Immune Relationship to Lung Tumor Evolution Characterized
|
By LabMedica International staff writers Posted on 04 Apr 2019 |
Image: A scanning electron micrograph (SEM) of lung cancer cells (Photo courtesy of Cancer Research UK).
Non-small-cell lung carcinoma (NSCLC) is any type of epithelial lung cancer other than small cell lung carcinoma (SCLC). NSCLC accounts for about 85% of all lung cancers. As a class, NSCLCs are relatively insensitive to chemotherapy, compared to small cell carcinoma.
The interplay between an evolving cancer and a dynamic immune microenvironment remains unclear. Scientists have started to unravel the complex relationships between immunoediting, immune cell infiltration, neoantigen formation, and clonal evolution in non-small cell lung cancer (NSCLC) tumors.
A team of scientists at the University College London Cancer Institute (London, UK) used RNA sequencing, tumor infiltrating lymphocyte analyses, reduced-representation bisulfite sequencing, and other approaches to assess hundreds of samples from 88 early-stage, untreated NSCLC cases, selected from a set of lung cancers previously profiled by multi-region exome sequencing for the Tracking Non-Small Cell Lung Cancer Evolution through Therapy (TRACERx) project.
Along with promoter methylation shifts for genes with new antigen-producing mutations, or neoantigens, the team saw differences in immune cell infiltration from one tumor to the next, and within different parts of the same NSCLC tumor. Those immune infiltration differences appeared to influence tumor immunoediting and the extent to which neoantigens turned up in the tumors, highlighting the combined impact that the tumor microenvironment, tumor mutations, and altered gene regulation can have on tumor evolution.
The group focused on immune cell infiltration in 258 regions from 88 NSCLCs in the exome-sequenced TRACERx 100 cohort, including 164 regions from 64 tumors that were assessed by RNA-seq. They also considered histopathology-based tumor infiltrating lymphocyte profiles for 234 regions from 83 NSCLC tumors. After looking at how well the RNA-seq-based immune estimates lined up with tumor infiltrating lymphocyte profiles generated by pathology, the team compared expression, mutation, and methylation features in the context of tumor region, immune cell infiltration levels, patient outcomes, and the histology of the NSCLC tumor involved.
The results indicated that more than 40% of the tumors had consistently low immune infiltration, while 28% apiece had either consistently high infiltration or immune infiltration that varied by region. In the latter tumors, they noted, variability in immune infiltration appeared to coincide with tumor mutation heterogeneity. In the NSCLC tumors with adenocarcinoma histology, the team saw declining sub-clonal diversity as CD8+ T cell infiltration increased, and vice versa, though this pattern did not hold in the lung squamous cell carcinoma cases.
The investigators found evidence supporting the notion that immune infiltration levels influenced tumor immunoediting, clonal evolution, and neoantigen loss through copy number changes or decreased transcript expression. With RRBS-based methylation analysis on 79 tumor samples from 28 cases, for example, they detected a significant uptick in promoter methylation in genes with non-expression neoantigens.
The authors concluded that their results provide evidence that tumor evolution is shaped through immunoediting mechanisms that affect either antigen presentation or neoantigenic mutations themselves, at both the DNA and RNA level arguing that the beneficial role of successful immune surveillance, and the diversity of immune-evasion mechanisms, should be considered and harnessed in immunotherapeutic interventions. The study was published on March 20, 2019, in the journal Nature.
Related Links:
University College London Cancer Institute
The interplay between an evolving cancer and a dynamic immune microenvironment remains unclear. Scientists have started to unravel the complex relationships between immunoediting, immune cell infiltration, neoantigen formation, and clonal evolution in non-small cell lung cancer (NSCLC) tumors.
A team of scientists at the University College London Cancer Institute (London, UK) used RNA sequencing, tumor infiltrating lymphocyte analyses, reduced-representation bisulfite sequencing, and other approaches to assess hundreds of samples from 88 early-stage, untreated NSCLC cases, selected from a set of lung cancers previously profiled by multi-region exome sequencing for the Tracking Non-Small Cell Lung Cancer Evolution through Therapy (TRACERx) project.
Along with promoter methylation shifts for genes with new antigen-producing mutations, or neoantigens, the team saw differences in immune cell infiltration from one tumor to the next, and within different parts of the same NSCLC tumor. Those immune infiltration differences appeared to influence tumor immunoediting and the extent to which neoantigens turned up in the tumors, highlighting the combined impact that the tumor microenvironment, tumor mutations, and altered gene regulation can have on tumor evolution.
