Eosinophilic Biomarker Found for Aggressive IBD
|
By LabMedica International staff writers Posted on 14 Dec 2017 |
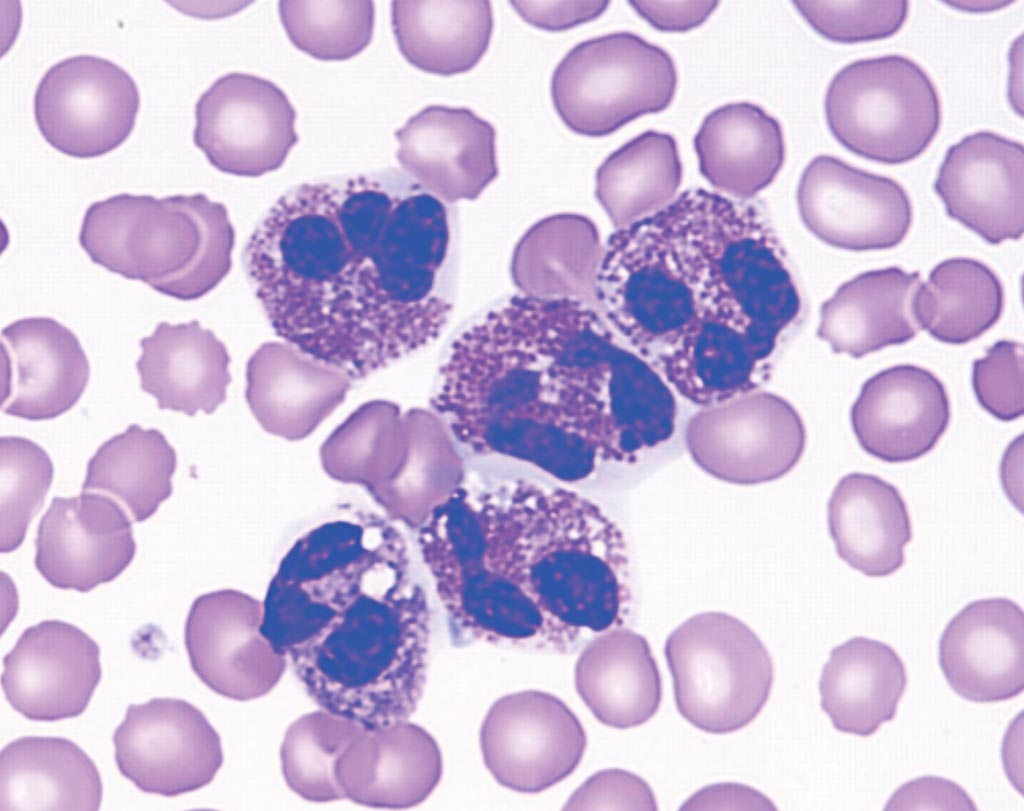
Image: Peripheral bloods smear showing five eosinophils, from a patient with eosinophilia (Photo courtesy of the Hospital for Sick Children, Toronto).
Peripheral blood eosinophilia (PBE) in inflammatory bowel disease is associated with ulcerative colitis (UC) and active disease. Little data exist on the long-term impact of PBE on disease course.
Inflammatory bowel disease (IBD) is a term mainly used to describe two conditions: ulcerative colitis and Crohn's disease. Ulcerative colitis and Crohn's disease are long-term conditions that involve inflammation of the gut. Ulcerative colitis only affects the colon or large intestine.
A large group of medical scientists working with the University of Pittsburgh Medical Center (Pittsburgh, PN, USA) performed a registry analysis of a consented, prospective, natural history IBD cohort at a tertiary center from 2009 to 2014. Demographics, comorbidities, disease activity, healthcare utilization, and time to hospitalization or surgical resection of patients who displayed PBE were compared to patients without PBE.
The team reported that of the 2,066 IBD patients, 19.2% developed PBE. PBE was significantly associated with UC, extensive colitis, and shorter disease duration. Over six years, PBE patients had more active disease, concurrent C-reactive protein elevation, healthcare utilization (hospitalization and IBD surgery), and more aggressive medical therapy (prednisone and anti- tumor necrosis factor). Patients with PBE had a significantly reduced time to hospitalization in both UC and Crohn’s disease (CD) and reduced time to colectomy in UC. PBE remained significantly associated with hospitalization and surgery in both CD and UC. New diagnosis of UC with PBE was associated with increased steroid and anti- tumor necrosis factor requirement.
