Rapid Diagnostic Panel Used for Pediatric Musculoskeletal Infections
|
By LabMedica International staff writers Posted on 31 Jul 2019 |

Image: The Xpert MRSA/SA SSTI assay detects methicillin-resistant S. aureus (MRSA) & S. aureus (SA) in skin and soft tissue infections in less than one hour (Photo courtesy of Cepheid).
The findings from a retrospective analysis suggested that the use of a rapid musculoskeletal diagnostic panel, or MDP, could have shortened the time it took to identify the cause of infection, provide appropriate antibiotics and reduce the length of stay for children in hospital.
The MDP, which was recently validated in another study, combined three separate tests: the Xpert MRSA/Staphylococcus aureus skin and soft tissue infection (SA SSTI) assay, a polymerase chain reaction (PCR) assays for ermA, ermB and ermC genes to determine clindamycin resistance; and a Kingella kingae PCR assay to identify the rtxA gene. Results from the Xpert MRSA/SA SSTI assay were available within three hours, and results for the PCR assays were available by 1400 hours the following calendar day.
Scientists at the Children’s Hospital Colorado (Aurora, CO, USA) included in a study 53 children aged six months to 18 years who were admitted to the hospital with symptoms persisting for less than two weeks, had bone or joint specimens collected and were administered antibiotic therapy, excluding perioperative antibiotics. The investigators identified pathogens in 69.8% of patients (37/53) who underwent standard culturing techniques and in 13 patients (16%) who had a blood culture performed. The most commonly identified pathogen was S. aureus (47.2%), and methicillin-resistant S. aureus (MRSA) was identified in 16% of these patients. Two patients had clindamycin-resistant S. aureus, and one patient had a K. kingae infection.
The MDP identified most children with culture-confirmed S. aureus infection (88%), with three patients having MRSA. When cultured, all three patients were confirmed to have MRSA. Although the MDP identified three isolates as clindamycin resistant, culture showed that one of these isolates was clindamycin susceptible. The results showed that MDP would have saved seven hours to pathogen identification (45.6 hours; interquartile range [IQR] = 23-62) compared with standard microbiology culture techniques (52.5 hours; IQR = 36.1-65.6). Additionally, use of the MDP would have improved the time to definitive antibiotic therapy by nearly 22 hours and reduced the hospital length of stay by a median of 26.4 hours.
The authors noted that cost is an important factor when considering a new diagnostic tool like the MDA. Theoretically, the decrease in length of stay would justify its expense. Justin B. Searns, MD, a hospitalist and first author of the study, said, “No approved rapid diagnostic platforms currently exist for bone and joint specimens from pediatric patients with acute musculoskeletal infection.” The study was published on June 13, 2019, in the Journal of The Pediatric Infectious Disease Society.
Related Links:
Children’s Hospital Colorado
The MDP, which was recently validated in another study, combined three separate tests: the Xpert MRSA/Staphylococcus aureus skin and soft tissue infection (SA SSTI) assay, a polymerase chain reaction (PCR) assays for ermA, ermB and ermC genes to determine clindamycin resistance; and a Kingella kingae PCR assay to identify the rtxA gene. Results from the Xpert MRSA/SA SSTI assay were available within three hours, and results for the PCR assays were available by 1400 hours the following calendar day.
Scientists at the Children’s Hospital Colorado (Aurora, CO, USA) included in a study 53 children aged six months to 18 years who were admitted to the hospital with symptoms persisting for less than two weeks, had bone or joint specimens collected and were administered antibiotic therapy, excluding perioperative antibiotics. The investigators identified pathogens in 69.8% of patients (37/53) who underwent standard culturing techniques and in 13 patients (16%) who had a blood culture performed. The most commonly identified pathogen was S. aureus (47.2%), and methicillin-resistant S. aureus (MRSA) was identified in 16% of these patients. Two patients had clindamycin-resistant S. aureus, and one patient had a K. kingae infection.
The MDP identified most children with culture-confirmed S. aureus infection (88%), with three patients having MRSA. When cultured, all three patients were confirmed to have MRSA. Although the MDP identified three isolates as clindamycin resistant, culture showed that one of these isolates was clindamycin susceptible. The results showed that MDP would have saved seven hours to pathogen identification (45.6 hours; interquartile range [IQR] = 23-62) compared with standard microbiology culture techniques (52.5 hours; IQR = 36.1-65.6). Additionally, use of the MDP would have improved the time to definitive antibiotic therapy by nearly 22 hours and reduced the hospital length of stay by a median of 26.4 hours.
