Standalone HPV Testing Recommended for Cervical Cancer Screening
|
By LabMedica International staff writers Posted on 02 Oct 2018 |
The number of deaths from cervical cancer in the USA has decreased substantially since the implementation of widespread cervical cancer screening and has declined from 2.8 to 2.3 deaths per 100,000 women from 2000 to 2015.
The evidence on screening for cervical cancer has been reviewed with a focus on clinical trials and cohort studies that evaluated screening with high-risk human papillomavirus (hrHPV) testing alone or hrHPV and cytology together (co-testing) compared with cervical cytology alone.
The US Preventive Services Task Force (Rockville, MD, USA) besides reviewing and evaluating cervical cancer screening also commissioned a decision analysis model to evaluate the age at which to begin and end screening, the optimal interval for screening, the effectiveness of different screening strategies, and related benefits and harms of different screening strategies.
The experts reported on screening with cervical cytology alone, primary hrHPV testing alone, or co-testing can detect high-grade precancerous cervical lesions and cervical cancer. Screening women aged 21 to 65 years substantially reduces cervical cancer incidence and mortality. The harms of screening for cervical cancer in women aged 30 to 65 years are moderate. Four studies identified in the review found that primary hrHPV testing detected higher rates of stage 3 (or worse) cervical intraepithelial neoplasia compared with the standalone Pap test in the first round of testing. In comparing the Pap, hrHPV and co-testing methods, the latter two methods were associated with higher colposcopy and false-positive rates.
The scientists concluded with high certainty that the benefits of screening every three years with cytology alone in women aged 21 to 29 years substantially outweigh the harms. They also concluded with high certainty that the benefits of screening every three years with cytology alone, every five years with hrHPV testing alone, or every five years with both tests (co-testing) in women aged 30 to 65 years outweigh the harms. Screening women older than 65 years who have had adequate prior screening and women younger than 21 years does not provide significant benefit. The anticipation is hrHPV testing every five years for women aged 30 to 65 could reduce cervical cancer mortality from 8.34 to 0.29 deaths per 1,000 women.
Lee A. Learman, MD, PhD, professor of obstetrics and gynecology, said, “HPV testing every five years is an attractive option for patients who want to avoid pelvic exams and Pap smears. The Pap test is well known and accepted by patients and women’s healthcare providers, and there would need to be powerful incentives to move away from it. Switching from Pap tests annually to every three years has been the USPSTF recommendation since 2012, but patient and provider preferences have been hard to change. I expect the same phenomenon will delay implementation of primary HPV screening every 5 years.” The study was published on August 21, 2018, in the Journal of the American Medical Association.
Related Links:
US Preventive Services Task Force
The evidence on screening for cervical cancer has been reviewed with a focus on clinical trials and cohort studies that evaluated screening with high-risk human papillomavirus (hrHPV) testing alone or hrHPV and cytology together (co-testing) compared with cervical cytology alone.
The US Preventive Services Task Force (Rockville, MD, USA) besides reviewing and evaluating cervical cancer screening also commissioned a decision analysis model to evaluate the age at which to begin and end screening, the optimal interval for screening, the effectiveness of different screening strategies, and related benefits and harms of different screening strategies.
The experts reported on screening with cervical cytology alone, primary hrHPV testing alone, or co-testing can detect high-grade precancerous cervical lesions and cervical cancer. Screening women aged 21 to 65 years substantially reduces cervical cancer incidence and mortality. The harms of screening for cervical cancer in women aged 30 to 65 years are moderate. Four studies identified in the review found that primary hrHPV testing detected higher rates of stage 3 (or worse) cervical intraepithelial neoplasia compared with the standalone Pap test in the first round of testing. In comparing the Pap, hrHPV and co-testing methods, the latter two methods were associated with higher colposcopy and false-positive rates.
The scientists concluded with high certainty that the benefits of screening every three years with cytology alone in women aged 21 to 29 years substantially outweigh the harms. They also concluded with high certainty that the benefits of screening every three years with cytology alone, every five years with hrHPV testing alone, or every five years with both tests (co-testing) in women aged 30 to 65 years outweigh the harms. Screening women older than 65 years who have had adequate prior screening and women younger than 21 years does not provide significant benefit. The anticipation is hrHPV testing every five years for women aged 30 to 65 could reduce cervical cancer mortality from 8.34 to 0.29 deaths per 1,000 women.
