Autoantibodies Are Early Diabetes Warning Signs
|
By LabMedica International staff writers Posted on 09 Mar 2015 |
Detection of autoantibodies directed against pancreatic islet cells can be used to predict the likelihood of a child developing type I diabetes.
Investigators at Lund University (Sweden) recruited 8,503 participants in the TEDDY (The Environmental Determinants of Diabetes in the Young) study to take part in their autoantibody experiment. The TEDDY study, funded by the [US] National Institutes of Health, involved 8,600 children from Sweden, the USA, Finland, and Germany, who showed an increased hereditary risk of type I diabetes, detected at birth through tests on umbilical cord blood.
Infants with HLA-DR high-risk genotypes (DR3/4, DR4/4, DR4/8, and DR3/3) from the TEDDY group were prospectively followed with standardized autoantibody assessments quarterly throughout the first four years of life and then semiannually thereafter. The Lund University researchers reported that 6.5% of the participating children had their first autoantibody before the age of six. In 44% of cases, they only had an autoantibody against insulin (IAA). Most of them had this by the age of one to two years. In 38% of cases, GAD65 autoantibodies (GADA) were detected. The numbers increased until the age of two and then remained constant. In 14% of cases both autoantibodies were found at the same time, with a peak at the age of two to three.
The investigators concluded from the results that there were three ways to predict development of type I diabetes: 1) if the autoantibody first discovered attacked insulin (IAA); 2) if the first autoantibody targeted GAD65 (GADA), a protein inside the insulin-producing cells; or 3) if both autoantibodies were first found together.
"In the TEDDY study we have found that autoantibodies often appear during the first few years of life", said contributing author Dr. Åke Lernmark, professor of experimental diabetes at Lund University. "If a second autoantibody is detected later, then the person will get diabetes - but it may take up to 20 years. In TEDDY, 40% of these children had already developed diabetes. It is possible that there are two different diseases involved. Perhaps one virus triggers the autoantibodies against insulin and another one the autoantibodies against GAD65."
The study was published in the February 10, 2015, online edition of the journal Diabetologia.
Related Links:
Lund University
Investigators at Lund University (Sweden) recruited 8,503 participants in the TEDDY (The Environmental Determinants of Diabetes in the Young) study to take part in their autoantibody experiment. The TEDDY study, funded by the [US] National Institutes of Health, involved 8,600 children from Sweden, the USA, Finland, and Germany, who showed an increased hereditary risk of type I diabetes, detected at birth through tests on umbilical cord blood.
Infants with HLA-DR high-risk genotypes (DR3/4, DR4/4, DR4/8, and DR3/3) from the TEDDY group were prospectively followed with standardized autoantibody assessments quarterly throughout the first four years of life and then semiannually thereafter. The Lund University researchers reported that 6.5% of the participating children had their first autoantibody before the age of six. In 44% of cases, they only had an autoantibody against insulin (IAA). Most of them had this by the age of one to two years. In 38% of cases, GAD65 autoantibodies (GADA) were detected. The numbers increased until the age of two and then remained constant. In 14% of cases both autoantibodies were found at the same time, with a peak at the age of two to three.
The investigators concluded from the results that there were three ways to predict development of type I diabetes: 1) if the autoantibody first discovered attacked insulin (IAA); 2) if the first autoantibody targeted GAD65 (GADA), a protein inside the insulin-producing cells; or 3) if both autoantibodies were first found together.
"In the TEDDY study we have found that autoantibodies often appear during the first few years of life", said contributing author Dr. Åke Lernmark, professor of experimental diabetes at Lund University. "If a second autoantibody is detected later, then the person will get diabetes - but it may take up to 20 years. In TEDDY, 40% of these children had already developed diabetes. It is possible that there are two different diseases involved. Perhaps one virus triggers the autoantibodies against insulin and another one the autoantibodies against GAD65."
The study was published in the February 10, 2015, online edition of the journal Diabetologia.
