Graphene-Based Sensor Helps Predict Asthma Attacks
|
By LabMedica International staff writers Posted on 05 Jun 2017 |
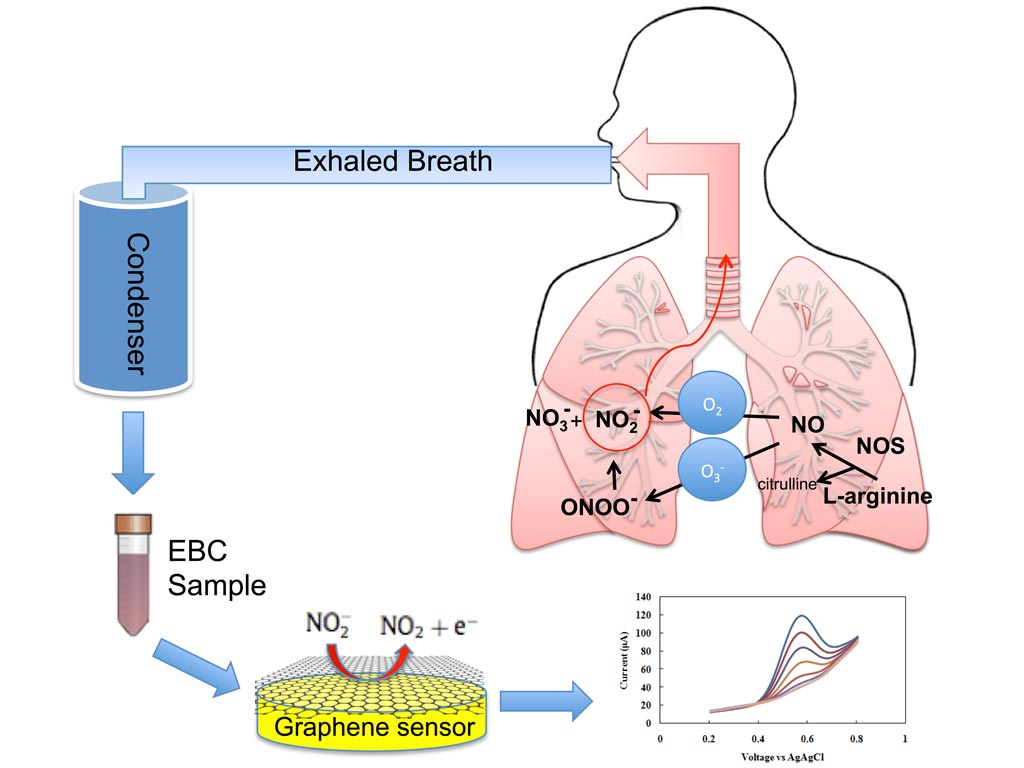
Image: Exhaled breath condensate is rapidly analyzed by a new graphene-based nanoelectronic sensor that detects nitrite, a key inflammatory marker in the inner lining of the respiratory airway (Photo courtesy of Azam Gholizadeh, Rutgers University).
Researchers have developed a prototype graphene-based device that detects inflammation in lungs, which could lead to earlier detection of asthma attacks and improve the management of asthma and other respiratory diseases, preventing hospitalizations and deaths. The invention helps pave the way for developing small wearable devices that could indicate when and at what dosage to take medication.
A diverse team of experts at Rutgers University-New Brunswick (New Brunswick, NJ, USA) created the sensor in response to the need for improved, minimally invasive methods for the molecular diagnosis and monitoring of asthma. Today’s non-invasive methods are limited in characterizing the nature and degree of airway inflammation, and require costly, bulky equipment that patients cannot easily keep with them. The methods include spirometry, which measures breathing capacity, and testing for exhaled nitric oxide, an indicator of airway inflammation.
Asthma causes inflammation of the airway and obstructs airflow. Other serious lung ailments include chronic obstructive pulmonary disease (COPD), which encompasses emphysema and chronic bronchitis.
“Our vision is to develop a device that someone with asthma or another respiratory disease can wear around their neck or on their wrist and blow into it periodically to predict the onset of an asthma attack or other problems,” said Mehdi Javanmard, assistant professor at Rutgers, “It advances the field of personalized and precision medicine.” Measuring biomarkers in exhaled breath condensate (tiny liquid droplets discharged during breathing) can also contribute to understanding asthma at the molecular level and lead to targeted treatment and better disease management.
