HDL-Cholesterol Predicts Survival in Cirrhotic Patients with Gastrointestinal Bleeding
|
By LabMedica International staff writers Posted on 10 Dec 2020 |
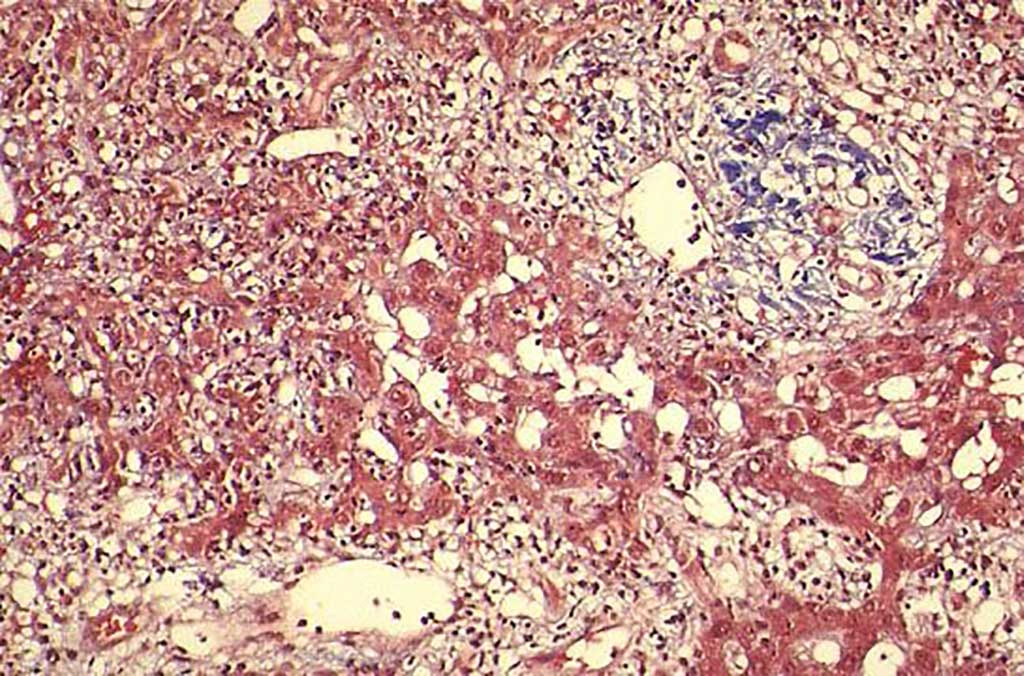
Image: Histopathology of a cirrhotic liver. High-density lipoprotein cholesterol predicts survival in cirrhotic patients with acute gastrointestinal bleeding (Photo courtesy of Loyola University Chicago).
Liver cirrhosis is an important cause of morbidity and mortality as a consequence of continuous liver injuries. Acute gastrointestinal bleeding is a serious complication and critical clinical event in cirrhotic patients. Hepatitis B virus (HBV) is the leading cause of liver cirrhosis in China.
Since the liver plays a crucial role in cholesterol homeostasis, hypercholesterolemia often occurs in patients with chronic liver diseases. The decrease in serum levels of lipids and lipoproteins is highly prevalent in cirrhotic patients, with a prevalence that increases in parallel with the disease severity.
Infectious disease specialists at the Peking University First Hospital (Beijing, China) evaluated from January 2008 to December 2015, consecutive cirrhotic patients with acute gastrointestinal bleeding who were randomly divided into the derivation (n = 629) and validation (n = 314) cohorts. Liver cirrhosis was confirmed either by liver biopsy or by clinical presentations, routine liver function tests and medical imaging techniques. A logistic regression model was established to confirm the association between lipoprotein cholesterol and mortality. Routine biochemical tests were performed in the hospital laboratory. Lipid profiles include triglyceride, cholesterol, high-density lipoprotein cholesterol (HDL-C) and low-density lipoprotein cholesterol (LDL-C).
