New Technology Could Help Diagnose Sepsis in Hours
|
By LabMedica International staff writers Posted on 08 Nov 2016 |
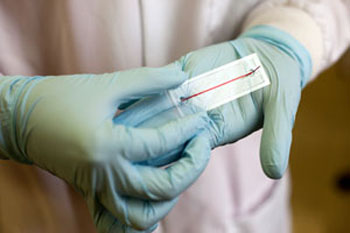
Image: A new microfluidics chip being developed for a blood test to rapidly diagnose sepsis would enable doctors to intervene sooner and as necessary, as well as to monitor treatment progress (Photo courtesy of Pappas Lab / Texas Tech University).
Researchers have developed a microfluidics chip that detected mock-sepsis conditions within a few hours, instead of at least two days by currently used methods. As sepsis left untreated can be fatal in as little as two days, a rapid blood test would provide medical professionals with a critical window of time in which to begin early antibiotics treatment of diagnosed patients.
“Normally when you detect sepsis, you do it through bacterial culture; that takes two days on the short end to 15 days on the long end. Most people die of sepsis at two days. The detection currently is on the exact same time scale as mortality, so we’re trying to speed that up,” said Dimitri Pappas, associate professor of chemistry at Texas Tech University (Lubbock, TX, USA), “Instead of the bacteria, we’re looking at the body’s immune response to those bacteria, because that’s what you really care about: the bacteria cause the infection, but it’s the body’s response that causes sepsis.” It begins with a systemic inflammatory response then progresses into sepsis and eventually septic shock, in which blood pressure plummets and organs fail.
“In the elderly, in people who are immune-compromised – people who have had surgeries, for example, or burns or they’re already fighting off infection – and in children as well, you see a runaway immune response where the body’s act of saving itself can actually be lethal,” said Prof. Pappas. When not fatal, sepsis can result in amputation of a limb or prolonged hospitalization.
Sepsis is suspected by a patient’s abnormal body temperature and rapid heart and breathing rates. “Those are all incredibly crude measurements,” said Prof. Pappas, “It leads to a lot of false positives.” Because doctors know the bacterial culture likely will take longer than a septic patient’s life span, they often order treatment immediately. “The way they treat sepsis right now is through a massive antibiotic administration,” said Prof. Pappas “That’s good, actually, but if you do it prophylactically and when it’s not needed, you’re basically helping create drug-resistant bacteria. So there’s a need to detect sepsis and to treat it but not to over treat it.”
To successfully treat septic patients, doctors need two critical pieces of information: the microorganism causing the infection and whether it can be eradicated by antibiotics. “Waiting for that information over several days is one of the main problems and reasons for the devastating outcomes,” said Dr. John Griswold, professor and chair emeritus, Department of Surgery, TTU’s Health Sciences Center, “Dr. Pappas has developed a test that should give us at least the indication of bacterial invasion within a matter of hours as opposed to days. The sooner we have an indication of microorganism invasion, the sooner we are on the path to successful treatment of these very sick patients.” Prof. Griswold added that sepsis is considered one of the most costly diseases in healthcare.
Prof. Pappas and graduate student Ye Zhang recently filed a provisional patent for a microfluidics chip that can speed up detection. “We can take a blood sample, introduce it into this chip and capture one cell type or move fluids around and add chemicals to dye the cells certain colors and do diagnostic measurements,” said Prof. Pappas.
Using their chip, a sepsis diagnosis can be confirmed in just four hours. “That rapid detection will let doctors intervene sooner and intervene when necessary, but it also allows them not just to detect it but to follow up treatment,” said Prof. Pappas, “you can follow and retest them over time to make sure the body’s response is returning to normal.”
Another advantage is that the chip requires less than a drop of blood per test. “It’s so minimal we could do this multiple times throughout the course of the treatment of the patient. If they’re not septic at hour zero, but they still look septic by other methods, we could test them in six hours and see if they’ve progressed or not,” said Prof. Pappas.
The chips are designed to detect certain white blood cells activated by the immune system to fight the infection. To this point, all testing has been done with using transformed stem cells. “We have stem cells that we transform into white blood cells, then we trick them into thinking there’s an infection. We add those infection-response blood cells to human blood in the concentrations we want and the timeframe we want,” said Prof. Pappas. The blood is then tested to see if the chip registers it as septic. “That allows us to refine the technique to make sure it’ll work, because human samples are far more variable,” he said, “Before moving to humans, we had to show it’ll work in the first place.”
“Ultimately, this type of work – for it to be successful – has to be commercialized,” he said. “It has to be out there in the hands of physicians.” The next step is to test the chip with patient blood. In collaboration with Dr. Griswold, Dr. Pappas will now begin enrolling patients.
