Stem Cell and CRISPR Technologies Combine to Study Mutant Tau Genes
By LabMedica International staff writers
Posted on 26 Dec 2018
A mutant form of the gene coding for tau protein contributes to the development of frontotemporal dementia by reducing the expression of GABA (gamma-aminobutyric acid) receptor genes in the brain.Posted on 26 Dec 2018
Frontotemporal dementia, which accounts for about 20% of all cases of early-onset dementia, tends to afflict people with memory loss from the age of 40 to the early 60s. Previous studies have shown that mutations in the microtubule-associated protein tau (MAPT) gene cause autosomal dominant frontotemporal lobar degeneration with tau inclusions (FTLD-tau). Individuals carrying the MAPT p.R406W mutation present clinically with progressive memory loss and neuropathologically with neuronal and glial tauopathy. However, the pathogenic events triggered by the expression of the mutant tau protein remain poorly understood.
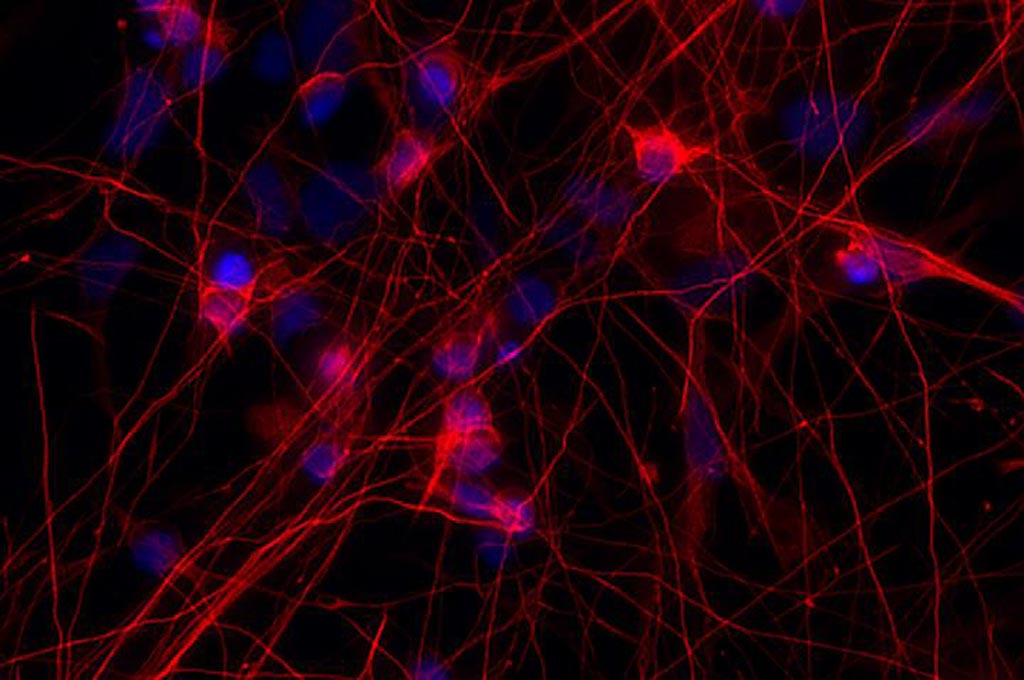
Image: The photomicrograph shows neurons (red) with a mutation in the MAPT gene - a gene that makes the protein tau. People with this mutation develop frontotemporal dementia. Researchers found that cells carrying the MAPT mutation developed abnormalities in genes that control communication between the brain cells (Photo courtesy of Sidhartha Mahali, Washington University School of Medicine).
To determine how mutant tau protein causes memory loss, investigators at Washington University School of Medicine (St, Louis, MO, USA) used a combination of stem cell technology and CRISPR/cas9 gene editing.
The investigators prepared neurons with the MAPT mutation that had been derived from induced pluripotent stem cells (iPSCs) generated from skin cells obtained from FTLD-tau patients. CRISPR/Cas9 gene editing was used to eliminate the mutation in some neurons but not in others (isogeneic controls).
The investigators reported in the December 13, 2018, online edition of the journal Translational Psychiatry that the expression of the MAPT p.R406W mutation was sufficient to create a significantly different transcriptomic profile compared with that of the isogeneic controls and to cause the differential expression of 328 genes. Sixty-one of these genes were also differentially expressed in the same direction between MAPT p.R406W carriers and pathology-free human control brains.
Genes differentially expressed in the stem cell models and human brains were enriched for pathways involving gamma-aminobutyric acid (GABA) receptors and pre-synaptic function. The expression of GABA receptor genes, including GABRB2 and GABRG2, were consistently reduced in iPSC-derived neurons and brains from MAPT p.R406W carriers. In addition, GABA receptor genes, including GABRB2 and GABRG2, are significantly lower in symptomatic mouse models of tauopathy. Genome wide association analyses reveal that common variants within GABRB2 were associated with increased risk for frontotemporal dementia.
The investigators suggested that by demonstrating that MAPT p.R406W was sufficient to induce changes in GABA-mediated signaling and synaptic function, which may contribute to the pathogenesis of FTLD-tau and other primary tauopathies, they had confirmed a systems biology approach, which leveraged molecular data from stem cells, animal models, and human brain tissue to reveal novel disease mechanisms.
"We have demonstrated that we can capture changes in human cells cultured in a dish that also are appearing in the brains of individuals suffering with frontotemporal dementia," said senior author Dr. Celeste M. Karch, assistant professor of psychiatry at Washington University School of Medicine. "Importantly, the approach we are using allows us to zero in on genes and pathways that are altered in cells and in patient brains that may be influenced by compounds already approved by the FDA. We want to evaluate whether any of these compounds could prevent memory loss, or even restore memory, in people with frontotemporal dementia by improving the function of these pathways that have been disrupted."
Related Links:
Washington University School of Medicine