Measurement of Calcium-Binding Protein Diagnoses Intracranial Hemorrhage
|
By LabMedica International staff writers Posted on 19 Jul 2015 |
Cranial computed tomography scans and hospital admission are increasingly performed to rule out intracranial hemorrhage in patients after minor head injury (MHI), particularly in older patients and in those receiving antiplatelet therapy.
This leads to high radiation exposure and a growing financial burden, so a blood test for the astroglial-derived protein S100B has been developed as a reliable negative predictive tool for intracranial bleeding in patients after MHI, when they are older than 65 years or being treated with antiplatelet drugs such as low-dose aspirin or clopidogrel.
Scientists at the Medical University of Vienna (Austria) conducted a prospective observational study in two trauma hospitals and a total of 782 patients with MHI who were on medication with platelet aggregation inhibitors (PAIs) or were age 65 years and older, independent of antiplatelet therapy, were included. The median age of the patients was 83 years, and 69% were female. All patients underwent cranial computed tomography (CCT).
Blood was drawn from all patients and laboratory measurements were performed immediately. The time interval between the index event and the blood draw was limited to three hours as this time period is based on the half-life of about 90 minutes for the calcium-binding protein B (S100B) molecule. All blood specimens were processed to serum and the serum S100B levels were determined by electrochemiluminescence immunoassay Elecsys S100 (Roche Diagnostics; Basel, Switzerland) on the Roche cobas e601 and cobas e411 instruments. The analytical range was 0.005µg/L to 39 µg/L and the cutoff was set at 0.105 μg/L.
In the CCT-positive group, 24 patients were diagnosed with subdural, 14 with intracerebral, and 12 with subarachnoid hematoma; no epidural hematoma was found and the median serum S100B concentration was 0.285 μg/L. In the CCT-negative group, 35.3% showed S100B concentrations below the cutoff value of 0.105 μg/L; 64.7% were at or above the cutoff value and the median serum S100B concentration was 0.143 μg/L in this group. Of all 782 patients, 259 (33.1%) showed an S100B value below the cutoff of 0.105 μg/L. Calculation of sensitivity and specificity yielded the following results: 98.0% sensitivity; negative predictive value (NPV) was 99.6%; 35.3% specificity; and positive predictive value (PPV) was 9.4%.
Heinrich Wolfgang Thaler, MD, the lead author of the study said, “We undertook the study with the aim to reduce the workload of medical staff and costs as well as the radiation burden in the management of patients with mild head injuries. We are confident that this study will prove to be useful in achieving these aims.” The study was published on July 7, 2015, in the Journal of Neurosurgery.
Related Links:
Medical University of Vienna
Roche Diagnostics
This leads to high radiation exposure and a growing financial burden, so a blood test for the astroglial-derived protein S100B has been developed as a reliable negative predictive tool for intracranial bleeding in patients after MHI, when they are older than 65 years or being treated with antiplatelet drugs such as low-dose aspirin or clopidogrel.
Scientists at the Medical University of Vienna (Austria) conducted a prospective observational study in two trauma hospitals and a total of 782 patients with MHI who were on medication with platelet aggregation inhibitors (PAIs) or were age 65 years and older, independent of antiplatelet therapy, were included. The median age of the patients was 83 years, and 69% were female. All patients underwent cranial computed tomography (CCT).
Blood was drawn from all patients and laboratory measurements were performed immediately. The time interval between the index event and the blood draw was limited to three hours as this time period is based on the half-life of about 90 minutes for the calcium-binding protein B (S100B) molecule. All blood specimens were processed to serum and the serum S100B levels were determined by electrochemiluminescence immunoassay Elecsys S100 (Roche Diagnostics; Basel, Switzerland) on the Roche cobas e601 and cobas e411 instruments. The analytical range was 0.005µg/L to 39 µg/L and the cutoff was set at 0.105 μg/L.
In the CCT-positive group, 24 patients were diagnosed with subdural, 14 with intracerebral, and 12 with subarachnoid hematoma; no epidural hematoma was found and the median serum S100B concentration was 0.285 μg/L. In the CCT-negative group, 35.3% showed S100B concentrations below the cutoff value of 0.105 μg/L; 64.7% were at or above the cutoff value and the median serum S100B concentration was 0.143 μg/L in this group. Of all 782 patients, 259 (33.1%) showed an S100B value below the cutoff of 0.105 μg/L. Calculation of sensitivity and specificity yielded the following results: 98.0% sensitivity; negative predictive value (NPV) was 99.6%; 35.3% specificity; and positive predictive value (PPV) was 9.4%.