Lee A. Learman, MD, PhD, professor of obstetrics and gynecology, said, “HPV testing every five years is an attractive option for patients who want to avoid pelvic exams and Pap smears. The Pap test is well known and accepted by patients and women’s healthcare providers, and there would need to be powerful incentives to move away from it. Switching from Pap tests annually to every three years has been the USPSTF recommendation since 2012, but patient and provider preferences have been hard to change. I expect the same phenomenon will delay implementation of primary HPV screening every 5 years.” The study was published on August 21, 2018, in the Journal of the American Medical Association.
Related Links:
US Preventive Services Task Force
Latest Microbiology News
- Rapid Antigen Biosensor Detects Active Tuberculosis in One Hour
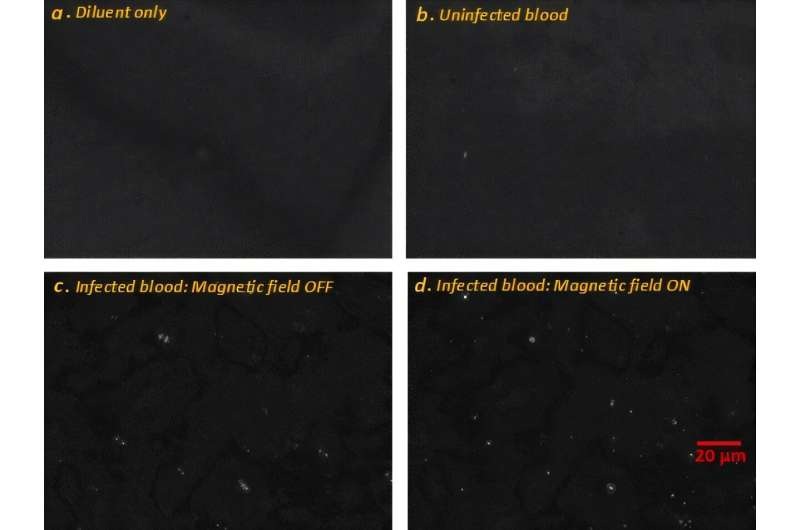
- Label-Free Microscopy Method Enables Faster, Quantitative Detection of Malaria
- Oral–Gut Microbiome Signatures Identify Early Gastric Cancer
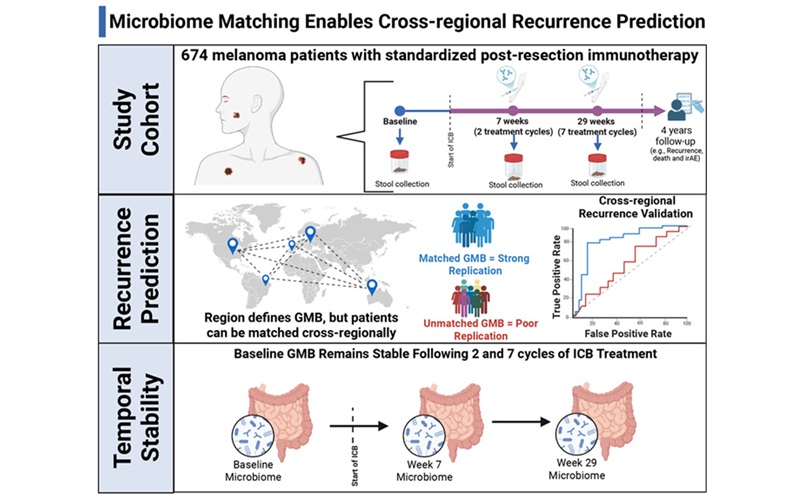
- Gut Microbiome Test Predicts Melanoma Recurrence After Surgery
- Rapid Blood-Culture Susceptibility Panel Expands Coverage for Gram-Negative Infections
- Antibiotic Resistance Genes Found in Newborns Within Hours of Birth
- Rapid Color Test Stratifies Virulent and Resistant Staph Strains
- mNGS CSF Test Identifies CNS Pathogens Missed by Standard Panels
- Syndromic Panel Enables Rapid Identification of Bloodstream Infections
- RNA-Based Workflow Identifies Active Skin Microbes for Dermatology Research
