Peptide Biomarker Predicts Risk of Dying in Patients with Stable Heart Failure
|
By LabMedica International staff writers Posted on 13 Jan 2020 |
Image: NMR solution structure of neuropeptide Y (Photo courtesy of Wikimedia Commons)
Cardiovascular disease researchers have identified a biomarker that predicts when a patient with chronic stable heart failure (CHF) is likely to die.
Individuals with stable CHF have suffered damage to their heart muscles but do not usually require hospitalization. While these individuals are at increased risk of dying within five years from the time of injury, some experience rapid disease progression while others remain in a stable condition.
Investigators at the University of California, Los Angeles (USA) searched for biomarkers that could distinguish between these two classes of CHF patients. To this end, they analyzed blood samples from 105 patients with stable heart failure, searching for a distinct biomarker in the blood that could predict how likely a person would be to die within a few years. The investigators examined coronary sinus (CS) blood in a prospective cohort of patients with stable CHF at the time of elective cardiac resynchronization therapy (CRT) device implantation, during which the CS was readily accessible. Coronary sinus blood was chosen for sampling over peripheral venous blood to avoid the potential contaminating effect of other tissues such as the gastrointestinal tract. The mean age of the patients was 68 years and 82 (78%) were men.
Results revealed that neuropeptide Y levels were the clearest and most significant predictor of which patients were most likely to die within one to three years. Neuropeptide Y (NPY) is a 36 amino-acid neuropeptide that is involved in various physiological and homeostatic processes in both the central and peripheral nervous systems. NPY has been identified as the most abundant peptide present in the mammalian central nervous system, which consists of the brain and spinal cord. It is secreted alongside other neurotransmitters such as GABA and glutamate.
Overall, findings obtained during this study indicated that patients with higher levels of neuropeptide Y were nearly 10 times more likely to die within one to three years than those with lower levels of NPY. Thus, determination of NPY level could serve as a tool to distinguish very-high-risk patients with stable heart failure from lower risk patients with the same condition. This information would identify those patients requiring more aggressive and targeted therapies.
The study was published in the December 26, 2019, online edition of the journal JAMA Cardiology.
Related Links:
University of California, Los Angeles
Individuals with stable CHF have suffered damage to their heart muscles but do not usually require hospitalization. While these individuals are at increased risk of dying within five years from the time of injury, some experience rapid disease progression while others remain in a stable condition.
Investigators at the University of California, Los Angeles (USA) searched for biomarkers that could distinguish between these two classes of CHF patients. To this end, they analyzed blood samples from 105 patients with stable heart failure, searching for a distinct biomarker in the blood that could predict how likely a person would be to die within a few years. The investigators examined coronary sinus (CS) blood in a prospective cohort of patients with stable CHF at the time of elective cardiac resynchronization therapy (CRT) device implantation, during which the CS was readily accessible. Coronary sinus blood was chosen for sampling over peripheral venous blood to avoid the potential contaminating effect of other tissues such as the gastrointestinal tract. The mean age of the patients was 68 years and 82 (78%) were men.
Results revealed that neuropeptide Y levels were the clearest and most significant predictor of which patients were most likely to die within one to three years. Neuropeptide Y (NPY) is a 36 amino-acid neuropeptide that is involved in various physiological and homeostatic processes in both the central and peripheral nervous systems. NPY has been identified as the most abundant peptide present in the mammalian central nervous system, which consists of the brain and spinal cord. It is secreted alongside other neurotransmitters such as GABA and glutamate.
Overall, findings obtained during this study indicated that patients with higher levels of neuropeptide Y were nearly 10 times more likely to die within one to three years than those with lower levels of NPY. Thus, determination of NPY level could serve as a tool to distinguish very-high-risk patients with stable heart failure from lower risk patients with the same condition. This information would identify those patients requiring more aggressive and targeted therapies.
The study was published in the December 26, 2019, online edition of the journal JAMA Cardiology.
