Genetic Background and Clinicopathologic Features Established for Adult-Onset Nephronophthisis
|
By LabMedica International staff writers Posted on 06 May 2021 |

Image: The Hamamatsu Photonics Nanozoomer 1 Digital Slide Scanner (Photo courtesy of University of Adelaide)
Nephronophthisis (NPH) is a genetic disorder of the kidneys which mainly affects children. It is classified as a medullary cystic kidney disease. The disorder is inherited in an autosomal recessive fashion and, although rare, is the most common genetic cause of childhood kidney failure.
Even in adult patients, accurate diagnosis of NPH is important because management options, such as kidney transplantation and appropriate genetic counseling, are available. The clinical diagnosis of adult NPH is problematic because clinical, radiologic and histologic features are non-specific. Even the extrarenal features are fewer in adults. Because management includes renal transplantation and genetic counseling, an accurate early diagnosis is essential.
Nephrologists at the Tokyo Medical and Dental University (Tokyo, Japan) investigated 18 adult patients who were suspected to have NPH by renal biopsy. The patients were recruited at 16 institutions in Japan between 2015 and 2019. For each patient, the tissue slides that were stained with hematoxylin-eosin, periodic acid-Schiff, and periodic acid–methenamine silver were digitized using the NanoZoomer HT Scan system (Hamamatsu Photonics, Hamamatsu, Japan).
Comprehensive genetic testing was performed using capture-based next-generation sequencing of 69 genes that cause nine types of hereditary cystic kidney disease, including NPH, NPH-related ciliopathies (Joubert syndrome, Meckel syndrome, Senior-Løken syndrome, Bardet-Biedl syndrome, and skeletal ciliopathies), autosomal dominant polycystic kidney disease, autosomal recessive polycystic kidney disease, and autosomal dominant tubulointerstitial kidney disease.
The scientists performed polymerase chain reaction for exons 1, 10, and 20 of NPHP1, if homozygous entire deletion of NPHP1 was detected by copy number variation analysis. To investigate what the essence of thick tubular basement membrane (TBM) duplication was, they performed low-vacuum scanning electron microscopic (Hitachi, Tokyo, Japan) analysis and immunofluorescence (IF) analysis in the representative cases with or without pathogenic mutations.
The investigators reported that seven of 18 patients had pathogenic NPH-causing mutations in NPHP1, NPHP3, NPHP4, or CEP164. Compared with patients without pathogenic mutations, those with pathogenic mutations were significantly younger, but did not significantly differ in the classic NPH pathologic findings, such as tubular cysts. On the other hand, the number of tubules with thick TBM duplication, which was defined as >10-μm thickness, was significantly higher in patients with genetically proven adult NPH than in those without pathogenic mutations. α-Smooth muscle actin (α-SMA)-positive myofibroblasts were detected inside thick TBM duplication.
The authors concluded that in adult patients with NPH, thick TBM duplication was the specific finding. Their analysis also suggested that older patients tended to have no pathogenic mutations, even when they were suspected to have NPH by renal biopsy. These findings could be the novel clinical clue for the diagnosis of NPH in adult patients. The study was published originally on March 3, 2021 in the journal Kidney International Reports.
Related Links:
Tokyo Medical and Dental University
Hamamatsu Photonics
Hitachi
Even in adult patients, accurate diagnosis of NPH is important because management options, such as kidney transplantation and appropriate genetic counseling, are available. The clinical diagnosis of adult NPH is problematic because clinical, radiologic and histologic features are non-specific. Even the extrarenal features are fewer in adults. Because management includes renal transplantation and genetic counseling, an accurate early diagnosis is essential.
Nephrologists at the Tokyo Medical and Dental University (Tokyo, Japan) investigated 18 adult patients who were suspected to have NPH by renal biopsy. The patients were recruited at 16 institutions in Japan between 2015 and 2019. For each patient, the tissue slides that were stained with hematoxylin-eosin, periodic acid-Schiff, and periodic acid–methenamine silver were digitized using the NanoZoomer HT Scan system (Hamamatsu Photonics, Hamamatsu, Japan).
