Unique Antibody Profile Differentiates Gluten Sensitivity from Celiac Disease
|
By LabMedica International staff writers Posted on 17 Sep 2020 |
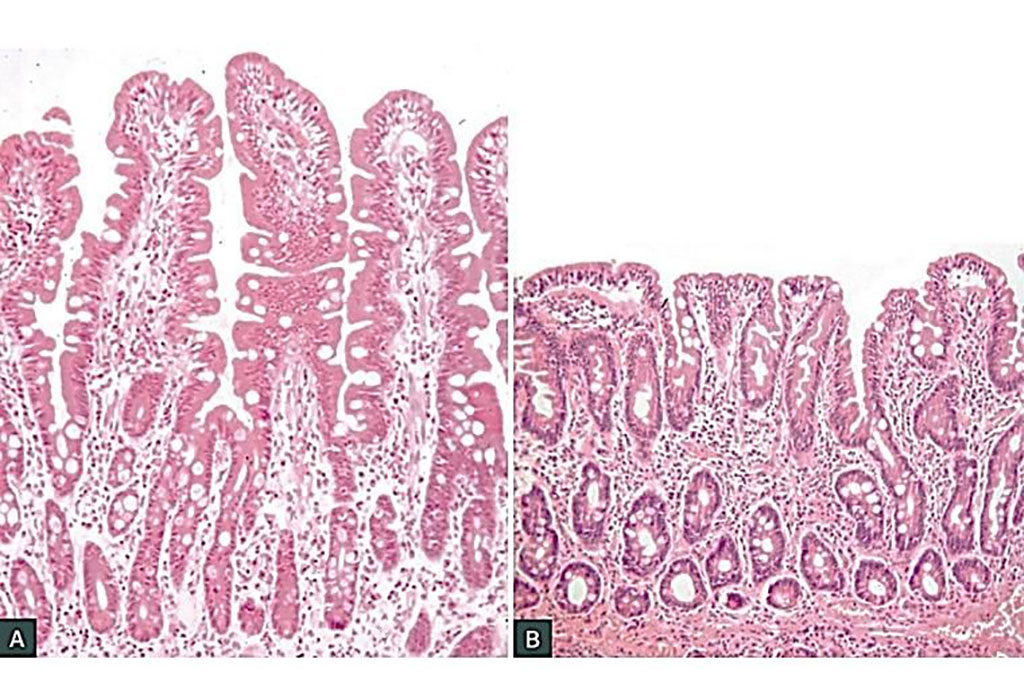
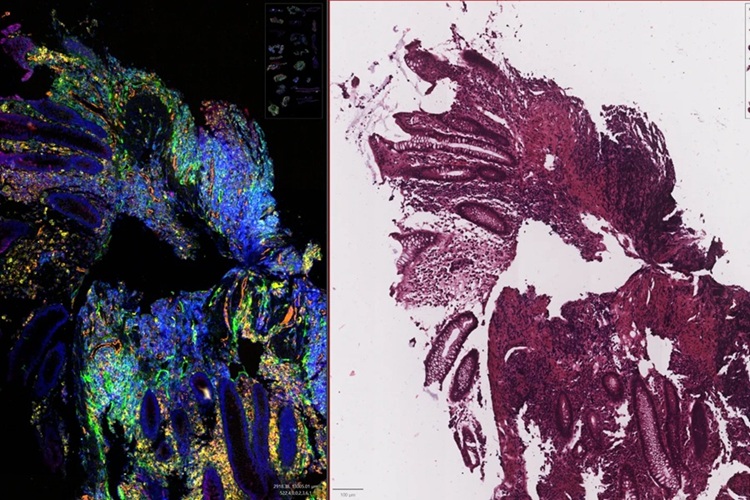
Image: Histology of normal small intestinal mucosa in adequately treated celiac disease (A). Untreated coeliac disease shows the classic triad of infiltration of the epithelium with lymphocytes, crypt hyperplasia and villous atrophy (B) (Photo courtesy of Professor Jason Tye-Din, MBBS PhD).
Until recently, many doctors often dismissed the complaints of people who claimed to be sensitive to foods containing gluten but did not have celiac disease, a well-documented autoimmune disease triggered by exposure to the dietary protein found in wheat, rye, and barley.