The investigators reported that on ROC analysis, HDL-C showed excellent diagnostic accuracy for six-week mortality, with an area under the receiver operating characteristic curves (AUROC) of 0.847 (95% CI 0.789–0.905). The best cut-off value of HDL-C was 0.54 mmol/L, with a sensitivity of 85.1% and specificity of 74.2%. The laboratory variables significantly associated with 6-week mortality in the univariate analysis were as follows: hepatocellular carcinoma (HCC), packed red blood cells (PRBC) transfusion, hemoglobin (HGB), total leukocyte count (WBC), alanine aminotransferase (ALT), serum sodium (Na), total bilirubin (TBIL), albumin (ALB), cholesterol, HDL-C, LDL-C, serum creatinine (Scr), international normalized ratio (INR), fibrinogen (FIB). Multivariate logistic regression analyses showed that TBIL, HDL-C, Na, and HGB were independently associated with six-week mortality.
The authors concluded that HDL-C is a potential indicator for the prognosis of patients with cirrhosis and acute gastrointestinal bleeding. The new algorithm based on HDL-C allowed an accurate predictive assessment of 6-week mortality after bleeding attack. The study was published on November 16, 2020 in the journal BMC Gastroenterology.
Related Links:
Peking University First Hospital
Since the liver plays a crucial role in cholesterol homeostasis, hypercholesterolemia often occurs in patients with chronic liver diseases. The decrease in serum levels of lipids and lipoproteins is highly prevalent in cirrhotic patients, with a prevalence that increases in parallel with the disease severity.
Infectious disease specialists at the Peking University First Hospital (Beijing, China) evaluated from January 2008 to December 2015, consecutive cirrhotic patients with acute gastrointestinal bleeding who were randomly divided into the derivation (n = 629) and validation (n = 314) cohorts. Liver cirrhosis was confirmed either by liver biopsy or by clinical presentations, routine liver function tests and medical imaging techniques. A logistic regression model was established to confirm the association between lipoprotein cholesterol and mortality. Routine biochemical tests were performed in the hospital laboratory. Lipid profiles include triglyceride, cholesterol, high-density lipoprotein cholesterol (HDL-C) and low-density lipoprotein cholesterol (LDL-C).
The investigators reported that on ROC analysis, HDL-C showed excellent diagnostic accuracy for six-week mortality, with an area under the receiver operating characteristic curves (AUROC) of 0.847 (95% CI 0.789–0.905). The best cut-off value of HDL-C was 0.54 mmol/L, with a sensitivity of 85.1% and specificity of 74.2%. The laboratory variables significantly associated with 6-week mortality in the univariate analysis were as follows: hepatocellular carcinoma (HCC), packed red blood cells (PRBC) transfusion, hemoglobin (HGB), total leukocyte count (WBC), alanine aminotransferase (ALT), serum sodium (Na), total bilirubin (TBIL), albumin (ALB), cholesterol, HDL-C, LDL-C, serum creatinine (Scr), international normalized ratio (INR), fibrinogen (FIB). Multivariate logistic regression analyses showed that TBIL, HDL-C, Na, and HGB were independently associated with six-week mortality.
The authors concluded that HDL-C is a potential indicator for the prognosis of patients with cirrhosis and acute gastrointestinal bleeding. The new algorithm based on HDL-C allowed an accurate predictive assessment of 6-week mortality after bleeding attack. The study was published on November 16, 2020 in the journal BMC Gastroenterology.
