Biomarker Identified for Novel Asthma Treatment
|
By LabMedica International staff writers Posted on 17 Sep 2018 |

Image: The LSM 780 inverted laser scanning confocal microscope (Photo courtesy of Zeiss).
Asthma is a widespread chronic airway disease characterized by airway obstruction, inflammation, and hyperresponsiveness. Symptoms such as bronchoconstriction and cough range from mild intermittent to severe persistent.
In eosinophilic asthma, the most common form of asthma, eosinophils in the airway alter nerve function and exacerbate the disease. However, whether eosinophils also affect airway nerve structure is unclear. In type 2-high asthma, interleukin-5 (IL-5) promotes eosinophil maturation, recruitment, and survival.
An international team of scientists working with the Oregon Health and Science University (Portland, OR, USA) evaluated airway sensory innervation and eosinophilia in humans with and without asthma and to characterize the physiologic consequences of eosinophil and airway nerve interactions using transgenic mice. Patients over the age of 17 were recruited and medication use, pulmonary function testing, blood eosinophil counts, serum immunoglobulin E (IgE) levels, and smoking history were obtained.
Human bronchial biopsies (three to five per subject) were taken from the bifurcation of the right middle lobe and immediately fixed in formalin overnight. Tissues were immunostained at 4 °C on a shaker. Airway nerves were labeled with rabbit polyclonal antibody against pan-neuronal marker PGP9.5 (protein gene product 9.5), and other immunostaining was performed and images were acquired using a Zeiss LSM 780 confocal microscope.
The scientists reported that subjects with a type 2-high asthma phenotype, defined as blood eosinophils greater than 300 cells/μL, had longer airway nerves and increased nerve branch points compared to control airways. In contrast, nerves in type 2-low asthmatics with blood eosinophils less than 300 cells/μL were not significantly different from healthy subjects. The mean blood eosinophils counts were 182 ± 93 μL in the 19 controls; 277 ± 289/μL in the 13 intermittent asthma patients; and 301 ± 225/μL in the persistent asthma sufferers. Moderate persistent asthmatics had increased eosinophil peroxidase both above and below the epithelial basement membrane compared to mild intermittent asthmatics and control subjects.
The authors concluded that their data indicated that airway nerves contribute to asthma pathology. They have shown that moderate persistent asthmatics have increased airway sensory innervation that is especially marked in asthmatics with accompanying eosinophilia. Richard W. Costello, MB, MD, FRCPI, a professor and a senior author of the study, said, “We identified that inflammatory cells, in particular, eosinophils, promote airway nerve growth in patients with asthma. These observations provide a unique insight into a fundamental mechanism of how the inflammation caused by asthma causes people to experience the symptoms of asthma such as coughing and breathlessness. This means that we now know which markers to look for in a patient with severe asthma. A patient with markers which show they have this particular form of asthma is likely to respond well to these new treatments.” The study was published on September 5, 2018, in the journal Science Translational Medicine.
Related Links:
Oregon Health and Science University
In eosinophilic asthma, the most common form of asthma, eosinophils in the airway alter nerve function and exacerbate the disease. However, whether eosinophils also affect airway nerve structure is unclear. In type 2-high asthma, interleukin-5 (IL-5) promotes eosinophil maturation, recruitment, and survival.
An international team of scientists working with the Oregon Health and Science University (Portland, OR, USA) evaluated airway sensory innervation and eosinophilia in humans with and without asthma and to characterize the physiologic consequences of eosinophil and airway nerve interactions using transgenic mice. Patients over the age of 17 were recruited and medication use, pulmonary function testing, blood eosinophil counts, serum immunoglobulin E (IgE) levels, and smoking history were obtained.
Human bronchial biopsies (three to five per subject) were taken from the bifurcation of the right middle lobe and immediately fixed in formalin overnight. Tissues were immunostained at 4 °C on a shaker. Airway nerves were labeled with rabbit polyclonal antibody against pan-neuronal marker PGP9.5 (protein gene product 9.5), and other immunostaining was performed and images were acquired using a Zeiss LSM 780 confocal microscope.
