Novel Immunoassay Predicts Risk of Breast Cancer Metastasis
|
By LabMedica International staff writers Posted on 16 Jun 2014 |
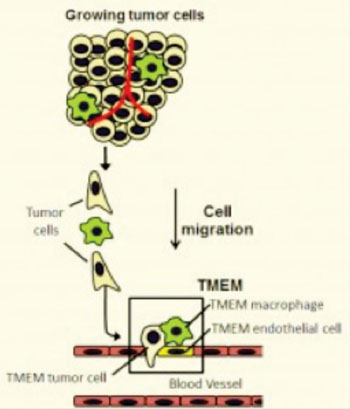
Image: Metastasis requires the presence of three cells in direct contact on a blood vessel wall: a tumor cell that produces the protein MENA; a perivascular macrophage (cells that guide tumor cells to blood vessels); and a blood-vessel endothelial cell. The presence of three such cells in contact with each other is called a tumor microenvironment of metastasis, or TMEM, which is depicted within the box in this illustration (Photo courtesy of Albert Einstein College of Medicine of Yeshiva University).
A novel diagnostic test that identifies sites where breast tumors are able to metastasize was used to predict risk of distant metastasis in ER+/HER2− breast cancer independently of IHC4 score and classical pathologic features.
Primary breast cancers are able to metastasize when three types of cells are present together in the same site: an endothelial cell, a perivascular macrophage, and a tumor cell that produces high levels of Mena, a protein that enhances a cancer cell’s ability to spread. Tumor cells can enter blood vessels at sites where these three cells are in contact. Such a site is referred to as a tumor microenvironment of metastasis, or TMEM.
Investigators at the Albert Einstein College of Medicine (New York, NY, USA) recently developed a test that uses a triple immunostain, which contains antibodies to the three cell types that make up a TMEM. They used this test to evaluate breast tumor specimens from 259 women who later developed a distant metastasis (the cases) and on specimens from women who were alive and had not developed a distant metastasis (the controls). Case patients and control subjects were matched (1:1) on age at and calendar year of primary diagnosis. Results for the TMEM assay were compared to those obtained by the IHC4 method.
IHC4 measures the levels of four key proteins (ER, PR, HER2 and Ki-67) in addition to classical clinical and pathological variables (for example, age, nodal status, tumor size, and grade) and calculates a risk score for distant recurrence using an algorithm. Quantitative assessments of ER, PR, and Ki-67 are needed for the IHC4 test. The test uses formalin-fixed paraffin-embedded samples.
Results showed that TMEM score was significantly associated with increased risk of distant metastasis in estrogen receptor (ER)+/human epidermal growth factor receptor (HER2)− tumors, whereas IHC4 score had only a borderline positive association. Furthermore, the association for TMEM score persisted after adjustment for the IHC4 score. The area under the curve for TMEM, adjusted for clinical variables, was 0.78. Neither TMEM score nor IHC4 score was independently associated with metastatic risk overall or in the triple negative or HER2+ breast tumor subgroups.
“Currently marketed tests assess risk for breast cancer metastasis by looking for changes in gene expression or in levels of proteins associated with growth of tumor cells,” said senior author Dr. Joan Jones, professor of pathology, anatomy, and epidemiology at the Albert Einstein College of Medicine. “But those changes do not reflect the mechanism by which individual tumor cells invade blood vessels, a necessary step for metastasis. By contrast, our test is based on what Einstein researchers learned from intravital imaging, which reveals biological processes deep within the tissues of a living animal. Using this technology, they determined how breast cancer tumor cells spread in rodents.”
The study was published in the August 8, 2014, online edition of the Journal of the National Cancer Institute.
Related Links:
Albert Einstein College of Medicine
Primary breast cancers are able to metastasize when three types of cells are present together in the same site: an endothelial cell, a perivascular macrophage, and a tumor cell that produces high levels of Mena, a protein that enhances a cancer cell’s ability to spread. Tumor cells can enter blood vessels at sites where these three cells are in contact. Such a site is referred to as a tumor microenvironment of metastasis, or TMEM.
