Thromboelastography Identifies Undetected Blood Clots in COVID-19 Patients
|
By LabMedica International staff writers Posted on 15 Jun 2020 |

Image: Doctors recommend that all COVID-19 patients admitted to the ICU undergo a thromboelastography (TEG) to test for the risk of forming blood clots. The TEG 6s system provides rapid, comprehensive and accurate identification of an individual’s hemostasis condition in a laboratory or point-of-care setting (Photo courtesy of Haemonetics Corporation).
The coronavirus disease 2019 (COVID-19) pandemic has caused more than 400,000 deaths globally. Disseminated intravascular coagulopathy and other COVID-19–associated coagulopathies occur among patients with severe SARS-CoV-2 infections.
Thromboelastography (TEG) is a method of testing the efficiency of blood coagulation. It is a test mainly used in surgery and anesthesiology, although increasingly used in resuscitations in Emergency Departments, intensive care units, and labor and delivery suites.
Intensive Care Physicians at the Baylor St Luke’s Medical Center (Houston, TX, USA) and their associates observed 21 patients with COVID-19 infection from March 15 to April 9, 2020, confirmed with reverse transcription–polymerase chain reaction test of nasopharyngeal swab. All patients underwent TEG and TEG with heparinase correction on ICU admission. Hypercoagulability was defined as elevated fibrinogen activity greater than a 73° angle or maximum amplitude (MA) more than 65 mm on TEG with heparinase correction.
The doctors found that the standard clotting profile or screening of the patients was fairly normal. They were then moved to the next level of more specific clotting tests, which included analyzing a patient's fibrinogen and D dimer levels. Fibrinogen is the protein that makes up the clot and D dimer levels are used to indicate the rate at which a patient's clots are being broken down, which would usually suggest that the body is "chewing up" all of the clotting factors. For the COVID-19 patients in the ICU, the team found that the levels of fibrinogen were more than three times the normal range, indicating that the body was churning out this protein. Looking at these two results together, there was no clear indication that these patients were at increased risk for forming blood clots.
When the investigators used the thromboelastography test, they discovered the patients who they found were clotting their central intravenous and arterial lines and dialysis catheters had abnormally high clotting function compared to the patients who did not have clotting issues, and the clot breakdown function was significantly higher in the patients who were clotting less than others. Among the 21 patients studied, 13 of them, or 62%, developed 46 blood clots that could only be detected through the TEG test. For patients who are at a higher risk of blood clots as indicated by the TEG test, the team recommended administering additional blood thinners.
Todd K. Rosengart, MD, a cardiothoracic surgeon and senior author of the study, said, “The TEG test should be performed on all COVID-19 ICU patients immediately to find those who are at a higher risk of clotting. At the point where physicians discover that their central line and catheter is clotting, the horse is out of the barn.” The study was published on June 5, 2020 in the journal JAMA Network Open.
Related Links:
Baylor St Luke’s Medical Center
Thromboelastography (TEG) is a method of testing the efficiency of blood coagulation. It is a test mainly used in surgery and anesthesiology, although increasingly used in resuscitations in Emergency Departments, intensive care units, and labor and delivery suites.
Intensive Care Physicians at the Baylor St Luke’s Medical Center (Houston, TX, USA) and their associates observed 21 patients with COVID-19 infection from March 15 to April 9, 2020, confirmed with reverse transcription–polymerase chain reaction test of nasopharyngeal swab. All patients underwent TEG and TEG with heparinase correction on ICU admission. Hypercoagulability was defined as elevated fibrinogen activity greater than a 73° angle or maximum amplitude (MA) more than 65 mm on TEG with heparinase correction.
The doctors found that the standard clotting profile or screening of the patients was fairly normal. They were then moved to the next level of more specific clotting tests, which included analyzing a patient's fibrinogen and D dimer levels. Fibrinogen is the protein that makes up the clot and D dimer levels are used to indicate the rate at which a patient's clots are being broken down, which would usually suggest that the body is "chewing up" all of the clotting factors. For the COVID-19 patients in the ICU, the team found that the levels of fibrinogen were more than three times the normal range, indicating that the body was churning out this protein. Looking at these two results together, there was no clear indication that these patients were at increased risk for forming blood clots.
When the investigators used the thromboelastography test, they discovered the patients who they found were clotting their central intravenous and arterial lines and dialysis catheters had abnormally high clotting function compared to the patients who did not have clotting issues, and the clot breakdown function was significantly higher in the patients who were clotting less than others. Among the 21 patients studied, 13 of them, or 62%, developed 46 blood clots that could only be detected through the TEG test. For patients who are at a higher risk of blood clots as indicated by the TEG test, the team recommended administering additional blood thinners.
