Heart Transplantation Recipients Unaffected by Donor Troponin Levels
|
By LabMedica International staff writers Posted on 14 Jul 2016 |

Image: According to new research, a blood test that leads to donor hearts being rejected may not effectively predict whether a heart transplant will succeed or fail (Photo courtesy of the AMA).
Many transplant centers routinely reject hearts if the donor’s blood test reveals elevated levels of troponin I, a protein found in heart muscle that enters the bloodstream when there is a heart attack or other heart muscle damage. Donors with previous heart disease are automatically excluded.
Heart transplantation is one of the greatest achievements in modern medicine and patients with advanced heart failure in whom survival is measured in weeks and months are offered the potential for survival of equal to or greater than 10 years with excellent quality of life.
Cardiologist at the Albert Einstein College of Medicine (Bronx, NY, USA) analyzed all adult heart transplant recipients at least 18 years of age, who received their transplants between January 1, 2007, and September 30, 2014. The study period coincides with the regular reporting of donor troponin levels by the United Network of Organ Sharing (UNOS). Of the 15,247 adult heart transplants performed in the USA from January 2007 to September 2014, 10 943 (71.8%) met all the inclusion/exclusion criteria and formed the final study cohort. There were three clinically meaningful donor troponin I groups: less than 1 ng/mL, 1 to 10 ng/mL, and more than10 ng/mL and compared mortality at 30 days, one year, three years, and five years of follow-up, primary graft failure (PGF) at 30 days, and cardiac allograft vasculopathy (CAV) of more than five years of follow-up.
The team set out to determine whether there are any differences in outcomes for patients who received a heart from a donor with high troponin I levels. At 30 days, one year, three years, and five years after heart transplantation, the scientists found no significant differences in survival between recipients whose donors had high troponin I levels and those whose levels were normal. There was also no association between donor troponin I levels and risk of recipient death one year after transplantation. Additionally, donor troponin I levels made no difference to recipients' incidence of primary graft failure, the loss of pumping action that occurs within 30 days of transplantation, and cardiac allograft vasculopathy, a form of heart disease that can limit long-term survival following heart transplantation.
Snehal R. Patel, MD, an assistant professor of medicine and the senior author of the study, said, “A lot of focus has been on finding ways to sign up more people as organ donors, but there is also a problem in that only an average of one in three donor hearts are placed. Our study shows that transplant centers should not exclude donor hearts based solely on elevated troponin I if the organ is otherwise suitable. At our institution it has already changed how we evaluate donors, and I think this data will lead to changes nationwide.” The study was published on June 21, 2016, in the journal Circulation: Heart Failure.
Related Links:
Albert Einstein College of Medicine
Heart transplantation is one of the greatest achievements in modern medicine and patients with advanced heart failure in whom survival is measured in weeks and months are offered the potential for survival of equal to or greater than 10 years with excellent quality of life.
Cardiologist at the Albert Einstein College of Medicine (Bronx, NY, USA) analyzed all adult heart transplant recipients at least 18 years of age, who received their transplants between January 1, 2007, and September 30, 2014. The study period coincides with the regular reporting of donor troponin levels by the United Network of Organ Sharing (UNOS). Of the 15,247 adult heart transplants performed in the USA from January 2007 to September 2014, 10 943 (71.8%) met all the inclusion/exclusion criteria and formed the final study cohort. There were three clinically meaningful donor troponin I groups: less than 1 ng/mL, 1 to 10 ng/mL, and more than10 ng/mL and compared mortality at 30 days, one year, three years, and five years of follow-up, primary graft failure (PGF) at 30 days, and cardiac allograft vasculopathy (CAV) of more than five years of follow-up.
The team set out to determine whether there are any differences in outcomes for patients who received a heart from a donor with high troponin I levels. At 30 days, one year, three years, and five years after heart transplantation, the scientists found no significant differences in survival between recipients whose donors had high troponin I levels and those whose levels were normal. There was also no association between donor troponin I levels and risk of recipient death one year after transplantation. Additionally, donor troponin I levels made no difference to recipients' incidence of primary graft failure, the loss of pumping action that occurs within 30 days of transplantation, and cardiac allograft vasculopathy, a form of heart disease that can limit long-term survival following heart transplantation.