The authors concluded that the multi-year study of a large IBD cohort suggests that peripheral blood eosinophilia represents a biomarker of a distinct IBD subgroup, with a unique inflammatory signature, and at risk for worse clinical outcomes. The study was published on November 7, 2017, in The American Journal of Gastroenterology.
Related Links:
University of Pittsburgh Medical Center
Inflammatory bowel disease (IBD) is a term mainly used to describe two conditions: ulcerative colitis and Crohn's disease. Ulcerative colitis and Crohn's disease are long-term conditions that involve inflammation of the gut. Ulcerative colitis only affects the colon or large intestine.
A large group of medical scientists working with the University of Pittsburgh Medical Center (Pittsburgh, PN, USA) performed a registry analysis of a consented, prospective, natural history IBD cohort at a tertiary center from 2009 to 2014. Demographics, comorbidities, disease activity, healthcare utilization, and time to hospitalization or surgical resection of patients who displayed PBE were compared to patients without PBE.
The team reported that of the 2,066 IBD patients, 19.2% developed PBE. PBE was significantly associated with UC, extensive colitis, and shorter disease duration. Over six years, PBE patients had more active disease, concurrent C-reactive protein elevation, healthcare utilization (hospitalization and IBD surgery), and more aggressive medical therapy (prednisone and anti- tumor necrosis factor). Patients with PBE had a significantly reduced time to hospitalization in both UC and Crohn’s disease (CD) and reduced time to colectomy in UC. PBE remained significantly associated with hospitalization and surgery in both CD and UC. New diagnosis of UC with PBE was associated with increased steroid and anti- tumor necrosis factor requirement.
The authors concluded that the multi-year study of a large IBD cohort suggests that peripheral blood eosinophilia represents a biomarker of a distinct IBD subgroup, with a unique inflammatory signature, and at risk for worse clinical outcomes. The study was published on November 7, 2017, in The American Journal of Gastroenterology.
Related Links:
University of Pittsburgh Medical Center
Latest Pathology News
- 3D Spatial Multi-Omics Maps Intra-Tumor Diversity in Colorectal Cancer
- Blood-Based Method Tracks Gene Activity in the Living Brain
- FDA Approval Expands Automated PD-L1 Testing Across Solid Tumors
- AI-Powered Atlas Maps Immune Structures Linked to Cancer Outcomes
- AI Tool Extracts Immune Signals from Biopsy to Inform Myeloma Therapy
- Rapid AI Tool Predicts Cancer Spatial Gene Expression from Pathology Images
