Infection Can Lead to False Negatives for Cerebrospinal Fluid β-2 Transferrin
|
By LabMedica International staff writers Posted on 21 Oct 2014 |
![Image: Scanning Electron Micrograph of Streptococcus pneumoniae by R. Facklam, J. Carr. Cerebrospinal fluid (CSF) β-2 transferrin detection decreases after inoculation with live or ciprofloxacin-inactived S. pneumoniae. This may be due to passive adsorption via distinctive features of the S. pneumoniae cell wall not present in the other bacterial species examined (Photo courtesy of MicrobeWiki and the CDC – [US] Centers for Disease Control and Prevention). Image: Scanning Electron Micrograph of Streptococcus pneumoniae by R. Facklam, J. Carr. Cerebrospinal fluid (CSF) β-2 transferrin detection decreases after inoculation with live or ciprofloxacin-inactived S. pneumoniae. This may be due to passive adsorption via distinctive features of the S. pneumoniae cell wall not present in the other bacterial species examined (Photo courtesy of MicrobeWiki and the CDC – [US] Centers for Disease Control and Prevention).](https://globetechcdn.com/mobile_labmedica/images/stories/articles/article_images/2014-10-21/MMS-117.jpg)
Image: Scanning Electron Micrograph of Streptococcus pneumoniae by R. Facklam, J. Carr. Cerebrospinal fluid (CSF) β-2 transferrin detection decreases after inoculation with live or ciprofloxacin-inactived S. pneumoniae. This may be due to passive adsorption via distinctive features of the S. pneumoniae cell wall not present in the other bacterial species examined (Photo courtesy of MicrobeWiki and the CDC – [US] Centers for Disease Control and Prevention).
Researchers have found that the presence of Streptococcus pneumoniae in cerebrospinal fluid (CSF) can lead to false-negative β-2 transferrin (β2TRNSF) test results and misdiagnosis that may detrimentally affect healthcare decisions for patients.
Free passage of bacterial flora from the nasal cavity and paranasal sinuses through a CSF fistula into the cranium may pose increased risk for meningitis and encephalitis. Thus, early diagnosis and treatment of CSF leakage could decrease the risk of a lethal infection. Although β2TRNSF is a highly reliable marker for diagnosing cases of CSF leakage (even in CSF contaminated with blood or other secretions)—it has not been examined in the presence of central nervous system bacterial infection.
In a prospective analysis, a team led by Nir Hirshoren, MD, at the Hebrew University School of Medicine–Hadassah Medical Center (Jerusalem, Israel) examined β2TRNSFdetection in artificially contaminated CSF as a research model. Sterile (tested for sterility) CSF was drawn from 9 prospectively-recruited neurosurgical patients. CSF samples were contaminated in vitro by controlled spiking with bacteria, chosen for ability to cause meningeal neurosurgical-related infections: Streptococcus pneumoniae, methicillin-sensitive Staphylococcus aureus (MSSA), Staphylococcus epidermidis, or Pseudomonas aeruginosa.
β2TRNSF analysis was performed using qualitative immunoblotting electrophoresis and quantitative enzyme-linked immunosorbent assay (ELISA). Two time points were examined, following immediate inoculation (t0 ) and following an overnight incubation (t18 ), over various bacterial-load concentrations. In this study, only S. pneumoniae was observed to significantly affect β2TRNSF detection. At both the t0 and t18 time points following S. pneumoniae inoculation, β2TRNSF was not detected when immunoblotting electrophoresis was used; quantitative analysis using ELISA demonstrated significant β2TRNSF concentration decrease.
A secondary objective of the study was to explore whether the disappearance of β2TRNSF in the assays is due to a passive or active mechanism. The researchers suspected that in some cases of bacterial infections, β2TRNSF might be adsorbed, degraded, or consumed by bacteria. CSF inoculated with S. pneumoniae was also examined in the presence of the non-cell-wall antibiotic ciprofloxacin, which led to the same results. Since β2TRNSF detection decreased also with inactivated (i.e. + ciprofloxacin) S. pneumoniae, a passive process was suggested, possibly due to adsorption via distinctive features of the S. pneumoniae cell wall not present in the other species examined.
The authors note that although the study was limited by a small sample number (n=9), potential bias was largely overcome by exploring different bacterial loads, examining diverse clinical bacterial species, and using two reliable assays. Further investigation in the clinical setting is needed, however the results indicate that, in the presence of a S. pneumoniae cerebral nervous system infection, using a β2TRNSF test for CFS leak detection may be deceiving and should be interpreted cautiously.