Investigators at the Albert Einstein College of Medicine (New York, NY, USA) recently developed a test that uses a triple immunostain, which contains antibodies to the three cell types that make up a TMEM. They used this test to evaluate breast tumor specimens from 259 women who later developed a distant metastasis (the cases) and on specimens from women who were alive and had not developed a distant metastasis (the controls). Case patients and control subjects were matched (1:1) on age at and calendar year of primary diagnosis. Results for the TMEM assay were compared to those obtained by the IHC4 method.
IHC4 measures the levels of four key proteins (ER, PR, HER2 and Ki-67) in addition to classical clinical and pathological variables (for example, age, nodal status, tumor size, and grade) and calculates a risk score for distant recurrence using an algorithm. Quantitative assessments of ER, PR, and Ki-67 are needed for the IHC4 test. The test uses formalin-fixed paraffin-embedded samples.
Results showed that TMEM score was significantly associated with increased risk of distant metastasis in estrogen receptor (ER)+/human epidermal growth factor receptor (HER2)− tumors, whereas IHC4 score had only a borderline positive association. Furthermore, the association for TMEM score persisted after adjustment for the IHC4 score. The area under the curve for TMEM, adjusted for clinical variables, was 0.78. Neither TMEM score nor IHC4 score was independently associated with metastatic risk overall or in the triple negative or HER2+ breast tumor subgroups.
“Currently marketed tests assess risk for breast cancer metastasis by looking for changes in gene expression or in levels of proteins associated with growth of tumor cells,” said senior author Dr. Joan Jones, professor of pathology, anatomy, and epidemiology at the Albert Einstein College of Medicine. “But those changes do not reflect the mechanism by which individual tumor cells invade blood vessels, a necessary step for metastasis. By contrast, our test is based on what Einstein researchers learned from intravital imaging, which reveals biological processes deep within the tissues of a living animal. Using this technology, they determined how breast cancer tumor cells spread in rodents.”
The study was published in the August 8, 2014, online edition of the Journal of the National Cancer Institute.
Related Links:
Albert Einstein College of Medicine
Latest Pathology News
- Engineered Yeast Cells Enable Rapid Testing of Cancer Immunotherapy
- First-Of-Its-Kind Test Identifies Autism Risk at Birth
- AI Algorithms Improve Genetic Mutation Detection in Cancer Diagnostics
- Skin Biopsy Offers New Diagnostic Method for Neurodegenerative Diseases
- Fast Label-Free Method Identifies Aggressive Cancer Cells
- New X-Ray Method Promises Advances in Histology
- Single-Cell Profiling Technique Could Guide Early Cancer Detection
- Intraoperative Tumor Histology to Improve Cancer Surgeries
- Rapid Stool Test Could Help Pinpoint IBD Diagnosis
- AI-Powered Label-Free Optical Imaging Accurately Identifies Thyroid Cancer During Surgery
- Deep Learning–Based Method Improves Cancer Diagnosis
- ADLM Updates Expert Guidance on Urine Drug Testing for Patients in Emergency Departments
- New Age-Based Blood Test Thresholds to Catch Ovarian Cancer Earlier
- Genetics and AI Improve Diagnosis of Aortic Stenosis
- AI Tool Simultaneously Identifies Genetic Mutations and Disease Type