Related Links:
University of California, Los Angeles
Latest Molecular Diagnostics News
- RNA Profiling Uncovers Therapeutic Targets in Solid Tumors
- Whole Genome Sequencing in Routine Care Expands Rare Disease Detection
- New AI Tool Improves Detection of Genetic Causes in Rare Disorders
- Adaptive PCR Platform Improves Consistency in Small-Batch NGS Workflows
- Portable Test Uses CRISPR to Rapidly Identify STIs and Resistance Markers
- New Molecular Test Boosts Accuracy of Bile Duct Cancer Diagnosis
- First IVDR‑Certified IGH Clonality Assay Supports Diagnosis of B-Cell Malignancies
- Plasma ctDNA Testing Predicts Breast Cancer Recurrence After Neoadjuvant Therapy
- New Respiratory Panel Expands Pathogen Detection to 25 Targets
- Nasal Swab May Reveal Early Signs of Alzheimer’s Disease
- Blood Biomarker Predicts Cognitive Outcomes After Cardiac Arrest
- Liquid Biopsy Enables Faster Diagnosis of Childhood Cancer in Africa
- Blood Test Helps Guide Treatment in Older Women with Breast Cancer
- Rapid Host-Response Test Distinguishes Bacterial and Viral Infections in Minutes
- Liquid Biopsy Method Pinpoints Disease Source From a Single Drop of Blood
- Study Reveals Widespread Errors in Gene Variant Naming
Channels
Clinical Chemistry
view channel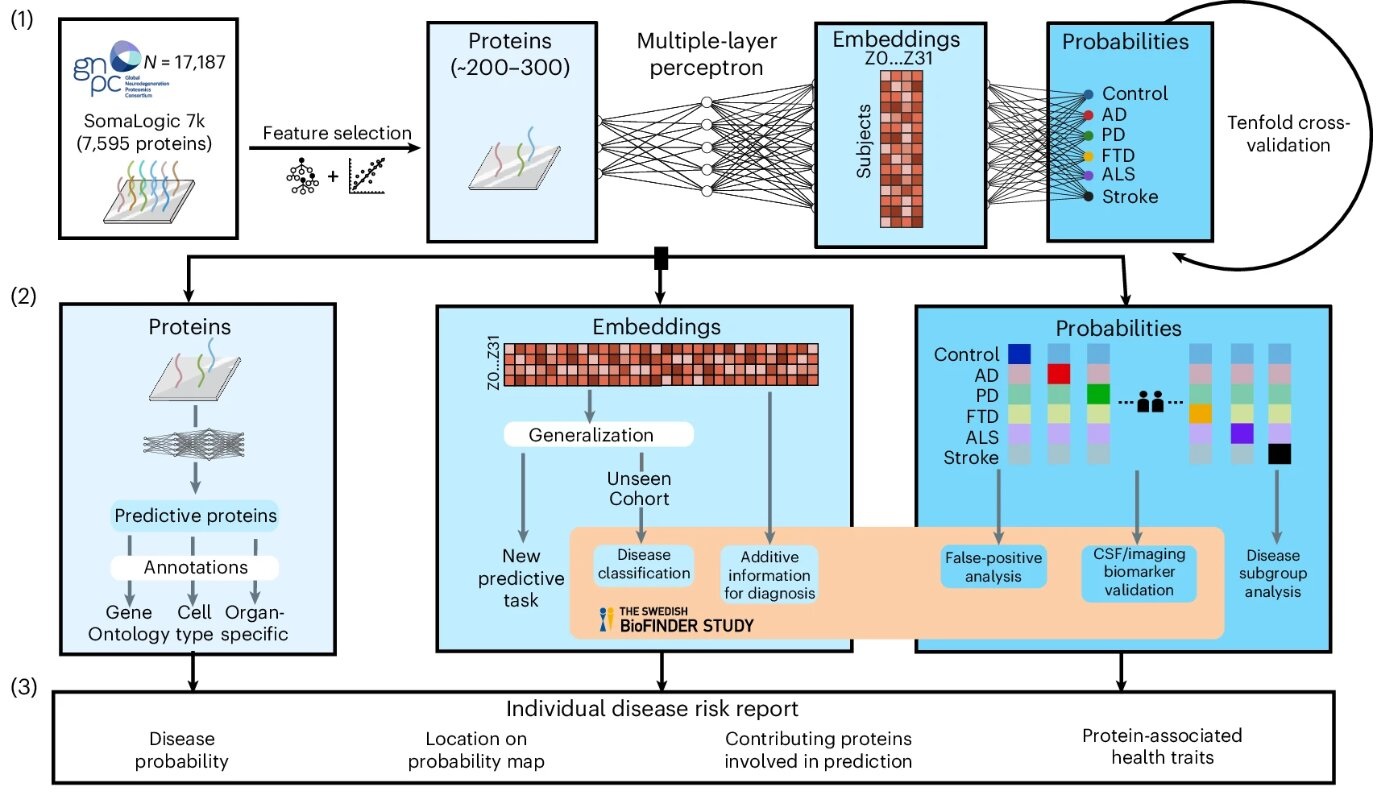
AI-Based Blood Test Diagnose Multiple Brain Disorders from Blood Sample
Diagnosing the cause of age-related cognitive symptoms remains challenging because clinical presentations of neurodegenerative diseases often overlap, and multiple pathologies can co-occur... Read more
New CLIA Status Brings Mass Spectrometry Steroid Testing to Routine Labs
Steroid hormone measurement is a core application of clinical mass spectrometry, which is widely regarded as a diagnostic gold standard. Access to these high-specificity methods has often been constrained... Read moreHematology