Comprehensive genetic testing was performed using capture-based next-generation sequencing of 69 genes that cause nine types of hereditary cystic kidney disease, including NPH, NPH-related ciliopathies (Joubert syndrome, Meckel syndrome, Senior-Løken syndrome, Bardet-Biedl syndrome, and skeletal ciliopathies), autosomal dominant polycystic kidney disease, autosomal recessive polycystic kidney disease, and autosomal dominant tubulointerstitial kidney disease.
The scientists performed polymerase chain reaction for exons 1, 10, and 20 of NPHP1, if homozygous entire deletion of NPHP1 was detected by copy number variation analysis. To investigate what the essence of thick tubular basement membrane (TBM) duplication was, they performed low-vacuum scanning electron microscopic (Hitachi, Tokyo, Japan) analysis and immunofluorescence (IF) analysis in the representative cases with or without pathogenic mutations.
The investigators reported that seven of 18 patients had pathogenic NPH-causing mutations in NPHP1, NPHP3, NPHP4, or CEP164. Compared with patients without pathogenic mutations, those with pathogenic mutations were significantly younger, but did not significantly differ in the classic NPH pathologic findings, such as tubular cysts. On the other hand, the number of tubules with thick TBM duplication, which was defined as >10-μm thickness, was significantly higher in patients with genetically proven adult NPH than in those without pathogenic mutations. α-Smooth muscle actin (α-SMA)-positive myofibroblasts were detected inside thick TBM duplication.
The authors concluded that in adult patients with NPH, thick TBM duplication was the specific finding. Their analysis also suggested that older patients tended to have no pathogenic mutations, even when they were suspected to have NPH by renal biopsy. These findings could be the novel clinical clue for the diagnosis of NPH in adult patients. The study was published originally on March 3, 2021 in the journal Kidney International Reports.
Related Links:
Tokyo Medical and Dental University
Hamamatsu Photonics
Hitachi
Latest Pathology News
- Hyperspectral Dark-Field Microscopy Enables Rapid and Accurate Identification of Cancerous Tissues
- AI Advancements Enable Leap into 3D Pathology
- New Blood Test Device Modeled on Leeches to Help Diagnose Malaria
- Robotic Blood Drawing Device to Revolutionize Sample Collection for Diagnostic Testing
- Use of DICOM Images for Pathology Diagnostics Marks Significant Step towards Standardization
- First of Its Kind Universal Tool to Revolutionize Sample Collection for Diagnostic Tests
- AI-Powered Digital Imaging System to Revolutionize Cancer Diagnosis
- New Mycobacterium Tuberculosis Panel to Support Real-Time Surveillance and Combat Antimicrobial Resistance
- New Method Offers Sustainable Approach to Universal Metabolic Cancer Diagnosis
- Spatial Tissue Analysis Identifies Patterns Associated With Ovarian Cancer Relapse
- Unique Hand-Warming Technology Supports High-Quality Fingertip Blood Sample Collection
- Image-Based AI Shows Promise for Parasite Detection in Digitized Stool Samples
- Deep Learning Powered AI Algorithms Improve Skin Cancer Diagnostic Accuracy
- Microfluidic Device for Cancer Detection Precisely Separates Tumor Entities
- Virtual Skin Biopsy Determines Presence of Cancerous Cells
- AI Detects Viable Tumor Cells for Accurate Bone Cancer Prognoses Post Chemotherapy
Channels