Snehal R. Patel, MD, an assistant professor of medicine and the senior author of the study, said, “A lot of focus has been on finding ways to sign up more people as organ donors, but there is also a problem in that only an average of one in three donor hearts are placed. Our study shows that transplant centers should not exclude donor hearts based solely on elevated troponin I if the organ is otherwise suitable. At our institution it has already changed how we evaluate donors, and I think this data will lead to changes nationwide.” The study was published on June 21, 2016, in the journal Circulation: Heart Failure.
Related Links:
Albert Einstein College of Medicine
Latest Clinical Chem. News
- New PSA-Based Prognostic Model Improves Prostate Cancer Risk Assessment
- Extracellular Vesicles Linked to Heart Failure Risk in CKD Patients
- Study Compares Analytical Performance of Quantitative Hepatitis B Surface Antigen Assays
- Blood Test Could Predict and Identify Early Relapses in Myeloma Patients
- Compact Raman Imaging System Detects Subtle Tumor Signals
- Noninvasive Blood-Glucose Monitoring to Replace Finger Pricks for Diabetics
- POC Breath Diagnostic System to Detect Pneumonia-Causing Pathogens
- Online Tool Detects Drug Exposure Directly from Patient Samples
- Chemical Imaging Probe Could Track and Treat Prostate Cancer
- Mismatch Between Two Common Kidney Function Tests Indicates Serious Health Problems
- VOCs Show Promise for Early Multi-Cancer Detection
- Portable Raman Spectroscopy Offers Cost-Effective Kidney Disease Diagnosis at POC
- Gold Nanoparticles to Improve Accuracy of Ovarian Cancer Diagnosis
- Simultaneous Cell Isolation Technology Improves Cancer Diagnostic Accuracy
- Simple Non-Invasive Hair-Based Test Could Speed ALS Diagnosis
- Paper Strip Saliva Test Detects Elevated Uric Acid Levels Without Blood Draws
Channels
Molecular Diagnostics
view channel
Diagnostic Device Predicts Treatment Response for Brain Tumors Via Blood Test
Glioblastoma is one of the deadliest forms of brain cancer, largely because doctors have no reliable way to determine whether treatments are working in real time. Assessing therapeutic response currently... Read more
