Test Discovered for Earlier Detection of Transplant Rejection
|
By LabMedica International staff writers Posted on 06 Apr 2017 |

Image: The NanoSight NS300 instrument provides an easy-to-use, reproducible platform for nanoparticle characterization (Photo courtesy of Malvern Instruments).
A method has been discovered that appears to provide earlier warning of organ transplant rejection compared to standard methods, and requires only a blood test rather than a more invasive and painful needle biopsy.
Approximately 30,000 organ transplants occur in the USA each year. However, depending on the organ type of the transplanted organs, between 20% and 50% fail within five years, most often because the recipient's immune system attacks, or "rejects," the donated organ.
Scientists at the Perelman School of Medicine at the University of Pennsylvania analyzed human blood and urine samples using a new method. The new method involves tiny, capsule-like structures known as exosomes, which normally are secreted from most types of cell. Precisely what exosomes evolved to do is not clear, but scientists know that these capsules contain proteins and other molecules from their mother cell that can influence the activities of neighboring cells. Like their mother cells, exosomes have protein markers on their surfaces, often called major histocompatibility complex (MHC) antigens that identify them to the immune system as part of the body. Just as donor and host cells usually differ in their MHC markers, so do donor and host exosomes.
Human pancreas was processed for islet isolation, and high-purity (>80%) islets were used for xenoislet transplantation. Islet isolation was performed and the islets were cultured in CMRL media supplemented with albumin, without any exogenous exosome contamination. Islet culture supernatant (20 mL) was obtained 24 to72 hours after isolation for exosome analysis. Exosomes were isolated from human islet culture supernatants by size exclusion limit gel chromatography along with ultracentrifugation. Exosomes were analyzed on the NanoSight NS300 (405 nm laser diode) on the light scatter mode for quantification and scatter distribution.
In an initial exploration of the transplant-exosome strategy in people, the team examined stored blood plasma samples from five recipients of transplanted islet cells in a clinical trial, and was able to detect donor exosomes in these samples following the transplants. They also found some preliminary evidence that their falling-exosome measure could be useful in predicting transplant rejection in people. For one patient who experienced a rejection of the transplanted islet cells, a steep drop in the level of donor exosomes was detectable in a blood sample taken six and a half months before the transplanted cells stopped working and the patient developed clinical signs of diabetes.
The scientists showed that they could isolate and detect donor-tissue exosomes in a different type of transplant: kidney transplant, currently the most common type of organ transplant. In this case, the team found that they could isolate and quantify donor-kidney exosomes not just in blood but also in urine, thus potentially enabling urine tests which are even less invasive than blood tests. Ali Naji, MD, PhD, a Professor of Surgery and senior author of the study said, “I believe that analyses of exosomes from transplanted organs will ultimately provide a very powerful and unprecedented ability to understand the conditional state of the organ as a whole.” The study was published on March 20, 2017, in the Journal of Clinical Investigation.
Approximately 30,000 organ transplants occur in the USA each year. However, depending on the organ type of the transplanted organs, between 20% and 50% fail within five years, most often because the recipient's immune system attacks, or "rejects," the donated organ.
Scientists at the Perelman School of Medicine at the University of Pennsylvania analyzed human blood and urine samples using a new method. The new method involves tiny, capsule-like structures known as exosomes, which normally are secreted from most types of cell. Precisely what exosomes evolved to do is not clear, but scientists know that these capsules contain proteins and other molecules from their mother cell that can influence the activities of neighboring cells. Like their mother cells, exosomes have protein markers on their surfaces, often called major histocompatibility complex (MHC) antigens that identify them to the immune system as part of the body. Just as donor and host cells usually differ in their MHC markers, so do donor and host exosomes.
Human pancreas was processed for islet isolation, and high-purity (>80%) islets were used for xenoislet transplantation. Islet isolation was performed and the islets were cultured in CMRL media supplemented with albumin, without any exogenous exosome contamination. Islet culture supernatant (20 mL) was obtained 24 to72 hours after isolation for exosome analysis. Exosomes were isolated from human islet culture supernatants by size exclusion limit gel chromatography along with ultracentrifugation. Exosomes were analyzed on the NanoSight NS300 (405 nm laser diode) on the light scatter mode for quantification and scatter distribution.
In an initial exploration of the transplant-exosome strategy in people, the team examined stored blood plasma samples from five recipients of transplanted islet cells in a clinical trial, and was able to detect donor exosomes in these samples following the transplants. They also found some preliminary evidence that their falling-exosome measure could be useful in predicting transplant rejection in people. For one patient who experienced a rejection of the transplanted islet cells, a steep drop in the level of donor exosomes was detectable in a blood sample taken six and a half months before the transplanted cells stopped working and the patient developed clinical signs of diabetes.
