Serum Magnesium Levels Associated with CAP Mortality
|
By LabMedica International staff writers Posted on 07 Jan 2019 |

Image: The Dimension EXL 200 integrated chemistry system (Photo courtesy of Siemens Healthcare).
Community acquired pneumonia (CAP) is a common illness affecting hundreds of millions worldwide, with increasing hospital admissions throughout the years mainly due to the aging population. It is a major cause of mortality and morbidity in all age groups, especially the elderly.
Magnesium deficiency has been associated with a number of clinical manifestations such as arrhythmias, cardiac insufficiency, sudden death, muscle weakness, bronchospasm, tetany, seizures, as well as hypokalemia, hypocalcaemia, hyponatremia, and hypophosphatemia. Hypermagnesemia may cause severe symptomatic hypotension, bradycardia and ECG changes like wide QRS.
Scientists at the Rambam Health Care Campus (Haifa, Israel) and their colleagues retrospectively reviewed between January 1, 2010, and December 31, 2016, the data of 4,708 patients diagnosed with CAP at discharge; 3,851 patients had magnesium levels within 48 hours, and 55% were males and the median age was 72 years old. Participants were analyzed retrospectively in order to identify the risk factors for a primary endpoint of 30-day mortality.
The Charlson’s comorbidity score was calculated based on data collected; laboratory values (first values within 48 hours): Hemoglobin (Hb), White blood cell count (WBC), red blood cell distribution width (RDW), pH, partial pressure of carbon dioxide (pCO2), serum glucose, serum creatinine, sodium, calcium, phosphorus, magnesium, blood urea nitrogen (BUN), and serum albumin. Hematological values were measured using the Advia 120 Hematology Analyzer. Serum glucose, serum creatinine, sodium, calcium, phosphorus, magnesium, blood urea nitrogen (BUN), and serum albumin were measured on admission using Siemens’ Dimension Integrated Chemistry System; PH, bicarbonate, partial pressure of CO2 and lactate were measured using GEM premier 3500.
The team reported that blood urea nitrogen (BUN) > 20 mg/dL, hypoalbuminemia, and abnormal levels of magnesium were all associated with increased risk of 30-day mortality. Normal magnesium levels were associated with the lowest mortality rate (14.7%). Notably, within the normal levels, high normal magnesium levels (2.0 to 2.4 mg/dL) were correlated with higher mortality rates (30.3%) as compared to levels that ranged between 1.35 to 2 mg/dL (12.9%). Hypomagnesemia and hypermagnesemia were both associated with excess of 30-day mortality, 18.4 and 50%, respectively. Normal levels of magnesium levels in their laboratory vary between 1.35 and 2.4 mg/dL.
The authors concluded that hypomagnesemia and hypermagnesemia on admission were associated with an increased rate of 30-day mortality among adult patients hospitalized with CAP. Interestingly, magnesium levels within the upper normal limits were associated with higher mortality. The study was published on December 27, 2018, in the journal BMC Infectious Diseases.
Related Links:
Rambam Health Care Campus
Magnesium deficiency has been associated with a number of clinical manifestations such as arrhythmias, cardiac insufficiency, sudden death, muscle weakness, bronchospasm, tetany, seizures, as well as hypokalemia, hypocalcaemia, hyponatremia, and hypophosphatemia. Hypermagnesemia may cause severe symptomatic hypotension, bradycardia and ECG changes like wide QRS.
Scientists at the Rambam Health Care Campus (Haifa, Israel) and their colleagues retrospectively reviewed between January 1, 2010, and December 31, 2016, the data of 4,708 patients diagnosed with CAP at discharge; 3,851 patients had magnesium levels within 48 hours, and 55% were males and the median age was 72 years old. Participants were analyzed retrospectively in order to identify the risk factors for a primary endpoint of 30-day mortality.
