Point-of-Care Tests Could Expand Access to Mpox Diagnosis
Posted on 04 May 2026
Mpox outbreaks in non-endemic regions have underscored the need for rapid, accessible diagnostics to limit transmission. Polymerase chain reaction (PCR) remains the clinical reference, yet it depends on specialized equipment and trained staff, constraining availability in many settings. Point-of-care approaches that can be deployed near patients are increasingly sought to complement centralized testing. A new review in Trends in Biotechnology outlines emerging strategies for faster detection and practical pathways to broaden mpox diagnostic access.
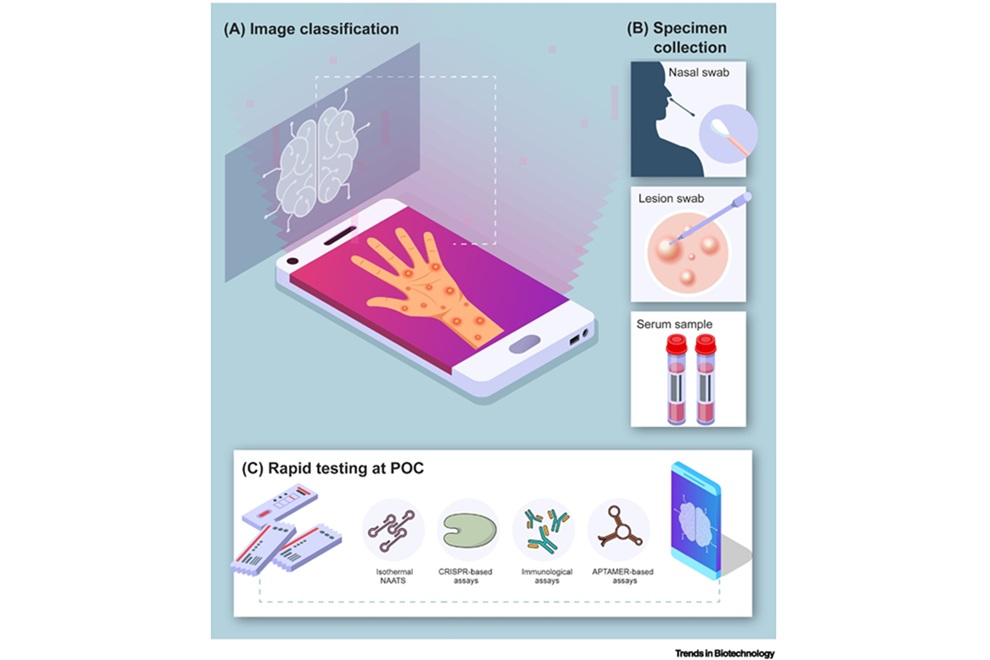
Koç University (Istanbul, Turkey) researchers reviewed point-of-care (POC) diagnostic approaches for mpox, including loop-mediated isothermal amplification (LAMP), recombinase polymerase amplification (RPA), CRISPR/Cas assays, rapid antigen tests, electrochemical biosensors, and artificial intelligence (AI)–supported lesion image analysis. The review emphasizes that clinical specimens such as nasal swabs, lesion swabs, or serum can support molecular or biochemical confirmation. It also details how field-deployable devices and assays are being developed to bring testing closer to the patient.
PCR, which detects viral genetic material in lesion-derived samples, provides highly sensitive and accurate results but requires complex infrastructure and trained personnel, limiting near-patient use. Immunological assays such as enzyme-linked immunosorbent assay (ELISA) have restricted clinical utility due to cross-reactivity with related orthopoxviruses, especially among individuals previously vaccinated against smallpox. Recently developed rapid antigen tests targeting viral proteins can yield results within 10–15 minutes, though they are generally less sensitive than PCR and do not readily quantify viral load.
Isothermal amplification methods (LAMP, RPA) operate at a constant temperature and avoid thermal cycling, with sensitivity in some studies approaching PCR, yet they may produce occasional false positives and face limited multiplexing. CRISPR/Cas-based diagnostics recognize viral nucleic acids with high specificity, and when coupled with LAMP or RPA can achieve very high sensitivity with potential to distinguish different mpox clades. Remaining constraints include cost, technical complexity, and cold-chain requirements for certain reagents.
The article frames “ideal” point-of-care tests using World Health Organization criteria and the expanded REASSURED framework, highlighting affordability, robustness, rapidity, connectivity, and simple specimen collection. Promising avenues include electrochemical biosensors, paper-based assays, microfluidic chips, and 3D-printed components, alongside smartphone integration to reduce costs and enhance scalability. AI-driven image analysis of skin lesions is presented as an adjunctive screening tool, particularly where specialist clinicians are scarce, rather than a replacement for molecular testing.
The review, published in Trends in Biotechnology, synthesizes work from Koç University School of Medicine, the Koç University İşbank Center for Infectious Diseases, the Department of Mechanical Engineering, and the Koç University Translational Medicine Research Center (KUTTAM). It concludes that while PCR remains the gold standard, there is a growing need for rapid, accessible diagnostics in low-resource settings. Technologies such as LAMP, RPA, and CRISPR are advancing toward this goal, but challenges in cost, large-scale production, field applicability, and health-system integration persist, with future progress likely to come from integrated platforms combining molecular testing, biosensors, and AI-supported decision systems.
Related Links
Koç University