Celiac disease (CD) is an autoimmune enteropathy triggered by exposure to gluten proteins, leading to intestinal inflammation and villous atrophy in genetically predisposed individuals. It is associated with robust B cell and antibody responses to gluten and to the transglutaminase 2 (TG2) autoantigen.
A team of scientists from various institutions and led by those at the Columbia University Medical Center (New York, NY, USA) analyzed blood samples from 40 patients with celiac disease, 80 patients with non-celiac gluten sensitivity (NCGS), and 40 healthy controls, all of whom consumed an unrestricted, gluten-containing diet. The most common gastrointestinal symptoms included bloating, abdominal pain, diarrhea, nausea, and heartburn, while the most prominent extra-intestinal symptoms were fatigue, headache, anxiety, cognitive difficulties, and numbness in arms and legs.
Serum levels of total IgG reactivity to gluten and individual IgG subclass reactivities to gluten were measured separately by an enzyme-linked immunosorbent assay (ELISA). Serum levels of intestinal fatty acid-binding protein (FABP2) were also measured. FABP2 is a cytosolic protein specific to intestinal epithelial cells that is released into systemic circulation upon cellular damage. The team measured IgA antibody to recombinant human TG2, a sensitive and specific serologic marker for CD. The investigators performed HLA genotyping to assess CD genetic predisposition.
The scientists reported that the anti-gliadin IgG response in CD patients was comprised primarily of IgG1 and IgG3, which were significantly increased in comparison with the healthy and NCGS cohorts. There was a modest elevation in anti-gliadin IgG2 compared with the healthy group and no comparative increase in the IgG4 subclass. Within the NCGS cohort, however, the lower contributions of anti-gliadin IgG1 and IgG3 in comparison with CD was compensated by significantly elevated IgG4 (compared with CD and healthy cohorts) and IgG2 (compared with healthy cohort). Serum concentrations of intestinal fatty acid-binding protein (FABP2), a specific marker of intestinal epithelial cell damage, were similarly elevated in the CD and NCGS groups in comparison with healthy cohort.
Armin Alaedini, PhD, an assistant professor of medicine and a senior author of the study, said, “We found that the B cells of celiac disease patients produced a subclass profile of IgG antibodies with a strong inflammatory potential that is linked to autoimmune activity and intestinal cell damage. In contrast, the patients with non-celiac gluten sensitivity produced IgG antibodies that are associated with a more restrained inflammatory response.” The study was published online July 21, 2020 in the journal Gastroenterology.
Related Links:
Columbia University Medical Center
Celiac disease (CD) is an autoimmune enteropathy triggered by exposure to gluten proteins, leading to intestinal inflammation and villous atrophy in genetically predisposed individuals. It is associated with robust B cell and antibody responses to gluten and to the transglutaminase 2 (TG2) autoantigen.
A team of scientists from various institutions and led by those at the Columbia University Medical Center (New York, NY, USA) analyzed blood samples from 40 patients with celiac disease, 80 patients with non-celiac gluten sensitivity (NCGS), and 40 healthy controls, all of whom consumed an unrestricted, gluten-containing diet. The most common gastrointestinal symptoms included bloating, abdominal pain, diarrhea, nausea, and heartburn, while the most prominent extra-intestinal symptoms were fatigue, headache, anxiety, cognitive difficulties, and numbness in arms and legs.
Serum levels of total IgG reactivity to gluten and individual IgG subclass reactivities to gluten were measured separately by an enzyme-linked immunosorbent assay (ELISA). Serum levels of intestinal fatty acid-binding protein (FABP2) were also measured. FABP2 is a cytosolic protein specific to intestinal epithelial cells that is released into systemic circulation upon cellular damage. The team measured IgA antibody to recombinant human TG2, a sensitive and specific serologic marker for CD. The investigators performed HLA genotyping to assess CD genetic predisposition.
The scientists reported that the anti-gliadin IgG response in CD patients was comprised primarily of IgG1 and IgG3, which were significantly increased in comparison with the healthy and NCGS cohorts. There was a modest elevation in anti-gliadin IgG2 compared with the healthy group and no comparative increase in the IgG4 subclass. Within the NCGS cohort, however, the lower contributions of anti-gliadin IgG1 and IgG3 in comparison with CD was compensated by significantly elevated IgG4 (compared with CD and healthy cohorts) and IgG2 (compared with healthy cohort). Serum concentrations of intestinal fatty acid-binding protein (FABP2), a specific marker of intestinal epithelial cell damage, were similarly elevated in the CD and NCGS groups in comparison with healthy cohort.