Todd K. Rosengart, MD, a cardiothoracic surgeon and senior author of the study, said, “The TEG test should be performed on all COVID-19 ICU patients immediately to find those who are at a higher risk of clotting. At the point where physicians discover that their central line and catheter is clotting, the horse is out of the barn.” The study was published on June 5, 2020 in the journal JAMA Network Open.
Related Links:
Baylor St Luke’s Medical Center
Latest Hematology News
- Single Assay Enables Rapid HLA and ABO Genotyping for Transplant Matching
- Prognostic Biomarker Identified in Diffuse Large B-Cell Lymphoma
- Routine Blood Test Parameters Link Anemia to Cancer Risk and Mortality
- Prognostic Tool Guides Personalized Treatment in Rare Blood Cancer
- New Platelet Function Assay Enables Monitoring of Antiplatelet Therapy
- Open Multi-Omics Platform Identifies Prognostic Subtypes in Blood Cancers
- AI-Powered Digital Workflow Standardizes Bone Marrow Aspirate Morphology
- Rapid Cartridge-Based Test Aims to Expand Access to Hemoglobin Disorder Diagnosis
- New Guidelines Aim to Improve AL Amyloidosis Diagnosis
- Automated Hemostasis System Helps Labs of All Sizes Optimize Workflow
- Fast and Easy Test Could Revolutionize Blood Transfusions
- High-Sensitivity Blood Test Improves Assessment of Clotting Risk in Heart Disease Patients
- AI Algorithm Effectively Distinguishes Alpha Thalassemia Subtypes
- MRD Tests Could Predict Survival in Leukemia Patients
- Platelet Activity Blood Test in Middle Age Could Identify Early Alzheimer’s Risk
- Microvesicles Measurement Could Detect Vascular Injury in Sickle Cell Disease Patients
Channels
Clinical Chemistry
view channel
Proteomic Data Underscore Need for Age-Specific Pediatric Reference Ranges
Serum proteins underpin many routine tests used to detect inflammation, hormonal imbalance, cardiovascular disease, and metabolic disorders. Yet pediatric interpretation often relies on adult reference... Read more
Routine Blood Count Ratio Linked to Future Alzheimer’s and Dementia Risk
