Test Detects Overdose Patients at Risk of Liver Damage
|
By LabMedica International staff writers Posted on 28 Nov 2017 |
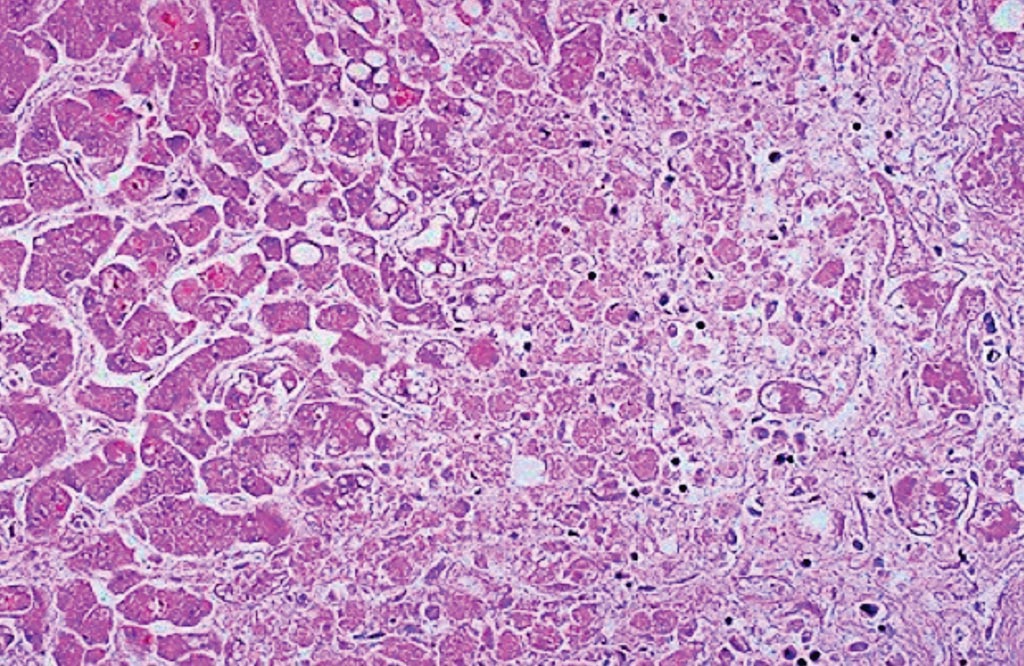
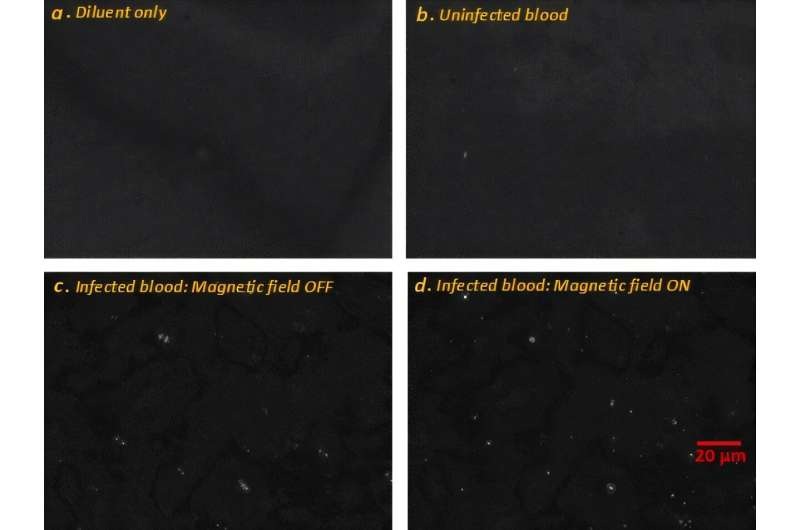
Image: A histopathology of extensive hepatocyte necrosis seen here in a case of paracetamol overdose. The hepatocytes at the right are dead, and those at the left are dying. This pattern can be seen with a variety of hepatotoxins (Photo courtesy of the University of Utah Medical School).
Paracetamol is a safe analgesic drug when taken at therapeutic doses; however, in overdose, paracetamol is hepatotoxic and is the most common cause of acute liver failure in the USA and Europe.