Related Links:
Texas Tech University
“Normally when you detect sepsis, you do it through bacterial culture; that takes two days on the short end to 15 days on the long end. Most people die of sepsis at two days. The detection currently is on the exact same time scale as mortality, so we’re trying to speed that up,” said Dimitri Pappas, associate professor of chemistry at Texas Tech University (Lubbock, TX, USA), “Instead of the bacteria, we’re looking at the body’s immune response to those bacteria, because that’s what you really care about: the bacteria cause the infection, but it’s the body’s response that causes sepsis.” It begins with a systemic inflammatory response then progresses into sepsis and eventually septic shock, in which blood pressure plummets and organs fail.
“In the elderly, in people who are immune-compromised – people who have had surgeries, for example, or burns or they’re already fighting off infection – and in children as well, you see a runaway immune response where the body’s act of saving itself can actually be lethal,” said Prof. Pappas. When not fatal, sepsis can result in amputation of a limb or prolonged hospitalization.
Sepsis is suspected by a patient’s abnormal body temperature and rapid heart and breathing rates. “Those are all incredibly crude measurements,” said Prof. Pappas, “It leads to a lot of false positives.” Because doctors know the bacterial culture likely will take longer than a septic patient’s life span, they often order treatment immediately. “The way they treat sepsis right now is through a massive antibiotic administration,” said Prof. Pappas “That’s good, actually, but if you do it prophylactically and when it’s not needed, you’re basically helping create drug-resistant bacteria. So there’s a need to detect sepsis and to treat it but not to over treat it.”
To successfully treat septic patients, doctors need two critical pieces of information: the microorganism causing the infection and whether it can be eradicated by antibiotics. “Waiting for that information over several days is one of the main problems and reasons for the devastating outcomes,” said Dr. John Griswold, professor and chair emeritus, Department of Surgery, TTU’s Health Sciences Center, “Dr. Pappas has developed a test that should give us at least the indication of bacterial invasion within a matter of hours as opposed to days. The sooner we have an indication of microorganism invasion, the sooner we are on the path to successful treatment of these very sick patients.” Prof. Griswold added that sepsis is considered one of the most costly diseases in healthcare.
Prof. Pappas and graduate student Ye Zhang recently filed a provisional patent for a microfluidics chip that can speed up detection. “We can take a blood sample, introduce it into this chip and capture one cell type or move fluids around and add chemicals to dye the cells certain colors and do diagnostic measurements,” said Prof. Pappas.
Using their chip, a sepsis diagnosis can be confirmed in just four hours. “That rapid detection will let doctors intervene sooner and intervene when necessary, but it also allows them not just to detect it but to follow up treatment,” said Prof. Pappas, “you can follow and retest them over time to make sure the body’s response is returning to normal.”
Another advantage is that the chip requires less than a drop of blood per test. “It’s so minimal we could do this multiple times throughout the course of the treatment of the patient. If they’re not septic at hour zero, but they still look septic by other methods, we could test them in six hours and see if they’ve progressed or not,” said Prof. Pappas.
The chips are designed to detect certain white blood cells activated by the immune system to fight the infection. To this point, all testing has been done with using transformed stem cells. “We have stem cells that we transform into white blood cells, then we trick them into thinking there’s an infection. We add those infection-response blood cells to human blood in the concentrations we want and the timeframe we want,” said Prof. Pappas. The blood is then tested to see if the chip registers it as septic. “That allows us to refine the technique to make sure it’ll work, because human samples are far more variable,” he said, “Before moving to humans, we had to show it’ll work in the first place.”
“Ultimately, this type of work – for it to be successful – has to be commercialized,” he said. “It has to be out there in the hands of physicians.” The next step is to test the chip with patient blood. In collaboration with Dr. Griswold, Dr. Pappas will now begin enrolling patients.