Blood Test Detects Early-Stage Cancers by Measuring Epigenetic Instability
Early-stage cancers are notoriously difficult to detect because molecular changes are subtle and often missed by existing screening tools. Many liquid biopsies rely on measuring absolute DNA methylation... Read more
“Lab-On-A-Disc” Device Paves Way for More Automated Liquid Biopsies
Extracellular vesicles (EVs) are tiny particles released by cells into the bloodstream that carry molecular information about a cell’s condition, including whether it is cancerous. However, EVs are highly... Read more
Blood Test Identifies Inflammatory Breast Cancer Patients at Increased Risk of Brain Metastasis
Brain metastasis is a frequent and devastating complication in patients with inflammatory breast cancer, an aggressive subtype with limited treatment options. Despite its high incidence, the biological... Read moreHematology
view channel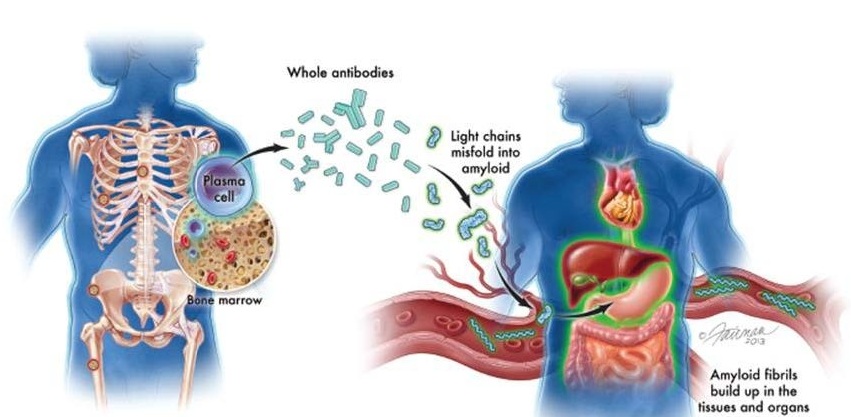
New Guidelines Aim to Improve AL Amyloidosis Diagnosis
Light chain (AL) amyloidosis is a rare, life-threatening bone marrow disorder in which abnormal amyloid proteins accumulate in organs. Approximately 3,260 people in the United States are diagnosed... Read more
Fast and Easy Test Could Revolutionize Blood Transfusions
Blood transfusions are a cornerstone of modern medicine, yet red blood cells can deteriorate quietly while sitting in cold storage for weeks. Although blood units have a fixed expiration date, cells from... Read more
Automated Hemostasis System Helps Labs of All Sizes Optimize Workflow
High-volume hemostasis sections must sustain rapid turnaround while managing reruns and reflex testing. Manual tube handling and preanalytical checks can strain staff time and increase opportunities for error.... Read more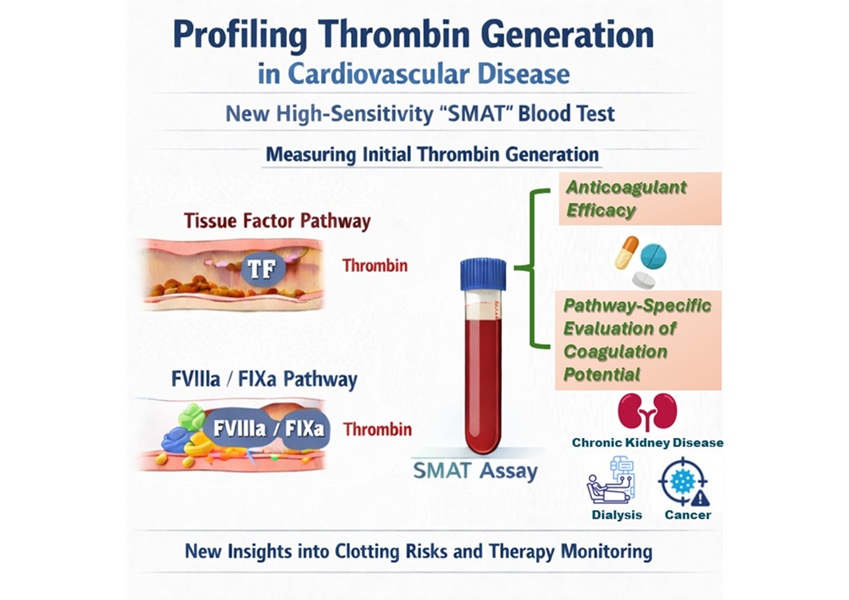
High-Sensitivity Blood Test Improves Assessment of Clotting Risk in Heart Disease Patients
Blood clotting is essential for preventing bleeding, but even small imbalances can lead to serious conditions such as thrombosis or dangerous hemorrhage. In cardiovascular disease, clinicians often struggle... Read moreImmunology
