Method Identifies Cancer in Early Onset Diabetics
|
By LabMedica International staff writers Posted on 04 Jul 2018 |
Image: Patients diagnosed with pancreatic cancer can develop elevated blood sugar levels up to three years before their cancer diagnosis (Photo courtesy of Mayo Clinic).
It is unclear how long pancreatic ductal adenocarcinomas (PDACs) are present before diagnosis. Patients with PDAC usually develop hyperglycemia and diabetes before the tumor is identified.
It has been suggested that if early invasive PDACs are associated with hyperglycemia, the duration of hyperglycemia should associate with the time that they have had the tumor. Of subjects with new-onset diabetes, based on glycemia, over the age of 50 years, approximately 1% are diagnosed with pancreatic cancer within three years.
Scientists at the Mayo Clinic (Rochester, MN, USA) and their colleagues carried out a study recently exploring methods to diagnose cancer in patients with early onset diabetes. In the first study, they plotted blood sugars levels of patients with pancreatic cancer going back five years prior to diagnosis. They also plotted the blood sugars of a control group of patients who were age and gender matched to the patients with pancreatic cancer. They analyzed temporal fasting blood glucose (FBG) profiles collected for 60 months before patients received a PDAC diagnosis (index date) (cohort A = 219)), FBG profiles of patients with resected PDAC (n=526) stratified by tumor volume and grade (cohort B =526), and temporal FBG profiles of patients with resected PDACs from whom long-term FBG data were available for 103. In another group of patients and controls, they plotted blood sugars of nearly 600 patients with pancreatic cancer just prior to surgical removal of the cancer.
In cohort A, the mean FBG did not differ significantly between cases and controls 36 months before the index date. Hyperglycemia was first noted 30–36 months before PDAC diagnosis in all cases, those with or without diabetes at baseline and those with or without resection at diagnosis. FBG level increased until diagnosis of PDAC. In cohort B, the mean FBG did not differ significantly in controls versus cases with PDACs below 1.0 cc. The smallest tumor volume associated with hyperglycemia was 1.1–2.0 cc; FBG level increased with tumor volume. FBG varied with tumor grade: well- or moderately differentiated tumors (5.8 cc) produced the same FBG levels as smaller, poorly differentiated tumors (1.5 cc). In cohort C, the duration of pre-diagnostic hyperglycemia for cases with large-, medium-, or small-volume PDACs was 24–36, 12–24, and 0–12 months, respectively. PDAC resection resolved hyperglycemia, regardless of tumor location.
Suresh Chari, MD, a gastroenterologist and senior author of the study, said, “Pancreatic cancer is rapidly fatal after its diagnosis, with average survival of six months. It has also been thought that its course prior to diagnosis is also rapid and that early detection is not feasible. But our studies provide hope that pancreatic cancer can indeed be diagnosed at an earlier stage when it is resectable.”
The authors concluded that in a case–control study of patients with PDAC from two databases, they associated FBG level with time to PDAC diagnosis and tumor volume and grade. Patients are hyperglycemic for a mean period of 30–36 months before PDAC diagnosis; this information might be incorporated in strategies for early detection. The study was originally published online on April 30, 2018, in the journal Gastroenterology.
Related Links:
Mayo Clinic
It has been suggested that if early invasive PDACs are associated with hyperglycemia, the duration of hyperglycemia should associate with the time that they have had the tumor. Of subjects with new-onset diabetes, based on glycemia, over the age of 50 years, approximately 1% are diagnosed with pancreatic cancer within three years.
Scientists at the Mayo Clinic (Rochester, MN, USA) and their colleagues carried out a study recently exploring methods to diagnose cancer in patients with early onset diabetes. In the first study, they plotted blood sugars levels of patients with pancreatic cancer going back five years prior to diagnosis. They also plotted the blood sugars of a control group of patients who were age and gender matched to the patients with pancreatic cancer. They analyzed temporal fasting blood glucose (FBG) profiles collected for 60 months before patients received a PDAC diagnosis (index date) (cohort A = 219)), FBG profiles of patients with resected PDAC (n=526) stratified by tumor volume and grade (cohort B =526), and temporal FBG profiles of patients with resected PDACs from whom long-term FBG data were available for 103. In another group of patients and controls, they plotted blood sugars of nearly 600 patients with pancreatic cancer just prior to surgical removal of the cancer.
