Blood Test May Trump Standard for Early Down Syndrome Screening
|
By LabMedica International staff writers Posted on 14 Apr 2015 |
A new multicenter study provides landmark evidence that a blood test undertaken between 10 to 14 weeks of pregnancy may be more accurate in diagnosing Down syndrome (DS), and two less common chromosomal abnormalities, than standard noninvasive screening techniques.
The research team, led by first author Mary Norton, MD, professor of clinical obstetrics and gynecology at University of California San Francisco (UCSF; San Francisco, CA, USA), followed pregnancy outcomes in close to 16,000 women (average age 30, with approximately 25% over 35). The cell-free DNA (cfDNA) blood test resulted in correctly identifying all 38 fetuses with DS, confirmed by newborn exam, prenatal or postnatal genetic analysis. The test focuses on the small percentage of fetal DNA in a pregnant woman’s blood. DNA from the targeted genes is molecularly “photocopied” and amplified by PCR, products are sequenced, and comparisons are made between relative amounts of the chromosomal DNA.
With standard screening, only 30 of the 38 fetuses with DS were identified. The standard screening comprises a blood sample in which hormones and proteins associated with chromosomal defects are identified, together with an ultrasound of the nuchal fold fluid in the back of the neck, an excess of which is suggestive of DS.
A second compelling advantage of cfDNA analysis was the relatively low incidence of DS misdiagnoses. While standard testing is acknowledged to result in a large number of false-positives, these were significantly less likely with the cfDNA test, which resulted in 9 false-positives vs. 854 with standard screening.
While far fewer cases of trisomy 18 (Edwards syndrome) and trisomy 13 (Patau syndrome) were found in the study population, the accuracy of cfDNA screening still surpassed standard screening.
The researchers emphasized areas of caution. Standard screening “can identify risk for a broad array of abnormalities that are not detectable on cfDNA testing,” they said. Additionally, a surprisingly high number of aneuploidies were present in the 488 pregnant women whose blood samples were disqualified (due to inadequate or immeasurable quantity of fetal DNA, or assay failure, or high sequencing-variance that could lead to misinterpreting results). Had this disqualified cohort been included in the findings, detection rates of the cfDNA test would have been lower.
cfDNA tests will result in far fewer false-positives than current screening, and so can reduce the number of invasive tests and of miscarriages wrongly attributed to positives. However, patients should be made aware of its limitations. “Providers need to be attuned to patients’ preferences and counsel them about the differences in prenatal screening options. Women who opt for cfDNA testing should be informed that it is highly accurate for DS, but it focuses on a small number of chromosomal abnormalities and does not provide the comprehensive assessment available with other approaches,” said Prof. Norton, “Counseling should also include information about the risks associated with failed tests and the pros and cons of pursuing invasive testing if no results are obtained.”
The study, by Norton M et al., was published April 1, 2015, in the New England Journal of Medicine.
Related Links:
University of California San Francisco
Ariosa Diagnostics’s Harmony prenatal blood test for trisomy 21, 18, & 13
Perinatal Quality Foundation
The research team, led by first author Mary Norton, MD, professor of clinical obstetrics and gynecology at University of California San Francisco (UCSF; San Francisco, CA, USA), followed pregnancy outcomes in close to 16,000 women (average age 30, with approximately 25% over 35). The cell-free DNA (cfDNA) blood test resulted in correctly identifying all 38 fetuses with DS, confirmed by newborn exam, prenatal or postnatal genetic analysis. The test focuses on the small percentage of fetal DNA in a pregnant woman’s blood. DNA from the targeted genes is molecularly “photocopied” and amplified by PCR, products are sequenced, and comparisons are made between relative amounts of the chromosomal DNA.
With standard screening, only 30 of the 38 fetuses with DS were identified. The standard screening comprises a blood sample in which hormones and proteins associated with chromosomal defects are identified, together with an ultrasound of the nuchal fold fluid in the back of the neck, an excess of which is suggestive of DS.
A second compelling advantage of cfDNA analysis was the relatively low incidence of DS misdiagnoses. While standard testing is acknowledged to result in a large number of false-positives, these were significantly less likely with the cfDNA test, which resulted in 9 false-positives vs. 854 with standard screening.
While far fewer cases of trisomy 18 (Edwards syndrome) and trisomy 13 (Patau syndrome) were found in the study population, the accuracy of cfDNA screening still surpassed standard screening.
