Cord Blood and Matched Related Donor Transplantation Compared in Acute Myeloid Leukemia
|
By LabMedica International staff writers Posted on 19 Jan 2022 |
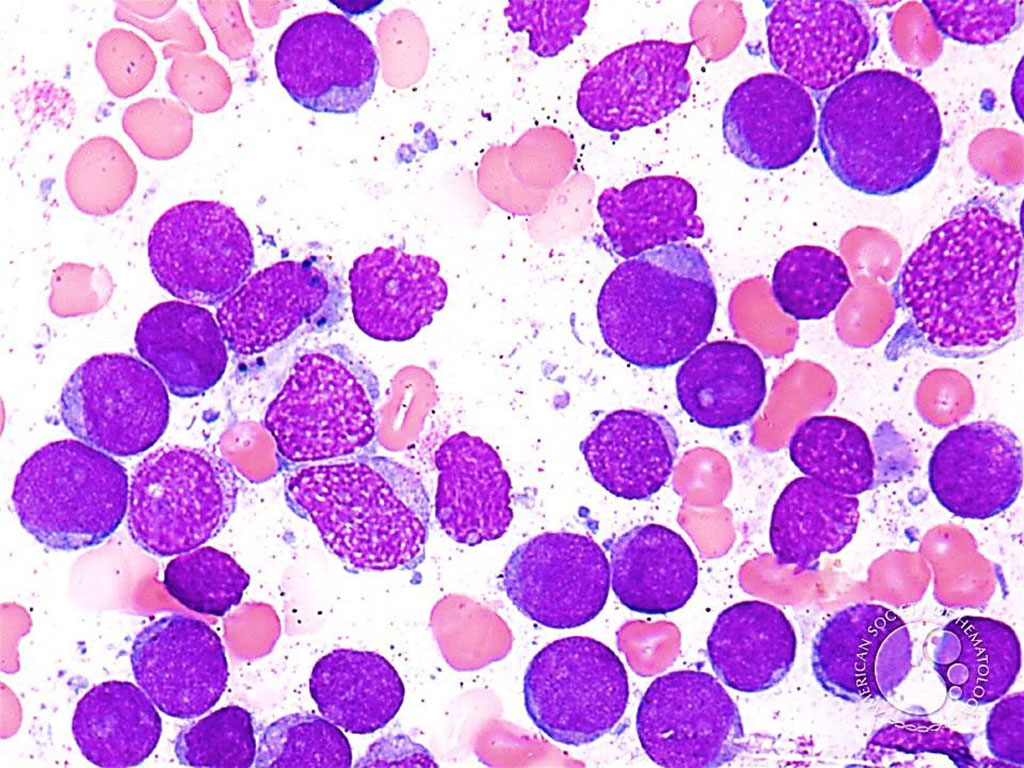
Image: Bone marrow aspirate from a patient with Acute Myeloid Leukemia: Blasts are the predominant population and have a high nuclear to cytoplasmic ratio and generally lack granules. (Photo courtesy of Professor Peter G. Maslak, MD)
The prognosis of primary refractory and relapsed acute myeloid leukemia is poor, with a five-year overall survival of less than 10%. Allogeneic hematopoietic stem cell transplantation (HSCT) is the only curative treatment option for these patients.
Cord blood transplantation (CBT) is an alternative donor transplantation method and has the advantages of rapid availability and the possibility of inducing a more potent graft-versus-leukemia effect, leading to a lower relapse rate for patients with non-remission relapse and refractory acute myeloid leukemia (R/R AML).
A large team of Hematologists at the Graduate School of Medicine Kyoto University (Kyoto, Japan) and their colleagues investigated the impact of CBT, compared to human leukocyte antigen-matched related donor transplantation (MRDT). The study included 2,451 adult patients with non-remission R/R AML who received CBT (1,738 patients) or MRDT (713 patients) between January 2009 and December 2018. The median age was 55 years (interquartile range, 43–63 years), with 1,484 patients (61%) being male. Karyotype risk, was estimated as 190 (8.2%), 1,352 (59%), and 768 (33%) patients had favorable, intermediate, and poor karyotypes, respectively.