The authors noted that cost is an important factor when considering a new diagnostic tool like the MDA. Theoretically, the decrease in length of stay would justify its expense. Justin B. Searns, MD, a hospitalist and first author of the study, said, “No approved rapid diagnostic platforms currently exist for bone and joint specimens from pediatric patients with acute musculoskeletal infection.” The study was published on June 13, 2019, in the Journal of The Pediatric Infectious Disease Society.
Related Links:
Children’s Hospital Colorado
Latest Microbiology News
- Gut Microbiome Signatures Help Identify Risk of IBD Progression
- FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
- New AMR Assay Supports Rapid Infection Control Screening in Hospitals
- Diagnostic Gaps Complicate Bundibugyo Ebola Outbreak Response in Congo
- Study Finds Hidden Mpox Infections May Drive Ongoing Spread
- Large-Scale Genomic Surveillance Tracks Resistant Bacteria Across European Hospitals
- Molecular Urine and Stool Tests Do Not Improve Early TB Treatment in Hospitalized HIV Patients
- Rapid Antigen Biosensor Detects Active Tuberculosis in One Hour
- Label-Free Microscopy Method Enables Faster, Quantitative Detection of Malaria
- Oral–Gut Microbiome Signatures Identify Early Gastric Cancer
- Gut Microbiome Test Predicts Melanoma Recurrence After Surgery
- Rapid Blood-Culture Susceptibility Panel Expands Coverage for Gram-Negative Infections
- Antibiotic Resistance Genes Found in Newborns Within Hours of Birth
- Rapid Color Test Stratifies Virulent and Resistant Staph Strains
- mNGS CSF Test Identifies CNS Pathogens Missed by Standard Panels
- Syndromic Panel Enables Rapid Identification of Bloodstream Infections
Channels
Clinical Chemistry
view channel
Saliva-Based Test Detects Biochemical Signs of Sleep Loss
Acute sleep loss impairs cognition and motor skills, raising safety risks that resemble alcohol intoxication. Clinicians currently lack an objective biochemical test to determine when someone is dangerously... Read more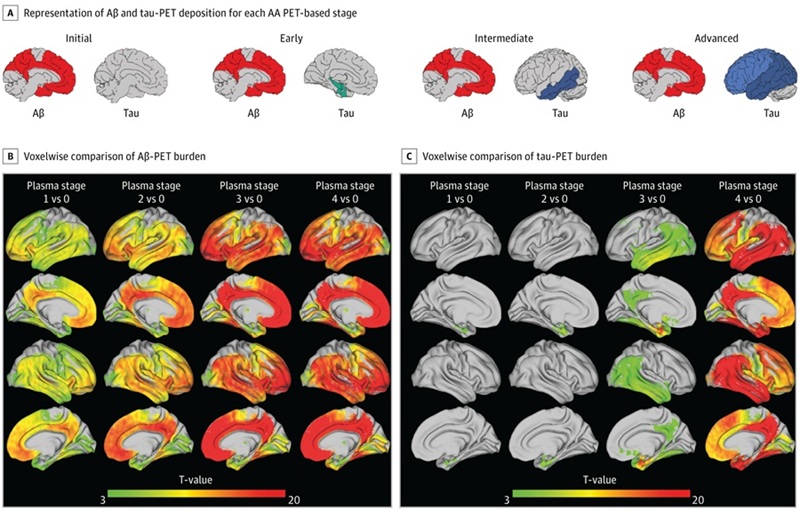
Simple Dual-Tau Blood Test Detects and Stages Alzheimer’s Disease
Alzheimer’s disease is typically confirmed and staged with positron emission tomography scans and cerebrospinal fluid testing, procedures that are costly and invasive. Broader access to minimally invasive... Read more
Alzheimer’s Blood Biomarkers Linked to Early Cognitive Differences Before Dementia
Blood-based screening for Alzheimer’s disease offers a noninvasive, lower-cost alternative to brain imaging or spinal fluid testing, yet its ability to flag the earliest cognitive changes has been unclear.... Read moreMolecular Diagnostics