The Charlson’s comorbidity score was calculated based on data collected; laboratory values (first values within 48 hours): Hemoglobin (Hb), White blood cell count (WBC), red blood cell distribution width (RDW), pH, partial pressure of carbon dioxide (pCO2), serum glucose, serum creatinine, sodium, calcium, phosphorus, magnesium, blood urea nitrogen (BUN), and serum albumin. Hematological values were measured using the Advia 120 Hematology Analyzer. Serum glucose, serum creatinine, sodium, calcium, phosphorus, magnesium, blood urea nitrogen (BUN), and serum albumin were measured on admission using Siemens’ Dimension Integrated Chemistry System; PH, bicarbonate, partial pressure of CO2 and lactate were measured using GEM premier 3500.
The team reported that blood urea nitrogen (BUN) > 20 mg/dL, hypoalbuminemia, and abnormal levels of magnesium were all associated with increased risk of 30-day mortality. Normal magnesium levels were associated with the lowest mortality rate (14.7%). Notably, within the normal levels, high normal magnesium levels (2.0 to 2.4 mg/dL) were correlated with higher mortality rates (30.3%) as compared to levels that ranged between 1.35 to 2 mg/dL (12.9%). Hypomagnesemia and hypermagnesemia were both associated with excess of 30-day mortality, 18.4 and 50%, respectively. Normal levels of magnesium levels in their laboratory vary between 1.35 and 2.4 mg/dL.
The authors concluded that hypomagnesemia and hypermagnesemia on admission were associated with an increased rate of 30-day mortality among adult patients hospitalized with CAP. Interestingly, magnesium levels within the upper normal limits were associated with higher mortality. The study was published on December 27, 2018, in the journal BMC Infectious Diseases.
Related Links:
Rambam Health Care Campus
Latest Microbiology News
- Large-Scale Genomic Surveillance Tracks Resistant Bacteria Across European Hospitals