The scientists showed that they could isolate and detect donor-tissue exosomes in a different type of transplant: kidney transplant, currently the most common type of organ transplant. In this case, the team found that they could isolate and quantify donor-kidney exosomes not just in blood but also in urine, thus potentially enabling urine tests which are even less invasive than blood tests. Ali Naji, MD, PhD, a Professor of Surgery and senior author of the study said, “I believe that analyses of exosomes from transplanted organs will ultimately provide a very powerful and unprecedented ability to understand the conditional state of the organ as a whole.” The study was published on March 20, 2017, in the Journal of Clinical Investigation.
Latest Molecular Diagnostics News
- Digital PCR Assays Support Surveillance of Bundibugyo Ebolavirus Outbreak
- Updated Guidance Prioritizes Stool-Based Colorectal Cancer Screening Tests
- Blood-Based Proteomic Test May Predict Treatment Response in Non-Small Cell Lung Cancer
- Position Statements Outline Evidence Standards for Multi-Cancer Detection Tests
- Ultrasensitive MRD Blood Test Detects Early Breast Cancer Recurrence
- Gene Fusion Patterns May Flag High Risk Solitary Fibrous Tumors
- New RNA Origami Method Supports Faster Targeted Testing for Repeat Expansion Disorders
- FDA Approves Expanded Liquid Biopsy Panel for Advanced Cancer Profiling
- Microbial Saliva Test Could Help Triage Esophageal Cancer Risk
- Expanded DPYD Genotyping Test Supports Safer Chemotherapy Dosing
- Blood Test Detects Early Nonresponse in Metastatic Prostate Cancer
- Multi-Omics Profiling Helps Predict BCG Response and Recurrence in Bladder Cancer
- New Computational Tool Reveals Genetic Driver of Idiopathic Neuropathy
- Breast Cancer-Specific Signatures Link Genome Instability to Outcomes
- FDA-Cleared Genomic Profiling Assay Guides Treatment Selection in Solid Tumors
- ctDNA Blood Test Could Help Guide Radiotherapy in Patients with Limited Metastases
Channels
Clinical Chemistry
view channel
Urine-Based Test Shows Promise for Autism Screening in Children
Autism spectrum disorder (ASD) is commonly diagnosed through behavioral assessments, which can involve long waits that delay intervention. Earlier identification is linked to better developmental outcomes,... Read more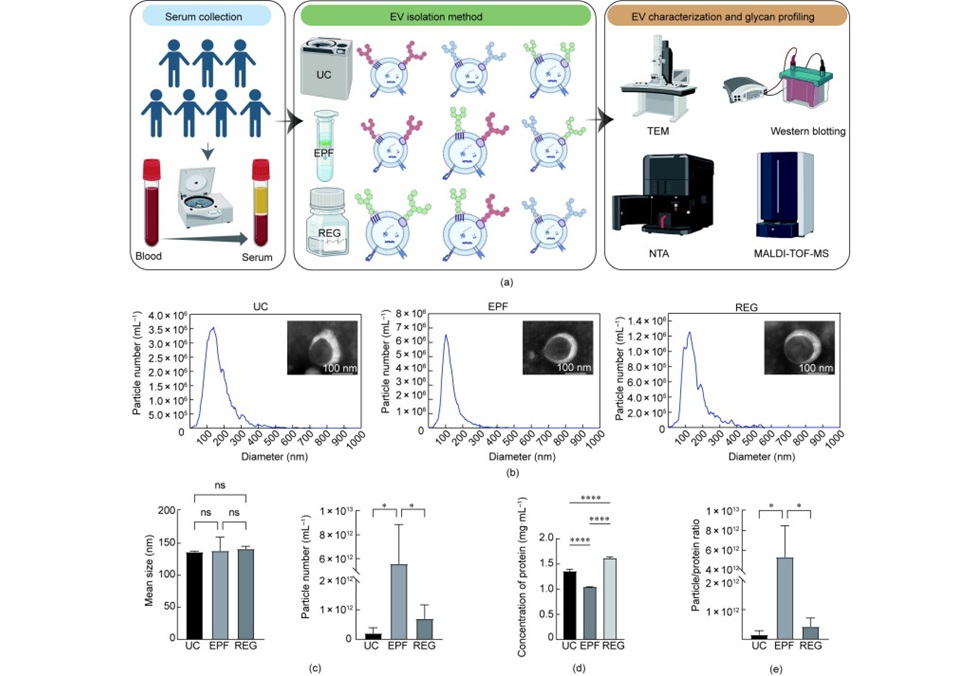
Liquid Biopsy Biomarkers May Improve Childhood Epilepsy Diagnosis
Childhood epilepsy remains a major neurological disorder with unmet needs for accurate, non-invasive biomarkers, as conventional tests such as electroencephalography and neuroimaging can have limited sensitivity... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channel