There were 1,499 (61%) patients with primary induction failures and 952 (39%) with relapses. Among these patients, 1,576 (65%) had blasts in the peripheral blood. The myeloablative conditioning regimen (MAC) and reduced-intensity conditioning regimen were defined as previously described. HLA match was defined as the same serologically identified HLA-A, HLA-B, and HLA-DRB1 between the donor and recipient. Comparisons were made by examining the 5-year progression-free survival (PFS) rates of these Japanese patients.
The investigators reported that the primary endpoint, the 5-year PFS, was 22.2% (95% CI: 20.1–24.3%) in the CBT group and 19.9% (95% CI: 16.8–23.1%) in the MRDT group. The adjusted hazard ratio (HR) was 0.83 (95% CI: 0.69–1.00); this was due to a more pronounced decrease in the relapse rate (HR: 0.78, 95% CI: 0.69–0.89) than an increase in the non-relapse mortality (NRM: 1.42, 1.15–1.76). The CBT group had more patients with infection-related death and fewer patients with graft-versus-host disease (GVHD)-related deaths and death due to primary diseases.
Yoshimitsu Shimomura, MD, a Hematologist and the lead author of the study, said, “We believe CBT would be a great treatment option for R/R AML patients in non-remission given the circumstances. However, there are currently limited data for how this subset of patients would respond to CBT. Before comparing PFS rates, we performed propensity score matching. This took into account factors such as patient age, sex, years of treatment, and others to ensure all comparisons were as fair as possible and no biases were introduced. CBT compared with MDRT that had a more pronounced decrease in relapse rate than increase in NRM.”
The authors concluded that their data support CBT as a potential superior alternative to MRDT for patient prognosis and thus provide evidence which may influence clinical guidelines on R/R AML treatment. Future studies will investigate if genetic factors play any roles in patients’ responses to these two transplantation methods. Additionally, patient quality of life will be considered to optimize therapeutic development for this deadly disease. The study was originally published on November 21, 2021 in the journal Leukemia.
Related Links:
Graduate School of Medicine Kyoto University
Cord blood transplantation (CBT) is an alternative donor transplantation method and has the advantages of rapid availability and the possibility of inducing a more potent graft-versus-leukemia effect, leading to a lower relapse rate for patients with non-remission relapse and refractory acute myeloid leukemia (R/R AML).
A large team of Hematologists at the Graduate School of Medicine Kyoto University (Kyoto, Japan) and their colleagues investigated the impact of CBT, compared to human leukocyte antigen-matched related donor transplantation (MRDT). The study included 2,451 adult patients with non-remission R/R AML who received CBT (1,738 patients) or MRDT (713 patients) between January 2009 and December 2018. The median age was 55 years (interquartile range, 43–63 years), with 1,484 patients (61%) being male. Karyotype risk, was estimated as 190 (8.2%), 1,352 (59%), and 768 (33%) patients had favorable, intermediate, and poor karyotypes, respectively.
There were 1,499 (61%) patients with primary induction failures and 952 (39%) with relapses. Among these patients, 1,576 (65%) had blasts in the peripheral blood. The myeloablative conditioning regimen (MAC) and reduced-intensity conditioning regimen were defined as previously described. HLA match was defined as the same serologically identified HLA-A, HLA-B, and HLA-DRB1 between the donor and recipient. Comparisons were made by examining the 5-year progression-free survival (PFS) rates of these Japanese patients.
The investigators reported that the primary endpoint, the 5-year PFS, was 22.2% (95% CI: 20.1–24.3%) in the CBT group and 19.9% (95% CI: 16.8–23.1%) in the MRDT group. The adjusted hazard ratio (HR) was 0.83 (95% CI: 0.69–1.00); this was due to a more pronounced decrease in the relapse rate (HR: 0.78, 95% CI: 0.69–0.89) than an increase in the non-relapse mortality (NRM: 1.42, 1.15–1.76). The CBT group had more patients with infection-related death and fewer patients with graft-versus-host disease (GVHD)-related deaths and death due to primary diseases.