- Molecular Urine and Stool Tests Do Not Improve Early TB Treatment in Hospitalized HIV Patients
- Rapid Antigen Biosensor Detects Active Tuberculosis in One Hour
- Label-Free Microscopy Method Enables Faster, Quantitative Detection of Malaria
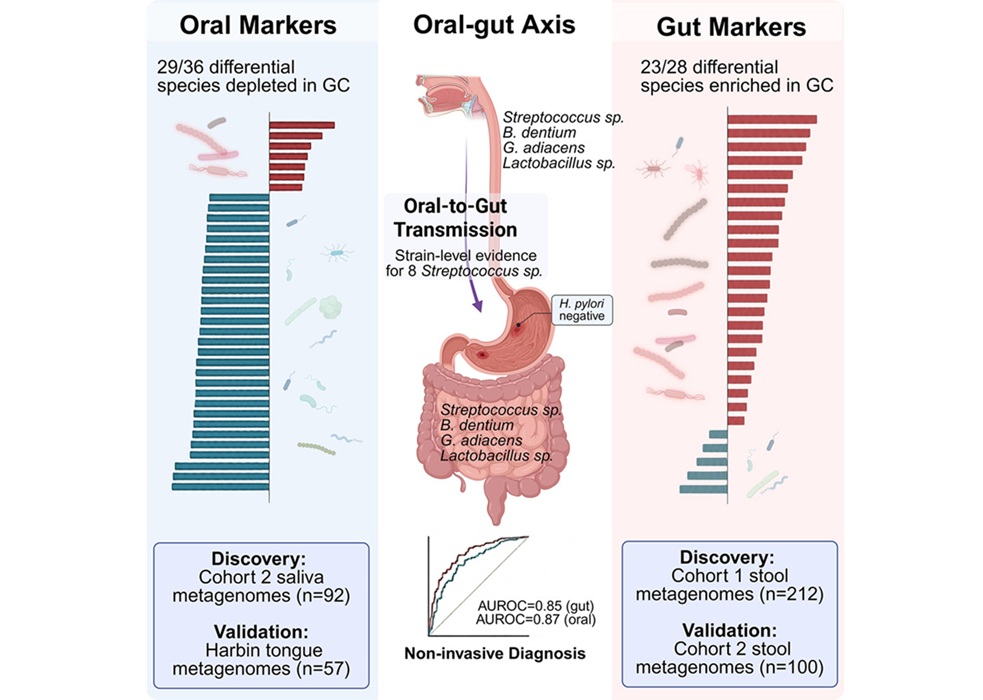
- Oral–Gut Microbiome Signatures Identify Early Gastric Cancer
- Gut Microbiome Test Predicts Melanoma Recurrence After Surgery
- Rapid Blood-Culture Susceptibility Panel Expands Coverage for Gram-Negative Infections
- Antibiotic Resistance Genes Found in Newborns Within Hours of Birth
- Rapid Color Test Stratifies Virulent and Resistant Staph Strains
- mNGS CSF Test Identifies CNS Pathogens Missed by Standard Panels
- Syndromic Panel Enables Rapid Identification of Bloodstream Infections
- RNA-Based Workflow Identifies Active Skin Microbes for Dermatology Research
- Cost-Effective Sampling and Sequencing Workflow Identifies ICU Infection Hotspots
- New Bacterial Target Identified for Early Detection of Noma
- Genomic Analysis Links Emerging Streptococcal Strains to Specific Infections
- Rapid Urine Test Speeds Antibiotic Selection for UTIs
Channels
Molecular Diagnostics
view channel
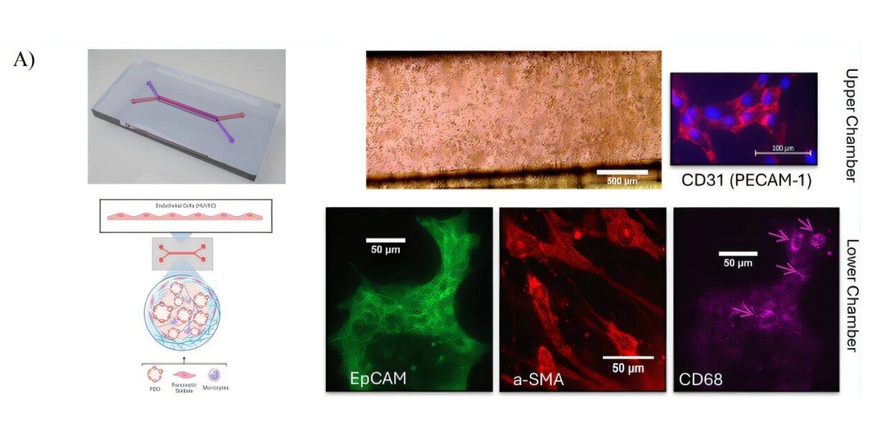
Gene Panel Shows Promise for Predicting Chemotherapy Response in TNBC
Triple-negative breast cancer (TNBC) is an aggressive subtype commonly treated with chemotherapy, yet outcomes vary widely among patients. Understanding the tumor features that drive this variability remains... Read more
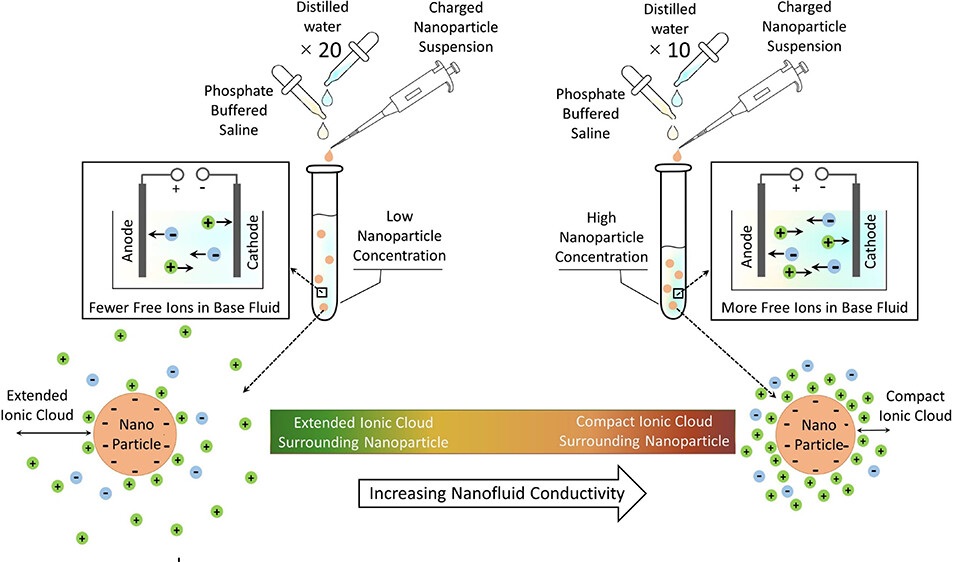
Realistic Mock Samples Aim to Speed Cervical Cancer Test Development
Cervical cancer remains highly preventable, yet screening access is limited in many low- and middle-income settings. Gold-standard tests for high-risk human papillomavirus (HPV) detect viral DNA or messenger... Read more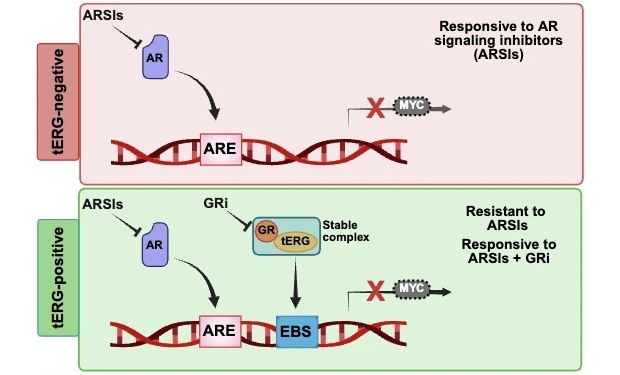