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read more
Immune Enzyme Linked to Treatment-Resistant Inflammatory Bowel Disease
Inflammatory bowel disease (IBD) affects nearly 3 million people in the United States and its prevalence continues to rise. Medications that target tumor necrosis factor (TNF)-alpha are widely used, but... Read moreMicrobiology
view channel
Gut Microbiome Signatures Help Identify Risk of IBD Progression
Inflammatory bowel disease (IBD), encompassing Crohn’s disease and ulcerative colitis, is a chronic relapsing inflammatory disorder of the gastrointestinal tract with highly variable outcomes.... Read more
FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
Clinical guidelines support testing based on patient presentation in suspected gastrointestinal infections, yet available technologies have often forced laboratories to choose between panels that are too... Read morePathology
view channel
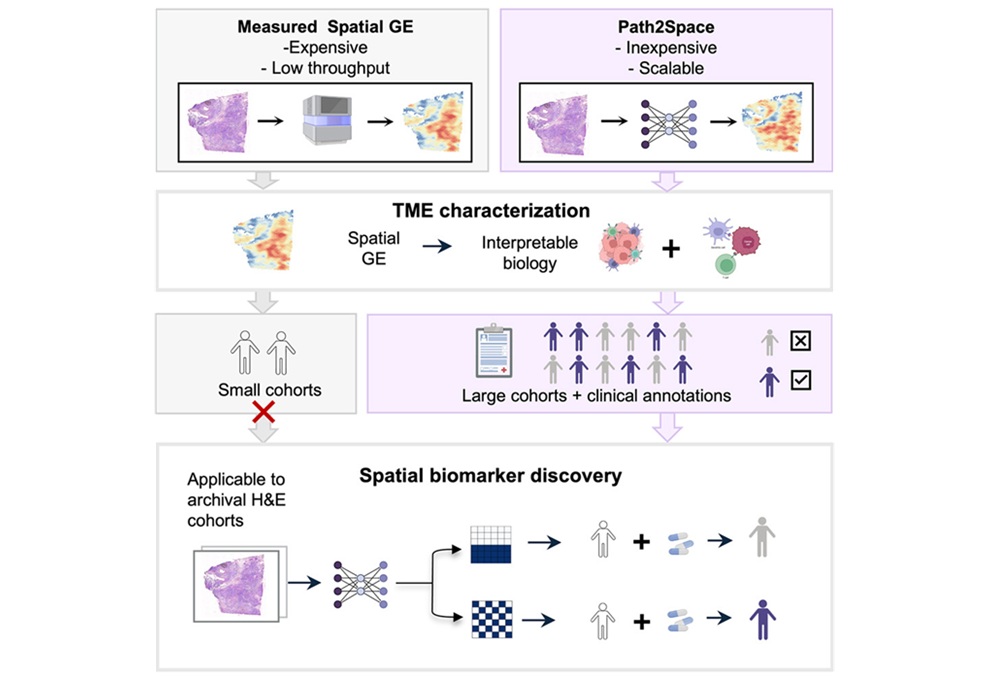
AI-Powered Atlas Maps Immune Structures Linked to Cancer Outcomes
Tertiary lymphoid structures are emerging as important indicators of antitumor immunity, but their heterogeneity and spatial context within tumors remain difficult to capture through routine diagnostics.... Read more
AI Tool Extracts Immune Signals from Biopsy to Inform Myeloma Therapy
Multiple myeloma is a bone marrow malignancy in which patients can respond very differently to the same treatments, making initial therapy decisions difficult. Clinicians must choose among options such... Read moreTechnology
view channel
Mailed Screening Kits Help Reduce Colorectal Cancer Screening Gaps
Colorectal cancer screening is a longstanding preventive priority, yet participation and follow-up remain uneven across patient groups. Safety‑net primary care settings often face barriers that limit screening... Read more
Algorithm Panel Aids Liver Fibrosis Assessment and Liver Cancer Surveillance
Chronic liver disease is common and often progresses silently, increasing the risk of cirrhosis and hepatocellular carcinoma when not detected early. With an estimated 1.5 billion people affected worldwide... Read moreIndustry
view channelWerfen and Oxford Nanopore Collaborate on Transplant Assay Development
Werfen (Barcelona, Spain), a global specialized diagnostics company, has announced a strategic collaboration with Oxford Nanopore Technologies (Oxford, UK), which develops nanopore-based sequencing technology,... Read more