Clinical Chemistry
view channel
3D Printed Point-Of-Care Mass Spectrometer Outperforms State-Of-The-Art Models
Mass spectrometry is a precise technique for identifying the chemical components of a sample and has significant potential for monitoring chronic illness health states, such as measuring hormone levels... Read more.jpg)
POC Biomedical Test Spins Water Droplet Using Sound Waves for Cancer Detection
Exosomes, tiny cellular bioparticles carrying a specific set of proteins, lipids, and genetic materials, play a crucial role in cell communication and hold promise for non-invasive diagnostics.... Read more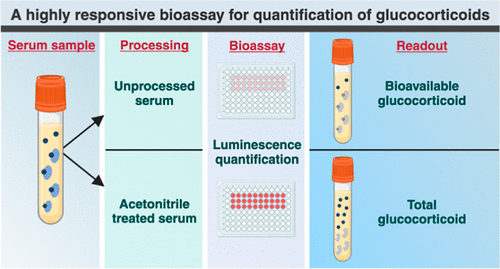
Highly Reliable Cell-Based Assay Enables Accurate Diagnosis of Endocrine Diseases
The conventional methods for measuring free cortisol, the body's stress hormone, from blood or saliva are quite demanding and require sample processing. The most common method, therefore, involves collecting... Read moreMolecular Diagnostics
view channel.jpg)
New Respiratory Syndromic Testing Panel Provides Fast and Accurate Results
Respiratory tract infections are a major reason for emergency department visits and hospitalizations. According to the CDC, the U.S. sees up to 41 million influenza cases annually, resulting in several... Read more
New Synthetic Biomarker Technology Differentiates Between Prior Zika and Dengue Infections
Until now, researchers and clinicians have lacked diagnostic tools to easily differentiate between past infections with different flaviviruses—a family of mostly mosquito- and tick-borne viruses that include... Read moreHematology
view channel
Next Generation Instrument Screens for Hemoglobin Disorders in Newborns
Hemoglobinopathies, the most widespread inherited conditions globally, affect about 7% of the population as carriers, with 2.7% of newborns being born with these conditions. The spectrum of clinical manifestations... Read more
First 4-in-1 Nucleic Acid Test for Arbovirus Screening to Reduce Risk of Transfusion-Transmitted Infections
Arboviruses represent an emerging global health threat, exacerbated by climate change and increased international travel that is facilitating their spread across new regions. Chikungunya, dengue, West... Read more
POC Finger-Prick Blood Test Determines Risk of Neutropenic Sepsis in Patients Undergoing Chemotherapy
Neutropenia, a decrease in neutrophils (a type of white blood cell crucial for fighting infections), is a frequent side effect of certain cancer treatments. This condition elevates the risk of infections,... Read more
First Affordable and Rapid Test for Beta Thalassemia Demonstrates 99% Diagnostic Accuracy
Hemoglobin disorders rank as some of the most prevalent monogenic diseases globally. Among various hemoglobin disorders, beta thalassemia, a hereditary blood disorder, affects about 1.5% of the world's... Read moreImmunology
view channel
Diagnostic Blood Test for Cellular Rejection after Organ Transplant Could Replace Surgical Biopsies
Transplanted organs constantly face the risk of being rejected by the recipient's immune system which differentiates self from non-self using T cells and B cells. T cells are commonly associated with acute... Read more
AI Tool Precisely Matches Cancer Drugs to Patients Using Information from Each Tumor Cell
Current strategies for matching cancer patients with specific treatments often depend on bulk sequencing of tumor DNA and RNA, which provides an average profile from all cells within a tumor sample.... Read more
