Establishment of Biomarker Panel May Lead to Rapid Tests for Early Diagnosis of Pancreatic Cancer
|
By LabMedica International staff writers Posted on 10 Apr 2016 |
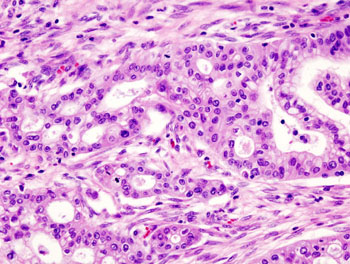
Image: Micrograph of pancreatic ductal adenocarcinoma (the most common type of pancreatic cancer) (Photo courtesy of Wikimedia Commons).
A panel comprising five genetic biomarkers was shown to accurately differentiate among tissues from pancreatic tumors and those taken from various non-malignant sources.
Investigators at Beth Israel Deaconess Medical Center (Boston, MA, USA) applied innovative data normalization and gene selection approaches to analyze a number of publicly available pancreatic cancer gene expression datasets. They combined the statistical power of multiple genomic studies while masking their variability and batch effects to identify robust early diagnostic biomarkers of pancreatic cancer.
The investigators established a panel comprising the genes TMPRSS4 (Transmembrane protease, serine 4), AHNAK2 (AHNAK nucleoprotein 2), POSTN (Periostin), ECT2 (Epithelial cell transforming 2), and SERPINB5 (Serpin peptidase inhibitor, clade B (ovalbumin), member 5) that achieved on average 95% sensitivity and 89% specificity in discriminating pancreatic ductal adenocarcinoma (PDAC) from non-tumor samples in four training sets and similar performance in five independent validation datasets. The five-gene classifier accurately discriminated PDAC from chronic pancreatitis, other cancers, and non-tumor samples from PDAC precursors in three independent datasets.
PDAC-specific expression of the biomarker panel was measured by qRT-PCR (qualitative real-time PCR) in microdissected patient-derived FFPE (formalin-fixed, paraffin-embedded) tissues. Cell-based assays were then used to assess the impact of two of the biomarkers, TMPRSS4 and ECT2, on PDAC cells.
Results revealed that knock-down of TMPRSS4 and ECT2 reduced PDAC soft agar growth and cell viability, and TMPRSS4 knockdown also blocked PDAC migration and invasion.
“Pancreatic cancer is a devastating disease with a death rate close to the incidence rate,” said senior author Dr. Towia Libermann, professor of medicine at Beth Israel Deaconess Medical Center. “Because more than 90% of pancreatic cancer cases are diagnosed at the metastatic stage, when there are only limited therapeutic options, earlier diagnosis is anticipated to have a major impact on extending life expectancy for patients. There has been a lack of reliable markers, early indicators, and risk factors associated with pancreatic cancer, but this new way of differentiating between healthy and malignant tissue offers hope for earlier diagnosis and treatment.”
“Because these five genes are turned on so early in the development of pancreatic cancer, they may play roles as drivers of this disease and may be exciting targets for therapies,” said Dr. Libermann. “Moving forward, we will explore the potential to convert this tissue-based diagnostic into a noninvasive blood or urine test.”
The study was published in the March 16, 2016, online edition of the journal Oncotarget.
Related Links:
Beth Israel Deaconess Medical Center
Investigators at Beth Israel Deaconess Medical Center (Boston, MA, USA) applied innovative data normalization and gene selection approaches to analyze a number of publicly available pancreatic cancer gene expression datasets. They combined the statistical power of multiple genomic studies while masking their variability and batch effects to identify robust early diagnostic biomarkers of pancreatic cancer.
The investigators established a panel comprising the genes TMPRSS4 (Transmembrane protease, serine 4), AHNAK2 (AHNAK nucleoprotein 2), POSTN (Periostin), ECT2 (Epithelial cell transforming 2), and SERPINB5 (Serpin peptidase inhibitor, clade B (ovalbumin), member 5) that achieved on average 95% sensitivity and 89% specificity in discriminating pancreatic ductal adenocarcinoma (PDAC) from non-tumor samples in four training sets and similar performance in five independent validation datasets. The five-gene classifier accurately discriminated PDAC from chronic pancreatitis, other cancers, and non-tumor samples from PDAC precursors in three independent datasets.
PDAC-specific expression of the biomarker panel was measured by qRT-PCR (qualitative real-time PCR) in microdissected patient-derived FFPE (formalin-fixed, paraffin-embedded) tissues. Cell-based assays were then used to assess the impact of two of the biomarkers, TMPRSS4 and ECT2, on PDAC cells.
Results revealed that knock-down of TMPRSS4 and ECT2 reduced PDAC soft agar growth and cell viability, and TMPRSS4 knockdown also blocked PDAC migration and invasion.
“Pancreatic cancer is a devastating disease with a death rate close to the incidence rate,” said senior author Dr. Towia Libermann, professor of medicine at Beth Israel Deaconess Medical Center. “Because more than 90% of pancreatic cancer cases are diagnosed at the metastatic stage, when there are only limited therapeutic options, earlier diagnosis is anticipated to have a major impact on extending life expectancy for patients. There has been a lack of reliable markers, early indicators, and risk factors associated with pancreatic cancer, but this new way of differentiating between healthy and malignant tissue offers hope for earlier diagnosis and treatment.”
“Because these five genes are turned on so early in the development of pancreatic cancer, they may play roles as drivers of this disease and may be exciting targets for therapies,” said Dr. Libermann. “Moving forward, we will explore the potential to convert this tissue-based diagnostic into a noninvasive blood or urine test.”
The study was published in the March 16, 2016, online edition of the journal Oncotarget.