Graphene is a thin layer of the graphite used in pencils. The new miniaturized electrochemical sensor accurately measures nitrite in exhaled breath condensate using reduced graphene oxide, which resists corrosion, has superior electrical properties, and is very accurate in detecting biomarkers.
“Nitrite level in breath condensate is a promising biomarker for inflammation in the respiratory tract. Having a rapid, easy method to measure it can help an asthmatic determine if air pollutants are affecting them so they can better manage use of medication and physical activity,” said Clifford Weisel, study co-author and professor at Rutgers, “It could also be used in a physician’s office and emergency departments to monitor the effectiveness of various anti-inflammatory drugs to optimize treatment.”
“Increases in airway inflammation may be an early warning sign of increased risk of an asthma attack or exacerbation of COPD, allowing for earlier and more-effective preventive measures or treatment,” said Robert Laumbach, study co-author and an occupational and environmental medicine physician at Rutgers.
“Just looking at coughing, wheezing, and other outward symptoms, diagnosis accuracy is often poor,” said Prof. Javanmard, “The ability to perform label-free quantification of nitrite content in exhaled breath condensate in a single step without any sample pre-treatment resolves a key bottleneck to enabling portable asthma management.” The next step is to develop a portable, wearable system. The researchers also envision expanding the number of inflammation biomarkers a device could detect and measure.
The study, by Gholizadeh A et al, was published May 22, 2017, in the journal Microsystems & Nanoengineering.
Related Links
Rutgers University-New Brunswick
A diverse team of experts at Rutgers University-New Brunswick (New Brunswick, NJ, USA) created the sensor in response to the need for improved, minimally invasive methods for the molecular diagnosis and monitoring of asthma. Today’s non-invasive methods are limited in characterizing the nature and degree of airway inflammation, and require costly, bulky equipment that patients cannot easily keep with them. The methods include spirometry, which measures breathing capacity, and testing for exhaled nitric oxide, an indicator of airway inflammation.
Asthma causes inflammation of the airway and obstructs airflow. Other serious lung ailments include chronic obstructive pulmonary disease (COPD), which encompasses emphysema and chronic bronchitis.
“Our vision is to develop a device that someone with asthma or another respiratory disease can wear around their neck or on their wrist and blow into it periodically to predict the onset of an asthma attack or other problems,” said Mehdi Javanmard, assistant professor at Rutgers, “It advances the field of personalized and precision medicine.” Measuring biomarkers in exhaled breath condensate (tiny liquid droplets discharged during breathing) can also contribute to understanding asthma at the molecular level and lead to targeted treatment and better disease management.
Graphene is a thin layer of the graphite used in pencils. The new miniaturized electrochemical sensor accurately measures nitrite in exhaled breath condensate using reduced graphene oxide, which resists corrosion, has superior electrical properties, and is very accurate in detecting biomarkers.
“Nitrite level in breath condensate is a promising biomarker for inflammation in the respiratory tract. Having a rapid, easy method to measure it can help an asthmatic determine if air pollutants are affecting them so they can better manage use of medication and physical activity,” said Clifford Weisel, study co-author and professor at Rutgers, “It could also be used in a physician’s office and emergency departments to monitor the effectiveness of various anti-inflammatory drugs to optimize treatment.”
“Increases in airway inflammation may be an early warning sign of increased risk of an asthma attack or exacerbation of COPD, allowing for earlier and more-effective preventive measures or treatment,” said Robert Laumbach, study co-author and an occupational and environmental medicine physician at Rutgers.
“Just looking at coughing, wheezing, and other outward symptoms, diagnosis accuracy is often poor,” said Prof. Javanmard, “The ability to perform label-free quantification of nitrite content in exhaled breath condensate in a single step without any sample pre-treatment resolves a key bottleneck to enabling portable asthma management.” The next step is to develop a portable, wearable system. The researchers also envision expanding the number of inflammation biomarkers a device could detect and measure.
The study, by Gholizadeh A et al, was published May 22, 2017, in the journal Microsystems & Nanoengineering.