view channel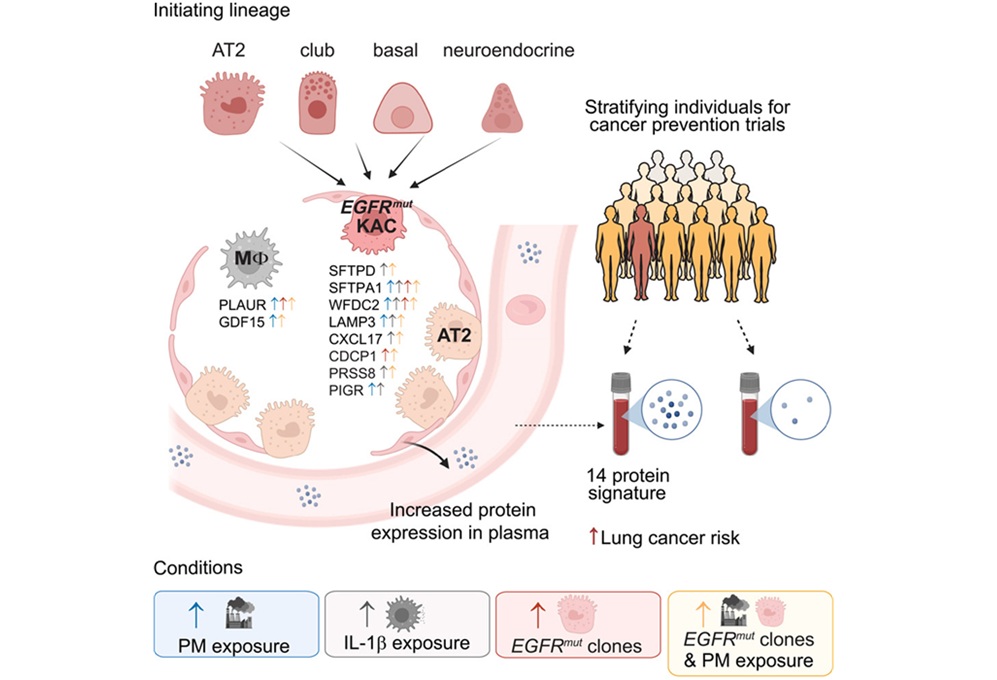
Plasma Protein Signature Predicts Lung Cancer Risk Up to Five Years Ahead
Lung cancer remains a leading cause of cancer death, and many cases are detected only after symptoms appear. Current screening programs largely target people with a history of smoking, leaving other at-risk... Read more
Circulating Tumor DNA Testing Guides Chemotherapy, Reduces Relapse in Colon Cancer
Adjuvant therapy decisions after curative surgery for colon cancer remain difficult, as conventional clinicopathologic factors often fail to capture residual disease risk. Liquid biopsy approaches that... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channelAptamer-Based Biosensor Enables Mutation-Resilient SARS-CoV-2 Detection
Rapid evolution of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can undermine existing molecular diagnostics, especially when assays target small viral components. Double-antibody sandwich... Read more
Study Points to Autoimmune Pathway Behind Long COVID Symptoms
Long COVID leaves many SARS-CoV-2 survivors with persistent fatigue, cognitive issues, palpitations, and musculoskeletal pain for months or years. Estimates cited in new research suggest 4%–20% of infected... Read more
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read morePathology
view channel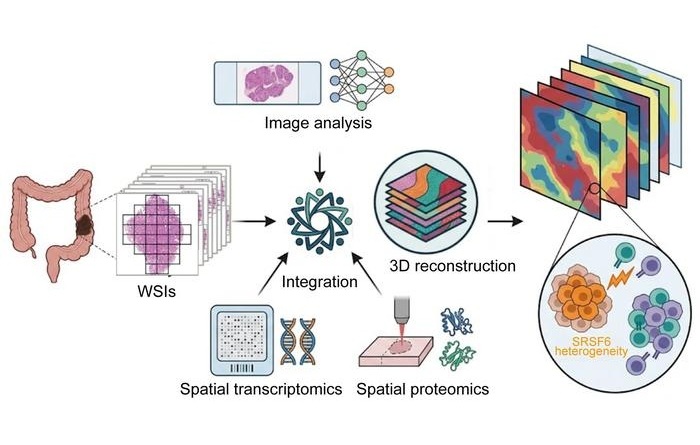
3D Spatial Multi-Omics Maps Intra-Tumor Diversity in Colorectal Cancer
Colorectal cancer remains a leading cause of cancer death, and clinical decision-making is complicated by marked intra-tumor heterogeneity. Conventional bulk sequencing averages molecular signals across... Read more
Blood-Based Method Tracks Gene Activity in the Living Brain
Real-time measurement of gene activity in the brain has been limited by assays requiring destructive tissue sampling. Tracking active genes could reveal how the body responds to environmental factors,... Read moreTechnology
view channel
AI Platform Links Biomarker Results to Cancer Clinical Trials and Guidelines
Oncology teams must manage growing volumes of genomic data, rapidly evolving clinical trial options, and frequently updated care guidelines, all within tight clinic schedules. Translating complex tumor... Read more
Agentic AI Platform Supports Genomic Decision-Making in Oncology
Oncology care teams increasingly face the challenge of managing complex molecular diagnostics, evolving treatment options, and extensive electronic health record documentation. Translating multimodal data... Read moreIndustry
view channel




.jpg)