Genomic Test Detects Lynch Syndrome in Colorectal Cancer
|
By LabMedica International staff writers Posted on 11 Apr 2018 |

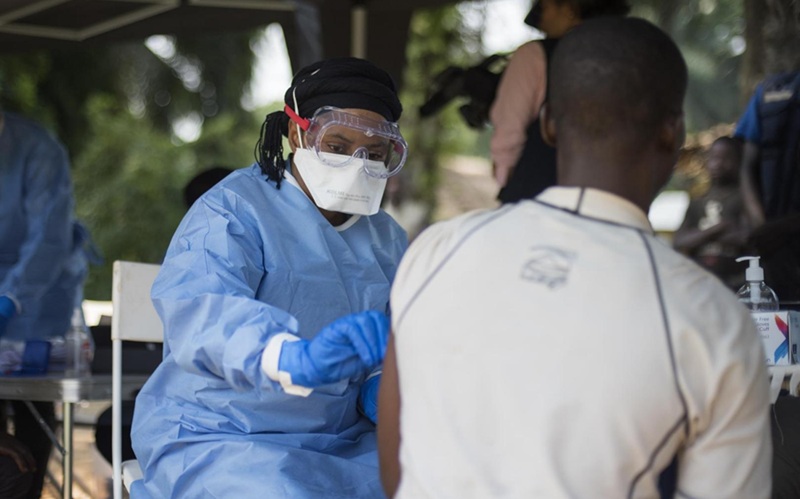
Image: UW-OncoPlex is a diagnostic tool that uses genetic sequencing to look for mutations that cause cancer (Photo courtesy of University of Washington).
Lynch syndrome (LS) affects approximately 3% of all patients with colorectal cancer (CRC), making it the most common hereditary syndrome that predisposes individuals to develop CRC. Universal tumor screening for LS in CRC is recommended and involves up to six sequential tests.
Somatic gene testing is performed on stage IV CRCs for treatment determination. The diagnostic workup for patients with CRC could be simplified and improved using a single up-front tumor next-generation sequencing test if it has higher sensitivity and specificity than the current screening protocol.
Scientists at Ohio State University (Columbus, OH, USA) and their colleagues analyzed tumor samples from 419 CRC patients who participated in the Ohio Colorectal Cancer Prevention Initiative (OCCPI), a statewide study to screen newly diagnosed CRC patients and their biological relatives for Lynch syndrome. All OCCPI study participants had their tumor samples analyzed using the traditional multi-test genetic testing approach and the single, upfront genomic tumor-sequencing test approach in which a single tumor sample was analyzed for multiple mutations simultaneously. A total of 197 of the 419 prospective cases underwent germline genetic testing.
Tumor sequencing was performed using University of Washington (UW)-OncoPlex in the Clinical Laboratory Improvement Amendments–certified laboratory setting (Seattle, WA, USA). UW-OncoPlex is a clinically validated targeted next-generation sequencing (NGS) deep sequencing panel that sequences to 500 × mean depth all exons, introns, and flanking regions of MLH1, MSH2, and MSH6, and all exons of PMS2 in addition to assessing BRAF, KRAS, NRAS, and MSI status among other genes.
The team compared the results from the two screening methods and found that the upfront tumor-sequencing approach was more sensitive and more specific for detecting Lynch syndrome than the old, multiple-test model. Tumor sequencing resulted in a 10% improvement in Lynch syndrome detection rates while also providing important information about treatment options for the patients.
Heather Hampel, MS, CGC, the principal investigator and corresponding author of the study, said, “Testing methods of the past would just point to a suspicion of Lynch syndrome, but they could not confirm the diagnosis without multiple additional tests, which slows down the diagnostic process and adds costs. This new approach points to the exact mutation patients were born with and does so through a single test. The mutation will need to be confirmed using a blood test but this requires a single mutation test, which is less expensive than multi-gene panel testing. The previous method could sometimes require patients to get up to five individual tests before knowing if they had Lynch syndrome.” The study was published on March 29, 2018, in the journal JAMA Oncology.
Related Links:
Ohio State University
University of Washington
Somatic gene testing is performed on stage IV CRCs for treatment determination. The diagnostic workup for patients with CRC could be simplified and improved using a single up-front tumor next-generation sequencing test if it has higher sensitivity and specificity than the current screening protocol.
Scientists at Ohio State University (Columbus, OH, USA) and their colleagues analyzed tumor samples from 419 CRC patients who participated in the Ohio Colorectal Cancer Prevention Initiative (OCCPI), a statewide study to screen newly diagnosed CRC patients and their biological relatives for Lynch syndrome. All OCCPI study participants had their tumor samples analyzed using the traditional multi-test genetic testing approach and the single, upfront genomic tumor-sequencing test approach in which a single tumor sample was analyzed for multiple mutations simultaneously. A total of 197 of the 419 prospective cases underwent germline genetic testing.