Molecular Marker Identifies Hormone Therapy Resistance Pathway in Prostate Cancer
Most prostate cancers depend on androgen signaling, making hormone suppression or blockade a central treatment strategy. Although many patients respond initially, tumors often adapt and eventually progress,... Read moreHematology
view channel
Stem Cell Biomarkers May Guide Precision Treatment in Acute Myeloid Leukemia
Acute myeloid leukemia (AML) is an aggressive blood cancer that most often affects older adults and still carries a poor prognosis despite therapeutic advances. Venetoclax-based regimens have improved... Read more
Advanced CBC-Derived Indices Integrated into Hematology Platforms
Diatron, a STRATEC brand, has introduced six advanced hematological indices on its Aquila, Aquarius 3, and Abacus 5 hematology analyzers. The new Research Use Only (RUO) indices include Neutrophil-to-Lymphocyte... Read moreImmunology
view channel
Routine TB Screening Test May Reveal Immune Aging and Mortality Risk
Immune aging is associated with weaker responses to vaccination, greater risks of infection, and higher levels of inflammation. Leveraging routinely ordered laboratory tests to quantify that responsiveness... Read more
Biomarkers and Molecular Testing Advance Precision Allergy Care
Allergic diseases often present with similar symptoms but can be driven by distinct biological mechanisms, making standardized care inefficient for many patients. Historically, individuals with pollen... Read moreMicrobiology
view channel
Large-Scale Genomic Surveillance Tracks Resistant Bacteria Across European Hospitals
Antimicrobial resistance (AMR) poses a growing threat to patient safety, with carbapenem-resistant Enterobacterales causing difficult-to-treat infections and leaving clinicians with limited therapeutic options.... Read more
Molecular Urine and Stool Tests Do Not Improve Early TB Treatment in Hospitalized HIV Patients
