Unified Approach Could Prevent Unnecessary Blood Tests in PICU without Increasing Sepsis Risk
|
By LabMedica International staff writers Posted on 03 May 2022 |
When a patient in the pediatric intensive care unit (PICU) develops a fever, physicians often routinely order a blood culture to identify the cause, particularly if they have reason to worry about sepsis, a life-threatening condition that occurs when chemicals released by immune system cells in the bloodstream to fight an infection trigger inflammation and shock throughout the body. However, repeated blood draws along with the use of antibiotics while awaiting culture results contribute to a rise in antibiotic resistance, leading to additional testing and extending the hospital length of stay. Now, researchers have developed and demonstrated the safety of a decision support program that appears to substantially reduce the number of blood draws in the PICU, and is likely to reduce antibiotic prescriptions without increasing the risk of sepsis.
The new study which was a national collaborative of 14 institutions and their experts, including researchers at Johns Hopkins University (Baltimore, MD, USA), builds on programs already in place that have safely reduced the use of other diagnostic tests, such as urine cultures. According to data from the U.S. Centers for Disease Control and Prevention, about 30% of antibiotics used in hospitals are unnecessary or prescribed incorrectly. Previous studies from other researchers have found that more than half of patients in the PICU often receive antibiotics for symptoms such as fever that may arise from noninfectious illnesses or even weaning from some medications.
In their study, the research team at Johns Hopkins Children’s Center led a national multidisciplinary collaborative of experts in pediatric infectious diseases, critical care medicine, quality improvement and other fields called BrighT STAR (Testing STewardship to reduce Antibiotic Resistance). The goal was to explore and compare existing studies and practices, and produce guidance recommendations to reduce blood draws in patients with low suspicion or risk for sepsis, and to measure the impact of the algorithm on blood culture rates, broad-spectrum antibiotic use and other patient outcomes. The 14 participating sites were diverse with respect to institution size, patient population and geographic area. Johns Hopkins Medicine investigators provided each site, which had its own team of experts, with a pre-implementation assessment tool while coaching them to launch their own quality improvement programs and strategies to execute the plans.
While the composition of the clinical support tools varied, each institution sought to standardize practices across its unit and reduce variability in decisions in ordering blood cultures, as well as highlight patient safety considerations. Blood culture rates, along with other measures, were tracked and reported monthly. The coordinating team held regular calls with individual sites and the larger collaborative throughout all steps of the project, conducted between 2017 and 2020.
In the 24-month period prior to implementation of the quality improvement algorithms, 41,731 blood cultures were performed at all 14 sites, compared with 22,408 cultures in the 18-month post-implementation period. Across sites, the median blood culture rate dropped from 146 per 1,000 patient days/month before implementation to 99 per 1,000 patient days/month after. Overall, 13 of 14 sites reduced their blood culture rates in the post-implementation period between 15% and 58%. Across the 14 sites, the blood culture rate was reduced by an average of 34% between the study’s pre- and post-implementation time frames (156.9 blood cultures per 1,000 patient days/month to 104.1 blood cultures per 1,000 patient days/month).
In the 11 sites that reported on antibiotic use, results showed a 13% overall average reduction in the amount of antibiotics prescribed (506.0 versus 440.3 total days per 1,000 patient days/month). At all 14 sites, central line-associated bloodstream infections decreased by 36% (1.79 to 1.14 per 1,000 central line days/month). There was no significant change in the rates of one of the most frequent and dangerous hospital-acquired infections, Clostridioides difficile (0.38 vs. 0.36 infections per 1,000 patient days/month). Mortality rates, length of stay and readmission in the PICU, as well as overall hospital readmissions, were similar before and after program implementation.
The research team has cautioned that the study may have missed instances in which antibiotics were prescribed without collecting blood cultures, which could have increased the amount prescribed. Also, all sites enrolled in the study had clinicians and others experienced in quality improvement. The researchers additionally say their analyses do not account for variations in individual site implementation plans. However, they believe their concept will help change clinician decision-making and, ultimately, benefit patients. The researchers are seeking to expand and implement a similar approach at all hospitals across the nation. They are also investigating ways to scale this concept to other hospital units, including those caring for adults.
“These findings suggest that multidisciplinary efforts to standardize blood culture collection and avoid unnecessary testing in the PICU can be done successfully and safely in diverse settings, and that reducing blood culture use can, in turn, reduce broad-spectrum antibiotic use,” said pediatric infectious diseases specialist Aaron Milstone, M.D., M.H.S., who is also a professor of pediatrics at the Johns Hopkins University School of Medicine and an expert on systems designed to prevent hospital-acquired infections and improve patient safety.