Armin Alaedini, PhD, an assistant professor of medicine and a senior author of the study, said, “We found that the B cells of celiac disease patients produced a subclass profile of IgG antibodies with a strong inflammatory potential that is linked to autoimmune activity and intestinal cell damage. In contrast, the patients with non-celiac gluten sensitivity produced IgG antibodies that are associated with a more restrained inflammatory response.” The study was published online July 21, 2020 in the journal Gastroenterology.
Related Links:
Columbia University Medical Center
Latest Immunology News
- Immune Enzyme Linked to Treatment-Resistant Inflammatory Bowel Disease
- Simple Blood Test Could Replace Biopsies for Lung Transplant Rejection Monitoring
- Routine TB Screening Test May Reveal Immune Aging and Mortality Risk
- Biomarkers and Molecular Testing Advance Precision Allergy Care
- Point-of-Care Tests Could Expand Access to Mpox Diagnosis
- T-Cell Senescence Profiling May Predict CAR T Responses
- Finger-Prick Lateral Flow Test Detects Sepsis Biomarkers at Point of Care
- Study Highlights Low Sensitivity of Current Lyme Tests in Early Infection
- Immune Aging Clock Quantifies Immunosenescence and Identifies Therapeutic Target
- Study Finds Influenza Often Undiagnosed in Winter Deaths
- Combined Screening Approach Identifies Early Leprosy Cases
- Antibody Blood Test Identifies Active TB and Distinguishes Latent Infection
- FDA Approval Expands Use of PD-L1 Companion Diagnostic in Esophageal and GEJ Carcinomas
- Study Identifies Inflammatory Pathway Driving Immunotherapy Resistance in Bladder Cancer
- Microfluidic Chip Detects Cancer Recurrence from Immune Response Signals
- Cancer Mutation ‘Fingerprints’ to Improve Prediction of Immunotherapy Response
Channels
Clinical Chemistry
view channel
New CA19-9 Cutoff Value Helps Identify High-Risk Pancreatic Cancer Patients
Pancreatic ductal adenocarcinoma (PDAC) is frequently diagnosed at an advanced stage and remains one of the most lethal solid tumors. Clinicians commonly use serum carbohydrate antigen 19-9 (CA19-9) to... Read more
Blood-Based Biomarkers Show Promise for Psychosis Risk Prediction
Psychosis commonly emerges in adolescence or early adulthood and can severely disrupt social and occupational functioning. Hallucinations, delusions, and disorganized thinking often evolve gradually, hindering... Read moreMolecular Diagnostics
view channel
New RNA Origami Method Supports Faster Targeted Testing for Repeat Expansion Disorders
Repeat expansion disorders drive conditions such as myotonic dystrophy, Huntington’s disease, and amyotrophic lateral sclerosis (ALS), yet accurately sizing the mutated sequences remains difficult.... Read more
FDA Approves Expanded Liquid Biopsy Panel for Advanced Cancer Profiling
Timely, comprehensive tumor profiling helps clinicians make treatment selection decisions for patients with advanced cancer. Blood-based approaches can provide actionable insights from a simple draw and... Read moreHematology
view channel
Higher Ferritin Threshold May Improve Iron Deficiency Detection in Children
