Elevated Lipoprotein(a) Mediates Risk of Atrial Fibrillation
|
By LabMedica International staff writers Posted on 27 Apr 2022 |
Atrial fibrillation (AF) is the most common cardiac arrhythmia in adults, with a prevalence between 0.5% and 2%. Longer life span and higher prevalence of AF risk factors are projected to further increase the global prevalence of AF.
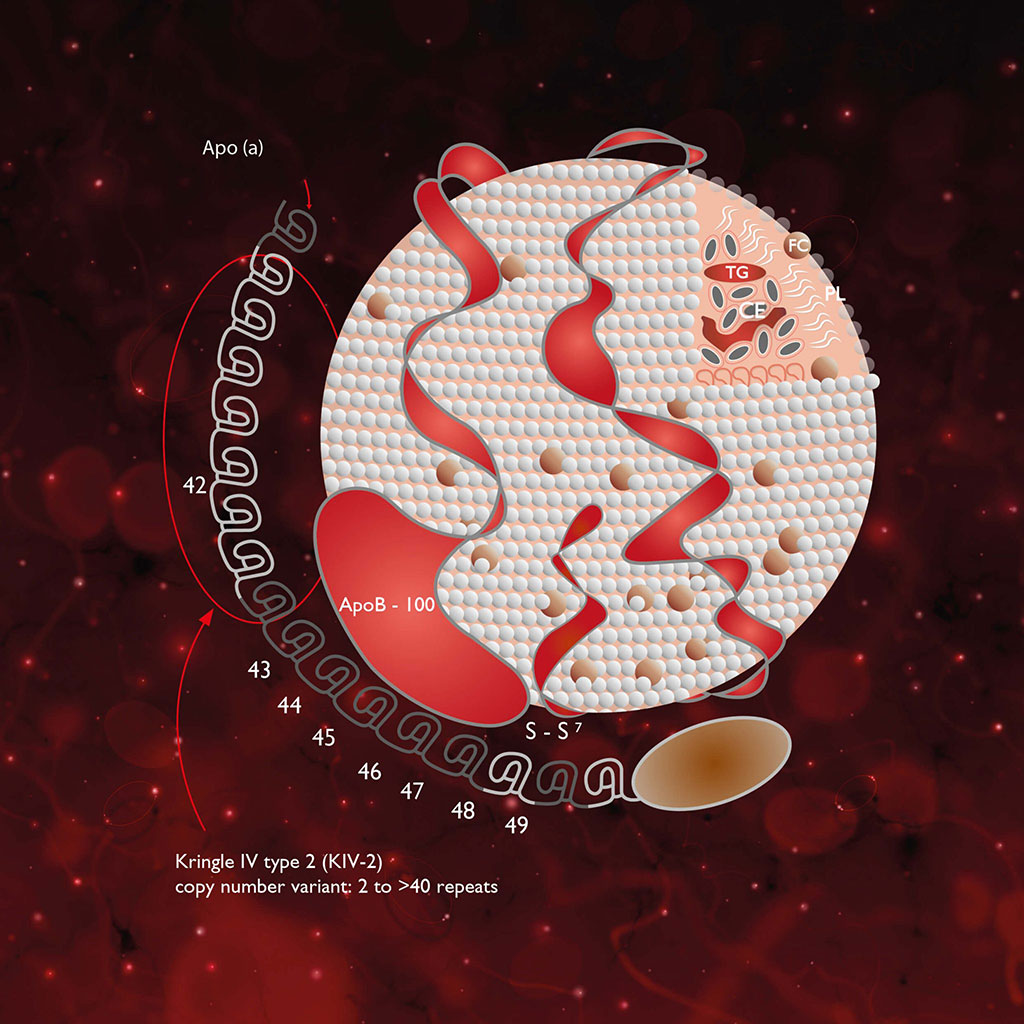
Patients with AF have greater risks of heart failure, ischemic stroke, dementia, and death, and are more likely to be hospitalized, resulting in higher health care costs. Lipoprotein(a) (Lp[a]) is a particle consisting of a low-density lipoprotein (LDL)-like core attached to an apolipoprotein(a) chain. Lp(a) plays a role in atherosclerotic cardiovascular disease and is a well-established risk factor for coronary artery disease, ischemic stroke, and aortic valve stenosis.