Current markers, serum alanine aminotransferase (ALT) activity and paracetamol concentration, lack sensitivity and specificity when measured soon after overdose such as at initial presentation to hospital. These limitations are further compounded in staggered overdose, for which there is an increased acute liver injury risk, but for which treatment nomograms are not recommended.
A team of medical scientists by the University of Liverpool (Liverpool, UK) and the University of Edinburgh (Edinburgh, UK) recruited two cohorts to assess the potential for biomarkers to stratify patients who overdose with paracetamol. The team completed two independent prospective studies: a derivation study (MAPP) in eight UK hospitals and a validation study (BIOPAR) in ten UK hospitals. Patients in both cohorts were adults (≥18 years in England, ≥16 years in Scotland), were diagnosed with paracetamol overdose.
Blood sample taken at first presentation to hospital was stored at −80 °C as plasma or serum. All blood results from the first hospital admission were recorded (paracetamol, alkaline phosphatase, γ-glutamyl transferase, bilirubin, creatinine, and alanine aminotransferase (ALT) concentration, prothrombin time, and international normalized ratio [INR]). The primary endpoint was acute liver injury indicating need for continued acetylcysteine treatment beyond the standard course (ALT activity >100 U/L.
The reference standard of injury was ALT concentration. MicroRNA-122 (miR-122), high mobility group box-1 (HMGB1), caspase-cleaved keratin-18 (K18), full-length K18, and glutamate dehydrogenase (GLDH) were measured in the admission blood sample, with miR-122 measured by polymerase chain reaction (PCR) and other markers measured by enzyme-linked immunosorbent assay (ELISA). Each biomarker was measured in each sample in duplicate. miR-122 concentration was expressed with reference to the circulating microRNA let-7d as the internal microRNA normalizer.
The team reported that between June 2, 2010, and May 29, 2014, 1,187 patients who required acetylcysteine treatment for paracetamol overdose were recruited (985 in the MAPP cohort; 202 in the BIOPAR cohort). In the derivation and validation cohorts, acute liver injury was predicted at hospital presentation by miR-122, HMGB1, and full-length K18, and results were similar in the validation cohort. A combined model of miR-122, HMGB1, and K18 predicted acute liver injury better than ALT alone.
James W Dear, FRCP, the lead author of the study, said, “Paracetamol overdose is very common and presents a large workload for already over-stretched Emergency Departments. These new blood tests can identify who will develop liver injury as soon as they first arrive at hospital. This could transform the care of this large, neglected, patient group.” The study was published on November 13, 2017, in the journal Lancet Gastroenterology & Hepatology.
Related Links:
University of Liverpool
University of Edinburgh
Current markers, serum alanine aminotransferase (ALT) activity and paracetamol concentration, lack sensitivity and specificity when measured soon after overdose such as at initial presentation to hospital. These limitations are further compounded in staggered overdose, for which there is an increased acute liver injury risk, but for which treatment nomograms are not recommended.
A team of medical scientists by the University of Liverpool (Liverpool, UK) and the University of Edinburgh (Edinburgh, UK) recruited two cohorts to assess the potential for biomarkers to stratify patients who overdose with paracetamol. The team completed two independent prospective studies: a derivation study (MAPP) in eight UK hospitals and a validation study (BIOPAR) in ten UK hospitals. Patients in both cohorts were adults (≥18 years in England, ≥16 years in Scotland), were diagnosed with paracetamol overdose.
Blood sample taken at first presentation to hospital was stored at −80 °C as plasma or serum. All blood results from the first hospital admission were recorded (paracetamol, alkaline phosphatase, γ-glutamyl transferase, bilirubin, creatinine, and alanine aminotransferase (ALT) concentration, prothrombin time, and international normalized ratio [INR]). The primary endpoint was acute liver injury indicating need for continued acetylcysteine treatment beyond the standard course (ALT activity >100 U/L.
The reference standard of injury was ALT concentration. MicroRNA-122 (miR-122), high mobility group box-1 (HMGB1), caspase-cleaved keratin-18 (K18), full-length K18, and glutamate dehydrogenase (GLDH) were measured in the admission blood sample, with miR-122 measured by polymerase chain reaction (PCR) and other markers measured by enzyme-linked immunosorbent assay (ELISA). Each biomarker was measured in each sample in duplicate. miR-122 concentration was expressed with reference to the circulating microRNA let-7d as the internal microRNA normalizer.