Iron deficiency in school-age children can affect brain development, learning, growth, and physical performance, yet early deficiency may be missed when screening focuses mainly on anemia.... Read more
Stem Cell Biomarkers May Guide Precision Treatment in Acute Myeloid Leukemia
Acute myeloid leukemia (AML) is an aggressive blood cancer that most often affects older adults and still carries a poor prognosis despite therapeutic advances. Venetoclax-based regimens have improved... Read moreMicrobiology
view channel
New AMR Assay Supports Rapid Infection Control Screening in Hospitals
As antimicrobial resistance spreads worldwide, healthcare-associated infections are placing a growing burden on hospitals, increasing the need for faster and broader diagnostic solutions.... Read more
Diagnostic Gaps Complicate Bundibugyo Ebola Outbreak Response in Congo
In eastern Democratic Republic of the Congo, communities are confronting a resurgence of Bundibugyo ebolavirus, a rarer species for which no vaccines or treatments have been approved. Ebola is a highly... Read more
Study Finds Hidden Mpox Infections May Drive Ongoing Spread
Mpox continues to circulate despite vaccination, and many cases show no known link to a symptomatic partner. The role of people without symptoms has remained uncertain, limiting clarity on how transmission persists.... Read more
Large-Scale Genomic Surveillance Tracks Resistant Bacteria Across European Hospitals
Antimicrobial resistance (AMR) poses a growing threat to patient safety, with carbapenem-resistant Enterobacterales causing difficult-to-treat infections and leaving clinicians with limited therapeutic options.... Read morePathology
view channel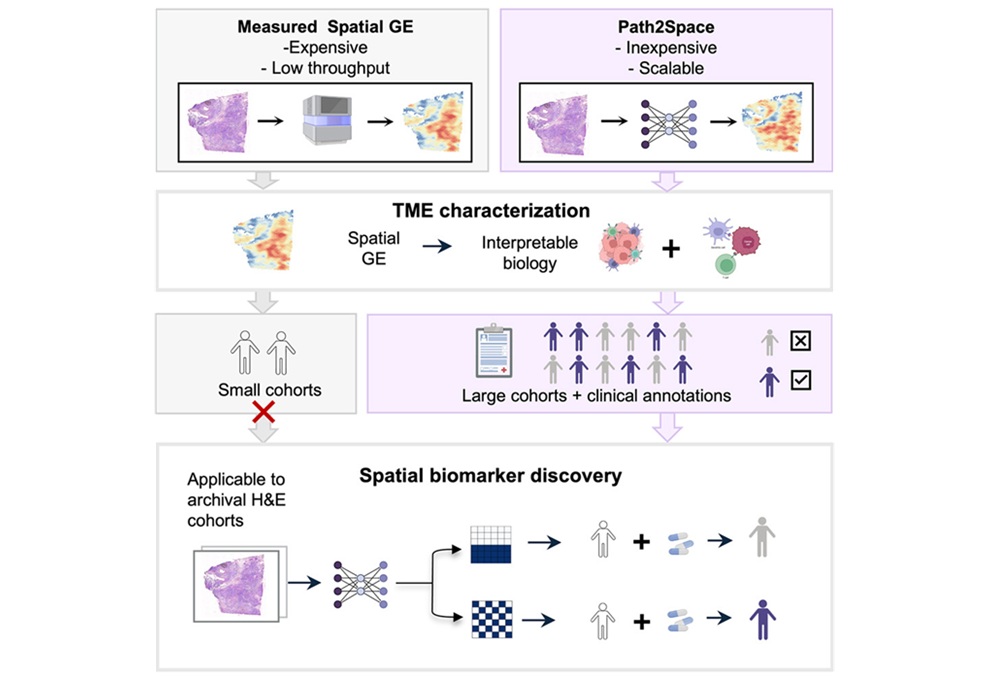
Rapid AI Tool Predicts Cancer Spatial Gene Expression from Pathology Images
Gene expression profiling can inform tumor biology and treatment selection, but spatial assays remain costly and time-consuming. Results can take weeks and cost thousands of dollars, limiting large-scale... Read more
AI Pathology Test Receives FDA Breakthrough for Bladder Cancer Risk Stratification
Non–muscle invasive bladder cancer has highly variable outcomes, complicating surveillance and treatment planning. Risk assessment typically relies on stage, grade, and tumor size, leaving uncertainty... Read moreTechnology
view channel
AI-Enabled Assistant Unifies Molecular Workflow Planning and Support
Clinical laboratories and research groups face increasingly complex molecular workflows and expanding technical documentation spread across multiple systems. Fragmented digital tools can slow experiment... Read more
AI Tool Automates Validation of Laboratory Software Configuration Changes
Regulated laboratories face heavy documentation and requalification demands when software configurations change, slowing improvements and discouraging beneficial updates. A new capability now automates... Read moreIndustry
view channel
Strategic Collaboration Advances RNA Foundation Models for Precision Oncology
Bulk RNA sequencing is increasingly used to study tumor biology, but standard analyses often reduce results to gene-level summaries that miss important transcript variants and mutation patterns.... Read more