The group focused on immune cell infiltration in 258 regions from 88 NSCLCs in the exome-sequenced TRACERx 100 cohort, including 164 regions from 64 tumors that were assessed by RNA-seq. They also considered histopathology-based tumor infiltrating lymphocyte profiles for 234 regions from 83 NSCLC tumors. After looking at how well the RNA-seq-based immune estimates lined up with tumor infiltrating lymphocyte profiles generated by pathology, the team compared expression, mutation, and methylation features in the context of tumor region, immune cell infiltration levels, patient outcomes, and the histology of the NSCLC tumor involved.
The results indicated that more than 40% of the tumors had consistently low immune infiltration, while 28% apiece had either consistently high infiltration or immune infiltration that varied by region. In the latter tumors, they noted, variability in immune infiltration appeared to coincide with tumor mutation heterogeneity. In the NSCLC tumors with adenocarcinoma histology, the team saw declining sub-clonal diversity as CD8+ T cell infiltration increased, and vice versa, though this pattern did not hold in the lung squamous cell carcinoma cases.
The investigators found evidence supporting the notion that immune infiltration levels influenced tumor immunoediting, clonal evolution, and neoantigen loss through copy number changes or decreased transcript expression. With RRBS-based methylation analysis on 79 tumor samples from 28 cases, for example, they detected a significant uptick in promoter methylation in genes with non-expression neoantigens.
The authors concluded that their results provide evidence that tumor evolution is shaped through immunoediting mechanisms that affect either antigen presentation or neoantigenic mutations themselves, at both the DNA and RNA level arguing that the beneficial role of successful immune surveillance, and the diversity of immune-evasion mechanisms, should be considered and harnessed in immunotherapeutic interventions. The study was published on March 20, 2019, in the journal Nature.
Related Links:
University College London Cancer Institute
Latest Immunology News
- Point-of-Care Tests Could Expand Access to Mpox Diagnosis
- T-Cell Senescence Profiling May Predict CAR T Responses
- Finger-Prick Lateral Flow Test Detects Sepsis Biomarkers at Point of Care
- Study Highlights Low Sensitivity of Current Lyme Tests in Early Infection
- Immune Aging Clock Quantifies Immunosenescence and Identifies Therapeutic Target