The team reported that between June 2, 2010, and May 29, 2014, 1,187 patients who required acetylcysteine treatment for paracetamol overdose were recruited (985 in the MAPP cohort; 202 in the BIOPAR cohort). In the derivation and validation cohorts, acute liver injury was predicted at hospital presentation by miR-122, HMGB1, and full-length K18, and results were similar in the validation cohort. A combined model of miR-122, HMGB1, and K18 predicted acute liver injury better than ALT alone.
James W Dear, FRCP, the lead author of the study, said, “Paracetamol overdose is very common and presents a large workload for already over-stretched Emergency Departments. These new blood tests can identify who will develop liver injury as soon as they first arrive at hospital. This could transform the care of this large, neglected, patient group.” The study was published on November 13, 2017, in the journal Lancet Gastroenterology & Hepatology.
Related Links:
University of Liverpool
University of Edinburgh
Latest Clinical Chem. News
- Ultrasensitive Test Detects Key Biomarker of Frontotemporal Dementia Subtype
- Routine Blood Tests Years Before Pregnancy Could Identify Preeclampsia Risk
- Blood Test Detects Testicular Cancer Missed by Standard Markers
- Routine Blood Tests Identify Biomarkers Linked to PTSD
- Proteomic Data Underscore Need for Age-Specific Pediatric Reference Ranges
- Routine Blood Count Ratio Linked to Future Alzheimer’s and Dementia Risk
- Label-Free Microfluidic Device Enriches Tumor Cells and Clusters from Pleural Effusions
- Rapid Biosensor Detects Pancreatic Cancer Biomarker for Early Detection
