Plasma ACE2 Predicts Prognosis of COVID-19 Hospitalized Patients
|
By LabMedica International staff writers Posted on 24 Jun 2021 |
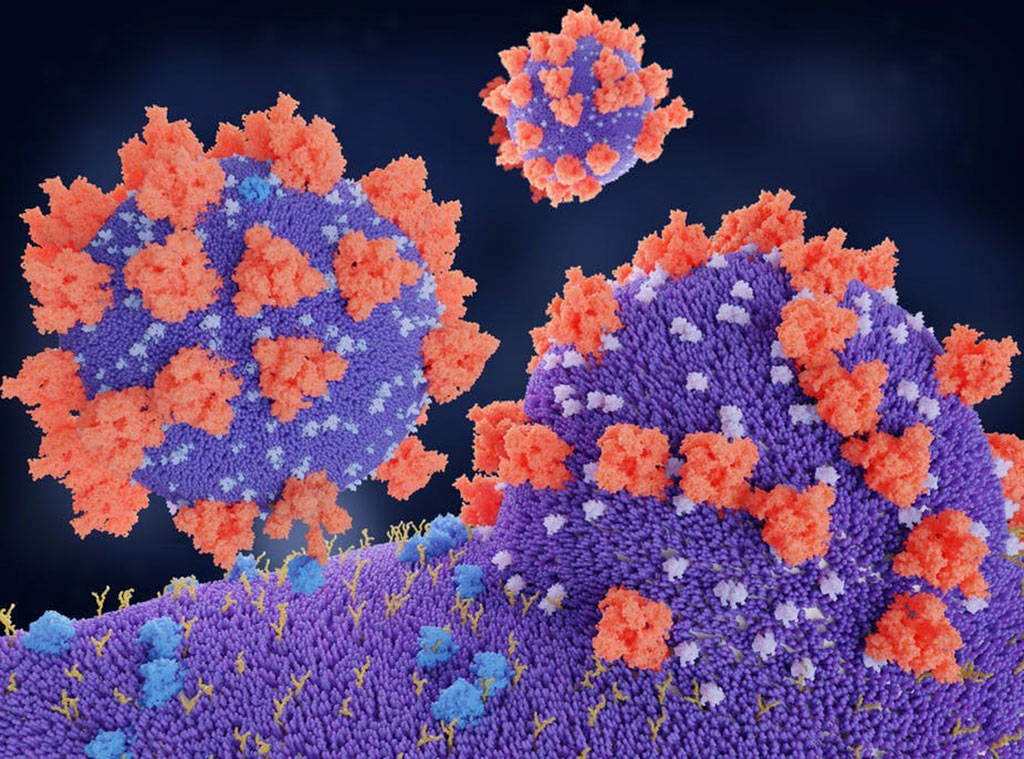
Image: A molecular model of the spike proteins (red) of SARS-CoV-2 binding to the angiotensin-converting enzyme 2 (ACE2) protein, the receptor (blue) which is it’s entry route to the target cell (Photo courtesy of the Juan Gaertner/ Science Photo Library)
Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), has caused a devastating global pandemic. The disease caused by SARS-CoV-2 infection has been termed coronavirus disease of 2019 (COVID-19) with clinical manifestations ranging from asymptomatic and subclinical infection to severe hyperinflammatory syndrome and death.
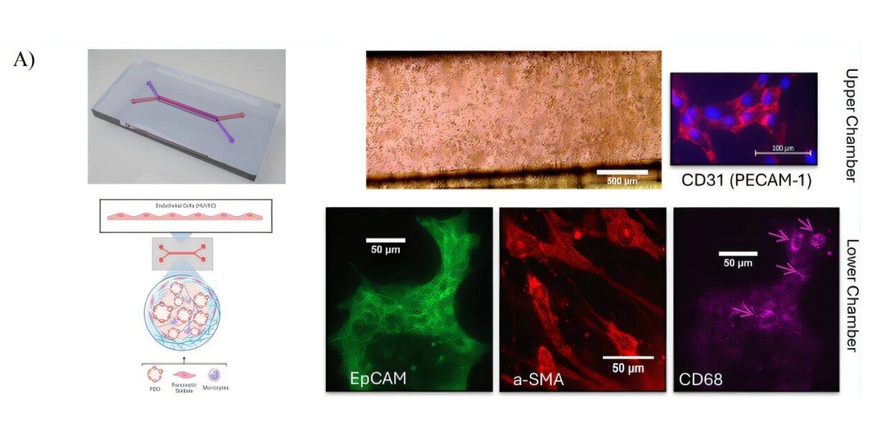
SARS-CoV-2 binds to the angiotensin converting enzyme 2 (ACE2) receptor enabling entrance into cells through membrane fusion and endocytosis. The ACE2-receptor is distributed in different tissues including vascular endothelial cells, smooth muscle cells, nasal and oral mucosa, enterocytes within the intestines, and is especially abundant in the kidneys and type II alveolar pneumocytes in the lungs.