view channelBlood Test Identifies Lung Cancer Patients Who Can Benefit from Immunotherapy Drug
Small cell lung cancer (SCLC) is an aggressive disease with limited treatment options, and even newly approved immunotherapies do not benefit all patients. While immunotherapy can extend survival for some,... Read more
Whole-Genome Sequencing Approach Identifies Cancer Patients Benefitting From PARP-Inhibitor Treatment
Targeted cancer therapies such as PARP inhibitors can be highly effective, but only for patients whose tumors carry specific DNA repair defects. Identifying these patients accurately remains challenging,... Read more
Ultrasensitive Liquid Biopsy Demonstrates Efficacy in Predicting Immunotherapy Response
Immunotherapy has transformed cancer treatment, but only a small proportion of patients experience lasting benefit, with response rates often remaining between 10% and 20%. Clinicians currently lack reliable... Read moreMicrobiology
view channel
Comprehensive Review Identifies Gut Microbiome Signatures Associated With Alzheimer’s Disease
Alzheimer’s disease affects approximately 6.7 million people in the United States and nearly 50 million worldwide, yet early cognitive decline remains difficult to characterize. Increasing evidence suggests... Read moreAI-Powered Platform Enables Rapid Detection of Drug-Resistant C. Auris Pathogens
Infections caused by the pathogenic yeast Candida auris pose a significant threat to hospitalized patients, particularly those with weakened immune systems or those who have invasive medical devices.... Read morePathology
view channel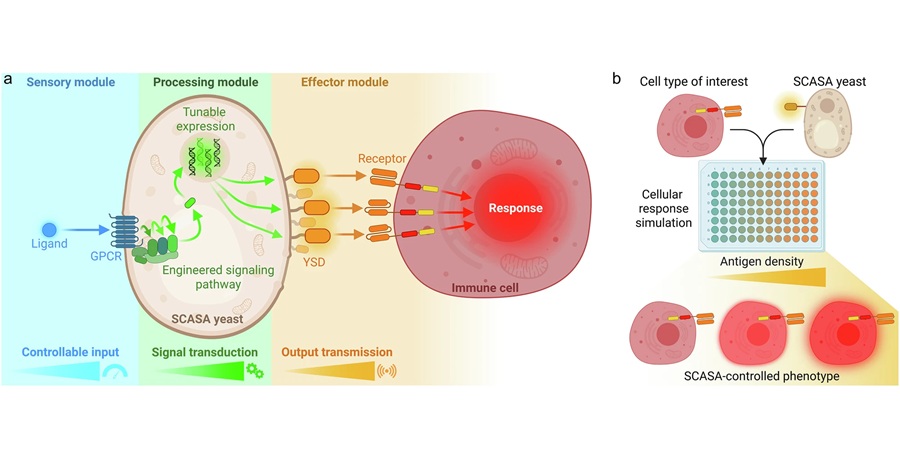
Engineered Yeast Cells Enable Rapid Testing of Cancer Immunotherapy
Developing new cancer immunotherapies is a slow, costly, and high-risk process, particularly for CAR T cell treatments that must precisely recognize cancer-specific antigens. Small differences in tumor... Read more
First-Of-Its-Kind Test Identifies Autism Risk at Birth
Autism spectrum disorder is treatable, and extensive research shows that early intervention can significantly improve cognitive, social, and behavioral outcomes. Yet in the United States, the average age... Read moreTechnology
view channel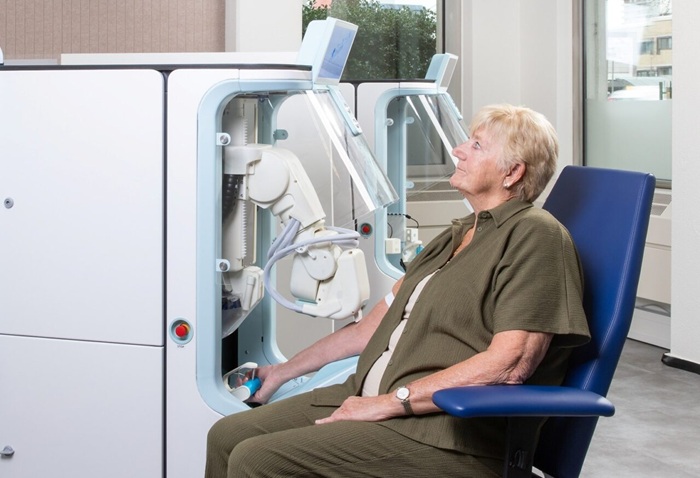
