Discarded Blood Tests May Offer Life-Saving Information
|
By LabMedica International staff writers Posted on 08 Sep 2014 |
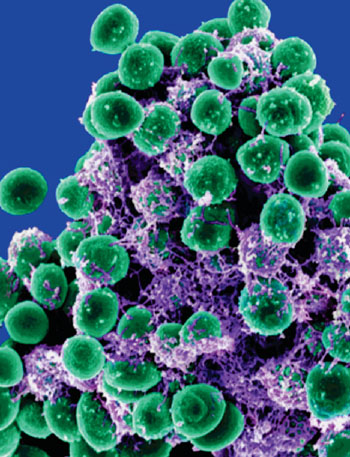
Image: Scanning electron micrograph of Staphylococcus epidermidis, the commonest coagulase-negative staphylococci found on the skin (Photo courtesy of the US National Institute of Allergy and Infectious Diseases).
Blood culture isolates are the cornerstone of adequate antibiotic treatment, but many blood cultures are contaminated with bacteria residing on the skin, and the most common contaminants are coagulase-negative staphylococci (CoNS).
Such contaminated cultures are mostly disregarded and discarded but in fact these contaminated cultures contain diagnostic information such as the antibiotic resistance profiles of CoNS contaminants and those of the actual infecting bacteria isolated subsequently from the same patient.
Clinical scientists at the Sackler Faculty of Medicine (Tel Aviv, Israel) conducted a retrospective study on patients with positive blood cultures from 2009 to 2012. Data included patient demographics, hospitalization records, comorbidities, blood culture results and date of death. The cohort consisted of 2,518 patients with 5,290 blood cultures, where 1,124 patients had 1,664 blood cultures with CoNS contaminants.
High overall CoNS resistance predicted high overall resistance of the subsequent bacterial isolates for Gram-positive and Gram-negative bacteria. The resistance of CoNS contaminants to a specific antibiotic predicted the resistance of the subsequent bacterial isolates to that antibiotic and highly resistant CoNS isolates were associated with higher short-term mortality.
The team noted that most hospital patients are treated at the outset with broad spectrum antibiotics. Days later, after initial test results are known, clinicians replace broad spectrum antibiotics with more precise narrow-spectrum antibiotics, which treat the specific bacteria identified by the blood sample. Narrow spectrum antibiotics are better for the body because they target specific bacteria as opposed to an entire microenvironment. Moreover, broad spectrum antibiotics might result in altered bacterial environments of the skin and gastro-intestinal tract, promoting inflammation and the emergence of resistant pathogens.
Gideon Y Stein, MD, PhD, a lead author of the study said, “Because we have found a direct correlation between resistance profiles of CoNS contaminants and those of the actual infecting bacteria isolated from the same patient, the results of these “junk” samples can be used to predict patient mortality and correct empirical antibiotic therapy. This should serve as an additional, noninvasive, diagnostic tool.” The study was published in the September issue of the Journal of Antimicrobial Chemotherapy.
Related Links:
Tel Aviv University Sackler Faculty of Medicine
Such contaminated cultures are mostly disregarded and discarded but in fact these contaminated cultures contain diagnostic information such as the antibiotic resistance profiles of CoNS contaminants and those of the actual infecting bacteria isolated subsequently from the same patient.
Clinical scientists at the Sackler Faculty of Medicine (Tel Aviv, Israel) conducted a retrospective study on patients with positive blood cultures from 2009 to 2012. Data included patient demographics, hospitalization records, comorbidities, blood culture results and date of death. The cohort consisted of 2,518 patients with 5,290 blood cultures, where 1,124 patients had 1,664 blood cultures with CoNS contaminants.
High overall CoNS resistance predicted high overall resistance of the subsequent bacterial isolates for Gram-positive and Gram-negative bacteria. The resistance of CoNS contaminants to a specific antibiotic predicted the resistance of the subsequent bacterial isolates to that antibiotic and highly resistant CoNS isolates were associated with higher short-term mortality.
The team noted that most hospital patients are treated at the outset with broad spectrum antibiotics. Days later, after initial test results are known, clinicians replace broad spectrum antibiotics with more precise narrow-spectrum antibiotics, which treat the specific bacteria identified by the blood sample. Narrow spectrum antibiotics are better for the body because they target specific bacteria as opposed to an entire microenvironment. Moreover, broad spectrum antibiotics might result in altered bacterial environments of the skin and gastro-intestinal tract, promoting inflammation and the emergence of resistant pathogens.