Related Links:
Texas Tech University
Latest Technology News
- Algorithm Panel Aids Liver Fibrosis Assessment and Liver Cancer Surveillance
- Mailed Screening Kits Help Reduce Colorectal Cancer Screening Gaps
- AI-Enabled Assistant Unifies Molecular Workflow Planning and Support
- AI Tool Automates Validation of Laboratory Software Configuration Changes
- Point-of-Care Testing Enhances Health Literacy and Self-Management in Chronic Disease
- Fully Automated Sample-to-Insight Workflow Advances Latent TB Testing
- Tumor-on-a-Chip Platform Models Pancreatic Cancer Treatment Response
- New Platform Captures Extracellular Vesicles for Early Cancer Detection
- Microfluidic Single-Cell Assay Predicts Breast Cancer Risk
- AI Tool Predicts Non-Response to Targeted Therapy in Colorectal Cancer
- Integrated System Streamlines Pre-Analytical Workflow for Molecular Testing
- Noninvasive Sputum Test Detects Early Lung Cancer
- New AI Tool Enables Rapid Treatment Selection in Pediatric Leukemia
- Rapid Biosensor Detects Drug Sensitivity in Breast Tumors
- Breakthrough Mass Spectrometry Design Could Enable Ultra-Low Abundance Detection
- Online Tool Supports Family Screening for Inherited Cancer Risk
Channels
Clinical Chemistry
view channel
Urine-Based Test Shows Promise for Autism Screening in Children
Autism spectrum disorder (ASD) is commonly diagnosed through behavioral assessments, which can involve long waits that delay intervention. Earlier identification is linked to better developmental outcomes,... Read more
Liquid Biopsy Biomarkers May Improve Childhood Epilepsy Diagnosis
Childhood epilepsy remains a major neurological disorder with unmet needs for accurate, non-invasive biomarkers, as conventional tests such as electroencephalography and neuroimaging can have limited sensitivity... Read moreMolecular Diagnostics
view channel
Updated Guidance Prioritizes Stool-Based Colorectal Cancer Screening Tests
Colorectal cancer is the second-leading cause of cancer death in the United States and claimed an estimated 55,000 lives in 2026. Incidence is rising among adults younger than 50, even as overall mortality... Read more
Digital PCR Assays Support Surveillance of Bundibugyo Ebolavirus Outbreak
QIAGEN (Venlo, Netherlands) has introduced two custom-designed research-use-only (RUO) QIAcuity dPCR assays to support infectious disease research and surveillance connected to the Bundibugyo ebolavirus outbreak.... Read more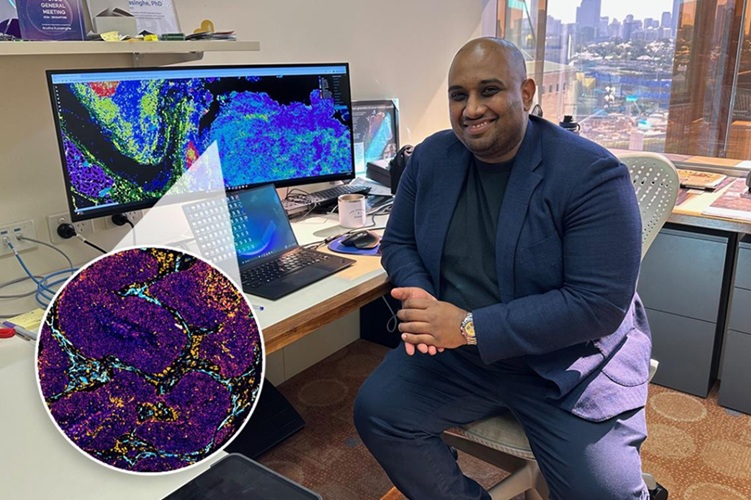
Blood-Based Proteomic Test May Predict Treatment Response in Non-Small Cell Lung Cancer
Lung cancer remains the leading cause of cancer death, with non-small cell lung cancer (NSCLC) accounting for most cases. Treatment decisions are often made without a clear indication of how a patient... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channel
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read more
Immune Enzyme Linked to Treatment-Resistant Inflammatory Bowel Disease
Inflammatory bowel disease (IBD) affects nearly 3 million people in the United States and its prevalence continues to rise. Medications that target tumor necrosis factor (TNF)-alpha are widely used, but... Read morePathology
view channel
AI-Powered Atlas Maps Immune Structures Linked to Cancer Outcomes
Tertiary lymphoid structures are emerging as important indicators of antitumor immunity, but their heterogeneity and spatial context within tumors remain difficult to capture through routine diagnostics.... Read more
AI Tool Extracts Immune Signals from Biopsy to Inform Myeloma Therapy
Multiple myeloma is a bone marrow malignancy in which patients can respond very differently to the same treatments, making initial therapy decisions difficult. Clinicians must choose among options such... Read moreTechnology
view channel
Mailed Screening Kits Help Reduce Colorectal Cancer Screening Gaps
Colorectal cancer screening is a longstanding preventive priority, yet participation and follow-up remain uneven across patient groups. Safety‑net primary care settings often face barriers that limit screening... Read more
Algorithm Panel Aids Liver Fibrosis Assessment and Liver Cancer Surveillance
Chronic liver disease is common and often progresses silently, increasing the risk of cirrhosis and hepatocellular carcinoma when not detected early. With an estimated 1.5 billion people affected worldwide... Read moreIndustry
view channelWerfen and Oxford Nanopore Collaborate on Transplant Assay Development
Werfen (Barcelona, Spain), a global specialized diagnostics company, has announced a strategic collaboration with Oxford Nanopore Technologies (Oxford, UK), which develops nanopore-based sequencing technology,... Read more