The authors further caution that the importance of β2TRNSF assays is limited to borderline, clinical-uncertainty cases. In other cases, a β2TRNSF negative result may not change a clinical decision regardless of CSF S. pneumoniae presence, and appropriate imaging modalities and surgery may be warranted anyway.
The study was reported by Korem M. et al. in the journal Laryngoscope, September 29, 2014, online ahead of print.
Related Links:
Hebrew University School of Medicine – Hadassah Medical Center
Hebrew University Hadassah Medical School
Free passage of bacterial flora from the nasal cavity and paranasal sinuses through a CSF fistula into the cranium may pose increased risk for meningitis and encephalitis. Thus, early diagnosis and treatment of CSF leakage could decrease the risk of a lethal infection. Although β2TRNSF is a highly reliable marker for diagnosing cases of CSF leakage (even in CSF contaminated with blood or other secretions)—it has not been examined in the presence of central nervous system bacterial infection.
In a prospective analysis, a team led by Nir Hirshoren, MD, at the Hebrew University School of Medicine–Hadassah Medical Center (Jerusalem, Israel) examined β2TRNSFdetection in artificially contaminated CSF as a research model. Sterile (tested for sterility) CSF was drawn from 9 prospectively-recruited neurosurgical patients. CSF samples were contaminated in vitro by controlled spiking with bacteria, chosen for ability to cause meningeal neurosurgical-related infections: Streptococcus pneumoniae, methicillin-sensitive Staphylococcus aureus (MSSA), Staphylococcus epidermidis, or Pseudomonas aeruginosa.
β2TRNSF analysis was performed using qualitative immunoblotting electrophoresis and quantitative enzyme-linked immunosorbent assay (ELISA). Two time points were examined, following immediate inoculation (t0 ) and following an overnight incubation (t18 ), over various bacterial-load concentrations. In this study, only S. pneumoniae was observed to significantly affect β2TRNSF detection. At both the t0 and t18 time points following S. pneumoniae inoculation, β2TRNSF was not detected when immunoblotting electrophoresis was used; quantitative analysis using ELISA demonstrated significant β2TRNSF concentration decrease.
A secondary objective of the study was to explore whether the disappearance of β2TRNSF in the assays is due to a passive or active mechanism. The researchers suspected that in some cases of bacterial infections, β2TRNSF might be adsorbed, degraded, or consumed by bacteria. CSF inoculated with S. pneumoniae was also examined in the presence of the non-cell-wall antibiotic ciprofloxacin, which led to the same results. Since β2TRNSF detection decreased also with inactivated (i.e. + ciprofloxacin) S. pneumoniae, a passive process was suggested, possibly due to adsorption via distinctive features of the S. pneumoniae cell wall not present in the other species examined.
The authors note that although the study was limited by a small sample number (n=9), potential bias was largely overcome by exploring different bacterial loads, examining diverse clinical bacterial species, and using two reliable assays. Further investigation in the clinical setting is needed, however the results indicate that, in the presence of a S. pneumoniae cerebral nervous system infection, using a β2TRNSF test for CFS leak detection may be deceiving and should be interpreted cautiously.
The authors further caution that the importance of β2TRNSF assays is limited to borderline, clinical-uncertainty cases. In other cases, a β2TRNSF negative result may not change a clinical decision regardless of CSF S. pneumoniae presence, and appropriate imaging modalities and surgery may be warranted anyway.
The study was reported by Korem M. et al. in the journal Laryngoscope, September 29, 2014, online ahead of print.