- Cost-Effective Sampling and Sequencing Workflow Identifies ICU Infection Hotspots
- New Bacterial Target Identified for Early Detection of Noma
- Genomic Analysis Links Emerging Streptococcal Strains to Specific Infections
- Rapid Urine Test Speeds Antibiotic Selection for UTIs
- WHO Endorses Rapid Point-of-Care Testing to Improve TB Detection
- Breath Analysis Approach Offers Rapid Detection of Bacterial Infection
Channels
Clinical Chemistry
view channel
Ultrasensitive Test Detects Key Biomarker of Frontotemporal Dementia Subtype
Dementia affects more than 57 million people worldwide and is projected to nearly double within two decades, straining health systems and families. While biomarkers now enable accurate identification of... Read more
Routine Blood Tests Years Before Pregnancy Could Identify Preeclampsia Risk
High blood pressure during pregnancy is common and can progress to pre-eclampsia, making close monitoring at antenatal visits essential. However, most risk assessment begins only after pregnancy has started.... Read moreMolecular Diagnostics
view channel
Liquid Biopsy Biomarkers Distinguish Inflammatory Breast Cancer and Support Monitoring
Inflammatory breast cancer is among the most aggressive forms of breast malignancy and remains challenging to diagnose and monitor. Obtaining tumor tissue can be difficult, and standard genome and RNA... Read more
Blood Test Maps Tumor Microenvironment to Predict Immunotherapy Response
Immunotherapy has transformed cancer care, yet durable benefit remains limited to a subset of patients, and clinicians still lack reliable tools to predict response before treatment begins.... Read more