Related Links:
Peking University First Hospital
Latest Clinical Chem. News
- Saliva-Based Test Detects Biochemical Signs of Sleep Loss
- Simple Dual-Tau Blood Test Detects and Stages Alzheimer’s Disease
- Alzheimer’s Blood Biomarkers Linked to Early Cognitive Differences Before Dementia
- Urine-Based Test Shows Promise for Autism Screening in Children
- Blood-Based Sensor Detects Early Signs of Alzheimer’s and Parkinson’s
- Liquid Biopsy Biomarkers May Improve Childhood Epilepsy Diagnosis
- Urine-Based Alzheimer’s Test Receives FDA Breakthrough Device Designation
- Fluid Biomarker Improves Diagnosis and Monitoring of Primary CNS Lymphoma
- New CA19-9 Cutoff Value Helps Identify High-Risk Pancreatic Cancer Patients
- Blood-Based Biomarkers Show Promise for Psychosis Risk Prediction
- International Experts Recommend Ending Routine 'Corrected' Calcium Reporting
- Long-Term Data Show PSA Screening Modestly Reduces Prostate Cancer Deaths
- Urine-Based Nanosensor Tracks Lung Cancer and Fibrosis Noninvasively
- FDA-Cleared Assay Enables Comprehensive Automated Testosterone Testing
- CE-Marked Blood Biomarker Test Advances Automated Alzheimer’s Diagnostics
- Blood-Based Alzheimer’s Test Gains CE Mark for Amyloid Pathology Detection
Channels
Molecular Diagnostics
view channel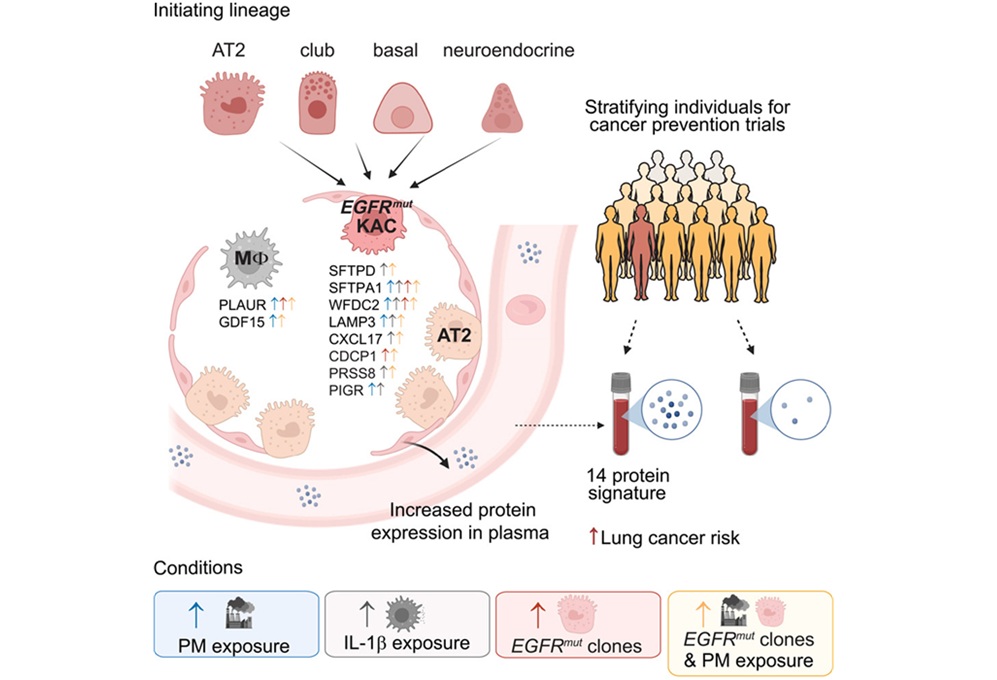
Plasma Protein Signature Predicts Lung Cancer Risk Up to Five Years Ahead
Lung cancer remains a leading cause of cancer death, and many cases are detected only after symptoms appear. Current screening programs largely target people with a history of smoking, leaving other at-risk... Read more
Circulating Tumor DNA Testing Guides Chemotherapy, Reduces Relapse in Colon Cancer
Adjuvant therapy decisions after curative surgery for colon cancer remain difficult, as conventional clinicopathologic factors often fail to capture residual disease risk. Liquid biopsy approaches that... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channelAptamer-Based Biosensor Enables Mutation-Resilient SARS-CoV-2 Detection
Rapid evolution of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can undermine existing molecular diagnostics, especially when assays target small viral components. Double-antibody sandwich... Read more