Yoshimitsu Shimomura, MD, a Hematologist and the lead author of the study, said, “We believe CBT would be a great treatment option for R/R AML patients in non-remission given the circumstances. However, there are currently limited data for how this subset of patients would respond to CBT. Before comparing PFS rates, we performed propensity score matching. This took into account factors such as patient age, sex, years of treatment, and others to ensure all comparisons were as fair as possible and no biases were introduced. CBT compared with MDRT that had a more pronounced decrease in relapse rate than increase in NRM.”
The authors concluded that their data support CBT as a potential superior alternative to MRDT for patient prognosis and thus provide evidence which may influence clinical guidelines on R/R AML treatment. Future studies will investigate if genetic factors play any roles in patients’ responses to these two transplantation methods. Additionally, patient quality of life will be considered to optimize therapeutic development for this deadly disease. The study was originally published on November 21, 2021 in the journal Leukemia.
Related Links:
Graduate School of Medicine Kyoto University
Latest Hematology News
- Stem Cell Biomarkers May Guide Precision Treatment in Acute Myeloid Leukemia
- Advanced CBC-Derived Indices Integrated into Hematology Platforms
- Blood Test Enables Early Detection of Multiple Myeloma Relapse
- Single Assay Enables Rapid HLA and ABO Genotyping for Transplant Matching
- Prognostic Biomarker Identified in Diffuse Large B-Cell Lymphoma
- Routine Blood Test Parameters Link Anemia to Cancer Risk and Mortality
- Prognostic Tool Guides Personalized Treatment in Rare Blood Cancer
- New Platelet Function Assay Enables Monitoring of Antiplatelet Therapy
- Open Multi-Omics Platform Identifies Prognostic Subtypes in Blood Cancers
- AI-Powered Digital Workflow Standardizes Bone Marrow Aspirate Morphology
- Rapid Cartridge-Based Test Aims to Expand Access to Hemoglobin Disorder Diagnosis
- New Guidelines Aim to Improve AL Amyloidosis Diagnosis
- Automated Hemostasis System Helps Labs of All Sizes Optimize Workflow
- Fast and Easy Test Could Revolutionize Blood Transfusions
- High-Sensitivity Blood Test Improves Assessment of Clotting Risk in Heart Disease Patients