Related Links
Rutgers University-New Brunswick
Latest Immunology News
- Aptamer-Based Biosensor Enables Mutation-Resilient SARS-CoV-2 Detection
- Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
- Study Points to Autoimmune Pathway Behind Long COVID Symptoms
- Immune Enzyme Linked to Treatment-Resistant Inflammatory Bowel Disease
- Simple Blood Test Could Replace Biopsies for Lung Transplant Rejection Monitoring
- Routine TB Screening Test May Reveal Immune Aging and Mortality Risk
- Biomarkers and Molecular Testing Advance Precision Allergy Care
- Point-of-Care Tests Could Expand Access to Mpox Diagnosis
- T-Cell Senescence Profiling May Predict CAR T Responses
- Finger-Prick Lateral Flow Test Detects Sepsis Biomarkers at Point of Care
- Study Highlights Low Sensitivity of Current Lyme Tests in Early Infection
- Immune Aging Clock Quantifies Immunosenescence and Identifies Therapeutic Target
- Study Finds Influenza Often Undiagnosed in Winter Deaths
- Combined Screening Approach Identifies Early Leprosy Cases
- Antibody Blood Test Identifies Active TB and Distinguishes Latent Infection
- FDA Approval Expands Use of PD-L1 Companion Diagnostic in Esophageal and GEJ Carcinomas
Channels
Clinical Chemistry
view channel
Saliva-Based Test Detects Biochemical Signs of Sleep Loss
Acute sleep loss impairs cognition and motor skills, raising safety risks that resemble alcohol intoxication. Clinicians currently lack an objective biochemical test to determine when someone is dangerously... Read more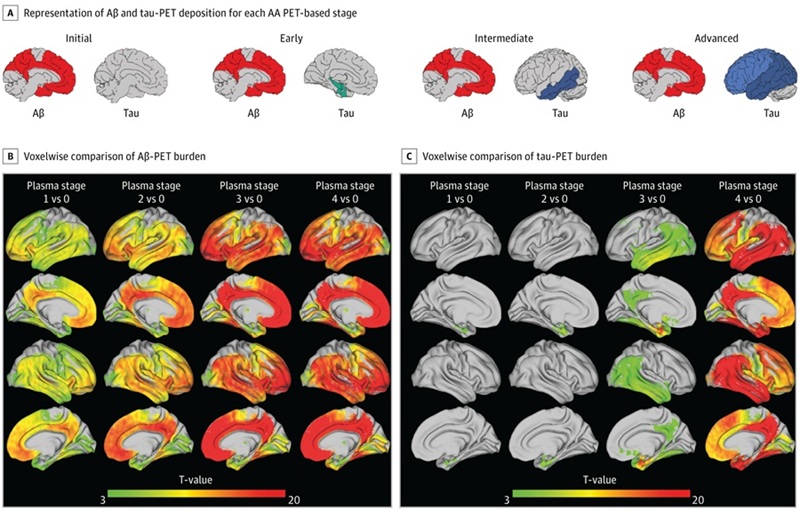
Simple Dual-Tau Blood Test Detects and Stages Alzheimer’s Disease
Alzheimer’s disease is typically confirmed and staged with positron emission tomography scans and cerebrospinal fluid testing, procedures that are costly and invasive. Broader access to minimally invasive... Read more
Alzheimer’s Blood Biomarkers Linked to Early Cognitive Differences Before Dementia
Blood-based screening for Alzheimer’s disease offers a noninvasive, lower-cost alternative to brain imaging or spinal fluid testing, yet its ability to flag the earliest cognitive changes has been unclear.... Read moreMolecular Diagnostics
view channel
New PCR Assay Supports Bundibugyo Ebola Outbreak Surveillance
Rapid identification of Ebola infections is essential to limit transmission and guide public health response, yet detection can be difficult when outbreaks involve rare variants. The current outbreaks... Read more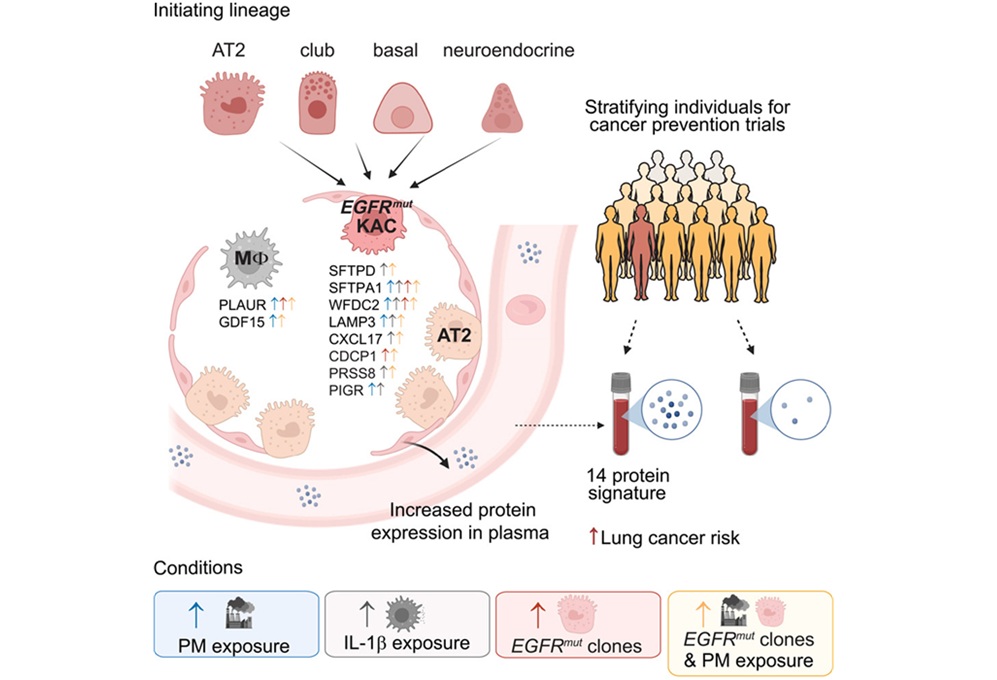