In cohort A, the mean FBG did not differ significantly between cases and controls 36 months before the index date. Hyperglycemia was first noted 30–36 months before PDAC diagnosis in all cases, those with or without diabetes at baseline and those with or without resection at diagnosis. FBG level increased until diagnosis of PDAC. In cohort B, the mean FBG did not differ significantly in controls versus cases with PDACs below 1.0 cc. The smallest tumor volume associated with hyperglycemia was 1.1–2.0 cc; FBG level increased with tumor volume. FBG varied with tumor grade: well- or moderately differentiated tumors (5.8 cc) produced the same FBG levels as smaller, poorly differentiated tumors (1.5 cc). In cohort C, the duration of pre-diagnostic hyperglycemia for cases with large-, medium-, or small-volume PDACs was 24–36, 12–24, and 0–12 months, respectively. PDAC resection resolved hyperglycemia, regardless of tumor location.
Suresh Chari, MD, a gastroenterologist and senior author of the study, said, “Pancreatic cancer is rapidly fatal after its diagnosis, with average survival of six months. It has also been thought that its course prior to diagnosis is also rapid and that early detection is not feasible. But our studies provide hope that pancreatic cancer can indeed be diagnosed at an earlier stage when it is resectable.”
The authors concluded that in a case–control study of patients with PDAC from two databases, they associated FBG level with time to PDAC diagnosis and tumor volume and grade. Patients are hyperglycemic for a mean period of 30–36 months before PDAC diagnosis; this information might be incorporated in strategies for early detection. The study was originally published online on April 30, 2018, in the journal Gastroenterology.
Related Links:
Mayo Clinic
Latest Pathology News
- FDA Clears AI Digital Pathology Tool for Breast Cancer Risk Stratification
- New AI Tool Reveals Hidden Genetic Signals in Routine H&E Slides
- AI System Analyzes Routine Pathology Slides to Predict Cancer Outcomes
- New Tissue Mapping Approach Identifies High-Risk Form of Diabetic Kidney Disease
- Multimodal AI Tool Predicts Genetic Alterations to Guide Breast Cancer Treatment
- Interpretable AI Reveals Hidden Cellular Features from Microscopy Images
- Tumor Immune Structure Predicts Response to Immunotherapy in Melanoma
- Plug-and-Play AI Pathology System Classifies Multiple Cancers from Few Slides
- AI-Based Assays Support Risk Stratification in Prostate and Breast Cancer