Robotic Technology Unveiled for Automated Diagnostic Blood Draws
Routine diagnostic blood collection is a high‑volume task that can strain staffing and introduce human‑dependent variability, with downstream implications for sample quality and patient experience.... Read more
ADLM Launches First-of-Its-Kind Data Science Program for Laboratory Medicine Professionals
Clinical laboratories generate billions of test results each year, creating a treasure trove of data with the potential to support more personalized testing, improve operational efficiency, and enhance patient care.... Read moreAptamer Biosensor Technology to Transform Virus Detection
Rapid and reliable virus detection is essential for controlling outbreaks, from seasonal influenza to global pandemics such as COVID-19. Conventional diagnostic methods, including cell culture, antigen... Read more
AI Models Could Predict Pre-Eclampsia and Anemia Earlier Using Routine Blood Tests
Pre-eclampsia and anemia are major contributors to maternal and child mortality worldwide, together accounting for more than half a million deaths each year and leaving millions with long-term health complications.... Read moreIndustry
view channelNew Collaboration Brings Automated Mass Spectrometry to Routine Laboratory Testing
Mass spectrometry is a powerful analytical technique that identifies and quantifies molecules based on their mass and electrical charge. Its high selectivity, sensitivity, and accuracy make it indispensable... Read more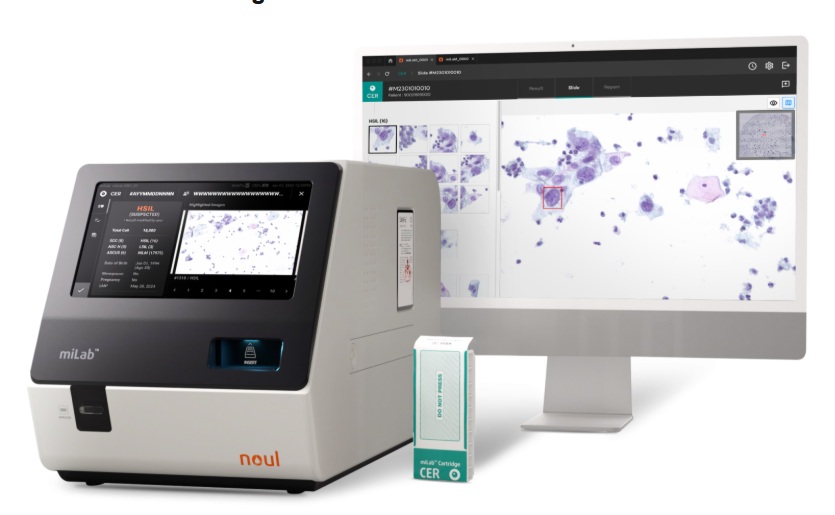
AI-Powered Cervical Cancer Test Set for Major Rollout in Latin America
Noul Co., a Korean company specializing in AI-based blood and cancer diagnostics, announced it will supply its intelligence (AI)-based miLab CER cervical cancer diagnostic solution to Mexico under a multi‑year... Read more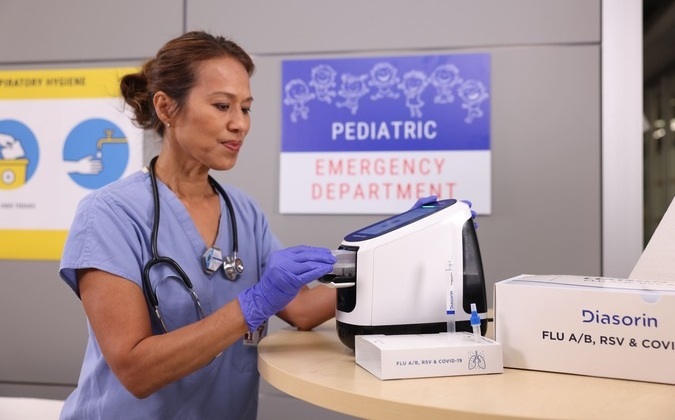
Diasorin and Fisher Scientific Enter into US Distribution Agreement for Molecular POC Platform
Diasorin (Saluggia, Italy) has entered into an exclusive distribution agreement with Fisher Scientific, part of Thermo Fisher Scientific (Waltham, MA, USA), for the LIAISON NES molecular point-of-care... Read more