Inflammation Associated with Heart Failure in Rheumatoid Arthritis
|
By LabMedica International staff writers Posted on 28 Oct 2021 |

Image: There is an association between inflammation, incident heart failure, and heart failure subtypes in patients with rheumatoid arthritis (Photo courtesy of Elite Learning)
Heart failure is a major cause of morbidity and mortality in Rheumatoid Arthritis (RA), but data for the subtypes of heart failure, with preserved ejection fraction versus reduced ejection fraction, have been sparse.
The two subtypes of heart failure are thought to differ in pathophysiology. The subtype with reduced ejection fraction is believed to result from ischemic factors, whereas with preserved ejection fraction, the primary driver is considered to be inflammation, reflected by the presence of inflammatory mediators such as interleukin 6 (IL-6) and tumor necrosis factor (TNF)-α.
Rheumatologists at the Brigham and Women’s Hospital (Boston, MA, USA) and their colleagues explored the association with heart failure in RA that could be specific to the subtype with preserved ejection fraction. Heart failure with reduced ejection fraction was defined as an ejection fraction of 40% or less, while preserved ejection fraction was 50% or higher. Those whose ejection fraction was 40%-50% were classified as mid-range and were not considered a specific subtype. Elevated inflammation at the time of RA diagnosis was defined as an erythrocyte sedimentation rate (ESR) of 20-30 mm/h, and/or a C-reactive protein (CRP) of 8-10 mg/L. The analysis included 9,087 RA patients, whose median follow-up was 10.7 years. Three-quarters were women, mean age was 56, and 55% were seropositive.
The scientists reported that the median ESR at baseline was 24.7 mm/h, and median CRP was 5.9 mg/L. Patients whose inflammatory markers were elevated typically were older, female, seropositive, and taking corticosteroids. They also more often had cardiovascular comorbidities such as hypertension, coronary artery disease, and diabetes. During 10 years of follow-up, heart failure was diagnosed in 749 patients, for an incidence rate of 11 per 1,000 person-years. The heart failure developed within five years of RA diagnosis in 379 patients. Ejection fraction was reduced in 127 and preserved in 561; the remainder of patients had mid-range ejection fraction.
In a secondary analysis that considered tertiles of inflammation, higher levels of inflammation were significantly associated with any heart failure at years 5 and 10, and also for the subtype with preserved ejection fraction; however, no association was seen among patients with reduced ejection fraction. Other factors that influenced heart failure risk included lower risks with seropositivity and the use of methotrexate, and higher risk with coronary artery disease, particularly among patients with reduced ejection fraction. That observation supports the concept that ischemia, rather than inflammation, is central to the pathogenesis of the reduced ejection fraction subtype of heart failure. After adjustment for demographics, traditional risk factors for heart failure, and RA disease factors, the hazard ratio for heart failure at 10 years was 1.46 (95% CI 1.13-1.90) among patients with elevated levels of inflammatory markers.
The authors concluded that a sizeable number of patients developed heart failure by five years suggested that evaluations for risk factors for heart failure in RA may need to begin earlier than the usual 10 years Moreover, although this study was conducted in RA patients, the findings also may inform the effect of chronic inflammation on heart failure risk in the general population without RA. The study was published on October 9, 2021 in the journal Arthritis Care & Research.
Related Links:
Brigham and Women’s Hospital
The two subtypes of heart failure are thought to differ in pathophysiology. The subtype with reduced ejection fraction is believed to result from ischemic factors, whereas with preserved ejection fraction, the primary driver is considered to be inflammation, reflected by the presence of inflammatory mediators such as interleukin 6 (IL-6) and tumor necrosis factor (TNF)-α.
Rheumatologists at the Brigham and Women’s Hospital (Boston, MA, USA) and their colleagues explored the association with heart failure in RA that could be specific to the subtype with preserved ejection fraction. Heart failure with reduced ejection fraction was defined as an ejection fraction of 40% or less, while preserved ejection fraction was 50% or higher. Those whose ejection fraction was 40%-50% were classified as mid-range and were not considered a specific subtype. Elevated inflammation at the time of RA diagnosis was defined as an erythrocyte sedimentation rate (ESR) of 20-30 mm/h, and/or a C-reactive protein (CRP) of 8-10 mg/L. The analysis included 9,087 RA patients, whose median follow-up was 10.7 years. Three-quarters were women, mean age was 56, and 55% were seropositive.