- Study Finds Influenza Often Undiagnosed in Winter Deaths
- Combined Screening Approach Identifies Early Leprosy Cases
- Antibody Blood Test Identifies Active TB and Distinguishes Latent Infection
- FDA Approval Expands Use of PD-L1 Companion Diagnostic in Esophageal and GEJ Carcinomas
- Study Identifies Inflammatory Pathway Driving Immunotherapy Resistance in Bladder Cancer
- Microfluidic Chip Detects Cancer Recurrence from Immune Response Signals
- Cancer Mutation ‘Fingerprints’ to Improve Prediction of Immunotherapy Response
- Immune Signature Identified in Treatment-Resistant Myasthenia Gravis
- New Biomarker Predicts Chemotherapy Response in Triple-Negative Breast Cancer
- Blood Test Identifies Lung Cancer Patients Who Can Benefit from Immunotherapy Drug
- Whole-Genome Sequencing Approach Identifies Cancer Patients Benefitting From PARP-Inhibitor Treatment
Channels
Clinical Chemistry
view channel
Ultrasensitive Test Detects Key Biomarker of Frontotemporal Dementia Subtype
Dementia affects more than 57 million people worldwide and is projected to nearly double within two decades, straining health systems and families. While biomarkers now enable accurate identification of... Read more
Routine Blood Tests Years Before Pregnancy Could Identify Preeclampsia Risk
High blood pressure during pregnancy is common and can progress to pre-eclampsia, making close monitoring at antenatal visits essential. However, most risk assessment begins only after pregnancy has started.... Read moreMolecular Diagnostics
view channel
Multiplex Respiratory Panel Integrates Automated Extraction to Streamline High-Volume Testing
Respiratory infections drive heavy testing volumes in clinical laboratories, where accurate, timely results across multiple pathogens are essential. Many labs are seeking to streamline workflows and increase... Read more
Whole-Blood RNA Test Predicts Disease Trajectory and Treatment Response
Clinicians often must predict whether acutely ill patients will recover or deteriorate despite limited time and clinical evidence. Earlier prognostic information could improve triage and guide treatment... Read more
Blood-Based Epigenetic Test Predicts GLP-1 Response and Tracks Treatment Effects
Prescriptions for GLP-1 medicines for weight loss are expanding rapidly, yet clinicians still lack scalable tools to predict biological response before treatment or monitor drug-driven changes beyond the scale.... Read moreHematology
view channel
