Blood Test Helps Determine Traumatic Brain Injury Severity
|
By LabMedica International staff writers Posted on 11 Aug 2015 |
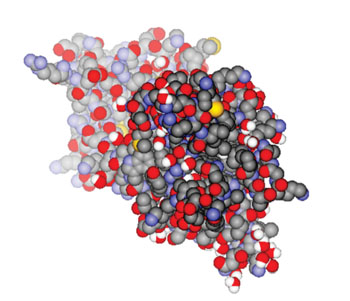
Image: Three-dimensional structure of the brain-derived neurotrophic factor protein (Photo courtesy of Microswitch/ Protein Data Bank).
A new blood test could help emergency room doctors quickly diagnose traumatic brain injury and determine its severity and the test could help identify patients who might benefit from extra therapy or novel treatments.
Brain derived neurotrophic factor (BDNF) is important for neuronal survival and regeneration the diagnostic and prognostic values of serum BDNF in traumatic brain injury (TBI) and its association with two other proteins has been investigated.
A large group of collaborating scientists led by those at Johns Hopkins University School of Medicine (Baltimore, MD, USA) examined serum BDNF in two independent cohorts of TBI cases presenting to the emergency departments. At Johns Hopkins Hospital, 76 patients were studied and at San Francisco General Hospital (CA, USA), 80 patient were included in the study and a control group of 150 patients without TBI were enrolled.
The teams investigated the association between BDNF, Glial fibrillary acidic protein (GFAP) and Ubiquitin C-terminal hydrolase -L1 (UCH-L1) and recovery from TBI at six months in a pilot cohort. The investigators found that the levels of BDNF, taken within 24 hours of someone's head injury, could predict the severity of a TBI and how a patient would fare. While healthy people averaged 60 ng/mL of BDNF in their bloodstreams, patients with brain injuries had less than one-third of that amount, averaging less than 20 ng/mL, and those with the most severe TBIs had even lower levels, around 4 ng/mL. Moreover, patients with high levels of BDNF had mostly recovered from their injuries six months later, but in patients with the lowest levels of BDNF, symptoms still lingered at follow-up. The results suggest that a test for BDNF levels, administered in the emergency room, could help stratify patients.
Frederick Korley, MD, PhD, an assistant professor of emergency medicine and first author of the study said, “Compared to other proteins that have been measured in traumatic brain injury, BDNF does a much better job of predicting outcomes. The advantage of being able to predict prognosis early on is that you can advise patients on what to do, recommend whether they need to take time off work or school, and decide whether they need to follow up with a rehab doctor or neurologist.” The study was published on July 10, 2015, in the Journal of Neurotrauma.
Related Links:
Johns Hopkins University School of Medicine
San Francisco General Hospital
Brain derived neurotrophic factor (BDNF) is important for neuronal survival and regeneration the diagnostic and prognostic values of serum BDNF in traumatic brain injury (TBI) and its association with two other proteins has been investigated.
A large group of collaborating scientists led by those at Johns Hopkins University School of Medicine (Baltimore, MD, USA) examined serum BDNF in two independent cohorts of TBI cases presenting to the emergency departments. At Johns Hopkins Hospital, 76 patients were studied and at San Francisco General Hospital (CA, USA), 80 patient were included in the study and a control group of 150 patients without TBI were enrolled.
The teams investigated the association between BDNF, Glial fibrillary acidic protein (GFAP) and Ubiquitin C-terminal hydrolase -L1 (UCH-L1) and recovery from TBI at six months in a pilot cohort. The investigators found that the levels of BDNF, taken within 24 hours of someone's head injury, could predict the severity of a TBI and how a patient would fare. While healthy people averaged 60 ng/mL of BDNF in their bloodstreams, patients with brain injuries had less than one-third of that amount, averaging less than 20 ng/mL, and those with the most severe TBIs had even lower levels, around 4 ng/mL. Moreover, patients with high levels of BDNF had mostly recovered from their injuries six months later, but in patients with the lowest levels of BDNF, symptoms still lingered at follow-up. The results suggest that a test for BDNF levels, administered in the emergency room, could help stratify patients.