Tuberculosis is the leading cause of death among people living with HIV, and diagnosis in hospital settings remains difficult. Symptoms are often non-specific, disease can be extrapulmonary, and many patients... Read morePathology
view channel
FDA Clears AI Digital Pathology Tool for Breast Cancer Risk Stratification
Risk assessment at diagnosis is central to guiding therapy for early-stage, hormone receptor-positive, human epidermal growth factor receptor 2-negative (HR+/HER2-) invasive breast cancer, where overtreatment... Read more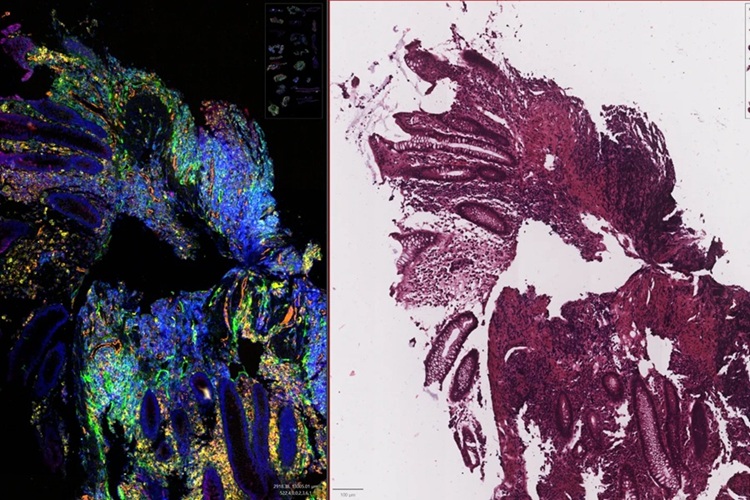
New AI Tool Reveals Hidden Genetic Signals in Routine H&E Slides
Pathologists worldwide rely on hematoxylin and eosin (H&E) slides to examine tissue architecture, yet these stains do not reveal the underlying molecular activity that often drives disease.... Read moreTechnology
view channel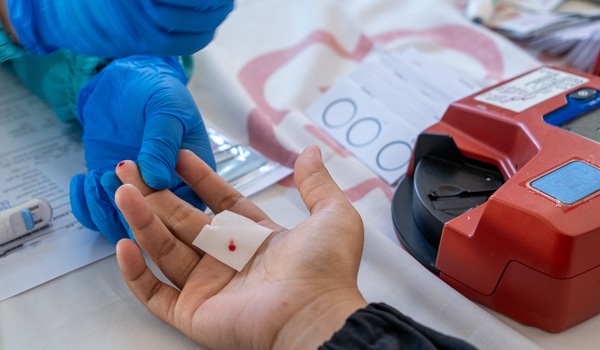
Point-of-Care Testing Enhances Health Literacy and Self-Management in Chronic Disease
Limited access to general practitioners and pathology services can delay diagnosis and monitoring for people in regional and remote communities. Rapid, on-the-spot testing can shorten turnaround times... Read more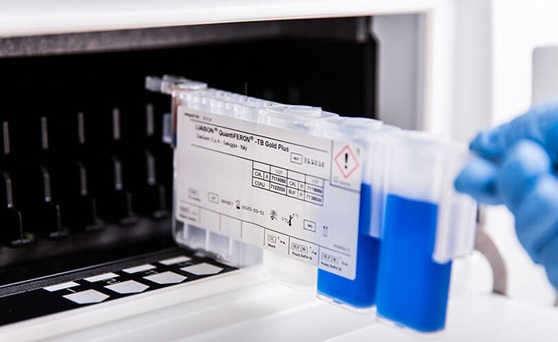
Fully Automated Sample-to-Insight Workflow Advances Latent TB Testing
Latent tuberculosis remains a substantial testing workload for clinical laboratories as screening programs expand. Despite this growth, only about 40% of testing has shifted from traditional skin tests... Read moreIndustry
view channel
Roche to Acquire PathAI for Up to $1.05 Billion to Strengthen AI Diagnostics Portfolio
Roche has entered into a definitive merger agreement to acquire PathAI, a company focused on digital pathology and artificial intelligence for pathology laboratories and the biopharma industry.... Read more