Study Points to Autoimmune Pathway Behind Long COVID Symptoms
Long COVID leaves many SARS-CoV-2 survivors with persistent fatigue, cognitive issues, palpitations, and musculoskeletal pain for months or years. Estimates cited in new research suggest 4%–20% of infected... Read more
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read moreMicrobiology
view channel
Gut Microbiome Signatures Help Identify Risk of IBD Progression
Inflammatory bowel disease (IBD), encompassing Crohn’s disease and ulcerative colitis, is a chronic relapsing inflammatory disorder of the gastrointestinal tract with highly variable outcomes.... Read more
FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
Clinical guidelines support testing based on patient presentation in suspected gastrointestinal infections, yet available technologies have often forced laboratories to choose between panels that are too... Read morePathology
view channel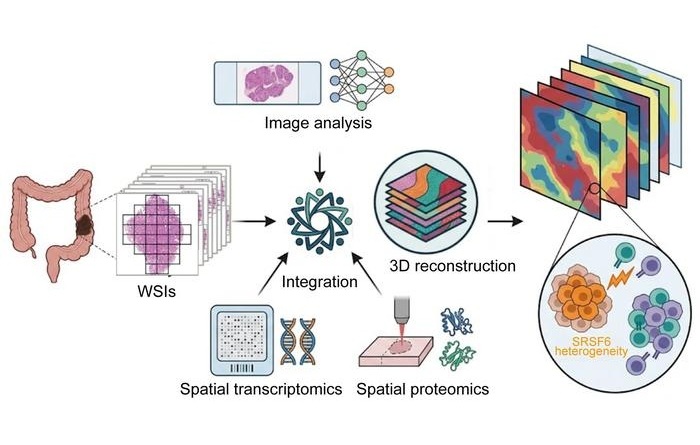
3D Spatial Multi-Omics Maps Intra-Tumor Diversity in Colorectal Cancer
Colorectal cancer remains a leading cause of cancer death, and clinical decision-making is complicated by marked intra-tumor heterogeneity. Conventional bulk sequencing averages molecular signals across... Read more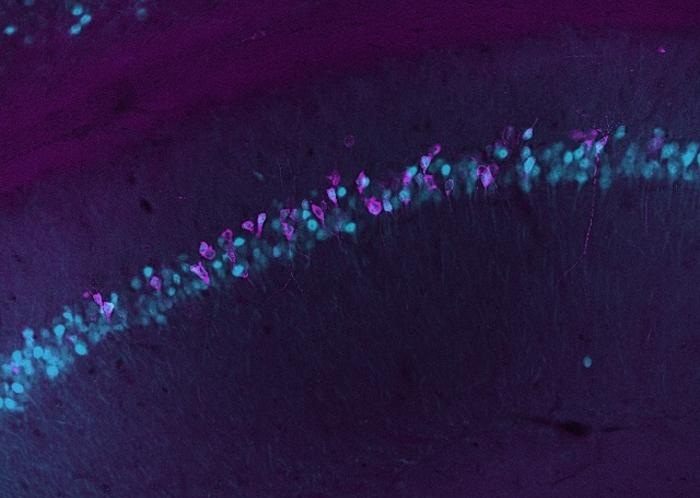
Blood-Based Method Tracks Gene Activity in the Living Brain
Real-time measurement of gene activity in the brain has been limited by assays requiring destructive tissue sampling. Tracking active genes could reveal how the body responds to environmental factors,... Read moreTechnology
view channel
AI Platform Links Biomarker Results to Cancer Clinical Trials and Guidelines
Oncology teams must manage growing volumes of genomic data, rapidly evolving clinical trial options, and frequently updated care guidelines, all within tight clinic schedules. Translating complex tumor... Read more
Agentic AI Platform Supports Genomic Decision-Making in Oncology
Oncology care teams increasingly face the challenge of managing complex molecular diagnostics, evolving treatment options, and extensive electronic health record documentation. Translating multimodal data... Read moreIndustry
view channel