- Urine-Based Multi-Cancer Screening Test Receives FDA Breakthrough Device Designation
- Blood Test Predicts Alzheimer Disease Risk Before Imaging Changes and Symptoms
- Study Finds ApoB Testing More Effective Than LDL for Guiding Lipid Therapy
- AI-Enabled POC Test Quantifies Multiple Cardiac Biomarkers
- Next Generation Automated Analyzers Increase Throughput for Clinical Chemistry and Electrolyte Testing
- Blood Metabolite Test Detects Early Cognitive Decline
- AI-Based Blood Test Diagnose Multiple Brain Disorders from Blood Sample
- Automated NfL Assay Supports Monitoring of Neurological Disorders
Channels
Molecular Diagnostics
view channel
Liquid Biopsy Biomarkers Distinguish Inflammatory Breast Cancer and Support Monitoring
Inflammatory breast cancer is among the most aggressive forms of breast malignancy and remains challenging to diagnose and monitor. Obtaining tumor tissue can be difficult, and standard genome and RNA... Read more
Blood Test Maps Tumor Microenvironment to Predict Immunotherapy Response
Immunotherapy has transformed cancer care, yet durable benefit remains limited to a subset of patients, and clinicians still lack reliable tools to predict response before treatment begins.... Read more
Multiplex Respiratory Panel Integrates Automated Extraction to Streamline High-Volume Testing
Respiratory infections drive heavy testing volumes in clinical laboratories, where accurate, timely results across multiple pathogens are essential. Many labs are seeking to streamline workflows and increase... Read moreHematology
view channel
Advanced CBC-Derived Indices Integrated into Hematology Platforms