- AI Pathology Test Receives FDA Breakthrough for Bladder Cancer Risk Stratification
- FDA Clears AI Digital Pathology Tool for Breast Cancer Risk Stratification
- New AI Tool Reveals Hidden Genetic Signals in Routine H&E Slides
- AI System Analyzes Routine Pathology Slides to Predict Cancer Outcomes
- New Tissue Mapping Approach Identifies High-Risk Form of Diabetic Kidney Disease
- Multimodal AI Tool Predicts Genetic Alterations to Guide Breast Cancer Treatment
- Interpretable AI Reveals Hidden Cellular Features from Microscopy Images
- Tumor Immune Structure Predicts Response to Immunotherapy in Melanoma
- Plug-and-Play AI Pathology System Classifies Multiple Cancers from Few Slides
- AI-Based Assays Support Risk Stratification in Prostate and Breast Cancer
Channels
Clinical Chemistry
view channel
Saliva-Based Test Detects Biochemical Signs of Sleep Loss
Acute sleep loss impairs cognition and motor skills, raising safety risks that resemble alcohol intoxication. Clinicians currently lack an objective biochemical test to determine when someone is dangerously... Read more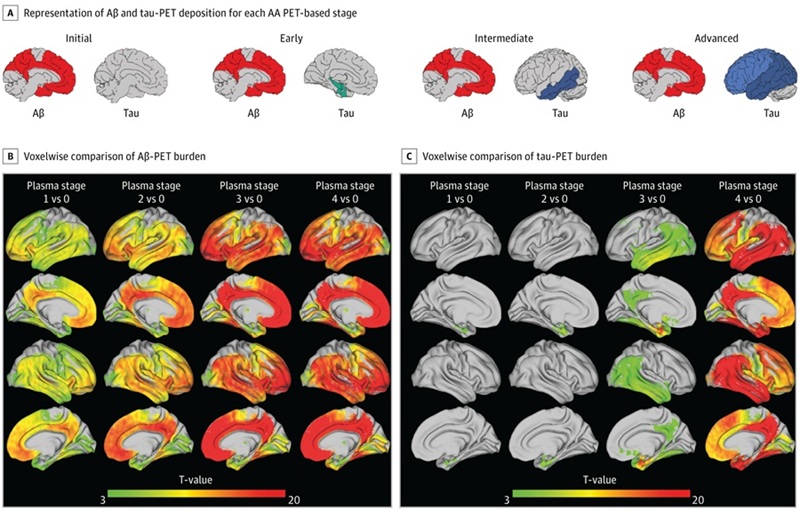
Simple Dual-Tau Blood Test Detects and Stages Alzheimer’s Disease
Alzheimer’s disease is typically confirmed and staged with positron emission tomography scans and cerebrospinal fluid testing, procedures that are costly and invasive. Broader access to minimally invasive... Read more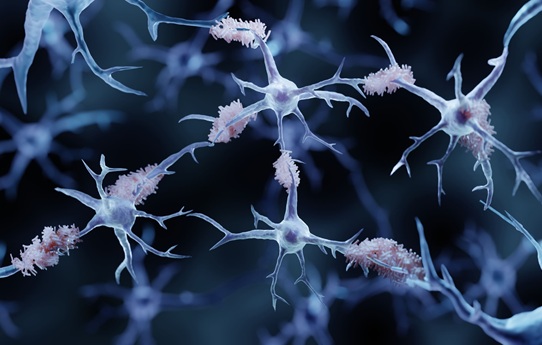
Alzheimer’s Blood Biomarkers Linked to Early Cognitive Differences Before Dementia
Blood-based screening for Alzheimer’s disease offers a noninvasive, lower-cost alternative to brain imaging or spinal fluid testing, yet its ability to flag the earliest cognitive changes has been unclear.... Read moreMolecular Diagnostics
view channel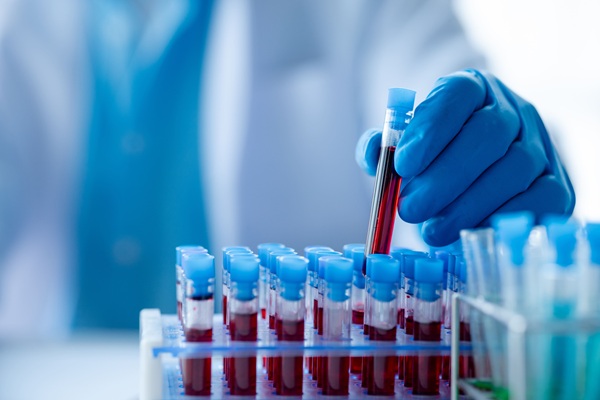
Blood Test Predicts Immunotherapy Response in Head and Neck Cancer
Head and neck squamous cell carcinoma affects hundreds of thousands of people worldwide each year, yet response rates to immunotherapy remain low. Clinicians lack reliable, minimally invasive tools to... Read more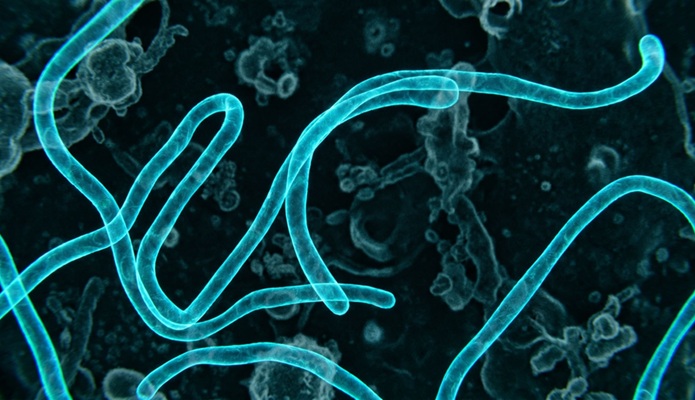
New PCR Assay Supports Bundibugyo Ebola Outbreak Surveillance
Rapid identification of Ebola infections is essential to limit transmission and guide public health response, yet detection can be difficult when outbreaks involve rare variants. The current outbreaks... Read moreImmunology
view channelAptamer-Based Biosensor Enables Mutation-Resilient SARS-CoV-2 Detection