Multiplex Respiratory Panel Integrates Automated Extraction to Streamline High-Volume Testing
Respiratory infections drive heavy testing volumes in clinical laboratories, where accurate, timely results across multiple pathogens are essential. Many labs are seeking to streamline workflows and increase... Read moreHematology
view channel
Advanced CBC-Derived Indices Integrated into Hematology Platforms
Diatron, a STRATEC brand, has introduced six advanced hematological indices on its Aquila, Aquarius 3, and Abacus 5 hematology analyzers. The new Research Use Only (RUO) indices include Neutrophil-to-Lymphocyte... Read more
Blood Test Enables Early Detection of Multiple Myeloma Relapse
Bone marrow biopsies remain central to diagnosing and monitoring multiple myeloma, yet the procedure is painful, invasive, and often repeated over time. Older patients—who represent most new cases—can... Read moreImmunology
view channel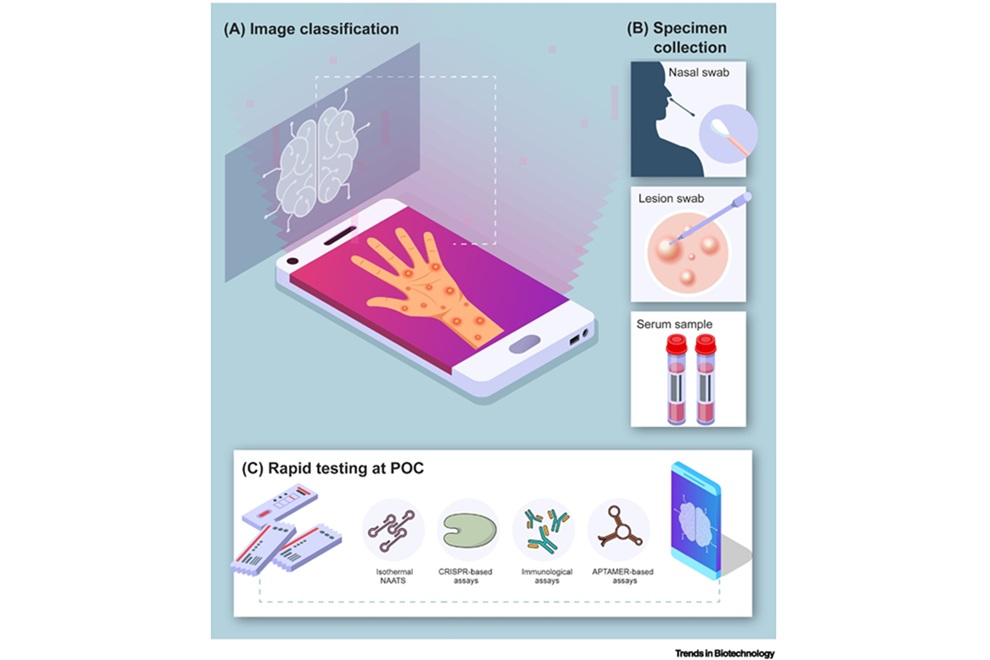
Point-of-Care Tests Could Expand Access to Mpox Diagnosis
Mpox outbreaks in non-endemic regions have underscored the need for rapid, accessible diagnostics to limit transmission. Polymerase chain reaction (PCR) remains the clinical reference, yet it depends on... Read more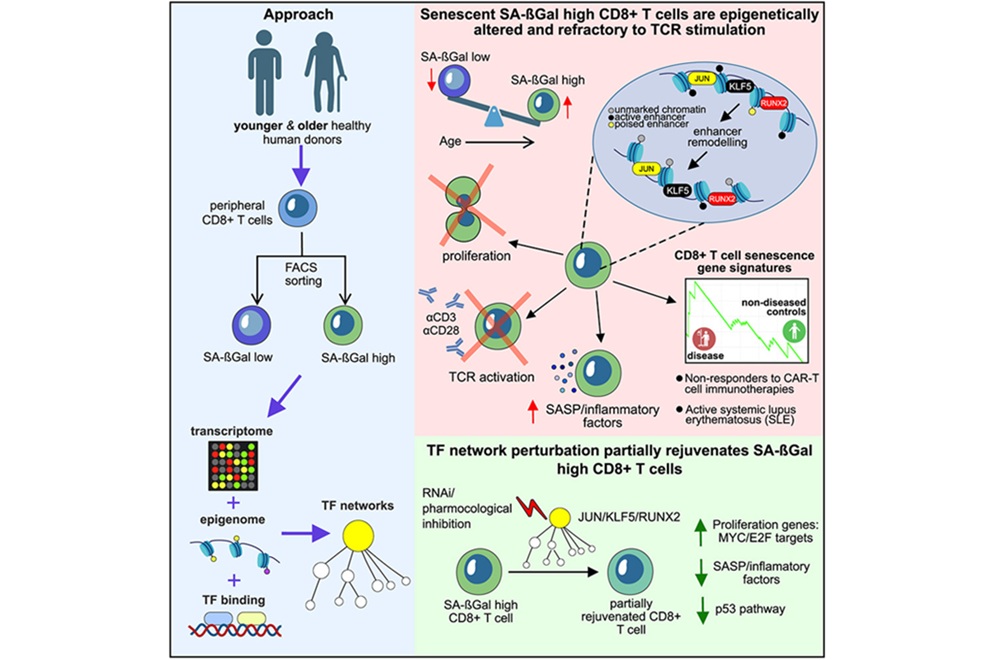
T-Cell Senescence Profiling May Predict CAR T Responses
Chimeric antigen receptor (CAR) T-cell therapy can deliver striking, durable remissions, yet many patients experience minimal or no benefit. The quality of patient-derived cytotoxic T lymphocytes used... Read moreMicrobiology