Related Links:
Beth Israel Deaconess Medical Center
Latest Pathology News
- Blood-Based Method Tracks Gene Activity in the Living Brain
- FDA Approval Expands Automated PD-L1 Testing Across Solid Tumors
- AI-Powered Atlas Maps Immune Structures Linked to Cancer Outcomes
- AI Tool Extracts Immune Signals from Biopsy to Inform Myeloma Therapy
- Rapid AI Tool Predicts Cancer Spatial Gene Expression from Pathology Images
- AI Pathology Test Receives FDA Breakthrough for Bladder Cancer Risk Stratification
- FDA Clears AI Digital Pathology Tool for Breast Cancer Risk Stratification
- New AI Tool Reveals Hidden Genetic Signals in Routine H&E Slides
- AI System Analyzes Routine Pathology Slides to Predict Cancer Outcomes
- New Tissue Mapping Approach Identifies High-Risk Form of Diabetic Kidney Disease
- Multimodal AI Tool Predicts Genetic Alterations to Guide Breast Cancer Treatment
- Interpretable AI Reveals Hidden Cellular Features from Microscopy Images
- Tumor Immune Structure Predicts Response to Immunotherapy in Melanoma
- Plug-and-Play AI Pathology System Classifies Multiple Cancers from Few Slides
- AI-Based Assays Support Risk Stratification in Prostate and Breast Cancer
- AI Pathology Model Predicts Immunotherapy Response in Lung Cancer
Channels
Clinical Chemistry
view channel
Saliva-Based Test Detects Biochemical Signs of Sleep Loss
Acute sleep loss impairs cognition and motor skills, raising safety risks that resemble alcohol intoxication. Clinicians currently lack an objective biochemical test to determine when someone is dangerously... Read more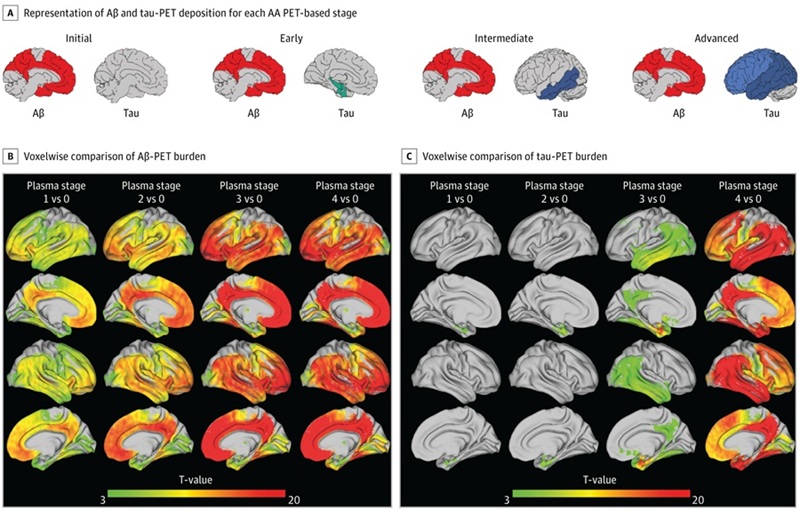
Simple Dual-Tau Blood Test Detects and Stages Alzheimer’s Disease
Alzheimer’s disease is typically confirmed and staged with positron emission tomography scans and cerebrospinal fluid testing, procedures that are costly and invasive. Broader access to minimally invasive... Read more
Alzheimer’s Blood Biomarkers Linked to Early Cognitive Differences Before Dementia
Blood-based screening for Alzheimer’s disease offers a noninvasive, lower-cost alternative to brain imaging or spinal fluid testing, yet its ability to flag the earliest cognitive changes has been unclear.... Read moreMolecular Diagnostics
view channel
Circulating Tumor DNA Testing Guides Chemotherapy, Reduces Relapse in Colon Cancer
Adjuvant therapy decisions after curative surgery for colon cancer remain difficult, as conventional clinicopathologic factors often fail to capture residual disease risk. Liquid biopsy approaches that... Read more
Researchers Uncover Distinct Chromosome Signature in Aggresive ALT Cancers
A subset of cancers rely on alternative lengthening of telomeres, a pathway associated with genomic instability and difficult-to-treat disease. These tumors span multiple cancer types and account for about... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channelAptamer-Based Biosensor Enables Mutation-Resilient SARS-CoV-2 Detection
Rapid evolution of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can undermine existing molecular diagnostics, especially when assays target small viral components. Double-antibody sandwich... Read more
Study Points to Autoimmune Pathway Behind Long COVID Symptoms
Long COVID leaves many SARS-CoV-2 survivors with persistent fatigue, cognitive issues, palpitations, and musculoskeletal pain for months or years. Estimates cited in new research suggest 4%–20% of infected... Read more
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read moreMicrobiology
view channel
Gut Microbiome Signatures Help Identify Risk of IBD Progression
Inflammatory bowel disease (IBD), encompassing Crohn’s disease and ulcerative colitis, is a chronic relapsing inflammatory disorder of the gastrointestinal tract with highly variable outcomes.... Read more
FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
Clinical guidelines support testing based on patient presentation in suspected gastrointestinal infections, yet available technologies have often forced laboratories to choose between panels that are too... Read moreTechnology
view channel
AI Platform Links Biomarker Results to Cancer Clinical Trials and Guidelines
Oncology teams must manage growing volumes of genomic data, rapidly evolving clinical trial options, and frequently updated care guidelines, all within tight clinic schedules. Translating complex tumor... Read more
Agentic AI Platform Supports Genomic Decision-Making in Oncology
Oncology care teams increasingly face the challenge of managing complex molecular diagnostics, evolving treatment options, and extensive electronic health record documentation. Translating multimodal data... Read moreIndustry
view channel