Rapid evolution of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can undermine existing molecular diagnostics, especially when assays target small viral components. Double-antibody sandwich... Read more
Study Points to Autoimmune Pathway Behind Long COVID Symptoms
Long COVID leaves many SARS-CoV-2 survivors with persistent fatigue, cognitive issues, palpitations, and musculoskeletal pain for months or years. Estimates cited in new research suggest 4%–20% of infected... Read more
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read moreMicrobiology
view channel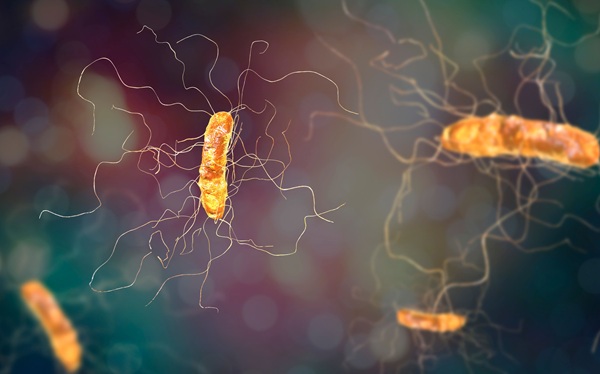
New Culture Medium Speeds C. difficile Resistance Detection and Reduces Costs
Clostridioides difficile infections remain a persistent threat in hospitals and communities, affecting about 500,000 people in the United States each year. Severe cases can be fatal within 30 days of diagnosis,... Read more
Automated Blood Culture System Speeds Detection of Bloodstream Infections
Bloodstream infections and sepsis require rapid laboratory detection to guide targeted antimicrobial therapy and reduce mortality. Conventional blood culture workflows can delay actionable results by critical... Read morePathology
view channel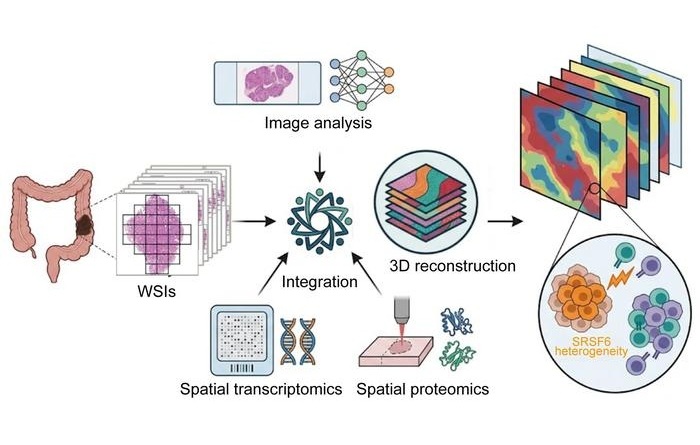
3D Spatial Multi-Omics Maps Intra-Tumor Diversity in Colorectal Cancer
Colorectal cancer remains a leading cause of cancer death, and clinical decision-making is complicated by marked intra-tumor heterogeneity. Conventional bulk sequencing averages molecular signals across... Read more
Blood-Based Method Tracks Gene Activity in the Living Brain
Real-time measurement of gene activity in the brain has been limited by assays requiring destructive tissue sampling. Tracking active genes could reveal how the body responds to environmental factors,... Read moreTechnology
view channel
AI Platform Links Biomarker Results to Cancer Clinical Trials and Guidelines
Oncology teams must manage growing volumes of genomic data, rapidly evolving clinical trial options, and frequently updated care guidelines, all within tight clinic schedules. Translating complex tumor... Read more
Agentic AI Platform Supports Genomic Decision-Making in Oncology
Oncology care teams increasingly face the challenge of managing complex molecular diagnostics, evolving treatment options, and extensive electronic health record documentation. Translating multimodal data... Read moreIndustry
view channel
Collaboration Advances ctDNA-Guided Development in Metastatic Colorectal Cancer
Natera, Inc. (Austin, TX, USA) and CytoDyn Inc. (Vancouver, WA, USA) announced a strategic collaboration focused on metastatic colorectal cancer (mCRC). Under the agreement, Natera will evaluate circulating... Read more