Heinrich Wolfgang Thaler, MD, the lead author of the study said, “We undertook the study with the aim to reduce the workload of medical staff and costs as well as the radiation burden in the management of patients with mild head injuries. We are confident that this study will prove to be useful in achieving these aims.” The study was published on July 7, 2015, in the Journal of Neurosurgery.
Related Links:
Medical University of Vienna
Roche Diagnostics
Read the full article by registering today, it's FREE! 

Register now for FREE to LabMedica.com and get complete access to news and events that shape the world of Clinical Laboratory Medicine. 
- Free digital version edition of LabMedica International sent by email on regular basis
- Free print version of LabMedica International magazine (available only outside USA and Canada).
- Free and unlimited access to back issues of LabMedica International in digital format
- Free LabMedica International Newsletter sent every week containing the latest news
- Free breaking news sent via email
- Free access to Events Calendar
- Free access to LinkXpress new product services
- REGISTRATION IS FREE AND EASY!
Sign in: Registered website members
Sign in: Registered magazine subscribers
Latest Immunology News
- AI Predicts Tumor-Killing Cells with High Accuracy
- Diagnostic Blood Test for Cellular Rejection after Organ Transplant Could Replace Surgical Biopsies
- AI Tool Precisely Matches Cancer Drugs to Patients Using Information from Each Tumor Cell
- Genetic Testing Combined With Personalized Drug Screening On Tumor Samples to Revolutionize Cancer Treatment
- Testing Method Could Help More Patients Receive Right Cancer Treatment
- Groundbreaking Test Monitors Radiation Therapy Toxicity in Cancer Patients
- State-Of-The Art Techniques to Investigate Immune Response in Deadly Strep A Infections
- Novel Immunoassays Enable Early Diagnosis of Antiphospholipid Syndrome
- New Test Could Predict Immunotherapy Success for Broader Range Of Cancers
- Simple Blood Protein Tests Predict CAR T Outcomes for Lymphoma Patients
- Cell Sorter Chip Technology to Pave Way for Immune Profiling at POC
- Chip Monitors Cancer Cells in Blood Samples to Assess Treatment Effectiveness
- Automated Immunohematology Approaches Can Resolve Transplant Incompatibility
- AI Leverages Tumor Genetics to Predict Patient Response to Chemotherapy
- World’s First Portable, Non-Invasive WBC Monitoring Device to Eliminate Need for Blood Draw
- Predictive T-Cell Test Detects Immune Response to Viruses Even Before Antibodies Form
Channels
Clinical Chemistry
view channel
3D Printed Point-Of-Care Mass Spectrometer Outperforms State-Of-The-Art Models
Mass spectrometry is a precise technique for identifying the chemical components of a sample and has significant potential for monitoring chronic illness health states, such as measuring hormone levels... Read more.jpg)
POC Biomedical Test Spins Water Droplet Using Sound Waves for Cancer Detection
Exosomes, tiny cellular bioparticles carrying a specific set of proteins, lipids, and genetic materials, play a crucial role in cell communication and hold promise for non-invasive diagnostics.... Read more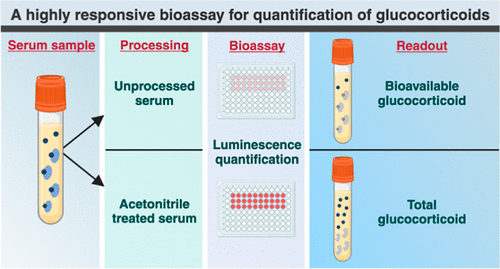