Related Links:
Hebrew University School of Medicine – Hadassah Medical Center
Hebrew University Hadassah Medical School
Latest Microbiology News
- Gut Microbiome Signatures Help Identify Risk of IBD Progression
- FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
- New AMR Assay Supports Rapid Infection Control Screening in Hospitals
- Diagnostic Gaps Complicate Bundibugyo Ebola Outbreak Response in Congo
- Study Finds Hidden Mpox Infections May Drive Ongoing Spread
- Large-Scale Genomic Surveillance Tracks Resistant Bacteria Across European Hospitals
- Molecular Urine and Stool Tests Do Not Improve Early TB Treatment in Hospitalized HIV Patients
- Rapid Antigen Biosensor Detects Active Tuberculosis in One Hour
- Label-Free Microscopy Method Enables Faster, Quantitative Detection of Malaria
- Oral–Gut Microbiome Signatures Identify Early Gastric Cancer
- Gut Microbiome Test Predicts Melanoma Recurrence After Surgery
- Rapid Blood-Culture Susceptibility Panel Expands Coverage for Gram-Negative Infections
- Antibiotic Resistance Genes Found in Newborns Within Hours of Birth
- Rapid Color Test Stratifies Virulent and Resistant Staph Strains
- mNGS CSF Test Identifies CNS Pathogens Missed by Standard Panels
- Syndromic Panel Enables Rapid Identification of Bloodstream Infections
Channels
Clinical Chemistry
view channel
Saliva-Based Test Detects Biochemical Signs of Sleep Loss
Acute sleep loss impairs cognition and motor skills, raising safety risks that resemble alcohol intoxication. Clinicians currently lack an objective biochemical test to determine when someone is dangerously... Read more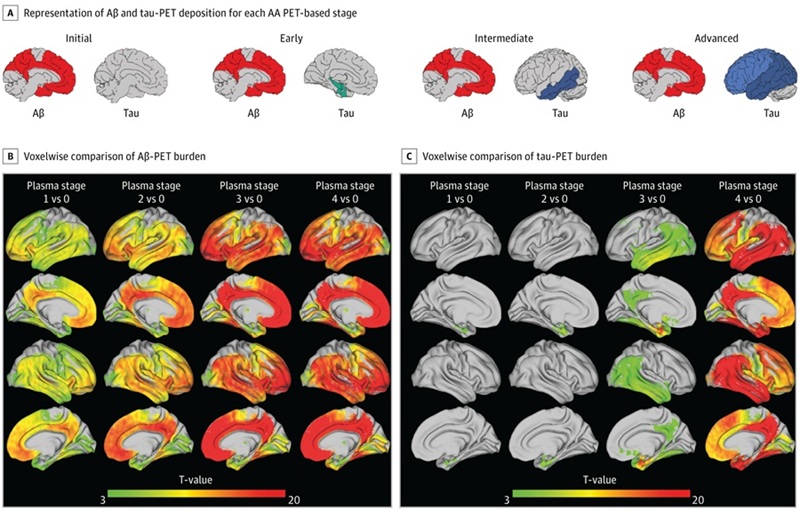
Simple Dual-Tau Blood Test Detects and Stages Alzheimer’s Disease
Alzheimer’s disease is typically confirmed and staged with positron emission tomography scans and cerebrospinal fluid testing, procedures that are costly and invasive. Broader access to minimally invasive... Read more
Alzheimer’s Blood Biomarkers Linked to Early Cognitive Differences Before Dementia
Blood-based screening for Alzheimer’s disease offers a noninvasive, lower-cost alternative to brain imaging or spinal fluid testing, yet its ability to flag the earliest cognitive changes has been unclear.... Read moreMolecular Diagnostics
view channel
Circulating Tumor DNA Testing Guides Chemotherapy, Reduces Relapse in Colon Cancer
Adjuvant therapy decisions after curative surgery for colon cancer remain difficult, as conventional clinicopathologic factors often fail to capture residual disease risk. Liquid biopsy approaches that... Read more
Researchers Uncover Distinct Chromosome Signature in Aggresive ALT Cancers
A subset of cancers rely on alternative lengthening of telomeres, a pathway associated with genomic instability and difficult-to-treat disease. These tumors span multiple cancer types and account for about... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channelAptamer-Based Biosensor Enables Mutation-Resilient SARS-CoV-2 Detection
Rapid evolution of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can undermine existing molecular diagnostics, especially when assays target small viral components. Double-antibody sandwich... Read more
Study Points to Autoimmune Pathway Behind Long COVID Symptoms
Long COVID leaves many SARS-CoV-2 survivors with persistent fatigue, cognitive issues, palpitations, and musculoskeletal pain for months or years. Estimates cited in new research suggest 4%–20% of infected... Read more
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read morePathology
view channel
Blood-Based Method Tracks Gene Activity in the Living Brain
Real-time measurement of gene activity in the brain has been limited by assays requiring destructive tissue sampling. Tracking active genes could reveal how the body responds to environmental factors,... Read more
FDA Approval Expands Automated PD-L1 Testing Across Solid Tumors
Clinical laboratories play a central role in guiding immunotherapy by reporting programmed death ligand-1 (PD‑L1) status across multiple solid tumors. Many sites are standardizing this work on fully automated... Read moreTechnology
view channel
AI Platform Links Biomarker Results to Cancer Clinical Trials and Guidelines
Oncology teams must manage growing volumes of genomic data, rapidly evolving clinical trial options, and frequently updated care guidelines, all within tight clinic schedules. Translating complex tumor... Read more
Agentic AI Platform Supports Genomic Decision-Making in Oncology
Oncology care teams increasingly face the challenge of managing complex molecular diagnostics, evolving treatment options, and extensive electronic health record documentation. Translating multimodal data... Read moreIndustry
view channel