Diatron, a STRATEC brand, has introduced six advanced hematological indices on its Aquila, Aquarius 3, and Abacus 5 hematology analyzers. The new Research Use Only (RUO) indices include Neutrophil-to-Lymphocyte... Read more
Blood Test Enables Early Detection of Multiple Myeloma Relapse
Bone marrow biopsies remain central to diagnosing and monitoring multiple myeloma, yet the procedure is painful, invasive, and often repeated over time. Older patients—who represent most new cases—can... Read moreImmunology
view channel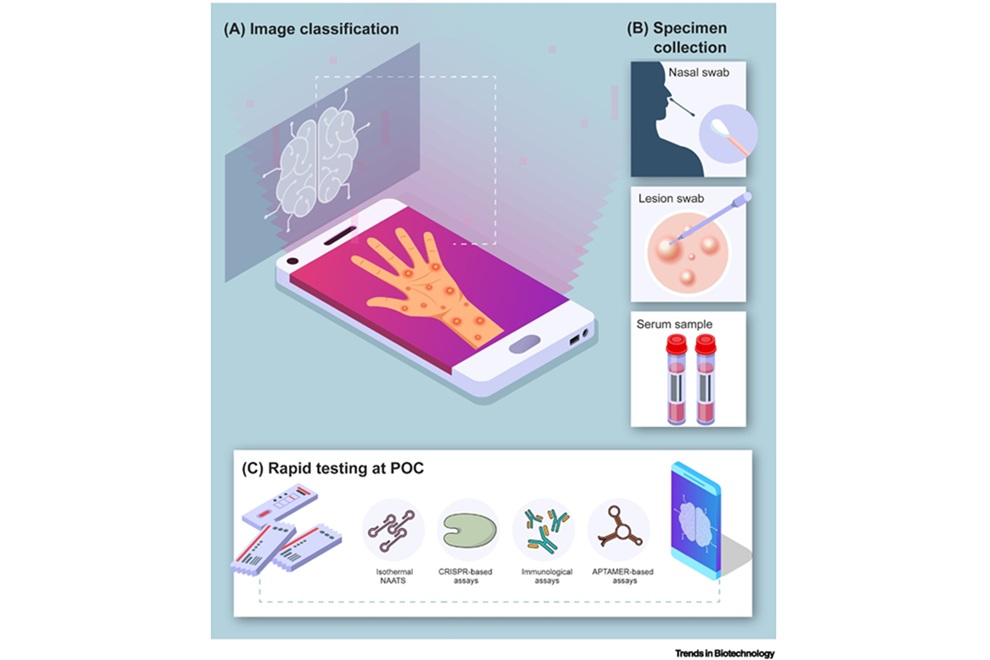
Point-of-Care Tests Could Expand Access to Mpox Diagnosis
Mpox outbreaks in non-endemic regions have underscored the need for rapid, accessible diagnostics to limit transmission. Polymerase chain reaction (PCR) remains the clinical reference, yet it depends on... Read more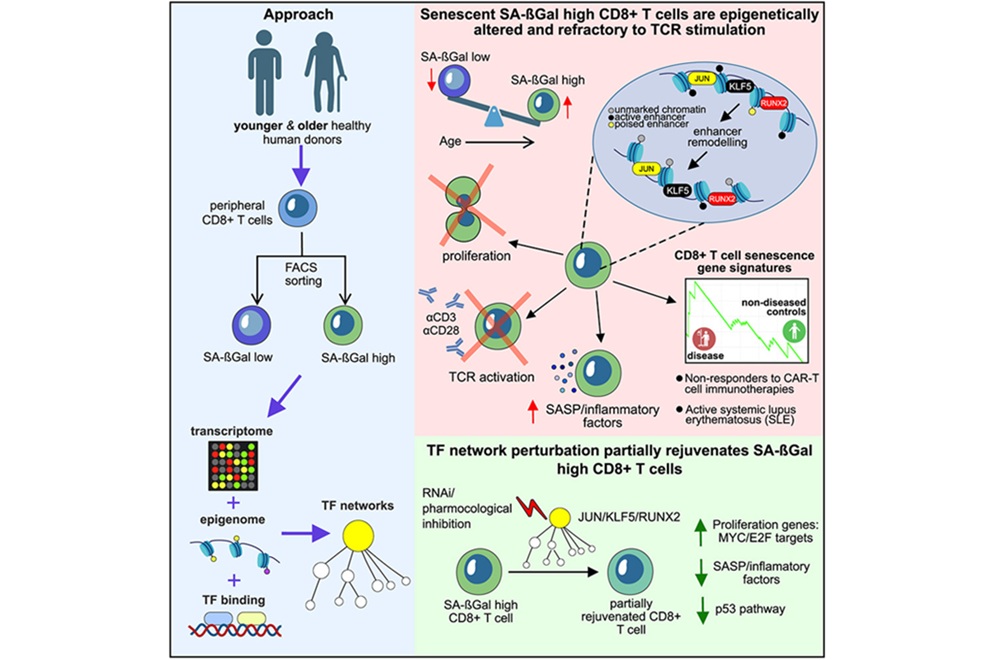
T-Cell Senescence Profiling May Predict CAR T Responses
Chimeric antigen receptor (CAR) T-cell therapy can deliver striking, durable remissions, yet many patients experience minimal or no benefit. The quality of patient-derived cytotoxic T lymphocytes used... Read moreMicrobiology
view channel
Rapid Antigen Biosensor Detects Active Tuberculosis in One Hour
Tuberculosis remains a major global health challenge and continues to drive significant morbidity and mortality. The World Health Organization’s 2024 global report cites it as the leading cause of death... Read more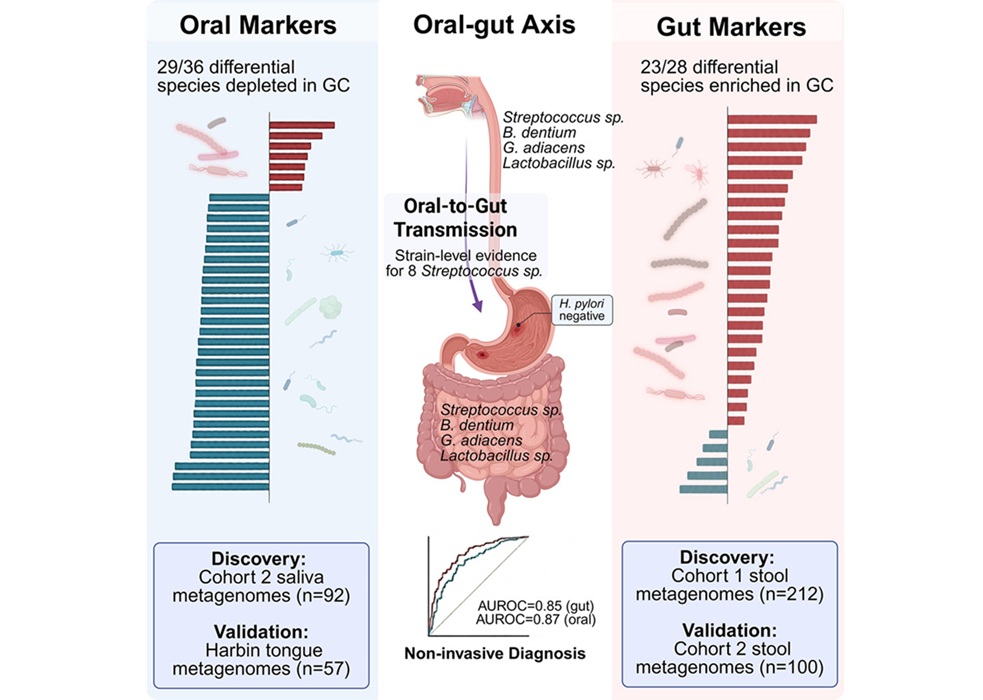
Oral–Gut Microbiome Signatures Identify Early Gastric Cancer
Early detection of gastric cancer could be advanced by scalable screening strategies using minimally invasive sampling. Saliva collection is noninvasive and cost-effective, supporting wider adoption... Read morePathology