Related Links:
Lund University
Latest Clinical Chem. News
- Saliva-Based Test Detects Biochemical Signs of Sleep Loss
- Simple Dual-Tau Blood Test Detects and Stages Alzheimer’s Disease
- Alzheimer’s Blood Biomarkers Linked to Early Cognitive Differences Before Dementia
- Urine-Based Test Shows Promise for Autism Screening in Children
- Blood-Based Sensor Detects Early Signs of Alzheimer’s and Parkinson’s
- Liquid Biopsy Biomarkers May Improve Childhood Epilepsy Diagnosis
- Urine-Based Alzheimer’s Test Receives FDA Breakthrough Device Designation
- Fluid Biomarker Improves Diagnosis and Monitoring of Primary CNS Lymphoma
- New CA19-9 Cutoff Value Helps Identify High-Risk Pancreatic Cancer Patients
- Blood-Based Biomarkers Show Promise for Psychosis Risk Prediction
- International Experts Recommend Ending Routine 'Corrected' Calcium Reporting
- Long-Term Data Show PSA Screening Modestly Reduces Prostate Cancer Deaths
- Urine-Based Nanosensor Tracks Lung Cancer and Fibrosis Noninvasively
- FDA-Cleared Assay Enables Comprehensive Automated Testosterone Testing
- CE-Marked Blood Biomarker Test Advances Automated Alzheimer’s Diagnostics
- Blood-Based Alzheimer’s Test Gains CE Mark for Amyloid Pathology Detection
Channels
Molecular Diagnostics
view channel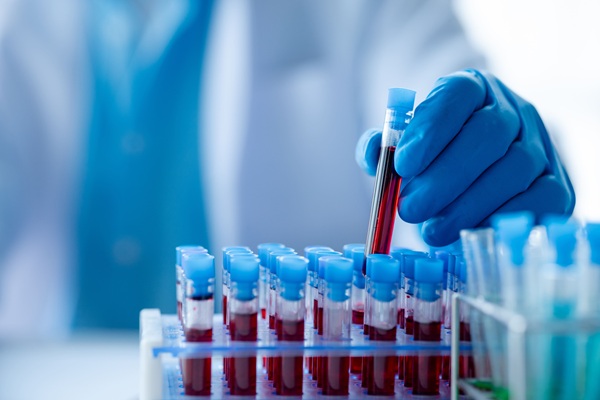
Blood Test Predicts Immunotherapy Response in Head and Neck Cancer
Head and neck squamous cell carcinoma affects hundreds of thousands of people worldwide each year, yet response rates to immunotherapy remain low. Clinicians lack reliable, minimally invasive tools to... Read more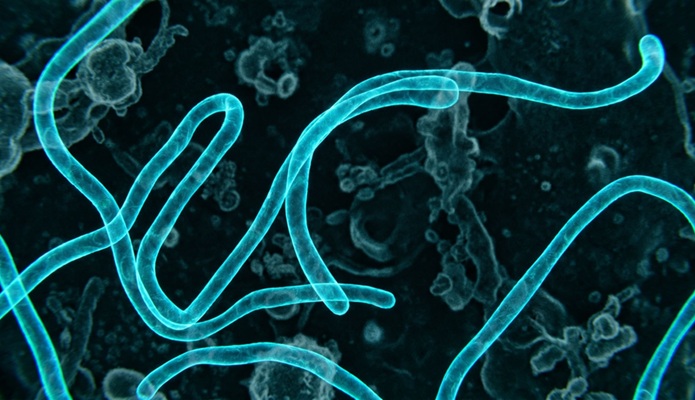
New PCR Assay Supports Bundibugyo Ebola Outbreak Surveillance
Rapid identification of Ebola infections is essential to limit transmission and guide public health response, yet detection can be difficult when outbreaks involve rare variants. The current outbreaks... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channelAptamer-Based Biosensor Enables Mutation-Resilient SARS-CoV-2 Detection
Rapid evolution of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can undermine existing molecular diagnostics, especially when assays target small viral components. Double-antibody sandwich... Read more
Study Points to Autoimmune Pathway Behind Long COVID Symptoms