Frederick Korley, MD, PhD, an assistant professor of emergency medicine and first author of the study said, “Compared to other proteins that have been measured in traumatic brain injury, BDNF does a much better job of predicting outcomes. The advantage of being able to predict prognosis early on is that you can advise patients on what to do, recommend whether they need to take time off work or school, and decide whether they need to follow up with a rehab doctor or neurologist.” The study was published on July 10, 2015, in the Journal of Neurotrauma.
Related Links:
Johns Hopkins University School of Medicine
San Francisco General Hospital
Latest Clinical Chem. News
- New CA19-9 Cutoff Value Helps Identify High-Risk Pancreatic Cancer Patients
- Blood-Based Biomarkers Show Promise for Psychosis Risk Prediction
- International Experts Recommend Ending Routine 'Corrected' Calcium Reporting
- Long-Term Data Show PSA Screening Modestly Reduces Prostate Cancer Deaths
- Urine-Based Nanosensor Tracks Lung Cancer and Fibrosis Noninvasively
- FDA-Cleared Assay Enables Comprehensive Automated Testosterone Testing
- CE-Marked Blood Biomarker Test Advances Automated Alzheimer’s Diagnostics
- Blood-Based Alzheimer’s Test Gains CE Mark for Amyloid Pathology Detection
- Noninvasive Urine Test May Support Earlier Diagnosis of Psychiatric Disorders
- At-Home Blood and Cognitive Tests Support Dementia Risk Stratification
- Ultrasensitive Test Detects Key Biomarker of Frontotemporal Dementia Subtype
- Routine Blood Tests Years Before Pregnancy Could Identify Preeclampsia Risk
- Blood Test Detects Testicular Cancer Missed by Standard Markers
- Routine Blood Tests Identify Biomarkers Linked to PTSD
- Proteomic Data Underscore Need for Age-Specific Pediatric Reference Ranges
- Routine Blood Count Ratio Linked to Future Alzheimer’s and Dementia Risk
Channels
Molecular Diagnostics
view channel
New RNA Origami Method Supports Faster Targeted Testing for Repeat Expansion Disorders
Repeat expansion disorders drive conditions such as myotonic dystrophy, Huntington’s disease, and amyotrophic lateral sclerosis (ALS), yet accurately sizing the mutated sequences remains difficult.... Read more
FDA Approves Expanded Liquid Biopsy Panel for Advanced Cancer Profiling
Timely, comprehensive tumor profiling helps clinicians make treatment selection decisions for patients with advanced cancer. Blood-based approaches can provide actionable insights from a simple draw and... Read moreHematology
view channel
Higher Ferritin Threshold May Improve Iron Deficiency Detection in Children
Iron deficiency in school-age children can affect brain development, learning, growth, and physical performance, yet early deficiency may be missed when screening focuses mainly on anemia.... Read more
Stem Cell Biomarkers May Guide Precision Treatment in Acute Myeloid Leukemia
Acute myeloid leukemia (AML) is an aggressive blood cancer that most often affects older adults and still carries a poor prognosis despite therapeutic advances. Venetoclax-based regimens have improved... Read moreImmunology
view channel
Immune Enzyme Linked to Treatment-Resistant Inflammatory Bowel Disease