Tumor sequencing was performed using University of Washington (UW)-OncoPlex in the Clinical Laboratory Improvement Amendments–certified laboratory setting (Seattle, WA, USA). UW-OncoPlex is a clinically validated targeted next-generation sequencing (NGS) deep sequencing panel that sequences to 500 × mean depth all exons, introns, and flanking regions of MLH1, MSH2, and MSH6, and all exons of PMS2 in addition to assessing BRAF, KRAS, NRAS, and MSI status among other genes.
The team compared the results from the two screening methods and found that the upfront tumor-sequencing approach was more sensitive and more specific for detecting Lynch syndrome than the old, multiple-test model. Tumor sequencing resulted in a 10% improvement in Lynch syndrome detection rates while also providing important information about treatment options for the patients.
Heather Hampel, MS, CGC, the principal investigator and corresponding author of the study, said, “Testing methods of the past would just point to a suspicion of Lynch syndrome, but they could not confirm the diagnosis without multiple additional tests, which slows down the diagnostic process and adds costs. This new approach points to the exact mutation patients were born with and does so through a single test. The mutation will need to be confirmed using a blood test but this requires a single mutation test, which is less expensive than multi-gene panel testing. The previous method could sometimes require patients to get up to five individual tests before knowing if they had Lynch syndrome.” The study was published on March 29, 2018, in the journal JAMA Oncology.
Related Links:
Ohio State University
University of Washington
Latest Pathology News
- 3D Spatial Multi-Omics Maps Intra-Tumor Diversity in Colorectal Cancer
- Blood-Based Method Tracks Gene Activity in the Living Brain
- FDA Approval Expands Automated PD-L1 Testing Across Solid Tumors
- AI-Powered Atlas Maps Immune Structures Linked to Cancer Outcomes
- AI Tool Extracts Immune Signals from Biopsy to Inform Myeloma Therapy
- Rapid AI Tool Predicts Cancer Spatial Gene Expression from Pathology Images
- AI Pathology Test Receives FDA Breakthrough for Bladder Cancer Risk Stratification
- FDA Clears AI Digital Pathology Tool for Breast Cancer Risk Stratification
- New AI Tool Reveals Hidden Genetic Signals in Routine H&E Slides
- AI System Analyzes Routine Pathology Slides to Predict Cancer Outcomes
- New Tissue Mapping Approach Identifies High-Risk Form of Diabetic Kidney Disease
- Multimodal AI Tool Predicts Genetic Alterations to Guide Breast Cancer Treatment
- Interpretable AI Reveals Hidden Cellular Features from Microscopy Images
- Tumor Immune Structure Predicts Response to Immunotherapy in Melanoma
- Plug-and-Play AI Pathology System Classifies Multiple Cancers from Few Slides
- AI-Based Assays Support Risk Stratification in Prostate and Breast Cancer
Channels
Clinical Chemistry
view channel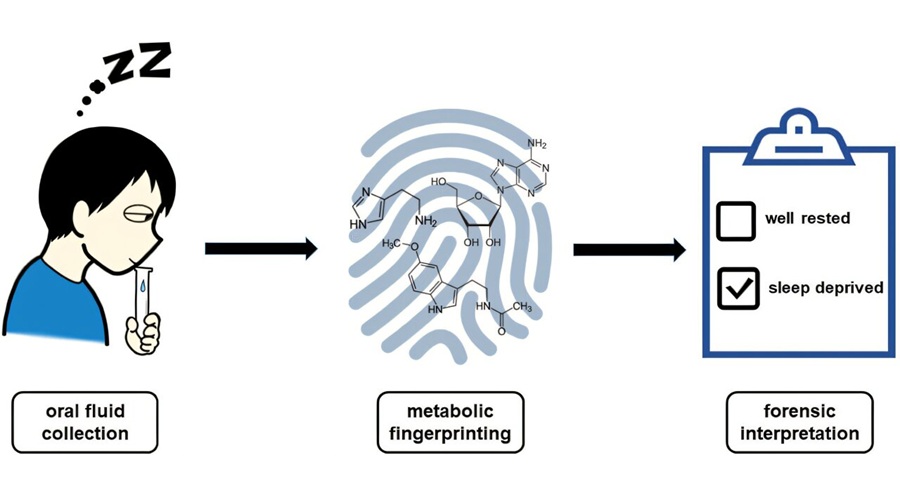
Saliva-Based Test Detects Biochemical Signs of Sleep Loss
Acute sleep loss impairs cognition and motor skills, raising safety risks that resemble alcohol intoxication. Clinicians currently lack an objective biochemical test to determine when someone is dangerously... Read more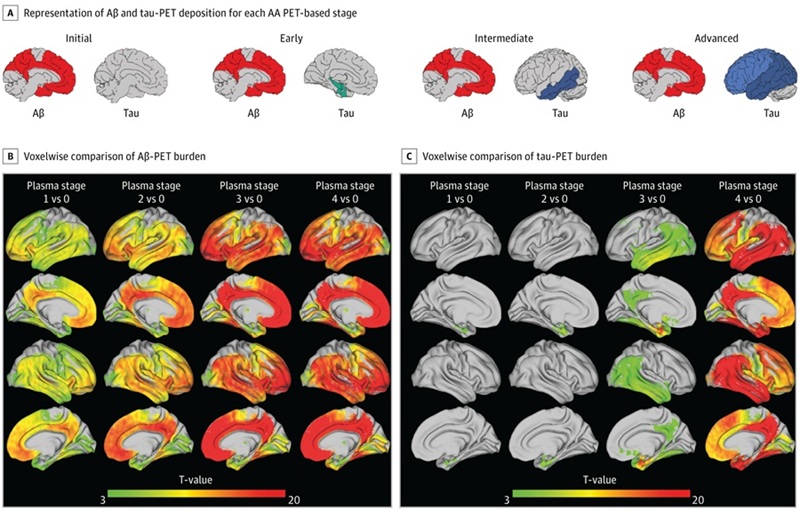