The scientists reported that subjects with a type 2-high asthma phenotype, defined as blood eosinophils greater than 300 cells/μL, had longer airway nerves and increased nerve branch points compared to control airways. In contrast, nerves in type 2-low asthmatics with blood eosinophils less than 300 cells/μL were not significantly different from healthy subjects. The mean blood eosinophils counts were 182 ± 93 μL in the 19 controls; 277 ± 289/μL in the 13 intermittent asthma patients; and 301 ± 225/μL in the persistent asthma sufferers. Moderate persistent asthmatics had increased eosinophil peroxidase both above and below the epithelial basement membrane compared to mild intermittent asthmatics and control subjects.
The authors concluded that their data indicated that airway nerves contribute to asthma pathology. They have shown that moderate persistent asthmatics have increased airway sensory innervation that is especially marked in asthmatics with accompanying eosinophilia. Richard W. Costello, MB, MD, FRCPI, a professor and a senior author of the study, said, “We identified that inflammatory cells, in particular, eosinophils, promote airway nerve growth in patients with asthma. These observations provide a unique insight into a fundamental mechanism of how the inflammation caused by asthma causes people to experience the symptoms of asthma such as coughing and breathlessness. This means that we now know which markers to look for in a patient with severe asthma. A patient with markers which show they have this particular form of asthma is likely to respond well to these new treatments.” The study was published on September 5, 2018, in the journal Science Translational Medicine.
Related Links:
Oregon Health and Science University
Latest Immunology News
- Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
- Immune Enzyme Linked to Treatment-Resistant Inflammatory Bowel Disease
- Simple Blood Test Could Replace Biopsies for Lung Transplant Rejection Monitoring
- Routine TB Screening Test May Reveal Immune Aging and Mortality Risk
- Biomarkers and Molecular Testing Advance Precision Allergy Care
- Point-of-Care Tests Could Expand Access to Mpox Diagnosis
- T-Cell Senescence Profiling May Predict CAR T Responses
- Finger-Prick Lateral Flow Test Detects Sepsis Biomarkers at Point of Care
- Study Highlights Low Sensitivity of Current Lyme Tests in Early Infection
- Immune Aging Clock Quantifies Immunosenescence and Identifies Therapeutic Target
- Study Finds Influenza Often Undiagnosed in Winter Deaths
- Combined Screening Approach Identifies Early Leprosy Cases
- Antibody Blood Test Identifies Active TB and Distinguishes Latent Infection
- FDA Approval Expands Use of PD-L1 Companion Diagnostic in Esophageal and GEJ Carcinomas
- Study Identifies Inflammatory Pathway Driving Immunotherapy Resistance in Bladder Cancer
- Microfluidic Chip Detects Cancer Recurrence from Immune Response Signals
Channels
Clinical Chemistry
view channel
Urine-Based Test Shows Promise for Autism Screening in Children
Autism spectrum disorder (ASD) is commonly diagnosed through behavioral assessments, which can involve long waits that delay intervention. Earlier identification is linked to better developmental outcomes,... Read more
Liquid Biopsy Biomarkers May Improve Childhood Epilepsy Diagnosis
Childhood epilepsy remains a major neurological disorder with unmet needs for accurate, non-invasive biomarkers, as conventional tests such as electroencephalography and neuroimaging can have limited sensitivity... Read moreMolecular Diagnostics