Medical Scientists at McMaster University (Hamilton, ON, Canada) and their colleagues investigated the role of Lp(a) in AF and whether it is independent of atherosclerotic cardiovascular disease (ASCVD). The team measured and genetically predicted Lp(a) levels were tested for association with 20,432 cases of incident AF in the UK Biobank (N = 435,579). Mendelian randomization analyses were performed by using summary-level data for AF from publicly available genome-wide association studies (N = 1,145,375). Lp(a) was measured on a Randox AU5800 immunoturbidimetric assay (Randox Laboratories, Crumlin, UK) that used a 5-point calibrator to reflect heterogeneity in Lp(a) isoform size.
The investigators reported that after a median 11 years of follow-up, the rate of incident AF was 4.37 events per 1,000 person-years. They found that each 23 mg/dL increase in Lp(a) was associated with a 3% increased risk for incident AF using measured Lp(a) (HR = 1.03) and genetically predicted Lp(a), with an OR of 1.03. Mendelian randomization analyses using independent data replicated the effect, with an OR of 1.04 per 23 mg/dL increase. They found no evidence of risk-conferring effect from LDL or triglycerides, whereas only 39% of Lp(a) risk was mediated through ASCVD, suggesting Lp(a) partly influences AF independent of its known effects on ASCVD.
Guillaume Pare, MD, MSc, FRCPC, a professor of pathology and molecular medicine and senior author of the study, said, “Lipoprotein(a) is associated with an increased risk for atrial fibrillation and this appears to be a causal relationship independent of coronary artery disease and aortic valve stenosis. The main clinical implication is the exciting possibility that novel Lp(a) inhibitors, currently undergoing clinical evaluation, could reduce incident AF as a side benefit. Our findings also establish a new risk factor for AF and could be used to complement AF risk assessment.”
The authors concluded that epidemiologic and genetic analyses implicate a potentially causal role for Lp(a) on risk of incident AF in population-scale cohorts that is independent of its effect on atherosclerotic cardiovascular disease. Given the role of Lp(a) as a risk factor for common comorbidities of AF, namely stroke and myocardial infarction, and the development of antisense oligonucleotides to lower Lp(a) to treat these comorbidities, these findings highlight an important beneficial pleiotropic effect these therapies may have on prevention or treatment of AF in high-risk groups with highly elevated Lp(a). The study was published in the April, 2022 issue of the Journal of the American College of Cardiology.
Related Links:
McMaster University
Randox Laboratories
Latest Clinical Chem. News
- Saliva-Based Test Detects Biochemical Signs of Sleep Loss
- Simple Dual-Tau Blood Test Detects and Stages Alzheimer’s Disease
- Alzheimer’s Blood Biomarkers Linked to Early Cognitive Differences Before Dementia
- Urine-Based Test Shows Promise for Autism Screening in Children
- Blood-Based Sensor Detects Early Signs of Alzheimer’s and Parkinson’s
- Liquid Biopsy Biomarkers May Improve Childhood Epilepsy Diagnosis
- Urine-Based Alzheimer’s Test Receives FDA Breakthrough Device Designation
- Fluid Biomarker Improves Diagnosis and Monitoring of Primary CNS Lymphoma
- New CA19-9 Cutoff Value Helps Identify High-Risk Pancreatic Cancer Patients
- Blood-Based Biomarkers Show Promise for Psychosis Risk Prediction
- International Experts Recommend Ending Routine 'Corrected' Calcium Reporting