Long COVID leaves many SARS-CoV-2 survivors with persistent fatigue, cognitive issues, palpitations, and musculoskeletal pain for months or years. Estimates cited in new research suggest 4%–20% of infected... Read more
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read moreMicrobiology
view channel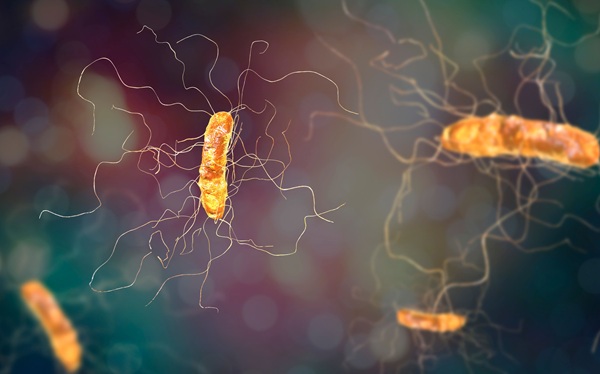
New Culture Medium Speeds C. difficile Resistance Detection and Reduces Costs
Clostridioides difficile infections remain a persistent threat in hospitals and communities, affecting about 500,000 people in the United States each year. Severe cases can be fatal within 30 days of diagnosis,... Read more
Automated Blood Culture System Speeds Detection of Bloodstream Infections
Bloodstream infections and sepsis require rapid laboratory detection to guide targeted antimicrobial therapy and reduce mortality. Conventional blood culture workflows can delay actionable results by critical... Read morePathology
view channel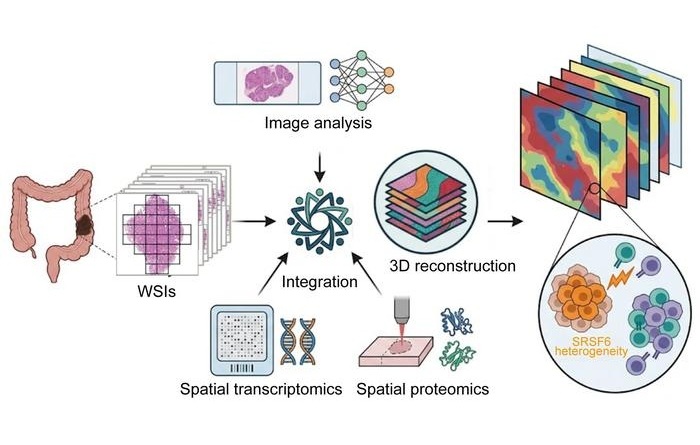
3D Spatial Multi-Omics Maps Intra-Tumor Diversity in Colorectal Cancer
Colorectal cancer remains a leading cause of cancer death, and clinical decision-making is complicated by marked intra-tumor heterogeneity. Conventional bulk sequencing averages molecular signals across... Read more
Blood-Based Method Tracks Gene Activity in the Living Brain
Real-time measurement of gene activity in the brain has been limited by assays requiring destructive tissue sampling. Tracking active genes could reveal how the body responds to environmental factors,... Read moreTechnology
view channel
AI Platform Links Biomarker Results to Cancer Clinical Trials and Guidelines
Oncology teams must manage growing volumes of genomic data, rapidly evolving clinical trial options, and frequently updated care guidelines, all within tight clinic schedules. Translating complex tumor... Read more
Agentic AI Platform Supports Genomic Decision-Making in Oncology
Oncology care teams increasingly face the challenge of managing complex molecular diagnostics, evolving treatment options, and extensive electronic health record documentation. Translating multimodal data... Read moreIndustry
view channel
Collaboration Advances ctDNA-Guided Development in Metastatic Colorectal Cancer
Natera, Inc. (Austin, TX, USA) and CytoDyn Inc. (Vancouver, WA, USA) announced a strategic collaboration focused on metastatic colorectal cancer (mCRC). Under the agreement, Natera will evaluate circulating... Read more