view channel
FDA Clears AI Digital Pathology Tool for Breast Cancer Risk Stratification
Risk assessment at diagnosis is central to guiding therapy for early-stage, hormone receptor-positive, human epidermal growth factor receptor 2-negative (HR+/HER2-) invasive breast cancer, where overtreatment... Read more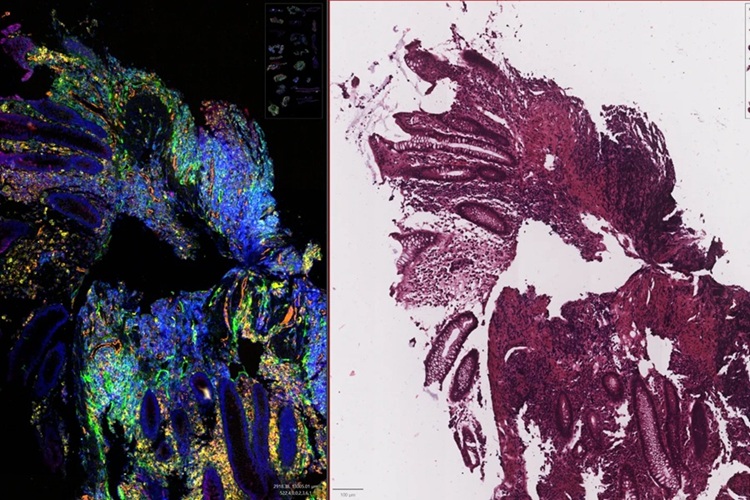
New AI Tool Reveals Hidden Genetic Signals in Routine H&E Slides
Pathologists worldwide rely on hematoxylin and eosin (H&E) slides to examine tissue architecture, yet these stains do not reveal the underlying molecular activity that often drives disease.... Read moreTechnology
view channel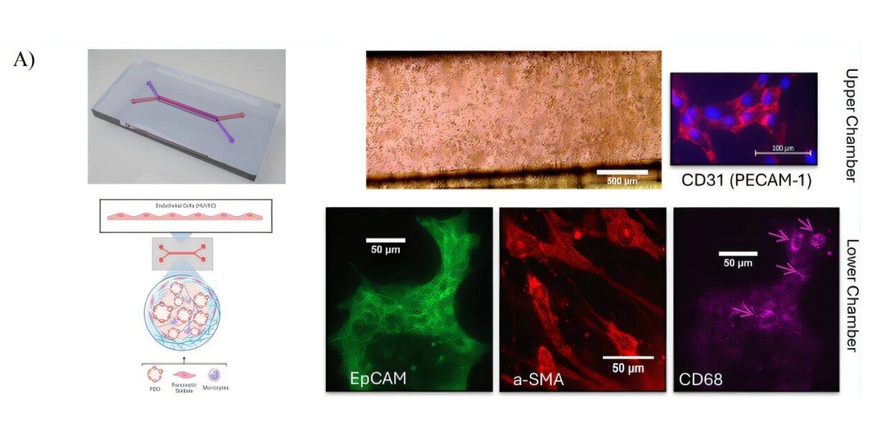
Tumor-on-a-Chip Platform Models Pancreatic Cancer Treatment Response
Pancreatic cancer remains one of the hardest malignancies to treat because tumors are embedded within a dense microenvironment that shapes growth and therapy response. Standard laboratory models often... Read more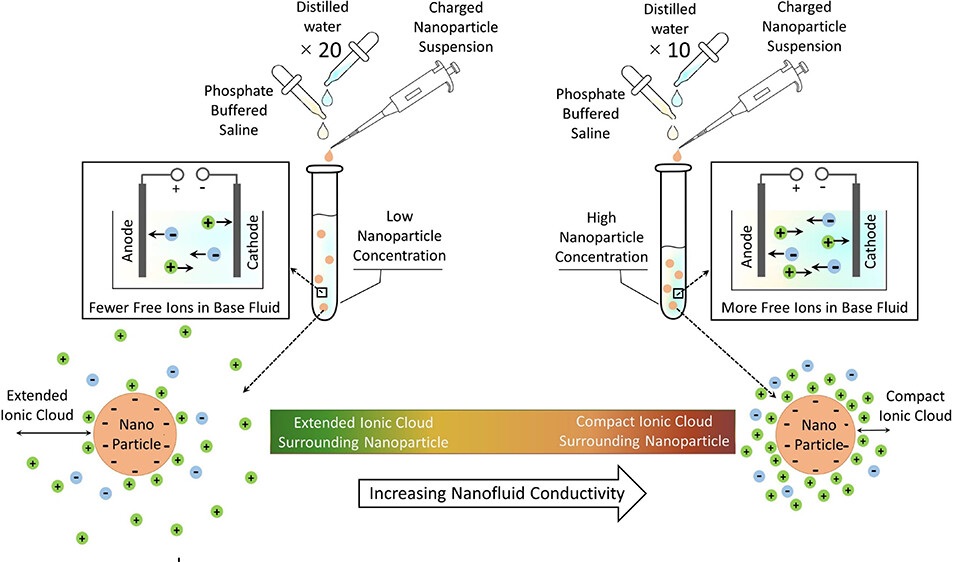
New Platform Captures Extracellular Vesicles for Early Cancer Detection
Early diagnosis remains the most effective way to reduce cancer mortality, yet many screening tools miss disease at its earliest stages. Biomarkers shed by tumors into blood and other fluids can be scarce... Read moreIndustry
view channel
Roche to Acquire PathAI for Up to $1.05 Billion to Strengthen AI Diagnostics Portfolio
Roche has entered into a definitive merger agreement to acquire PathAI, a company focused on digital pathology and artificial intelligence for pathology laboratories and the biopharma industry.... Read more