The researchers emphasized areas of caution. Standard screening “can identify risk for a broad array of abnormalities that are not detectable on cfDNA testing,” they said. Additionally, a surprisingly high number of aneuploidies were present in the 488 pregnant women whose blood samples were disqualified (due to inadequate or immeasurable quantity of fetal DNA, or assay failure, or high sequencing-variance that could lead to misinterpreting results). Had this disqualified cohort been included in the findings, detection rates of the cfDNA test would have been lower.
cfDNA tests will result in far fewer false-positives than current screening, and so can reduce the number of invasive tests and of miscarriages wrongly attributed to positives. However, patients should be made aware of its limitations. “Providers need to be attuned to patients’ preferences and counsel them about the differences in prenatal screening options. Women who opt for cfDNA testing should be informed that it is highly accurate for DS, but it focuses on a small number of chromosomal abnormalities and does not provide the comprehensive assessment available with other approaches,” said Prof. Norton, “Counseling should also include information about the risks associated with failed tests and the pros and cons of pursuing invasive testing if no results are obtained.”
The study, by Norton M et al., was published April 1, 2015, in the New England Journal of Medicine.
Related Links:
University of California San Francisco
Ariosa Diagnostics’s Harmony prenatal blood test for trisomy 21, 18, & 13
Perinatal Quality Foundation
Latest Molecular Diagnostics News
- New PCR Assay Supports Bundibugyo Ebola Outbreak Surveillance
- Plasma Protein Signature Predicts Lung Cancer Risk Up to Five Years Ahead
- Circulating Tumor DNA Testing Guides Chemotherapy, Reduces Relapse in Colon Cancer
- Researchers Uncover Distinct Chromosome Signature in Aggresive ALT Cancers
- Simple Cytogenetic Method Could Improve Classification of ALL Subtypes
- Blood-Based Assay Enables Noninvasive Monitoring of Sarcoma Immunotherapy Response
- Genomic Test Guides Chemotherapy Decisions in Early-Stage Breast Cancer
- Tumor Mutation Marker Helps Refine Lung Cancer Prognosis and Guide Therapy Selection
- Multi-Cancer Test Boosts Detection When Added to Standard Screening
- Blood-Based MRD Monitoring Supports Relapse Prevention in Leukemia
- Genomic Test Predicts Chemotherapy Benefit in Metastatic Prostate Cancer
- Blood Protein Markers Flag Multiple Sclerosis Risk Years Before Diagnosis
- Digital PCR Assays Support Surveillance of Bundibugyo Ebolavirus Outbreak
- Updated Guidance Prioritizes Stool-Based Colorectal Cancer Screening Tests
- Blood-Based Proteomic Test May Predict Treatment Response in Non-Small Cell Lung Cancer
- Position Statements Outline Evidence Standards for Multi-Cancer Detection Tests
Channels
Clinical Chemistry
view channel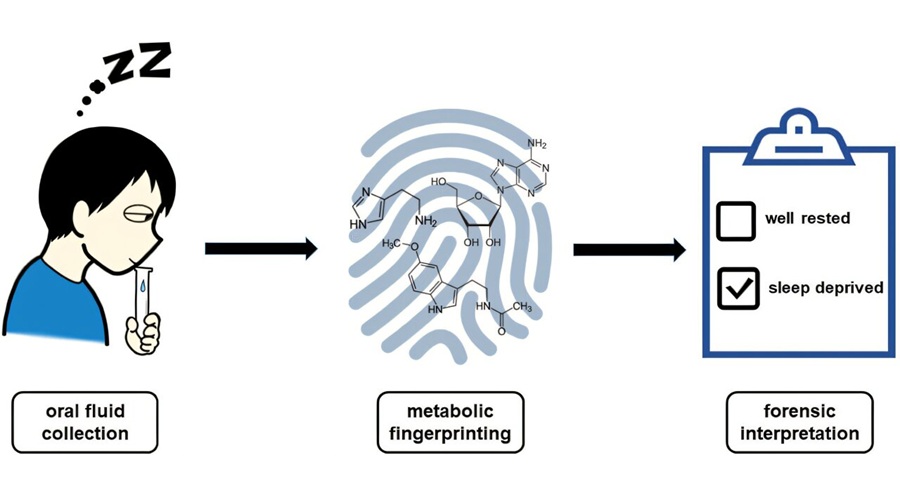
Saliva-Based Test Detects Biochemical Signs of Sleep Loss
Acute sleep loss impairs cognition and motor skills, raising safety risks that resemble alcohol intoxication. Clinicians currently lack an objective biochemical test to determine when someone is dangerously... Read more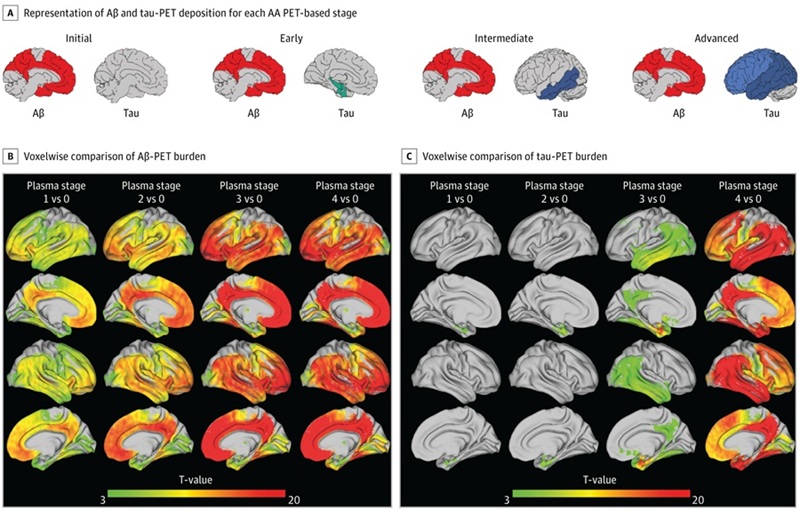
Simple Dual-Tau Blood Test Detects and Stages Alzheimer’s Disease