- AI Pathology Model Predicts Immunotherapy Response in Lung Cancer
- Study Reveals Moleclar Mechanism Driving Aggressive Skin Cancer
- AI Precision Tests Deliver Cancer Risk Insights from Routine H&E Slides
- Collaboration Applies AI Pathology to Predict Response to Antibody-Drug Conjugates
- Biomarker Predicts Immunotherapy Response and Prognosis in Colorectal Cancer
- AI Improves Completeness of Complex Cancer Pathology Reports
- AI Tool Predicts Chemotherapy Response in Small Cell Lung Cancer
Channels
Molecular Diagnostics
view channel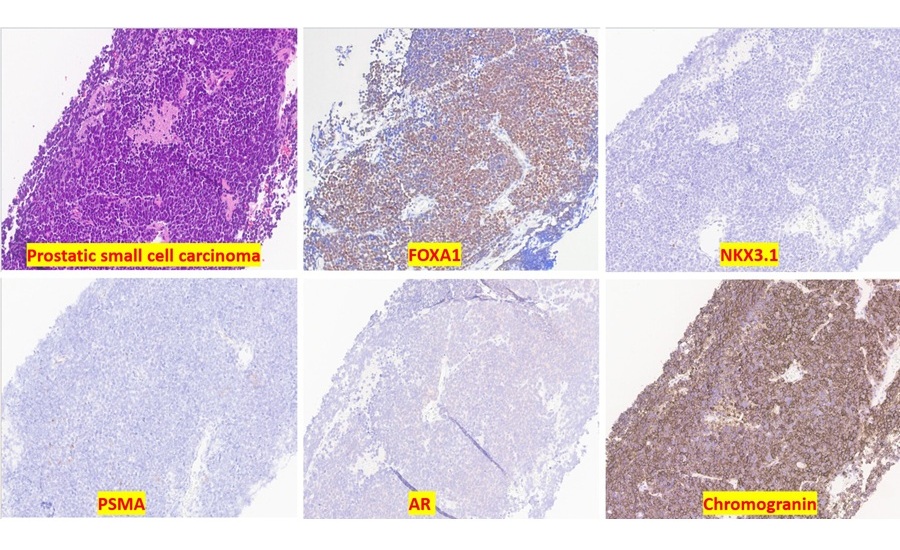
Sensitive Protein Marker Aids Diagnosis of Small Cell Prostate Cancer
Accurate identification of aggressive prostate cancer subtypes can be difficult when tumors lose expression of lineage markers used in routine pathology. Small cell carcinoma of the prostate, in particular,... Read more
Rapid Multiplex PCR Test Detects 11 Gastrointestinal Pathogens from Single Sample
Cepheid’s Xpert GI Panel has received CE marking under the In Vitro Diagnostic Medical Devices Regulation (IVDR) and is expected to begin shipping to countries that accept the CE mark in the coming weeks.... Read moreHematology
view channel
Stem Cell Biomarkers May Guide Precision Treatment in Acute Myeloid Leukemia
Acute myeloid leukemia (AML) is an aggressive blood cancer that most often affects older adults and still carries a poor prognosis despite therapeutic advances. Venetoclax-based regimens have improved... Read more
Advanced CBC-Derived Indices Integrated into Hematology Platforms
Diatron, a STRATEC brand, has introduced six advanced hematological indices on its Aquila, Aquarius 3, and Abacus 5 hematology analyzers. The new Research Use Only (RUO) indices include Neutrophil-to-Lymphocyte... Read moreImmunology
view channel
Routine TB Screening Test May Reveal Immune Aging and Mortality Risk
Immune aging is associated with weaker responses to vaccination, greater risks of infection, and higher levels of inflammation. Leveraging routinely ordered laboratory tests to quantify that responsiveness... Read more
Biomarkers and Molecular Testing Advance Precision Allergy Care
Allergic diseases often present with similar symptoms but can be driven by distinct biological mechanisms, making standardized care inefficient for many patients. Historically, individuals with pollen... Read moreMicrobiology
view channel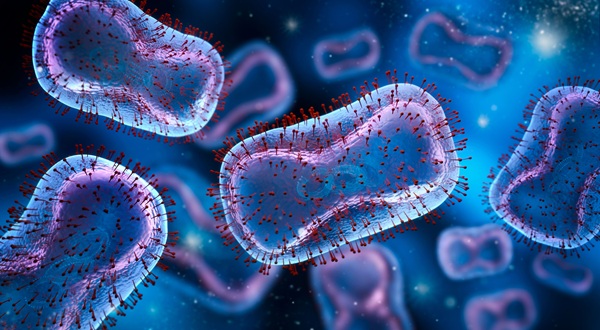
Study Finds Hidden Mpox Infections May Drive Ongoing Spread