The scientists reported that the median ESR at baseline was 24.7 mm/h, and median CRP was 5.9 mg/L. Patients whose inflammatory markers were elevated typically were older, female, seropositive, and taking corticosteroids. They also more often had cardiovascular comorbidities such as hypertension, coronary artery disease, and diabetes. During 10 years of follow-up, heart failure was diagnosed in 749 patients, for an incidence rate of 11 per 1,000 person-years. The heart failure developed within five years of RA diagnosis in 379 patients. Ejection fraction was reduced in 127 and preserved in 561; the remainder of patients had mid-range ejection fraction.
In a secondary analysis that considered tertiles of inflammation, higher levels of inflammation were significantly associated with any heart failure at years 5 and 10, and also for the subtype with preserved ejection fraction; however, no association was seen among patients with reduced ejection fraction. Other factors that influenced heart failure risk included lower risks with seropositivity and the use of methotrexate, and higher risk with coronary artery disease, particularly among patients with reduced ejection fraction. That observation supports the concept that ischemia, rather than inflammation, is central to the pathogenesis of the reduced ejection fraction subtype of heart failure. After adjustment for demographics, traditional risk factors for heart failure, and RA disease factors, the hazard ratio for heart failure at 10 years was 1.46 (95% CI 1.13-1.90) among patients with elevated levels of inflammatory markers.
The authors concluded that a sizeable number of patients developed heart failure by five years suggested that evaluations for risk factors for heart failure in RA may need to begin earlier than the usual 10 years Moreover, although this study was conducted in RA patients, the findings also may inform the effect of chronic inflammation on heart failure risk in the general population without RA. The study was published on October 9, 2021 in the journal Arthritis Care & Research.
Related Links:
Brigham and Women’s Hospital
Latest Pathology News
- AI-Powered Atlas Maps Immune Structures Linked to Cancer Outcomes
- AI Tool Extracts Immune Signals from Biopsy to Inform Myeloma Therapy
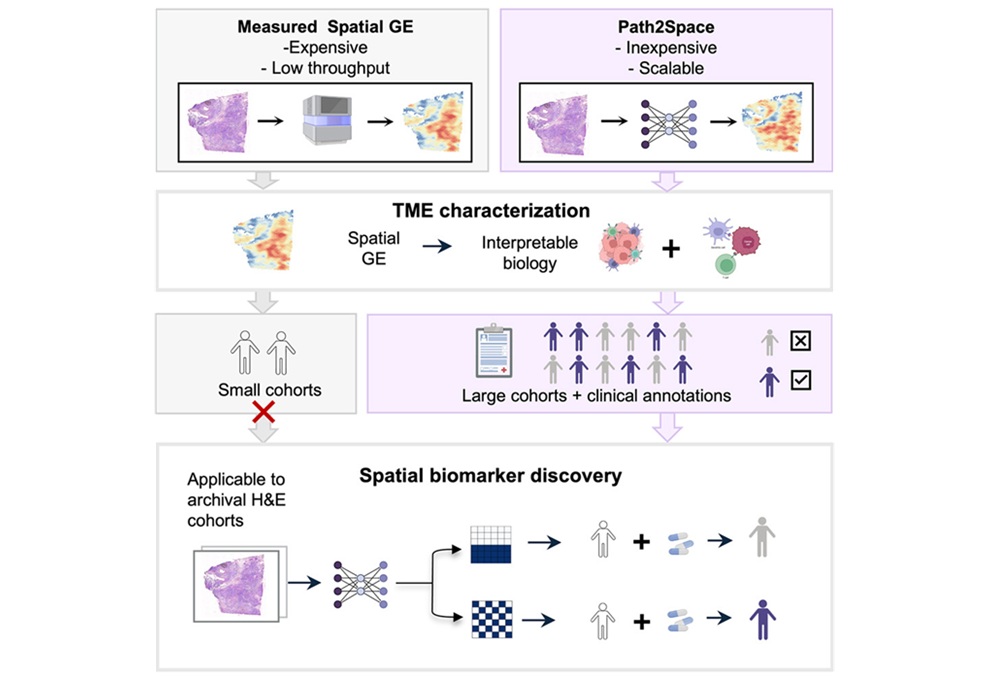
- Rapid AI Tool Predicts Cancer Spatial Gene Expression from Pathology Images
- AI Pathology Test Receives FDA Breakthrough for Bladder Cancer Risk Stratification
- FDA Clears AI Digital Pathology Tool for Breast Cancer Risk Stratification
- New AI Tool Reveals Hidden Genetic Signals in Routine H&E Slides
- AI System Analyzes Routine Pathology Slides to Predict Cancer Outcomes
- New Tissue Mapping Approach Identifies High-Risk Form of Diabetic Kidney Disease
- Multimodal AI Tool Predicts Genetic Alterations to Guide Breast Cancer Treatment
- Interpretable AI Reveals Hidden Cellular Features from Microscopy Images
- Tumor Immune Structure Predicts Response to Immunotherapy in Melanoma
- Plug-and-Play AI Pathology System Classifies Multiple Cancers from Few Slides
- AI-Based Assays Support Risk Stratification in Prostate and Breast Cancer
- AI Pathology Model Predicts Immunotherapy Response in Lung Cancer