Inflammatory bowel disease (IBD) affects nearly 3 million people in the United States and its prevalence continues to rise. Medications that target tumor necrosis factor (TNF)-alpha are widely used, but... Read more
Simple Blood Test Could Replace Biopsies for Lung Transplant Rejection Monitoring
Lung transplant recipients face some of the highest rates of acute cellular rejection, and routine surveillance often relies on repeated surgical biopsies. These procedures can cause complications such... Read moreMicrobiology
view channel
New AMR Assay Supports Rapid Infection Control Screening in Hospitals
As antimicrobial resistance spreads worldwide, healthcare-associated infections are placing a growing burden on hospitals, increasing the need for faster and broader diagnostic solutions.... Read more
Diagnostic Gaps Complicate Bundibugyo Ebola Outbreak Response in Congo
In eastern Democratic Republic of the Congo, communities are confronting a resurgence of Bundibugyo ebolavirus, a rarer species for which no vaccines or treatments have been approved. Ebola is a highly... Read more
Study Finds Hidden Mpox Infections May Drive Ongoing Spread
Mpox continues to circulate despite vaccination, and many cases show no known link to a symptomatic partner. The role of people without symptoms has remained uncertain, limiting clarity on how transmission persists.... Read more
Large-Scale Genomic Surveillance Tracks Resistant Bacteria Across European Hospitals
Antimicrobial resistance (AMR) poses a growing threat to patient safety, with carbapenem-resistant Enterobacterales causing difficult-to-treat infections and leaving clinicians with limited therapeutic options.... Read morePathology
view channel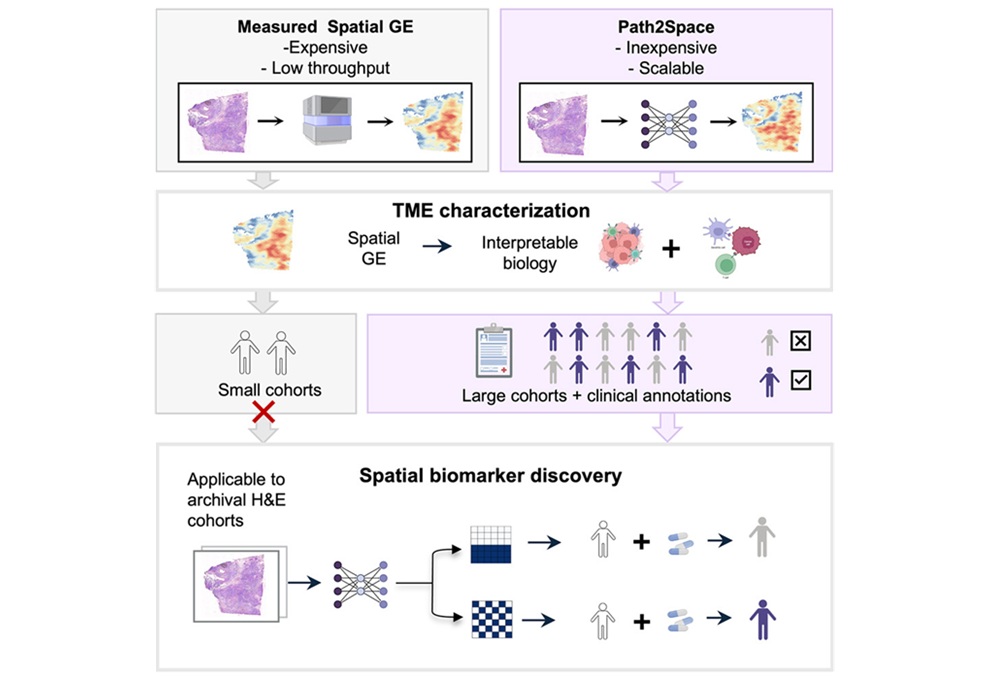
Rapid AI Tool Predicts Cancer Spatial Gene Expression from Pathology Images
Gene expression profiling can inform tumor biology and treatment selection, but spatial assays remain costly and time-consuming. Results can take weeks and cost thousands of dollars, limiting large-scale... Read more
AI Pathology Test Receives FDA Breakthrough for Bladder Cancer Risk Stratification
Non–muscle invasive bladder cancer has highly variable outcomes, complicating surveillance and treatment planning. Risk assessment typically relies on stage, grade, and tumor size, leaving uncertainty... Read moreTechnology
view channel
AI-Enabled Assistant Unifies Molecular Workflow Planning and Support
Clinical laboratories and research groups face increasingly complex molecular workflows and expanding technical documentation spread across multiple systems. Fragmented digital tools can slow experiment... Read more
AI Tool Automates Validation of Laboratory Software Configuration Changes
Regulated laboratories face heavy documentation and requalification demands when software configurations change, slowing improvements and discouraging beneficial updates. A new capability now automates... Read moreIndustry
view channel
Strategic Collaboration Advances RNA Foundation Models for Precision Oncology
Bulk RNA sequencing is increasingly used to study tumor biology, but standard analyses often reduce results to gene-level summaries that miss important transcript variants and mutation patterns.... Read more




.jpg)