Highly Reliable Cell-Based Assay Enables Accurate Diagnosis of Endocrine Diseases
The conventional methods for measuring free cortisol, the body's stress hormone, from blood or saliva are quite demanding and require sample processing. The most common method, therefore, involves collecting... Read moreMolecular Diagnostics
view channelBlood Proteins Could Warn of Cancer Seven Years before Diagnosis
Two studies have identified proteins in the blood that could potentially alert individuals to the presence of cancer more than seven years before the disease is clinically diagnosed. Researchers found... Read moreUltrasound-Aided Blood Testing Detects Cancer Biomarkers from Cells
Ultrasound imaging serves as a noninvasive method to locate and monitor cancerous tumors effectively. However, crucial details about the cancer, such as the specific types of cells and genetic mutations... Read moreHematology
view channel
Next Generation Instrument Screens for Hemoglobin Disorders in Newborns
Hemoglobinopathies, the most widespread inherited conditions globally, affect about 7% of the population as carriers, with 2.7% of newborns being born with these conditions. The spectrum of clinical manifestations... Read more
First 4-in-1 Nucleic Acid Test for Arbovirus Screening to Reduce Risk of Transfusion-Transmitted Infections
Arboviruses represent an emerging global health threat, exacerbated by climate change and increased international travel that is facilitating their spread across new regions. Chikungunya, dengue, West... Read more
POC Finger-Prick Blood Test Determines Risk of Neutropenic Sepsis in Patients Undergoing Chemotherapy
Neutropenia, a decrease in neutrophils (a type of white blood cell crucial for fighting infections), is a frequent side effect of certain cancer treatments. This condition elevates the risk of infections,... Read more
First Affordable and Rapid Test for Beta Thalassemia Demonstrates 99% Diagnostic Accuracy
Hemoglobin disorders rank as some of the most prevalent monogenic diseases globally. Among various hemoglobin disorders, beta thalassemia, a hereditary blood disorder, affects about 1.5% of the world's... Read moreMicrobiology
view channel
Integrated Solution Ushers New Era of Automated Tuberculosis Testing
Tuberculosis (TB) is responsible for 1.3 million deaths every year, positioning it as one of the top killers globally due to a single infectious agent. In 2022, around 10.6 million people were diagnosed... Read more
Automated Sepsis Test System Enables Rapid Diagnosis for Patients with Severe Bloodstream Infections
Sepsis affects up to 50 million people globally each year, with bacteraemia, formerly known as blood poisoning, being a major cause. In the United States alone, approximately two million individuals are... Read moreEnhanced Rapid Syndromic Molecular Diagnostic Solution Detects Broad Range of Infectious Diseases
GenMark Diagnostics (Carlsbad, CA, USA), a member of the Roche Group (Basel, Switzerland), has rebranded its ePlex® system as the cobas eplex system. This rebranding under the globally renowned cobas name... Read more