- Study Reveals Moleclar Mechanism Driving Aggressive Skin Cancer
- AI Precision Tests Deliver Cancer Risk Insights from Routine H&E Slides
Channels
Clinical Chemistry
view channel
Urine-Based Test Shows Promise for Autism Screening in Children
Autism spectrum disorder (ASD) is commonly diagnosed through behavioral assessments, which can involve long waits that delay intervention. Earlier identification is linked to better developmental outcomes,... Read more
Liquid Biopsy Biomarkers May Improve Childhood Epilepsy Diagnosis
Childhood epilepsy remains a major neurological disorder with unmet needs for accurate, non-invasive biomarkers, as conventional tests such as electroencephalography and neuroimaging can have limited sensitivity... Read moreMolecular Diagnostics
view channel
Blood-Based MRD Monitoring Supports Relapse Prevention in Leukemia
In myelodysplastic syndromes (MDS) and acute myeloid leukemia (AML), molecular blood testing for minimal residual disease (MRD) can detect signs of impending relapse before clinical symptoms emerge.... Read more
Genomic Test Predicts Chemotherapy Benefit in Metastatic Prostate Cancer
Metastatic prostate cancer remains a major treatment challenge, particularly when deciding whether to add chemotherapy to hormonal therapy. In the United States, about 334,000 men are diagnosed with prostate... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreMicrobiology
view channel
Gut Microbiome Signatures Help Identify Risk of IBD Progression
Inflammatory bowel disease (IBD), encompassing Crohn’s disease and ulcerative colitis, is a chronic relapsing inflammatory disorder of the gastrointestinal tract with highly variable outcomes.... Read more
FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
Clinical guidelines support testing based on patient presentation in suspected gastrointestinal infections, yet available technologies have often forced laboratories to choose between panels that are too... Read morePathology
view channel
AI-Powered Atlas Maps Immune Structures Linked to Cancer Outcomes
Tertiary lymphoid structures are emerging as important indicators of antitumor immunity, but their heterogeneity and spatial context within tumors remain difficult to capture through routine diagnostics.... Read more
AI Tool Extracts Immune Signals from Biopsy to Inform Myeloma Therapy
Multiple myeloma is a bone marrow malignancy in which patients can respond very differently to the same treatments, making initial therapy decisions difficult. Clinicians must choose among options such... Read moreTechnology
view channel
AI Platform Links Biomarker Results to Cancer Clinical Trials and Guidelines
Oncology teams must manage growing volumes of genomic data, rapidly evolving clinical trial options, and frequently updated care guidelines, all within tight clinic schedules. Translating complex tumor... Read more
Agentic AI Platform Supports Genomic Decision-Making in Oncology
Oncology care teams increasingly face the challenge of managing complex molecular diagnostics, evolving treatment options, and extensive electronic health record documentation. Translating multimodal data... Read moreIndustry
view channel




.jpg)