view channel
Rapid Antigen Biosensor Detects Active Tuberculosis in One Hour
Tuberculosis remains a major global health challenge and continues to drive significant morbidity and mortality. The World Health Organization’s 2024 global report cites it as the leading cause of death... Read more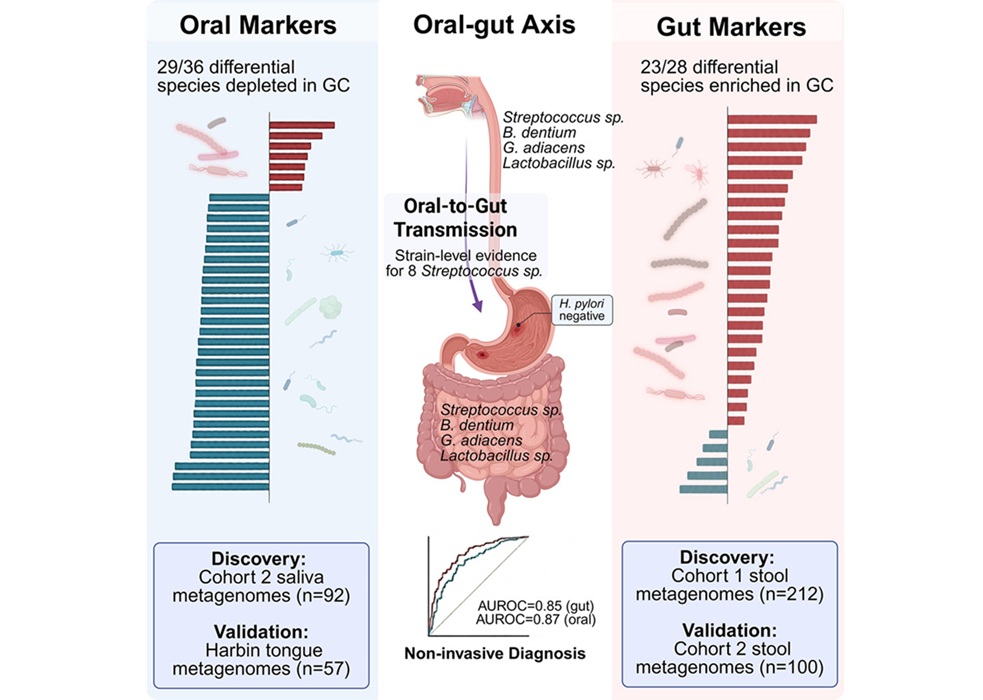
Oral–Gut Microbiome Signatures Identify Early Gastric Cancer
Early detection of gastric cancer could be advanced by scalable screening strategies using minimally invasive sampling. Saliva collection is noninvasive and cost-effective, supporting wider adoption... Read moreTechnology
view channel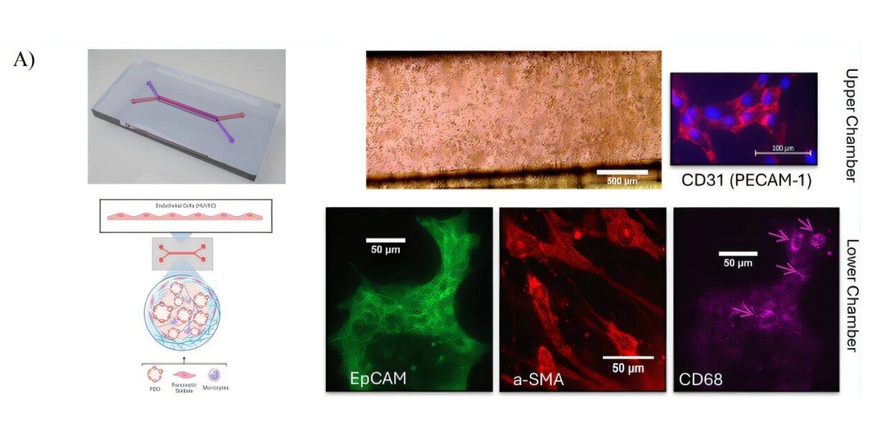
Tumor-on-a-Chip Platform Models Pancreatic Cancer Treatment Response
Pancreatic cancer remains one of the hardest malignancies to treat because tumors are embedded within a dense microenvironment that shapes growth and therapy response. Standard laboratory models often... Read more
New Platform Captures Extracellular Vesicles for Early Cancer Detection
Early diagnosis remains the most effective way to reduce cancer mortality, yet many screening tools miss disease at its earliest stages. Biomarkers shed by tumors into blood and other fluids can be scarce... Read moreIndustry
view channel
Roche to Acquire PathAI for Up to $1.05 Billion to Strengthen AI Diagnostics Portfolio
Roche has entered into a definitive merger agreement to acquire PathAI, a company focused on digital pathology and artificial intelligence for pathology laboratories and the biopharma industry.... Read more




.jpg)