Related Links:
Johns Hopkins University
Latest Microbiology News
- New AMR Assay Supports Rapid Infection Control Screening in Hospitals
- Diagnostic Gaps Complicate Bundibugyo Ebola Outbreak Response in Congo
- Study Finds Hidden Mpox Infections May Drive Ongoing Spread
- Large-Scale Genomic Surveillance Tracks Resistant Bacteria Across European Hospitals
- Molecular Urine and Stool Tests Do Not Improve Early TB Treatment in Hospitalized HIV Patients
- Rapid Antigen Biosensor Detects Active Tuberculosis in One Hour
- Label-Free Microscopy Method Enables Faster, Quantitative Detection of Malaria
- Oral–Gut Microbiome Signatures Identify Early Gastric Cancer
- Gut Microbiome Test Predicts Melanoma Recurrence After Surgery
- Rapid Blood-Culture Susceptibility Panel Expands Coverage for Gram-Negative Infections
- Antibiotic Resistance Genes Found in Newborns Within Hours of Birth
- Rapid Color Test Stratifies Virulent and Resistant Staph Strains
- mNGS CSF Test Identifies CNS Pathogens Missed by Standard Panels
- Syndromic Panel Enables Rapid Identification of Bloodstream Infections
- RNA-Based Workflow Identifies Active Skin Microbes for Dermatology Research
- Cost-Effective Sampling and Sequencing Workflow Identifies ICU Infection Hotspots
Channels
Clinical Chemistry
view channel
New CA19-9 Cutoff Value Helps Identify High-Risk Pancreatic Cancer Patients
Pancreatic ductal adenocarcinoma (PDAC) is frequently diagnosed at an advanced stage and remains one of the most lethal solid tumors. Clinicians commonly use serum carbohydrate antigen 19-9 (CA19-9) to... Read more
Blood-Based Biomarkers Show Promise for Psychosis Risk Prediction
Psychosis commonly emerges in adolescence or early adulthood and can severely disrupt social and occupational functioning. Hallucinations, delusions, and disorganized thinking often evolve gradually, hindering... Read moreMolecular Diagnostics
view channel
New RNA Origami Method Supports Faster Targeted Testing for Repeat Expansion Disorders
Repeat expansion disorders drive conditions such as myotonic dystrophy, Huntington’s disease, and amyotrophic lateral sclerosis (ALS), yet accurately sizing the mutated sequences remains difficult.... Read more
FDA Approves Expanded Liquid Biopsy Panel for Advanced Cancer Profiling
Timely, comprehensive tumor profiling helps clinicians make treatment selection decisions for patients with advanced cancer. Blood-based approaches can provide actionable insights from a simple draw and... Read moreHematology
view channel
Higher Ferritin Threshold May Improve Iron Deficiency Detection in Children
Iron deficiency in school-age children can affect brain development, learning, growth, and physical performance, yet early deficiency may be missed when screening focuses mainly on anemia.... Read more
Stem Cell Biomarkers May Guide Precision Treatment in Acute Myeloid Leukemia
Acute myeloid leukemia (AML) is an aggressive blood cancer that most often affects older adults and still carries a poor prognosis despite therapeutic advances. Venetoclax-based regimens have improved... Read moreImmunology
view channel
Immune Enzyme Linked to Treatment-Resistant Inflammatory Bowel Disease