- Rapid Low-Cost Tests Can Prevent Child Deaths from Contaminated Medicinal Syrups
Channels
Clinical Chemistry
view channel
New PSA-Based Prognostic Model Improves Prostate Cancer Risk Assessment
Prostate cancer is the second-leading cause of cancer death among American men, and about one in eight will be diagnosed in their lifetime. Screening relies on blood levels of prostate-specific antigen... Read more
Extracellular Vesicles Linked to Heart Failure Risk in CKD Patients
Chronic kidney disease (CKD) affects more than 1 in 7 Americans and is strongly associated with cardiovascular complications, which account for more than half of deaths among people with CKD.... Read moreMolecular Diagnostics
view channel
Diagnostic Device Predicts Treatment Response for Brain Tumors Via Blood Test
Glioblastoma is one of the deadliest forms of brain cancer, largely because doctors have no reliable way to determine whether treatments are working in real time. Assessing therapeutic response currently... Read more
Blood Test Detects Early-Stage Cancers by Measuring Epigenetic Instability
Early-stage cancers are notoriously difficult to detect because molecular changes are subtle and often missed by existing screening tools. Many liquid biopsies rely on measuring absolute DNA methylation... Read more
“Lab-On-A-Disc” Device Paves Way for More Automated Liquid Biopsies
Extracellular vesicles (EVs) are tiny particles released by cells into the bloodstream that carry molecular information about a cell’s condition, including whether it is cancerous. However, EVs are highly... Read more
Blood Test Identifies Inflammatory Breast Cancer Patients at Increased Risk of Brain Metastasis
Brain metastasis is a frequent and devastating complication in patients with inflammatory breast cancer, an aggressive subtype with limited treatment options. Despite its high incidence, the biological... Read moreHematology
view channel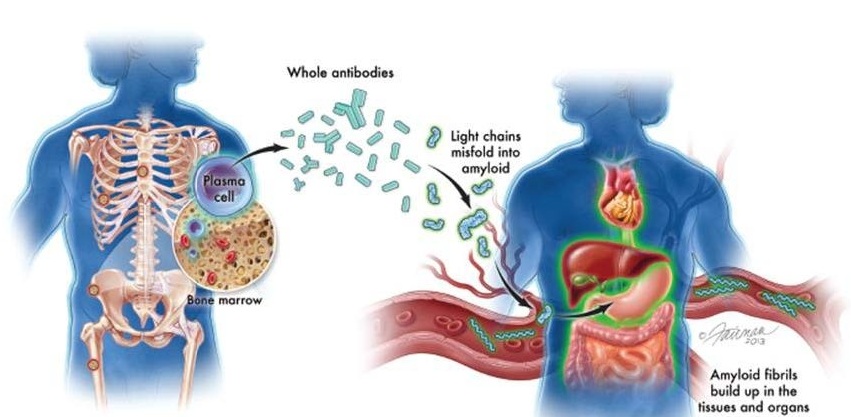
New Guidelines Aim to Improve AL Amyloidosis Diagnosis
Light chain (AL) amyloidosis is a rare, life-threatening bone marrow disorder in which abnormal amyloid proteins accumulate in organs. Approximately 3,260 people in the United States are diagnosed... Read more
Fast and Easy Test Could Revolutionize Blood Transfusions
Blood transfusions are a cornerstone of modern medicine, yet red blood cells can deteriorate quietly while sitting in cold storage for weeks. Although blood units have a fixed expiration date, cells from... Read more
Automated Hemostasis System Helps Labs of All Sizes Optimize Workflow
High-volume hemostasis sections must sustain rapid turnaround while managing reruns and reflex testing. Manual tube handling and preanalytical checks can strain staff time and increase opportunities for error.... Read more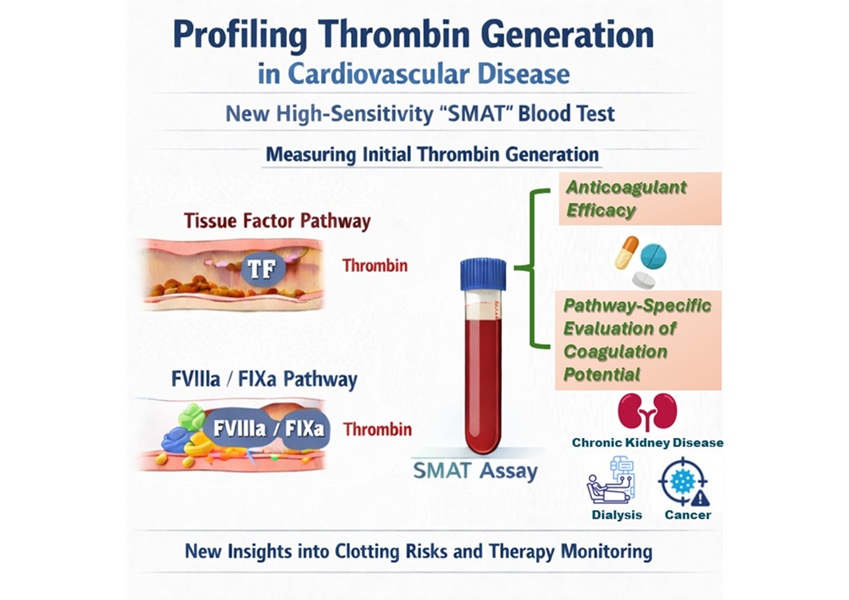
High-Sensitivity Blood Test Improves Assessment of Clotting Risk in Heart Disease Patients
Blood clotting is essential for preventing bleeding, but even small imbalances can lead to serious conditions such as thrombosis or dangerous hemorrhage. In cardiovascular disease, clinicians often struggle... Read moreImmunology
view channelBlood Test Identifies Lung Cancer Patients Who Can Benefit from Immunotherapy Drug
Small cell lung cancer (SCLC) is an aggressive disease with limited treatment options, and even newly approved immunotherapies do not benefit all patients. While immunotherapy can extend survival for some,... Read more