Gideon Y Stein, MD, PhD, a lead author of the study said, “Because we have found a direct correlation between resistance profiles of CoNS contaminants and those of the actual infecting bacteria isolated from the same patient, the results of these “junk” samples can be used to predict patient mortality and correct empirical antibiotic therapy. This should serve as an additional, noninvasive, diagnostic tool.” The study was published in the September issue of the Journal of Antimicrobial Chemotherapy.
Related Links:
Tel Aviv University Sackler Faculty of Medicine
Latest Microbiology News
- Automated Blood Culture System Speeds Detection of Bloodstream Infections
- New Culture Medium Speeds C. difficile Resistance Detection and Reduces Costs
- Gut Microbiome Signatures Help Identify Risk of IBD Progression
- FDA-Cleared Gastrointestinal Panel Detects 24 Pathogen Targets
- New AMR Assay Supports Rapid Infection Control Screening in Hospitals
- Diagnostic Gaps Complicate Bundibugyo Ebola Outbreak Response in Congo
- Study Finds Hidden Mpox Infections May Drive Ongoing Spread
- Large-Scale Genomic Surveillance Tracks Resistant Bacteria Across European Hospitals
- Molecular Urine and Stool Tests Do Not Improve Early TB Treatment in Hospitalized HIV Patients
- Rapid Antigen Biosensor Detects Active Tuberculosis in One Hour
- Label-Free Microscopy Method Enables Faster, Quantitative Detection of Malaria
- Oral–Gut Microbiome Signatures Identify Early Gastric Cancer
- Gut Microbiome Test Predicts Melanoma Recurrence After Surgery
- Rapid Blood-Culture Susceptibility Panel Expands Coverage for Gram-Negative Infections
- Antibiotic Resistance Genes Found in Newborns Within Hours of Birth
- Rapid Color Test Stratifies Virulent and Resistant Staph Strains
Channels
Clinical Chemistry
view channel
Saliva-Based Test Detects Biochemical Signs of Sleep Loss
Acute sleep loss impairs cognition and motor skills, raising safety risks that resemble alcohol intoxication. Clinicians currently lack an objective biochemical test to determine when someone is dangerously... Read more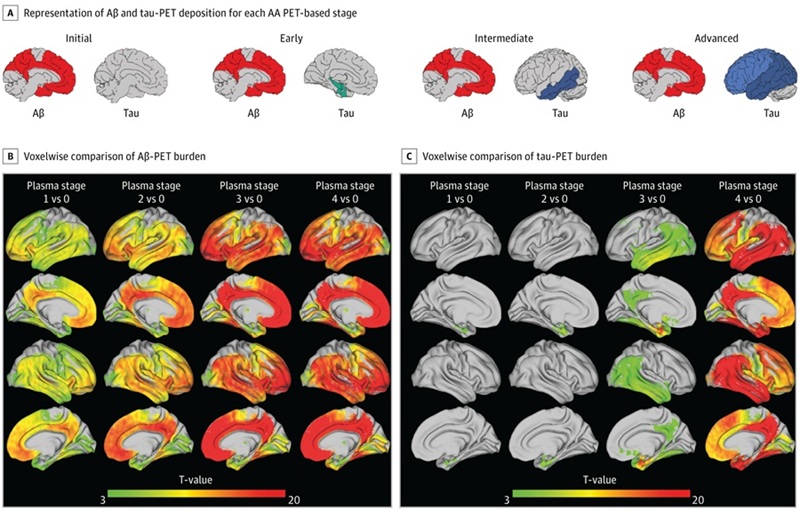
Simple Dual-Tau Blood Test Detects and Stages Alzheimer’s Disease
Alzheimer’s disease is typically confirmed and staged with positron emission tomography scans and cerebrospinal fluid testing, procedures that are costly and invasive. Broader access to minimally invasive... Read more
Alzheimer’s Blood Biomarkers Linked to Early Cognitive Differences Before Dementia
Blood-based screening for Alzheimer’s disease offers a noninvasive, lower-cost alternative to brain imaging or spinal fluid testing, yet its ability to flag the earliest cognitive changes has been unclear.... Read moreMolecular Diagnostics
view channel
Blood Test Predicts Immunotherapy Response in Head and Neck Cancer
Head and neck squamous cell carcinoma affects hundreds of thousands of people worldwide each year, yet response rates to immunotherapy remain low. Clinicians lack reliable, minimally invasive tools to... Read more
New PCR Assay Supports Bundibugyo Ebola Outbreak Surveillance