Clinical Decision Support Software a Game-Changer in Antimicrobial Resistance Battle
Antimicrobial resistance (AMR) is a serious global public health concern that claims millions of lives every year. It primarily results from the inappropriate and excessive use of antibiotics, which reduces... Read morePathology
view channel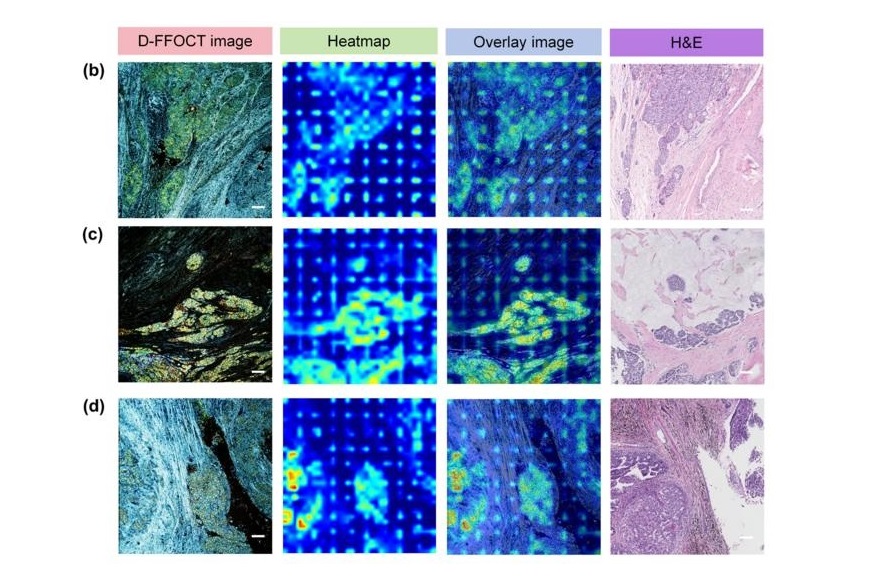
AI Integrated With Optical Imaging Technology Enables Rapid Intraoperative Diagnosis
Rapid and accurate intraoperative diagnosis is essential for tumor surgery as it guides surgical decisions with precision. Traditional intraoperative assessments, such as frozen sections based on H&E... Read more
HPV Self-Collection Solution Improves Access to Cervical Cancer Testing
Annually, over 604,000 women across the world are diagnosed with cervical cancer, and about 342,000 die from this disease, which is preventable and primarily caused by the Human Papillomavirus (HPV).... Read moreHyperspectral Dark-Field Microscopy Enables Rapid and Accurate Identification of Cancerous Tissues
Breast cancer remains a major cause of cancer-related mortality among women. Breast-conserving surgery (BCS), also known as lumpectomy, is the removal of the cancerous lump and a small margin of surrounding tissue.... Read moreTechnology
view channel
New Diagnostic System Achieves PCR Testing Accuracy
While PCR tests are the gold standard of accuracy for virology testing, they come with limitations such as complexity, the need for skilled lab operators, and longer result times. They also require complex... Read more
DNA Biosensor Enables Early Diagnosis of Cervical Cancer
Molybdenum disulfide (MoS2), recognized for its potential to form two-dimensional nanosheets like graphene, is a material that's increasingly catching the eye of the scientific community.... Read more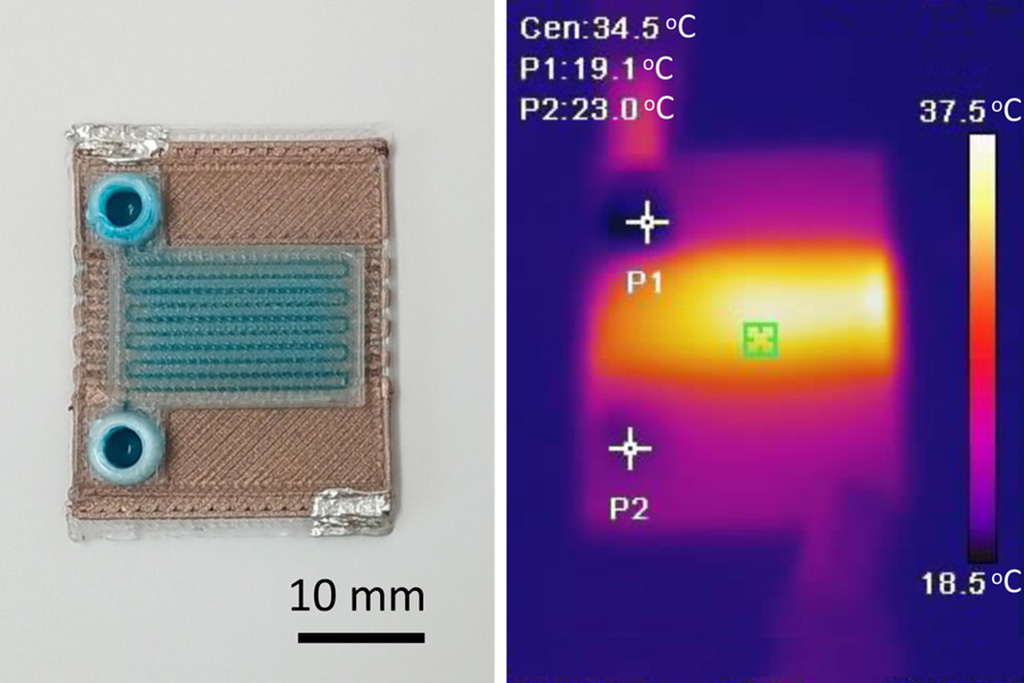
Self-Heating Microfluidic Devices Can Detect Diseases in Tiny Blood or Fluid Samples
Microfluidics, which are miniature devices that control the flow of liquids and facilitate chemical reactions, play a key role in disease detection from small samples of blood or other fluids.... Read more
Breakthrough in Diagnostic Technology Could Make On-The-Spot Testing Widely Accessible
Home testing gained significant importance during the COVID-19 pandemic, yet the availability of rapid tests is limited, and most of them can only drive one liquid across the strip, leading to continued... Read moreIndustry
view channel
Danaher and Johns Hopkins University Collaborate to Improve Neurological Diagnosis
Unlike severe traumatic brain injury (TBI), mild TBI often does not show clear correlations with abnormalities detected through head computed tomography (CT) scans. Consequently, there is a pressing need... Read more
Beckman Coulter and MeMed Expand Host Immune Response Diagnostics Partnership
Beckman Coulter Diagnostics (Brea, CA, USA) and MeMed BV (Haifa, Israel) have expanded their host immune response diagnostics partnership. Beckman Coulter is now an authorized distributor of the MeMed... Read more_1.jpg)













_1.jpg)
.jpg)