Plasma Protein Signature Predicts Lung Cancer Risk Up to Five Years Ahead
Lung cancer remains a leading cause of cancer death, and many cases are detected only after symptoms appear. Current screening programs largely target people with a history of smoking, leaving other at-risk... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channelAptamer-Based Biosensor Enables Mutation-Resilient SARS-CoV-2 Detection
Rapid evolution of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can undermine existing molecular diagnostics, especially when assays target small viral components. Double-antibody sandwich... Read more
Study Points to Autoimmune Pathway Behind Long COVID Symptoms
Long COVID leaves many SARS-CoV-2 survivors with persistent fatigue, cognitive issues, palpitations, and musculoskeletal pain for months or years. Estimates cited in new research suggest 4%–20% of infected... Read more
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read moreMicrobiology
view channel
New Culture Medium Speeds C. difficile Resistance Detection and Reduces Costs
Clostridioides difficile infections remain a persistent threat in hospitals and communities, affecting about 500,000 people in the United States each year. Severe cases can be fatal within 30 days of diagnosis,... Read more
Automated Blood Culture System Speeds Detection of Bloodstream Infections
Bloodstream infections and sepsis require rapid laboratory detection to guide targeted antimicrobial therapy and reduce mortality. Conventional blood culture workflows can delay actionable results by critical... Read morePathology
view channel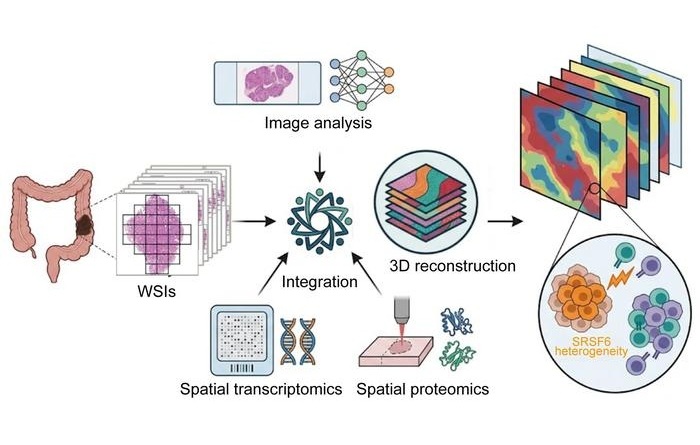
3D Spatial Multi-Omics Maps Intra-Tumor Diversity in Colorectal Cancer
Colorectal cancer remains a leading cause of cancer death, and clinical decision-making is complicated by marked intra-tumor heterogeneity. Conventional bulk sequencing averages molecular signals across... Read more
Blood-Based Method Tracks Gene Activity in the Living Brain
Real-time measurement of gene activity in the brain has been limited by assays requiring destructive tissue sampling. Tracking active genes could reveal how the body responds to environmental factors,... Read moreIndustry
view channel
Collaboration Advances ctDNA-Guided Development in Metastatic Colorectal Cancer
Natera, Inc. (Austin, TX, USA) and CytoDyn Inc. (Vancouver, WA, USA) announced a strategic collaboration focused on metastatic colorectal cancer (mCRC). Under the agreement, Natera will evaluate circulating... Read more