Simple Dual-Tau Blood Test Detects and Stages Alzheimer’s Disease
Alzheimer’s disease is typically confirmed and staged with positron emission tomography scans and cerebrospinal fluid testing, procedures that are costly and invasive. Broader access to minimally invasive... Read more
Alzheimer’s Blood Biomarkers Linked to Early Cognitive Differences Before Dementia
Blood-based screening for Alzheimer’s disease offers a noninvasive, lower-cost alternative to brain imaging or spinal fluid testing, yet its ability to flag the earliest cognitive changes has been unclear.... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channelAptamer-Based Biosensor Enables Mutation-Resilient SARS-CoV-2 Detection
Rapid evolution of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can undermine existing molecular diagnostics, especially when assays target small viral components. Double-antibody sandwich... Read more
Study Points to Autoimmune Pathway Behind Long COVID Symptoms
Long COVID leaves many SARS-CoV-2 survivors with persistent fatigue, cognitive issues, palpitations, and musculoskeletal pain for months or years. Estimates cited in new research suggest 4%–20% of infected... Read more
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read moreMicrobiology
view channel
Gut Microbiome Signatures Help Identify Risk of IBD Progression
Inflammatory bowel disease (IBD), encompassing Crohn’s disease and ulcerative colitis, is a chronic relapsing inflammatory disorder of the gastrointestinal tract with highly variable outcomes.... Read more
FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
Clinical guidelines support testing based on patient presentation in suspected gastrointestinal infections, yet available technologies have often forced laboratories to choose between panels that are too... Read morePathology
view channel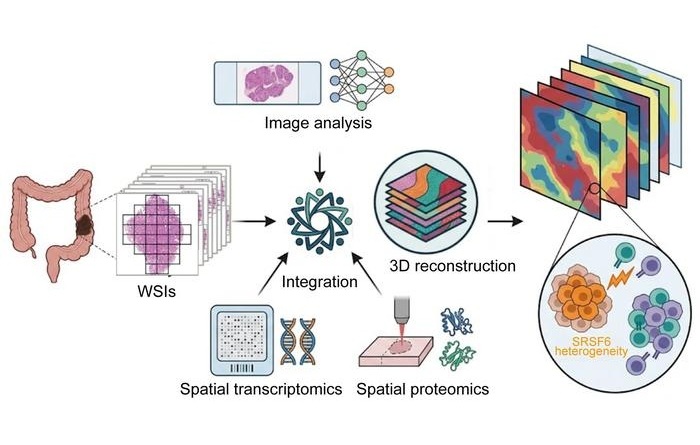
3D Spatial Multi-Omics Maps Intra-Tumor Diversity in Colorectal Cancer
Colorectal cancer remains a leading cause of cancer death, and clinical decision-making is complicated by marked intra-tumor heterogeneity. Conventional bulk sequencing averages molecular signals across... Read more
Blood-Based Method Tracks Gene Activity in the Living Brain
Real-time measurement of gene activity in the brain has been limited by assays requiring destructive tissue sampling. Tracking active genes could reveal how the body responds to environmental factors,... Read moreTechnology
view channel
AI Platform Links Biomarker Results to Cancer Clinical Trials and Guidelines
Oncology teams must manage growing volumes of genomic data, rapidly evolving clinical trial options, and frequently updated care guidelines, all within tight clinic schedules. Translating complex tumor... Read more
Agentic AI Platform Supports Genomic Decision-Making in Oncology
Oncology care teams increasingly face the challenge of managing complex molecular diagnostics, evolving treatment options, and extensive electronic health record documentation. Translating multimodal data... Read moreIndustry
view channel