Rapid identification of Ebola infections is essential to limit transmission and guide public health response, yet detection can be difficult when outbreaks involve rare variants. The current outbreaks... Read moreHematology
view channel
Next-Generation Hematology Platform Streamlines High-Complexity Lab Workflows
Sysmex America (Chicago, IL, USA) has introduced the next generation XR-Series, centered on the XR-10 Automated Hematology Module for high-complexity laboratories. The platform builds on the widely used... Read more
Blood Eosinophil Count May Predict Cancer Immunotherapy Response and Toxicity
Immune checkpoint inhibitors have improved outcomes across many cancers, yet only a subset of patients derive durable benefit and biomarkers to guide treatment remain limited. Eosinophils, best known for... Read moreImmunology
view channelAptamer-Based Biosensor Enables Mutation-Resilient SARS-CoV-2 Detection
Rapid evolution of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) can undermine existing molecular diagnostics, especially when assays target small viral components. Double-antibody sandwich... Read more
Study Points to Autoimmune Pathway Behind Long COVID Symptoms
Long COVID leaves many SARS-CoV-2 survivors with persistent fatigue, cognitive issues, palpitations, and musculoskeletal pain for months or years. Estimates cited in new research suggest 4%–20% of infected... Read more
Metabolic Biomarker Distinguishes Latent from Active Tuberculosis and Tracks Treatment Response
Tuberculosis (TB) remains the world’s leading infectious killer, with 10.8 million cases and 1.25 million deaths recorded globally in 2023. Yet many infected individuals never develop active disease, underscoring... Read morePathology
view channel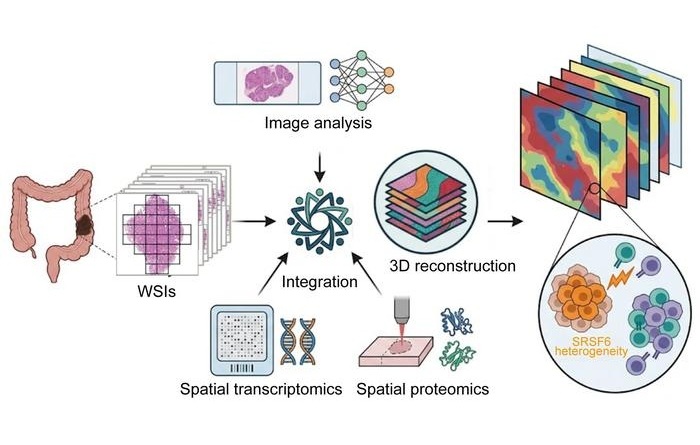
3D Spatial Multi-Omics Maps Intra-Tumor Diversity in Colorectal Cancer
Colorectal cancer remains a leading cause of cancer death, and clinical decision-making is complicated by marked intra-tumor heterogeneity. Conventional bulk sequencing averages molecular signals across... Read more
Blood-Based Method Tracks Gene Activity in the Living Brain
Real-time measurement of gene activity in the brain has been limited by assays requiring destructive tissue sampling. Tracking active genes could reveal how the body responds to environmental factors,... Read moreTechnology
view channel
AI Platform Links Biomarker Results to Cancer Clinical Trials and Guidelines
Oncology teams must manage growing volumes of genomic data, rapidly evolving clinical trial options, and frequently updated care guidelines, all within tight clinic schedules. Translating complex tumor... Read more
Agentic AI Platform Supports Genomic Decision-Making in Oncology
Oncology care teams increasingly face the challenge of managing complex molecular diagnostics, evolving treatment options, and extensive electronic health record documentation. Translating multimodal data... Read moreIndustry
view channel
Collaboration Advances ctDNA-Guided Development in Metastatic Colorectal Cancer
Natera, Inc. (Austin, TX, USA) and CytoDyn Inc. (Vancouver, WA, USA) announced a strategic collaboration focused on metastatic colorectal cancer (mCRC). Under the agreement, Natera will evaluate circulating... Read more