An international team of scientists collaborating with those at Aarhus University Hospital (Aarhus, Denmark) analyzed data from a large longitudinal study of 306 COVID-19-positive patients and 78 COVID-19-negative patients (Massachusetts General Hospital Emergency Department COVID-19 Cohort). Subjects included patients 18 years or older, who were in acute respiratory distress with a clinical concern for COVID-19 upon arrival to the Emergency Department. Samples from the patients were analyzed by the Olink Explore 1536 platform (Olink, Uppsala, Sweden), which includes measurement of the ACE2 protein. The Olink platform is based on Proximity Extension Assay (PEA) technology.
The team reported that the analysis demonstrated that high admission plasma ACE2 in patients with COVID-19 was associated with increased maximal illness severity within 28 days (odds ratio [OR] = 1.8). In models correcting for age, body mass index (BMI), hypertension, and pre-existing heart conditions, kidney disease, lung disease, diabetes, and immunosuppressive conditions, significant associations were still observed between plasma ACE2 at admission and maximal illness severity within 28 days.
Further, studies found that plasma ACE2 was also significantly higher in patients with COVID-19 with hypertension compared with patients without hypertension, and in patients with pre-existing heart conditions and kidney disease compared with those without these comorbidities. However, there was no significant difference in plasma ACE2 comparing patients with or without pre-existing lung disease, diabetes, or immunosuppressive conditions. Additionally, elevated plasma ACE2 in COVID-19-positive patients was significantly associated with increasing age, but there was no significant association between plasma ACE2 and BMI.
Tue W. Kragstrup, MD, an associate professor and lead author of the study, said, ““Elevated baseline plasma ACE2 in COVID-19 patients was significantly associated with increased disease severity during the 28-day study period. This indicates that abundant ACE2 production could be involved in increased viral spread and disease burden.”
The authors concluded that the design of the data analysis using the Olink platform does not allow assessment of quantitative differences. However, previous studies have described a positive correlation between plasma ACE2 and ACE1 activity. This is interesting because ACE1 (serum ACE) analysis is a standardized test in most hospital laboratories. Therefore, their study encourages quantitative investigations of both plasma ACE 1 and 2 in COVID-19. The study was published on June 4, 2021 in the journal PLOS ONE.
Related Links:
Aarhus University Hospital
Olink
SARS-CoV-2 binds to the angiotensin converting enzyme 2 (ACE2) receptor enabling entrance into cells through membrane fusion and endocytosis. The ACE2-receptor is distributed in different tissues including vascular endothelial cells, smooth muscle cells, nasal and oral mucosa, enterocytes within the intestines, and is especially abundant in the kidneys and type II alveolar pneumocytes in the lungs.
An international team of scientists collaborating with those at Aarhus University Hospital (Aarhus, Denmark) analyzed data from a large longitudinal study of 306 COVID-19-positive patients and 78 COVID-19-negative patients (Massachusetts General Hospital Emergency Department COVID-19 Cohort). Subjects included patients 18 years or older, who were in acute respiratory distress with a clinical concern for COVID-19 upon arrival to the Emergency Department. Samples from the patients were analyzed by the Olink Explore 1536 platform (Olink, Uppsala, Sweden), which includes measurement of the ACE2 protein. The Olink platform is based on Proximity Extension Assay (PEA) technology.
The team reported that the analysis demonstrated that high admission plasma ACE2 in patients with COVID-19 was associated with increased maximal illness severity within 28 days (odds ratio [OR] = 1.8). In models correcting for age, body mass index (BMI), hypertension, and pre-existing heart conditions, kidney disease, lung disease, diabetes, and immunosuppressive conditions, significant associations were still observed between plasma ACE2 at admission and maximal illness severity within 28 days.