Mpox continues to circulate despite vaccination, and many cases show no known link to a symptomatic partner. The role of people without symptoms has remained uncertain, limiting clarity on how transmission persists.... Read more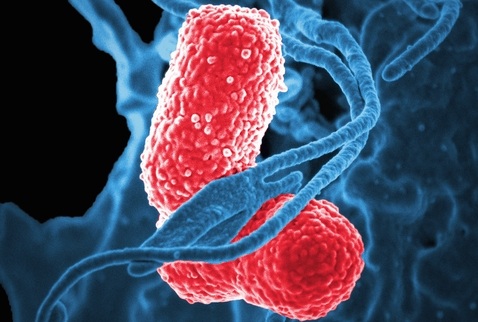
Large-Scale Genomic Surveillance Tracks Resistant Bacteria Across European Hospitals
Antimicrobial resistance (AMR) poses a growing threat to patient safety, with carbapenem-resistant Enterobacterales causing difficult-to-treat infections and leaving clinicians with limited therapeutic options.... Read more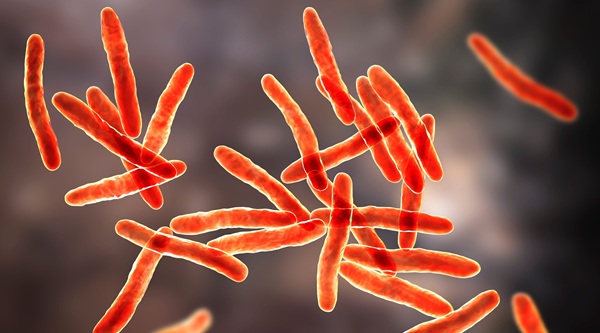
Molecular Urine and Stool Tests Do Not Improve Early TB Treatment in Hospitalized HIV Patients
Tuberculosis is the leading cause of death among people living with HIV, and diagnosis in hospital settings remains difficult. Symptoms are often non-specific, disease can be extrapulmonary, and many patients... Read morePathology
view channel
FDA Clears AI Digital Pathology Tool for Breast Cancer Risk Stratification
Risk assessment at diagnosis is central to guiding therapy for early-stage, hormone receptor-positive, human epidermal growth factor receptor 2-negative (HR+/HER2-) invasive breast cancer, where overtreatment... Read more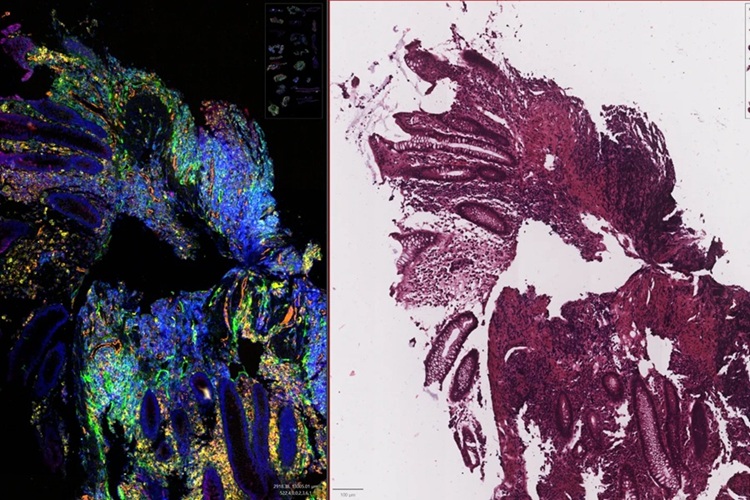
New AI Tool Reveals Hidden Genetic Signals in Routine H&E Slides
Pathologists worldwide rely on hematoxylin and eosin (H&E) slides to examine tissue architecture, yet these stains do not reveal the underlying molecular activity that often drives disease.... Read moreTechnology
view channel
Point-of-Care Testing Enhances Health Literacy and Self-Management in Chronic Disease
Limited access to general practitioners and pathology services can delay diagnosis and monitoring for people in regional and remote communities. Rapid, on-the-spot testing can shorten turnaround times... Read more
Fully Automated Sample-to-Insight Workflow Advances Latent TB Testing
Latent tuberculosis remains a substantial testing workload for clinical laboratories as screening programs expand. Despite this growth, only about 40% of testing has shifted from traditional skin tests... Read moreIndustry
view channel
AI-Powered Multi-Functional Analyzer Wins German Innovation Award
Hematology services are increasingly delivered across distributed care settings, where limited staffing and complex workflows can extend turnaround times. Advanced morphology review still often depends... Read more