- AI Algorithm Effectively Distinguishes Alpha Thalassemia Subtypes
Channels
Clinical Chemistry
view channel
Urine-Based Nanosensor Tracks Lung Cancer and Fibrosis Noninvasively
Lung cancer remains difficult to monitor for early progression and treatment resistance, while pulmonary fibrosis continues to pose major challenges for early diagnosis. Clinicians need repeatable, noninvasive... Read more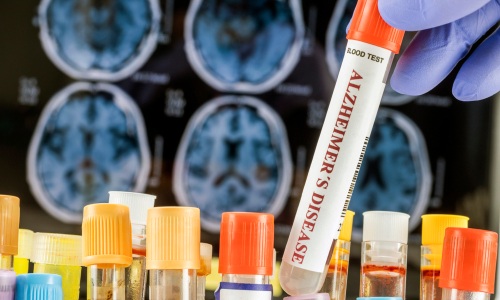
Blood-Based Alzheimer’s Test Gains CE Mark for Amyloid Pathology Detection
Alzheimer’s disease is the most common cause of dementia, yet confirmatory testing remains invasive and hard to access. Diagnosis currently takes an average of 3.5 years, and about 75% of people with dementia... Read moreMolecular Diagnostics
view channel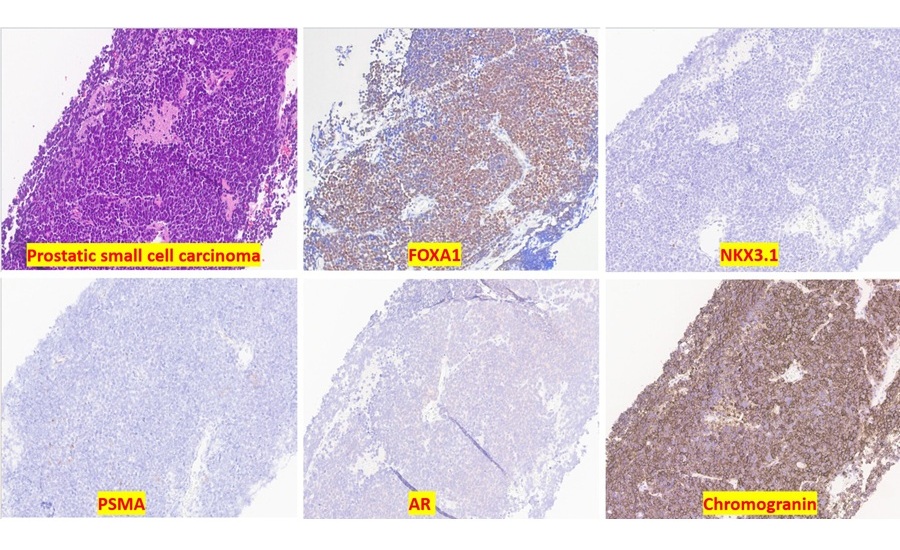
Sensitive Protein Marker Aids Diagnosis of Small Cell Prostate Cancer
Accurate identification of aggressive prostate cancer subtypes can be difficult when tumors lose expression of lineage markers used in routine pathology. Small cell carcinoma of the prostate, in particular,... Read more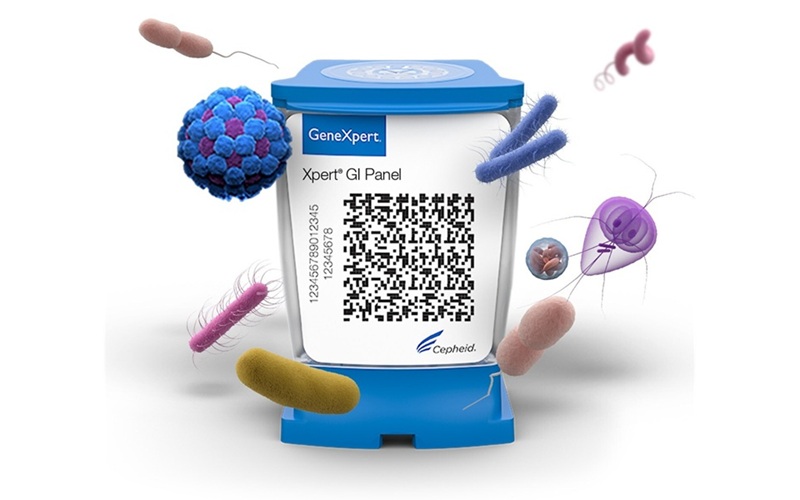
Rapid Multiplex PCR Test Detects 11 Gastrointestinal Pathogens from Single Sample
Cepheid’s Xpert GI Panel has received CE marking under the In Vitro Diagnostic Medical Devices Regulation (IVDR) and is expected to begin shipping to countries that accept the CE mark in the coming weeks.... Read moreImmunology
view channel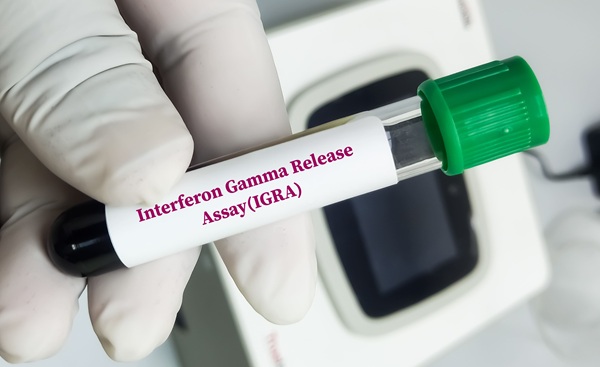
Routine TB Screening Test May Reveal Immune Aging and Mortality Risk
Immune aging is associated with weaker responses to vaccination, greater risks of infection, and higher levels of inflammation. Leveraging routinely ordered laboratory tests to quantify that responsiveness... Read more
Biomarkers and Molecular Testing Advance Precision Allergy Care
Allergic diseases often present with similar symptoms but can be driven by distinct biological mechanisms, making standardized care inefficient for many patients. Historically, individuals with pollen... Read moreMicrobiology
view channel
Study Finds Hidden Mpox Infections May Drive Ongoing Spread