Genetic Testing Combined With Personalized Drug Screening On Tumor Samples to Revolutionize Cancer Treatment
Cancer treatment typically adheres to a standard of care—established, statistically validated regimens that are effective for the majority of patients. However, the disease’s inherent variability means... Read moreMicrobiology
view channel
Integrated Solution Ushers New Era of Automated Tuberculosis Testing
Tuberculosis (TB) is responsible for 1.3 million deaths every year, positioning it as one of the top killers globally due to a single infectious agent. In 2022, around 10.6 million people were diagnosed... Read more
Automated Sepsis Test System Enables Rapid Diagnosis for Patients with Severe Bloodstream Infections
Sepsis affects up to 50 million people globally each year, with bacteraemia, formerly known as blood poisoning, being a major cause. In the United States alone, approximately two million individuals are... Read moreEnhanced Rapid Syndromic Molecular Diagnostic Solution Detects Broad Range of Infectious Diseases
GenMark Diagnostics (Carlsbad, CA, USA), a member of the Roche Group (Basel, Switzerland), has rebranded its ePlex® system as the cobas eplex system. This rebranding under the globally renowned cobas name... Read more
Clinical Decision Support Software a Game-Changer in Antimicrobial Resistance Battle
Antimicrobial resistance (AMR) is a serious global public health concern that claims millions of lives every year. It primarily results from the inappropriate and excessive use of antibiotics, which reduces... Read moreTechnology
view channel
New Diagnostic System Achieves PCR Testing Accuracy
While PCR tests are the gold standard of accuracy for virology testing, they come with limitations such as complexity, the need for skilled lab operators, and longer result times. They also require complex... Read more
DNA Biosensor Enables Early Diagnosis of Cervical Cancer
Molybdenum disulfide (MoS2), recognized for its potential to form two-dimensional nanosheets like graphene, is a material that's increasingly catching the eye of the scientific community.... Read more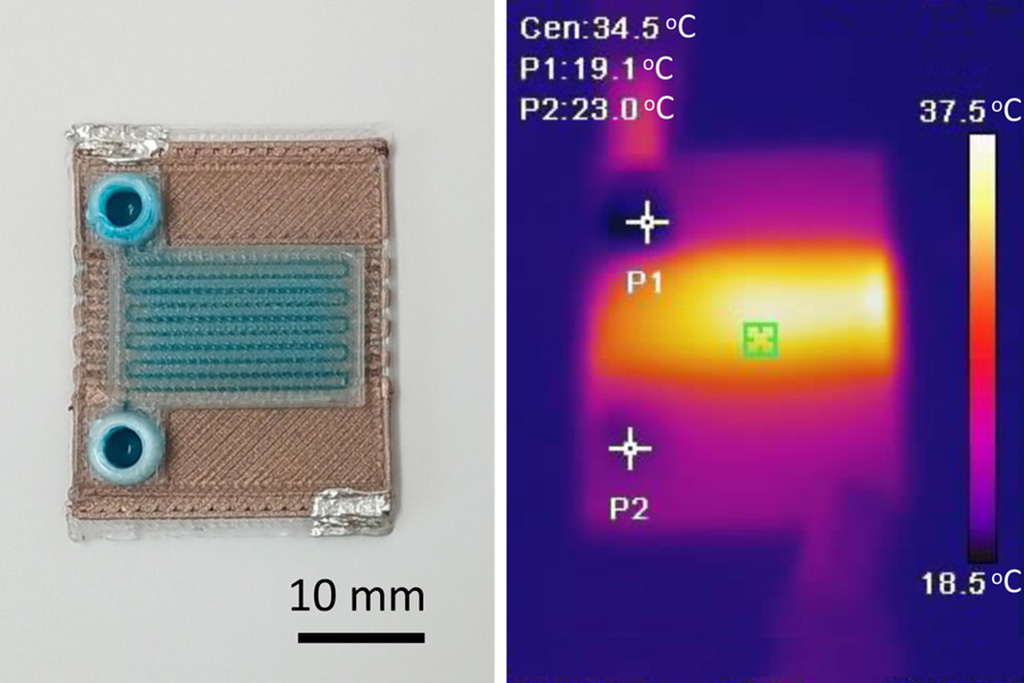
Self-Heating Microfluidic Devices Can Detect Diseases in Tiny Blood or Fluid Samples
Microfluidics, which are miniature devices that control the flow of liquids and facilitate chemical reactions, play a key role in disease detection from small samples of blood or other fluids.... Read more
Breakthrough in Diagnostic Technology Could Make On-The-Spot Testing Widely Accessible
Home testing gained significant importance during the COVID-19 pandemic, yet the availability of rapid tests is limited, and most of them can only drive one liquid across the strip, leading to continued... Read moreIndustry
view channel
Danaher and Johns Hopkins University Collaborate to Improve Neurological Diagnosis
Unlike severe traumatic brain injury (TBI), mild TBI often does not show clear correlations with abnormalities detected through head computed tomography (CT) scans. Consequently, there is a pressing need... Read more
Beckman Coulter and MeMed Expand Host Immune Response Diagnostics Partnership
Beckman Coulter Diagnostics (Brea, CA, USA) and MeMed BV (Haifa, Israel) have expanded their host immune response diagnostics partnership. Beckman Coulter is now an authorized distributor of the MeMed... Read more_1.jpg)