view channel
Rapid Cartridge-Based Test Aims to Expand Access to Hemoglobin Disorder Diagnosis
Sickle cell disease and beta thalassemia are hemoglobin disorders that often require referral to specialized laboratories for definitive diagnosis, delaying results for patients and clinicians.... Read more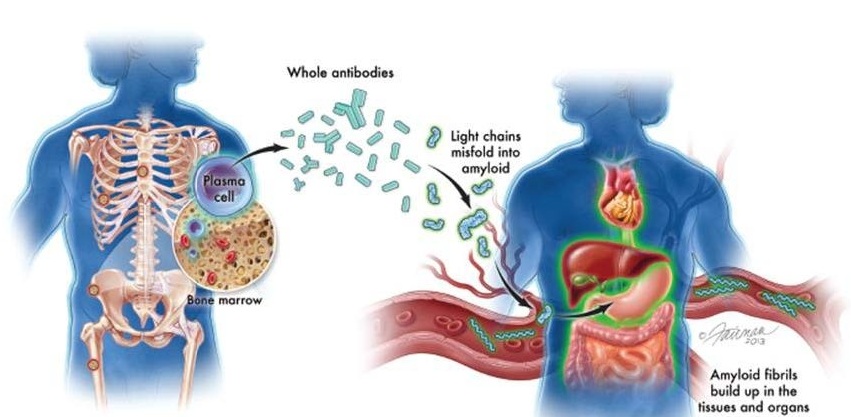
New Guidelines Aim to Improve AL Amyloidosis Diagnosis
Light chain (AL) amyloidosis is a rare, life-threatening bone marrow disorder in which abnormal amyloid proteins accumulate in organs. Approximately 3,260 people in the United States are diagnosed... Read moreImmunology
view channel
FDA Approval Expands Use of PD-L1 Companion Diagnostic in Esophageal and GEJ Carcinomas
Esophageal and gastroesophageal junction carcinomas (GEJ) have a poor prognosis, with approximately 16,250 deaths in the United States in 2025 and a five-year relative survival of 21.9%.... Read more
Study Identifies Inflammatory Pathway Driving Immunotherapy Resistance in Bladder Cancer
Bladder cancer remains a prevalent malignancy with variable responses to immune checkpoint inhibitors. Clinicians often observe elevated C-reactive protein and interleukin-6 in affected patients, yet the... Read moreMicrobiology
view channel
New Bacterial Target Identified for Early Detection of Noma
Noma is a rapidly progressing orofacial infection that begins as gingivitis and can destroy oral and facial tissues, primarily affecting young children living in extreme poverty. Without treatment, it... Read more
Genomic Analysis Links Emerging Streptococcal Strains to Specific Infections