Mpox continues to circulate despite vaccination, and many cases show no known link to a symptomatic partner. The role of people without symptoms has remained uncertain, limiting clarity on how transmission persists.... Read more
Large-Scale Genomic Surveillance Tracks Resistant Bacteria Across European Hospitals
Antimicrobial resistance (AMR) poses a growing threat to patient safety, with carbapenem-resistant Enterobacterales causing difficult-to-treat infections and leaving clinicians with limited therapeutic options.... Read more
Molecular Urine and Stool Tests Do Not Improve Early TB Treatment in Hospitalized HIV Patients
Tuberculosis is the leading cause of death among people living with HIV, and diagnosis in hospital settings remains difficult. Symptoms are often non-specific, disease can be extrapulmonary, and many patients... Read morePathology
view channel
FDA Clears AI Digital Pathology Tool for Breast Cancer Risk Stratification
Risk assessment at diagnosis is central to guiding therapy for early-stage, hormone receptor-positive, human epidermal growth factor receptor 2-negative (HR+/HER2-) invasive breast cancer, where overtreatment... Read more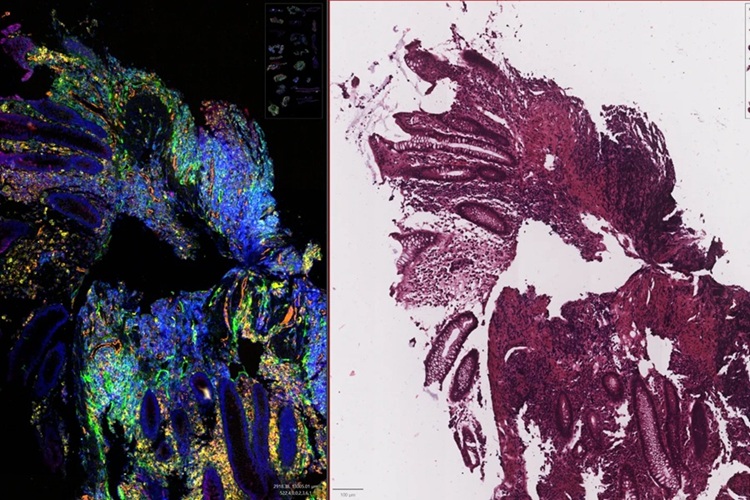
New AI Tool Reveals Hidden Genetic Signals in Routine H&E Slides
Pathologists worldwide rely on hematoxylin and eosin (H&E) slides to examine tissue architecture, yet these stains do not reveal the underlying molecular activity that often drives disease.... Read moreTechnology
view channel
Point-of-Care Testing Enhances Health Literacy and Self-Management in Chronic Disease
Limited access to general practitioners and pathology services can delay diagnosis and monitoring for people in regional and remote communities. Rapid, on-the-spot testing can shorten turnaround times... Read more
Fully Automated Sample-to-Insight Workflow Advances Latent TB Testing
Latent tuberculosis remains a substantial testing workload for clinical laboratories as screening programs expand. Despite this growth, only about 40% of testing has shifted from traditional skin tests... Read moreIndustry
view channel
AI-Powered Multi-Functional Analyzer Wins German Innovation Award
Hematology services are increasingly delivered across distributed care settings, where limited staffing and complex workflows can extend turnaround times. Advanced morphology review still often depends... Read more