Further, studies found that plasma ACE2 was also significantly higher in patients with COVID-19 with hypertension compared with patients without hypertension, and in patients with pre-existing heart conditions and kidney disease compared with those without these comorbidities. However, there was no significant difference in plasma ACE2 comparing patients with or without pre-existing lung disease, diabetes, or immunosuppressive conditions. Additionally, elevated plasma ACE2 in COVID-19-positive patients was significantly associated with increasing age, but there was no significant association between plasma ACE2 and BMI.
Tue W. Kragstrup, MD, an associate professor and lead author of the study, said, ““Elevated baseline plasma ACE2 in COVID-19 patients was significantly associated with increased disease severity during the 28-day study period. This indicates that abundant ACE2 production could be involved in increased viral spread and disease burden.”
The authors concluded that the design of the data analysis using the Olink platform does not allow assessment of quantitative differences. However, previous studies have described a positive correlation between plasma ACE2 and ACE1 activity. This is interesting because ACE1 (serum ACE) analysis is a standardized test in most hospital laboratories. Therefore, their study encourages quantitative investigations of both plasma ACE 1 and 2 in COVID-19. The study was published on June 4, 2021 in the journal PLOS ONE.
Related Links:
Aarhus University Hospital
Olink
Latest Clinical Chem. News
- Urine-Based Nanosensor Tracks Lung Cancer and Fibrosis Noninvasively
- FDA-Cleared Assay Enables Comprehensive Automated Testosterone Testing
- CE-Marked Blood Biomarker Test Advances Automated Alzheimer’s Diagnostics
- Blood-Based Alzheimer’s Test Gains CE Mark for Amyloid Pathology Detection
- Noninvasive Urine Test May Support Earlier Diagnosis of Psychiatric Disorders
- At-Home Blood and Cognitive Tests Support Dementia Risk Stratification
- Ultrasensitive Test Detects Key Biomarker of Frontotemporal Dementia Subtype
- Routine Blood Tests Years Before Pregnancy Could Identify Preeclampsia Risk
- Blood Test Detects Testicular Cancer Missed by Standard Markers
- Routine Blood Tests Identify Biomarkers Linked to PTSD
- Proteomic Data Underscore Need for Age-Specific Pediatric Reference Ranges
- Routine Blood Count Ratio Linked to Future Alzheimer’s and Dementia Risk
- Label-Free Microfluidic Device Enriches Tumor Cells and Clusters from Pleural Effusions
- Rapid Biosensor Detects Pancreatic Cancer Biomarker for Early Detection
- Urine-Based Multi-Cancer Screening Test Receives FDA Breakthrough Device Designation
- Blood Test Predicts Alzheimer Disease Risk Before Imaging Changes and Symptoms
Channels
Molecular Diagnostics
view channel
ctDNA Blood Test Could Help Guide Radiotherapy in Patients with Limited Metastases
Selecting the right therapy for patients whose solid tumors have begun to spread remains a major clinical challenge. Clinicians often count metastatic lesions on X-ray, computed tomography (CT), or magnetic... Read more
FDA-Approved MRD Blood Test Guides Adjuvant Bladder Cancer Therapy
Muscle-invasive bladder cancer (MIBC) carries a substantial risk of recurrence after radical cystectomy, and selecting which patients require adjuvant therapy remains challenging. Approximately 30,000... Read moreHematology
view channel
Stem Cell Biomarkers May Guide Precision Treatment in Acute Myeloid Leukemia