- Long-Term Data Show PSA Screening Modestly Reduces Prostate Cancer Deaths
- Urine-Based Nanosensor Tracks Lung Cancer and Fibrosis Noninvasively
- FDA-Cleared Assay Enables Comprehensive Automated Testosterone Testing
- CE-Marked Blood Biomarker Test Advances Automated Alzheimer’s Diagnostics
- Blood-Based Alzheimer’s Test Gains CE Mark for Amyloid Pathology Detection
Channels
Molecular Diagnostics
view channel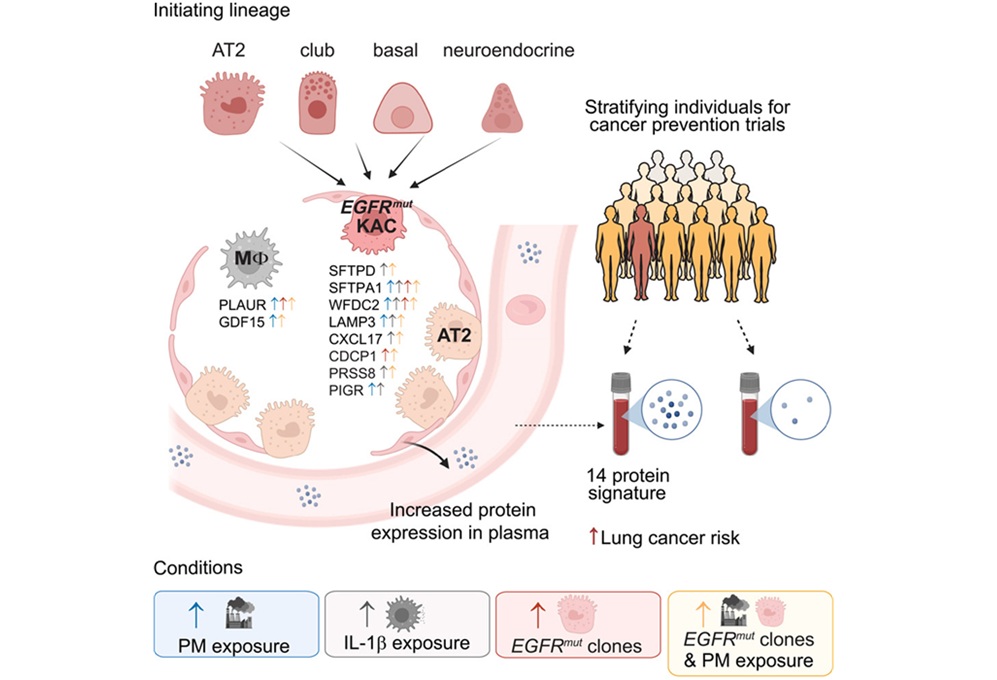
Plasma Protein Signature Predicts Lung Cancer Risk Up to Five Years Ahead
Lung cancer remains a leading cause of cancer death, and many cases are detected only after symptoms appear. Current screening programs largely target people with a history of smoking, leaving other at-risk... Read more
Circulating Tumor DNA Testing Guides Chemotherapy, Reduces Relapse in Colon Cancer
Adjuvant therapy decisions after curative surgery for colon cancer remain difficult, as conventional clinicopathologic factors often fail to capture residual disease risk. Liquid biopsy approaches that... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channelAptamer-Based Biosensor Enables Mutation-Resilient SARS-CoV-2 Detection
Rapid evolution of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can undermine existing molecular diagnostics, especially when assays target small viral components. Double-antibody sandwich... Read more
Study Points to Autoimmune Pathway Behind Long COVID Symptoms
Long COVID leaves many SARS-CoV-2 survivors with persistent fatigue, cognitive issues, palpitations, and musculoskeletal pain for months or years. Estimates cited in new research suggest 4%–20% of infected... Read more
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read moreMicrobiology
view channel
Gut Microbiome Signatures Help Identify Risk of IBD Progression
Inflammatory bowel disease (IBD), encompassing Crohn’s disease and ulcerative colitis, is a chronic relapsing inflammatory disorder of the gastrointestinal tract with highly variable outcomes.... Read more
FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
Clinical guidelines support testing based on patient presentation in suspected gastrointestinal infections, yet available technologies have often forced laboratories to choose between panels that are too... Read morePathology
view channel
Blood-Based Method Tracks Gene Activity in the Living Brain
Real-time measurement of gene activity in the brain has been limited by assays requiring destructive tissue sampling. Tracking active genes could reveal how the body responds to environmental factors,... Read more
FDA Approval Expands Automated PD-L1 Testing Across Solid Tumors
Clinical laboratories play a central role in guiding immunotherapy by reporting programmed death ligand-1 (PD‑L1) status across multiple solid tumors. Many sites are standardizing this work on fully automated... Read moreTechnology
view channel
AI Platform Links Biomarker Results to Cancer Clinical Trials and Guidelines
Oncology teams must manage growing volumes of genomic data, rapidly evolving clinical trial options, and frequently updated care guidelines, all within tight clinic schedules. Translating complex tumor... Read more
Agentic AI Platform Supports Genomic Decision-Making in Oncology
Oncology care teams increasingly face the challenge of managing complex molecular diagnostics, evolving treatment options, and extensive electronic health record documentation. Translating multimodal data... Read moreIndustry
view channel