Whole-Genome Sequencing Approach Identifies Cancer Patients Benefitting From PARP-Inhibitor Treatment
Targeted cancer therapies such as PARP inhibitors can be highly effective, but only for patients whose tumors carry specific DNA repair defects. Identifying these patients accurately remains challenging,... Read more
Ultrasensitive Liquid Biopsy Demonstrates Efficacy in Predicting Immunotherapy Response
Immunotherapy has transformed cancer treatment, but only a small proportion of patients experience lasting benefit, with response rates often remaining between 10% and 20%. Clinicians currently lack reliable... Read moreMicrobiology
view channel
Comprehensive Review Identifies Gut Microbiome Signatures Associated With Alzheimer’s Disease
Alzheimer’s disease affects approximately 6.7 million people in the United States and nearly 50 million worldwide, yet early cognitive decline remains difficult to characterize. Increasing evidence suggests... Read moreAI-Powered Platform Enables Rapid Detection of Drug-Resistant C. Auris Pathogens
Infections caused by the pathogenic yeast Candida auris pose a significant threat to hospitalized patients, particularly those with weakened immune systems or those who have invasive medical devices.... Read moreTechnology
view channel
Robotic Technology Unveiled for Automated Diagnostic Blood Draws
Routine diagnostic blood collection is a high‑volume task that can strain staffing and introduce human‑dependent variability, with downstream implications for sample quality and patient experience.... Read more
ADLM Launches First-of-Its-Kind Data Science Program for Laboratory Medicine Professionals
Clinical laboratories generate billions of test results each year, creating a treasure trove of data with the potential to support more personalized testing, improve operational efficiency, and enhance patient care.... Read moreAptamer Biosensor Technology to Transform Virus Detection
Rapid and reliable virus detection is essential for controlling outbreaks, from seasonal influenza to global pandemics such as COVID-19. Conventional diagnostic methods, including cell culture, antigen... Read more
AI Models Could Predict Pre-Eclampsia and Anemia Earlier Using Routine Blood Tests
Pre-eclampsia and anemia are major contributors to maternal and child mortality worldwide, together accounting for more than half a million deaths each year and leaving millions with long-term health complications.... Read moreIndustry
view channelNew Collaboration Brings Automated Mass Spectrometry to Routine Laboratory Testing
Mass spectrometry is a powerful analytical technique that identifies and quantifies molecules based on their mass and electrical charge. Its high selectivity, sensitivity, and accuracy make it indispensable... Read more
AI-Powered Cervical Cancer Test Set for Major Rollout in Latin America
Noul Co., a Korean company specializing in AI-based blood and cancer diagnostics, announced it will supply its intelligence (AI)-based miLab CER cervical cancer diagnostic solution to Mexico under a multi‑year... Read more
Diasorin and Fisher Scientific Enter into US Distribution Agreement for Molecular POC Platform
Diasorin (Saluggia, Italy) has entered into an exclusive distribution agreement with Fisher Scientific, part of Thermo Fisher Scientific (Waltham, MA, USA), for the LIAISON NES molecular point-of-care... Read more