Inflammatory bowel disease (IBD) affects nearly 3 million people in the United States and its prevalence continues to rise. Medications that target tumor necrosis factor (TNF)-alpha are widely used, but... Read more
Simple Blood Test Could Replace Biopsies for Lung Transplant Rejection Monitoring
Lung transplant recipients face some of the highest rates of acute cellular rejection, and routine surveillance often relies on repeated surgical biopsies. These procedures can cause complications such... Read moreMicrobiology
view channel
New AMR Assay Supports Rapid Infection Control Screening in Hospitals
As antimicrobial resistance spreads worldwide, healthcare-associated infections are placing a growing burden on hospitals, increasing the need for faster and broader diagnostic solutions.... Read more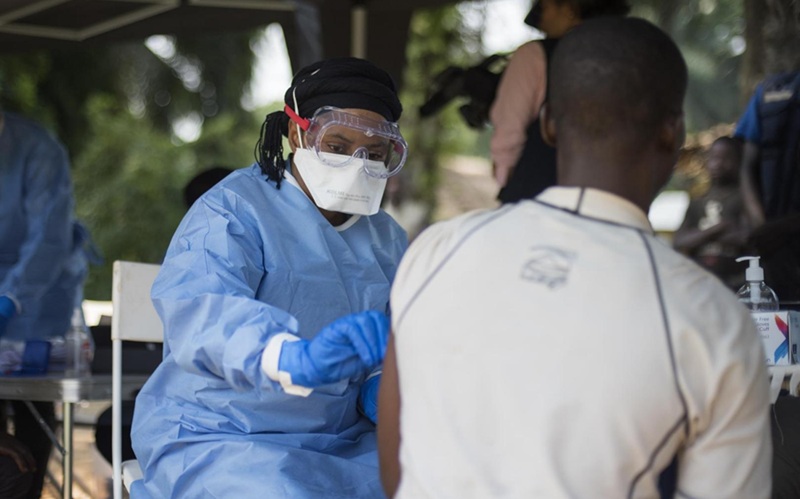
Diagnostic Gaps Complicate Bundibugyo Ebola Outbreak Response in Congo
In eastern Democratic Republic of the Congo, communities are confronting a resurgence of Bundibugyo ebolavirus, a rarer species for which no vaccines or treatments have been approved. Ebola is a highly... Read more
Study Finds Hidden Mpox Infections May Drive Ongoing Spread
Mpox continues to circulate despite vaccination, and many cases show no known link to a symptomatic partner. The role of people without symptoms has remained uncertain, limiting clarity on how transmission persists.... Read more
Large-Scale Genomic Surveillance Tracks Resistant Bacteria Across European Hospitals
Antimicrobial resistance (AMR) poses a growing threat to patient safety, with carbapenem-resistant Enterobacterales causing difficult-to-treat infections and leaving clinicians with limited therapeutic options.... Read morePathology
view channel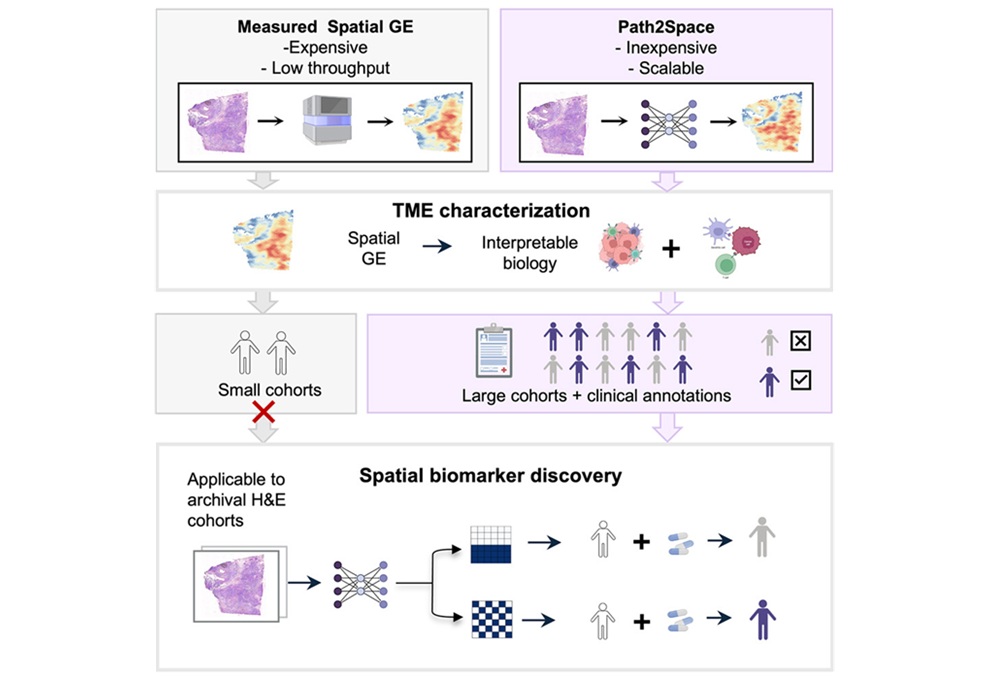
Rapid AI Tool Predicts Cancer Spatial Gene Expression from Pathology Images
Gene expression profiling can inform tumor biology and treatment selection, but spatial assays remain costly and time-consuming. Results can take weeks and cost thousands of dollars, limiting large-scale... Read more
AI Pathology Test Receives FDA Breakthrough for Bladder Cancer Risk Stratification
Non–muscle invasive bladder cancer has highly variable outcomes, complicating surveillance and treatment planning. Risk assessment typically relies on stage, grade, and tumor size, leaving uncertainty... Read moreTechnology
view channel
AI-Enabled Assistant Unifies Molecular Workflow Planning and Support
Clinical laboratories and research groups face increasingly complex molecular workflows and expanding technical documentation spread across multiple systems. Fragmented digital tools can slow experiment... Read more
AI Tool Automates Validation of Laboratory Software Configuration Changes
Regulated laboratories face heavy documentation and requalification demands when software configurations change, slowing improvements and discouraging beneficial updates. A new capability now automates... Read moreIndustry
view channel
Strategic Collaboration Advances RNA Foundation Models for Precision Oncology
Bulk RNA sequencing is increasingly used to study tumor biology, but standard analyses often reduce results to gene-level summaries that miss important transcript variants and mutation patterns.... Read more