Advanced CBC-Derived Indices Integrated into Hematology Platforms
Diatron, a STRATEC brand, has introduced six advanced hematological indices on its Aquila, Aquarius 3, and Abacus 5 hematology analyzers. The new Research Use Only (RUO) indices include Neutrophil-to-Lymphocyte... Read more
Blood Test Enables Early Detection of Multiple Myeloma Relapse
Bone marrow biopsies remain central to diagnosing and monitoring multiple myeloma, yet the procedure is painful, invasive, and often repeated over time. Older patients—who represent most new cases—can... Read moreMicrobiology
view channel
Rapid Antigen Biosensor Detects Active Tuberculosis in One Hour
Tuberculosis remains a major global health challenge and continues to drive significant morbidity and mortality. The World Health Organization’s 2024 global report cites it as the leading cause of death... Read more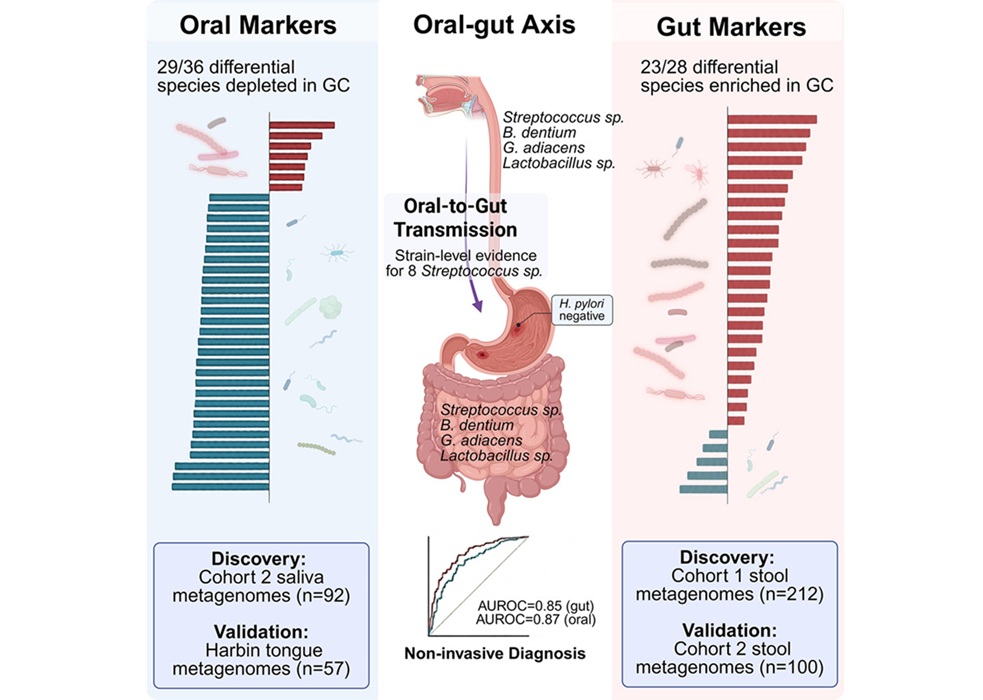
Oral–Gut Microbiome Signatures Identify Early Gastric Cancer
Early detection of gastric cancer could be advanced by scalable screening strategies using minimally invasive sampling. Saliva collection is noninvasive and cost-effective, supporting wider adoption... Read morePathology
view channel
FDA Clears AI Digital Pathology Tool for Breast Cancer Risk Stratification
Risk assessment at diagnosis is central to guiding therapy for early-stage, hormone receptor-positive, human epidermal growth factor receptor 2-negative (HR+/HER2-) invasive breast cancer, where overtreatment... Read more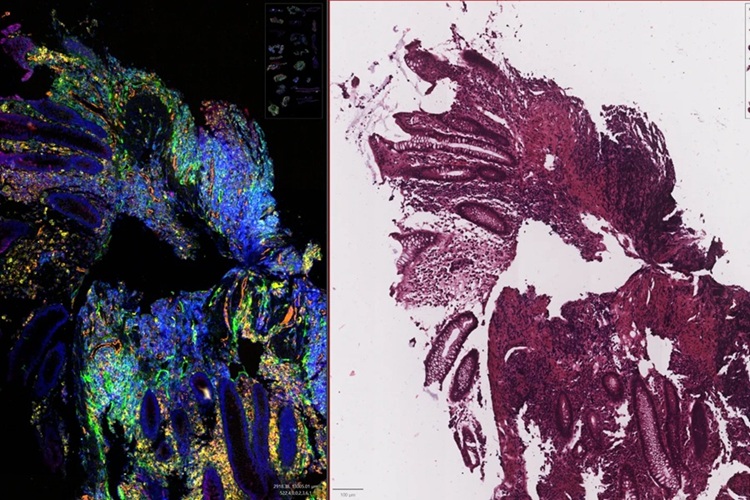
New AI Tool Reveals Hidden Genetic Signals in Routine H&E Slides
Pathologists worldwide rely on hematoxylin and eosin (H&E) slides to examine tissue architecture, yet these stains do not reveal the underlying molecular activity that often drives disease.... Read moreTechnology
view channel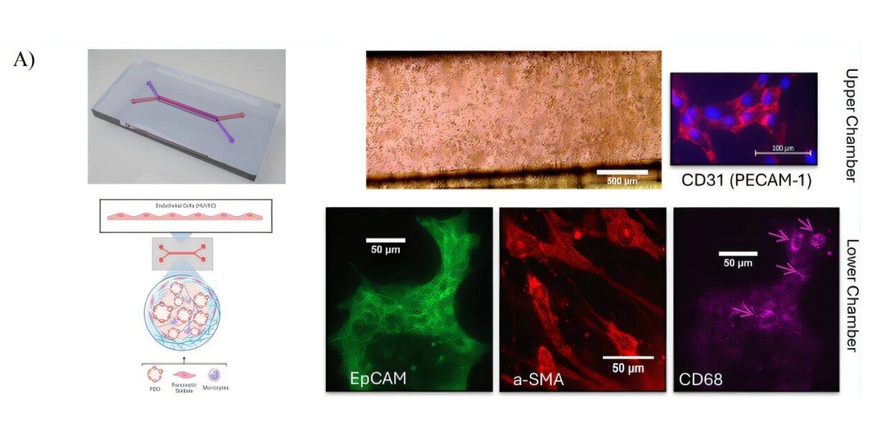
Tumor-on-a-Chip Platform Models Pancreatic Cancer Treatment Response
Pancreatic cancer remains one of the hardest malignancies to treat because tumors are embedded within a dense microenvironment that shapes growth and therapy response. Standard laboratory models often... Read more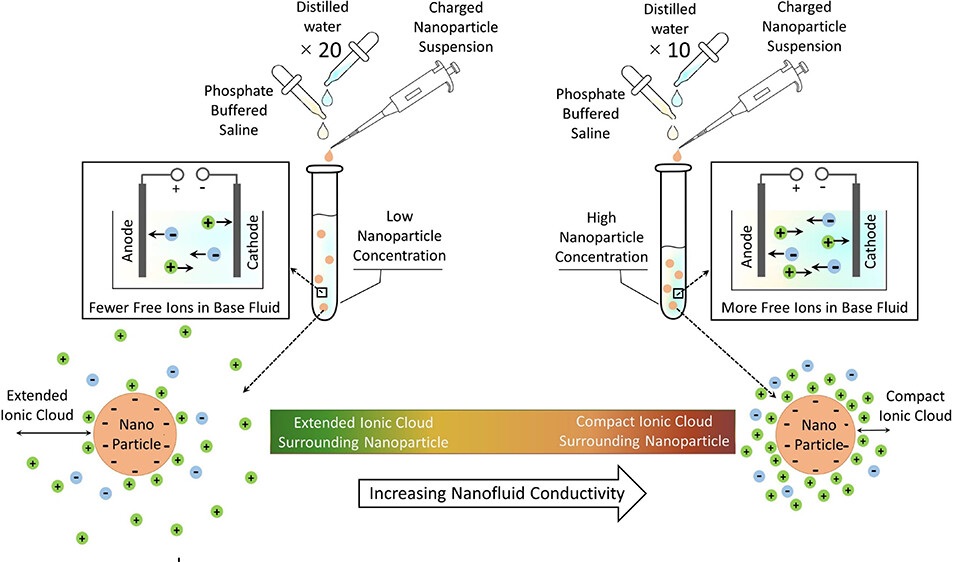
New Platform Captures Extracellular Vesicles for Early Cancer Detection
Early diagnosis remains the most effective way to reduce cancer mortality, yet many screening tools miss disease at its earliest stages. Biomarkers shed by tumors into blood and other fluids can be scarce... Read moreIndustry
view channel