Alzheimer’s disease is typically confirmed and staged with positron emission tomography scans and cerebrospinal fluid testing, procedures that are costly and invasive. Broader access to minimally invasive... Read more
Alzheimer’s Blood Biomarkers Linked to Early Cognitive Differences Before Dementia
Blood-based screening for Alzheimer’s disease offers a noninvasive, lower-cost alternative to brain imaging or spinal fluid testing, yet its ability to flag the earliest cognitive changes has been unclear.... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channelAptamer-Based Biosensor Enables Mutation-Resilient SARS-CoV-2 Detection
Rapid evolution of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can undermine existing molecular diagnostics, especially when assays target small viral components. Double-antibody sandwich... Read more
Study Points to Autoimmune Pathway Behind Long COVID Symptoms
Long COVID leaves many SARS-CoV-2 survivors with persistent fatigue, cognitive issues, palpitations, and musculoskeletal pain for months or years. Estimates cited in new research suggest 4%–20% of infected... Read more
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read moreMicrobiology
view channel
New Culture Medium Speeds C. difficile Resistance Detection and Reduces Costs
Clostridioides difficile infections remain a persistent threat in hospitals and communities, affecting about 500,000 people in the United States each year. Severe cases can be fatal within 30 days of diagnosis,... Read more
Automated Blood Culture System Speeds Detection of Bloodstream Infections
Bloodstream infections and sepsis require rapid laboratory detection to guide targeted antimicrobial therapy and reduce mortality. Conventional blood culture workflows can delay actionable results by critical... Read morePathology
view channel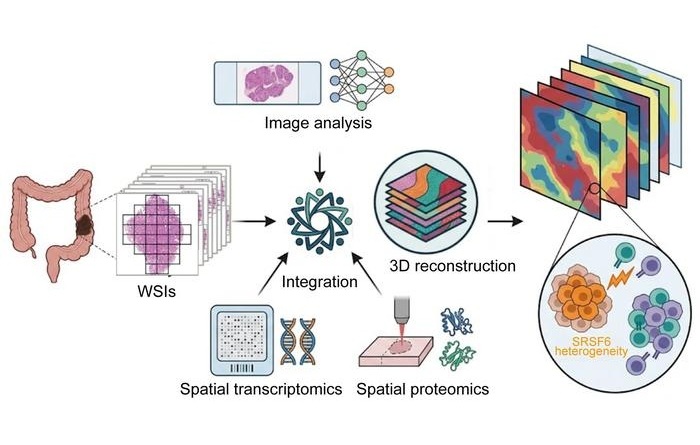
3D Spatial Multi-Omics Maps Intra-Tumor Diversity in Colorectal Cancer
Colorectal cancer remains a leading cause of cancer death, and clinical decision-making is complicated by marked intra-tumor heterogeneity. Conventional bulk sequencing averages molecular signals across... Read more
Blood-Based Method Tracks Gene Activity in the Living Brain
Real-time measurement of gene activity in the brain has been limited by assays requiring destructive tissue sampling. Tracking active genes could reveal how the body responds to environmental factors,... Read moreTechnology
view channel
AI Platform Links Biomarker Results to Cancer Clinical Trials and Guidelines
Oncology teams must manage growing volumes of genomic data, rapidly evolving clinical trial options, and frequently updated care guidelines, all within tight clinic schedules. Translating complex tumor... Read more
Agentic AI Platform Supports Genomic Decision-Making in Oncology
Oncology care teams increasingly face the challenge of managing complex molecular diagnostics, evolving treatment options, and extensive electronic health record documentation. Translating multimodal data... Read moreIndustry
view channel
Collaboration Advances ctDNA-Guided Development in Metastatic Colorectal Cancer
Natera, Inc. (Austin, TX, USA) and CytoDyn Inc. (Vancouver, WA, USA) announced a strategic collaboration focused on metastatic colorectal cancer (mCRC). Under the agreement, Natera will evaluate circulating... Read more