Acute myeloid leukemia (AML) is an aggressive blood cancer that most often affects older adults and still carries a poor prognosis despite therapeutic advances. Venetoclax-based regimens have improved... Read more
Advanced CBC-Derived Indices Integrated into Hematology Platforms
Diatron, a STRATEC brand, has introduced six advanced hematological indices on its Aquila, Aquarius 3, and Abacus 5 hematology analyzers. The new Research Use Only (RUO) indices include Neutrophil-to-Lymphocyte... Read moreImmunology
view channel
Routine TB Screening Test May Reveal Immune Aging and Mortality Risk
Immune aging is associated with weaker responses to vaccination, greater risks of infection, and higher levels of inflammation. Leveraging routinely ordered laboratory tests to quantify that responsiveness... Read more
Biomarkers and Molecular Testing Advance Precision Allergy Care
Allergic diseases often present with similar symptoms but can be driven by distinct biological mechanisms, making standardized care inefficient for many patients. Historically, individuals with pollen... Read moreMicrobiology
view channel
Study Finds Hidden Mpox Infections May Drive Ongoing Spread
Mpox continues to circulate despite vaccination, and many cases show no known link to a symptomatic partner. The role of people without symptoms has remained uncertain, limiting clarity on how transmission persists.... Read more
Large-Scale Genomic Surveillance Tracks Resistant Bacteria Across European Hospitals
Antimicrobial resistance (AMR) poses a growing threat to patient safety, with carbapenem-resistant Enterobacterales causing difficult-to-treat infections and leaving clinicians with limited therapeutic options.... Read more
Molecular Urine and Stool Tests Do Not Improve Early TB Treatment in Hospitalized HIV Patients
Tuberculosis is the leading cause of death among people living with HIV, and diagnosis in hospital settings remains difficult. Symptoms are often non-specific, disease can be extrapulmonary, and many patients... Read morePathology
view channel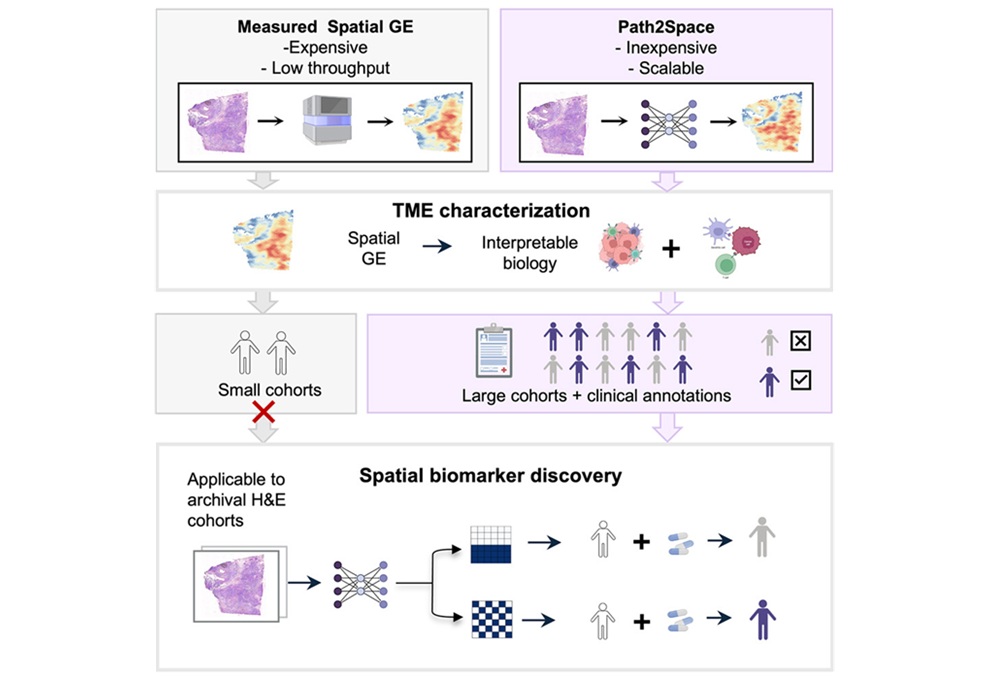
Rapid AI Tool Predicts Cancer Spatial Gene Expression from Pathology Images
Gene expression profiling can inform tumor biology and treatment selection, but spatial assays remain costly and time-consuming. Results can take weeks and cost thousands of dollars, limiting large-scale... Read more
AI Pathology Test Receives FDA Breakthrough for Bladder Cancer Risk Stratification
Non–muscle invasive bladder cancer has highly variable outcomes, complicating surveillance and treatment planning. Risk assessment typically relies on stage, grade, and tumor size, leaving uncertainty... Read moreTechnology
view channel
Point-of-Care Testing Enhances Health Literacy and Self-Management in Chronic Disease
Limited access to general practitioners and pathology services can delay diagnosis and monitoring for people in regional and remote communities. Rapid, on-the-spot testing can shorten turnaround times... Read more
Fully Automated Sample-to-Insight Workflow Advances Latent TB Testing
Latent tuberculosis remains a substantial testing workload for clinical laboratories as screening programs expand. Despite this growth, only about 40% of testing has shifted from traditional skin tests... Read moreIndustry
view channel
AI-Powered Multi-Functional Analyzer Wins German Innovation Award
Hematology services are increasingly delivered across distributed care settings, where limited staffing and complex workflows can extend turnaround times. Advanced morphology review still often depends... Read more