Streptococcus dysgalactiae subspecies equisimilis (SDSE) infections are increasing worldwide and include variants that may lead to severe disease. Researchers now report that whole-genome sequencing of... Read morePathology
view channel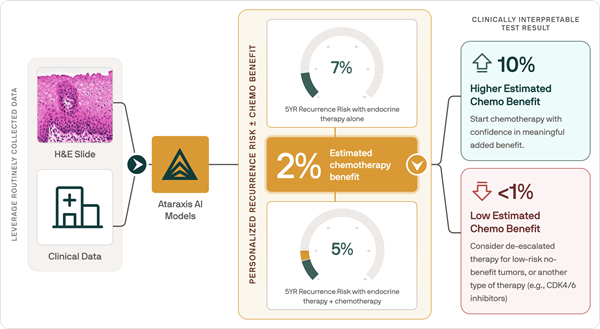
AI Tool Predicts Patient-Specific Chemotherapy Benefit in Breast Cancer
Selecting adjuvant chemotherapy for early-stage breast cancer is typically guided by recurrence risk and population-level averages rather than patient-specific benefit. However, existing clinicopathologic... Read more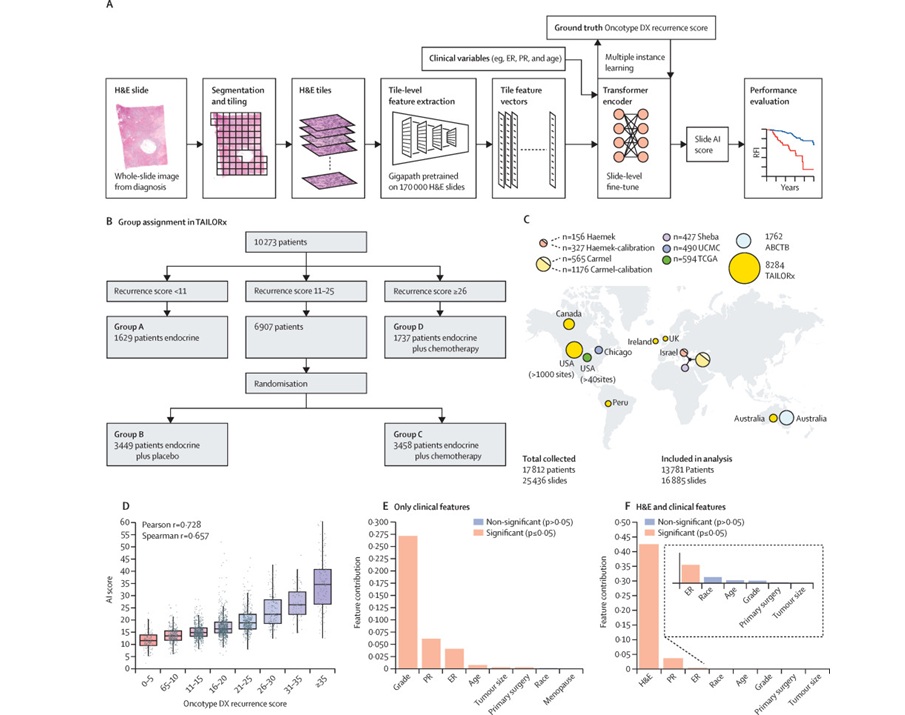
AI-Based Pathology Model Guides Chemotherapy Decisions in Breast Cancer
Selecting adjuvant chemotherapy for early-stage breast cancer remains a difficult decision because only a subset benefits and many undergo toxicity without gain. Genomic assays can help but are costly,... Read moreTechnology
view channel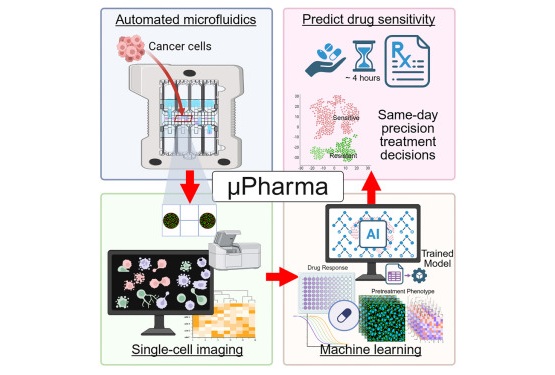
New AI Tool Enables Rapid Treatment Selection in Pediatric Leukemia
Children with T-cell acute lymphoblastic leukemia face an aggressive disease that remains difficult to treat. Although remission rates have improved, many survivors experience long-term effects from intensive... Read more
Breakthrough Mass Spectrometry Design Could Enable Ultra-Low Abundance Detection
Mass spectrometry is central to identifying and quantifying molecules in complex biological samples, but conventional instruments typically analyze ions sequentially, which can limit detection of rare species.... Read moreIndustry
view channel
Takara Bio USA and Hamilton Partner Partner to Automate NGS Library Preparation
Takara Bio USA, Inc. (San Jose, CA, USA), a wholly owned subsidiary of Takara Bio Inc., and Hamilton Company (Reno, NV, USA) announced a development and co-marketing agreement to deliver integrated, automated... Read more