view channel
Updated Guidance Prioritizes Stool-Based Colorectal Cancer Screening Tests
Colorectal cancer is the second-leading cause of cancer death in the United States and claimed an estimated 55,000 lives in 2026. Incidence is rising among adults younger than 50, even as overall mortality... Read more
Digital PCR Assays Support Surveillance of Bundibugyo Ebolavirus Outbreak
QIAGEN (Venlo, Netherlands) has introduced two custom-designed research-use-only (RUO) QIAcuity dPCR assays to support infectious disease research and surveillance connected to the Bundibugyo ebolavirus outbreak.... Read more
Blood-Based Proteomic Test May Predict Treatment Response in Non-Small Cell Lung Cancer
Lung cancer remains the leading cause of cancer death, with non-small cell lung cancer (NSCLC) accounting for most cases. Treatment decisions are often made without a clear indication of how a patient... Read moreImmunology
view channel
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read more
Immune Enzyme Linked to Treatment-Resistant Inflammatory Bowel Disease
Inflammatory bowel disease (IBD) affects nearly 3 million people in the United States and its prevalence continues to rise. Medications that target tumor necrosis factor (TNF)-alpha are widely used, but... Read moreMicrobiology
view channel
Gut Microbiome Signatures Help Identify Risk of IBD Progression
Inflammatory bowel disease (IBD), encompassing Crohn’s disease and ulcerative colitis, is a chronic relapsing inflammatory disorder of the gastrointestinal tract with highly variable outcomes.... Read more
FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
Clinical guidelines support testing based on patient presentation in suspected gastrointestinal infections, yet available technologies have often forced laboratories to choose between panels that are too... Read morePathology
view channel
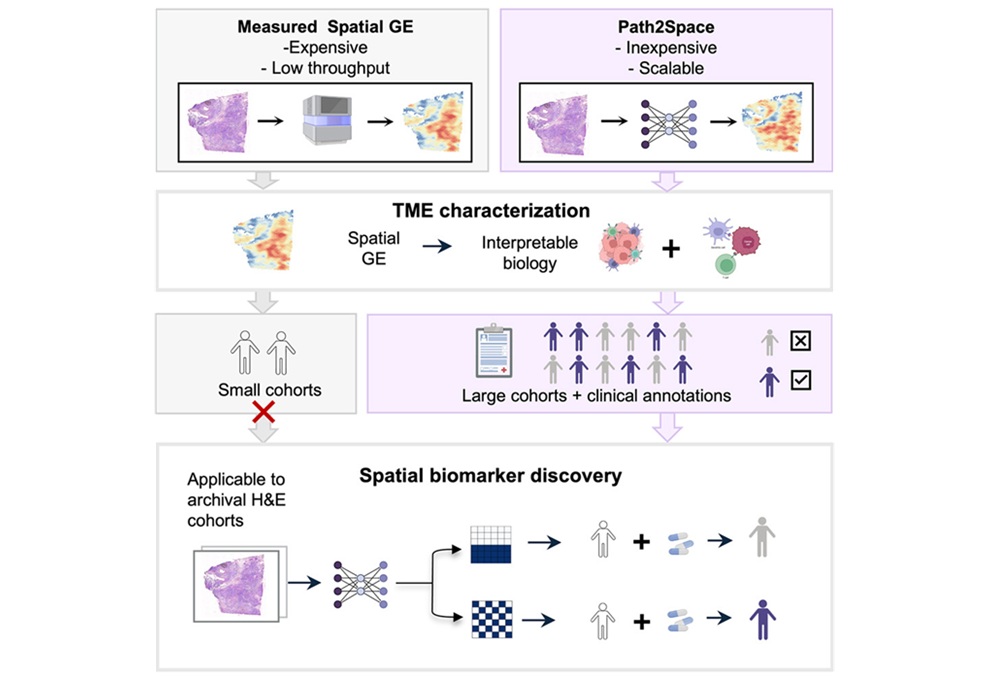
AI-Powered Atlas Maps Immune Structures Linked to Cancer Outcomes
Tertiary lymphoid structures are emerging as important indicators of antitumor immunity, but their heterogeneity and spatial context within tumors remain difficult to capture through routine diagnostics.... Read more
AI Tool Extracts Immune Signals from Biopsy to Inform Myeloma Therapy
Multiple myeloma is a bone marrow malignancy in which patients can respond very differently to the same treatments, making initial therapy decisions difficult. Clinicians must choose among options such... Read moreTechnology
view channel
Mailed Screening Kits Help Reduce Colorectal Cancer Screening Gaps
Colorectal cancer screening is a longstanding preventive priority, yet participation and follow-up remain uneven across patient groups. Safety‑net primary care settings often face barriers that limit screening... Read more
Algorithm Panel Aids Liver Fibrosis Assessment and Liver Cancer Surveillance
Chronic liver disease is common and often progresses silently, increasing the risk of cirrhosis and hepatocellular carcinoma when not detected early. With an estimated 1.5 billion people affected worldwide... Read moreIndustry
view channelWerfen and Oxford Nanopore Collaborate on Transplant Assay Development
Werfen (Barcelona, Spain), a global specialized diagnostics company, has announced a strategic collaboration with Oxford Nanopore Technologies (Oxford, UK), which develops nanopore-based sequencing technology,... Read more