intoxication. Clinicians currently lack an objective biochemical test to determine when someone is dangerously... Read more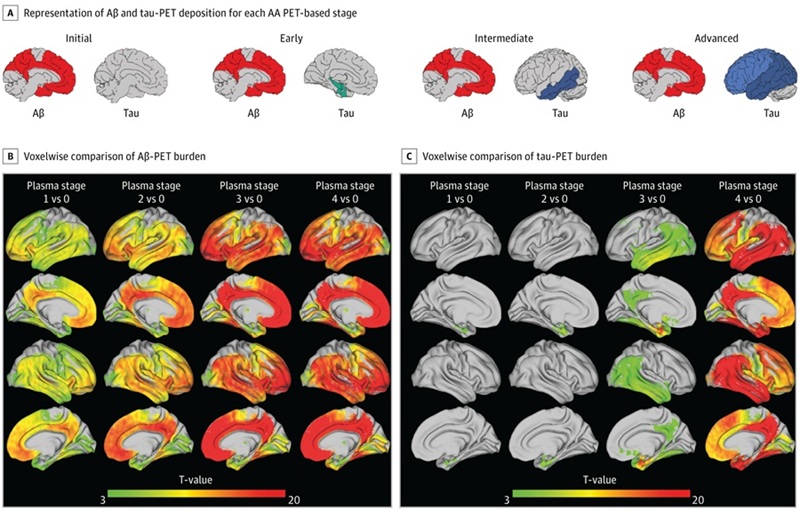
Simple Dual-Tau Blood Test Detects and Stages Alzheimer’s Disease
Alzheimer’s disease is typically confirmed and staged with positron emission tomography scans and cerebrospinal fluid testing, procedures that are costly and invasive. Broader access to minimally invasive... Read more
Alzheimer’s Blood Biomarkers Linked to Early Cognitive Differences Before Dementia
Blood-based screening for Alzheimer’s disease offers a noninvasive, lower-cost alternative to brain imaging or spinal fluid testing, yet its ability to flag the earliest cognitive changes has been unclear.... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channelAptamer-Based Biosensor Enables Mutation-Resilient SARS-CoV-2 Detection
Rapid evolution of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can undermine existing molecular diagnostics, especially when assays target small viral components. Double-antibody sandwich... Read more
Study Points to Autoimmune Pathway Behind Long COVID Symptoms
Long COVID leaves many SARS-CoV-2 survivors with persistent fatigue, cognitive issues, palpitations, and musculoskeletal pain for months or years. Estimates cited in new research suggest 4%–20% of infected... Read more
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read moreMicrobiology
view channel
Gut Microbiome Signatures Help Identify Risk of IBD Progression
Inflammatory bowel disease (IBD), encompassing Crohn’s disease and ulcerative colitis, is a chronic relapsing inflammatory disorder of the gastrointestinal tract with highly variable outcomes.... Read more
FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
Clinical guidelines support testing based on patient presentation in suspected gastrointestinal infections, yet available technologies have often forced laboratories to choose between panels that are too... Read morePathology
view channel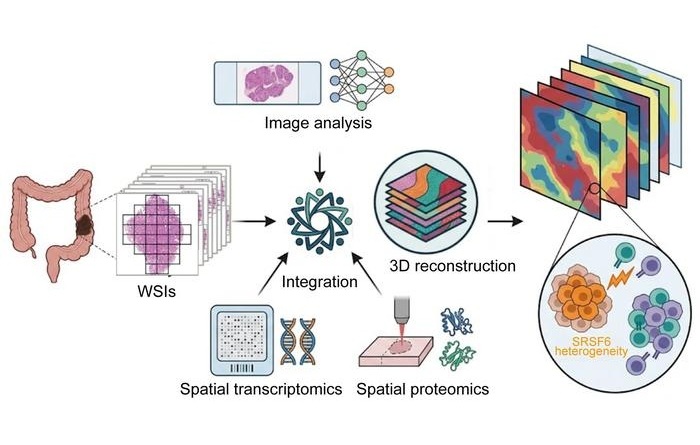
3D Spatial Multi-Omics Maps Intra-Tumor Diversity in Colorectal Cancer
Colorectal cancer remains a leading cause of cancer death, and clinical decision-making is complicated by marked intra-tumor heterogeneity. Conventional bulk sequencing averages molecular signals across... Read more
Blood-Based Method Tracks Gene Activity in the Living Brain
Real-time measurement of gene activity in the brain has been limited by assays requiring destructive tissue sampling. Tracking active genes could reveal how the body responds to environmental factors,... Read moreTechnology
view channel
AI Platform Links Biomarker Results to Cancer Clinical Trials and Guidelines
Oncology teams must manage growing volumes of genomic data, rapidly evolving clinical trial options, and frequently updated care guidelines, all within tight clinic schedules. Translating complex tumor... Read more
Agentic AI Platform Supports Genomic Decision-Making in Oncology
Oncology care teams increasingly face the challenge of managing complex molecular diagnostics, evolving treatment options, and extensive electronic health record documentation. Translating multimodal data... Read moreIndustry
view channel




.jpg)