Alzheimer’s disease and related dementias develop over years, making it difficult to identify at-risk patients before symptoms appear. Clinicians therefore need widely available laboratory markers that... Read more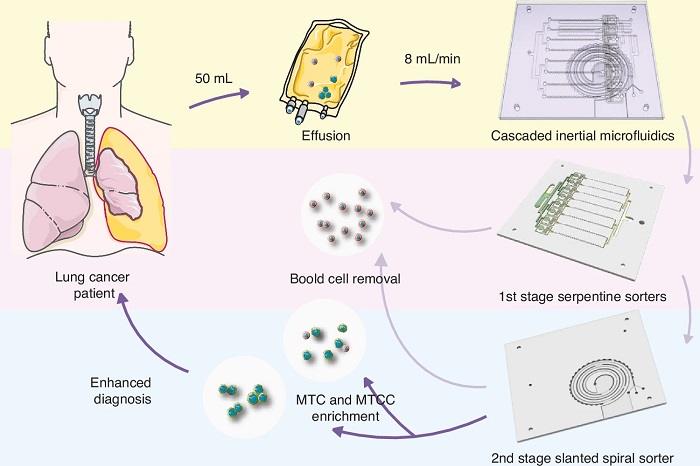
Label-Free Microfluidic Device Enriches Tumor Cells and Clusters from Pleural Effusions
Diagnosing malignancy from pleural effusion remains challenging because tumor cells are rare and clusters are easily disrupted during processing. Conventional cytology can miss malignant tumor cells and... Read moreMolecular Diagnostics
view channel
AI Blood Test Enhances Monitoring of Liver Cirrhosis Progression
Monitoring chronic liver disease remains difficult because clinicians rely on tools that can be inconsistent and may miss early progression. Standard approaches often combine ultrasound imaging with blood-based... Read more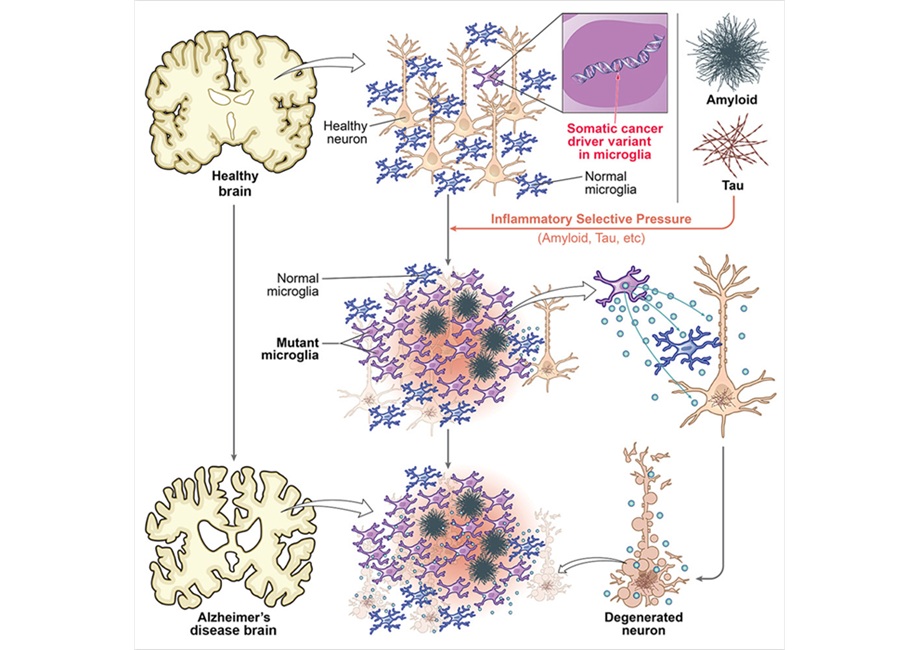
Cancer-Related Mutations in Immune Cells Linked to Alzheimer’s
Alzheimer’s disease is marked by protein aggregation and inflammatory changes in the brain’s immune system, yet its molecular drivers remain incompletely understood. With aging, human cells accumulate... Read more
Composite Blood Biomarkers Enable Early Detection of Common Cancers
Early diagnosis of colorectal, lung, and ovarian cancers remains challenging, with many patients identified only after tumors have begun to spread. A scalable blood test could expand access to screening,... Read more
Machine Learning Model Uses DNA Methylation to Predict Tumor Origin in Cancers of Unknown Primary
Cancers of unknown primary (CUP) are metastatic malignancies in which the primary site cannot be identified, complicating treatment selection. Many patients consequently receive broad, nonspecific chemotherapy... Read moreImmunology
view channel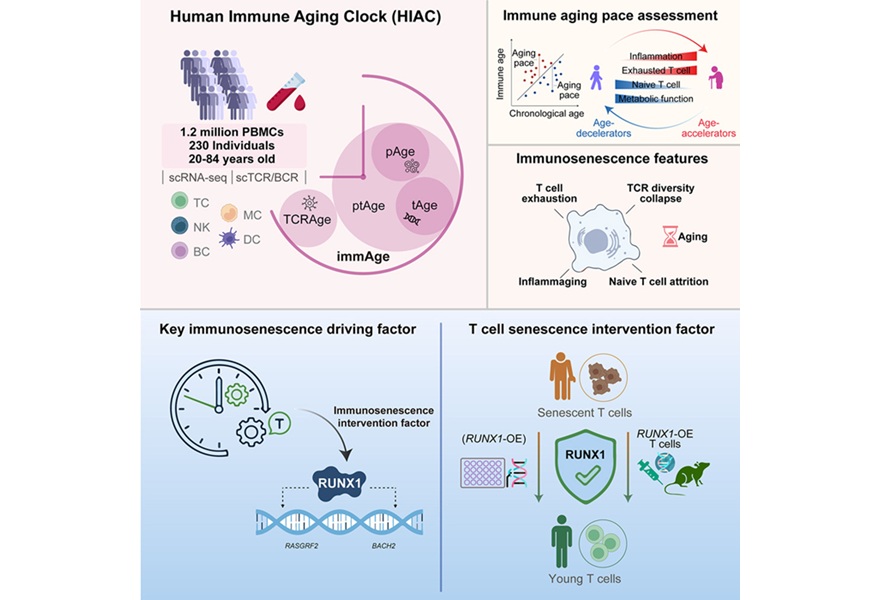
Immune Aging Clock Quantifies Immunosenescence and Identifies Therapeutic Target
Immune aging undermines host defense and contributes to multiple age-related diseases, yet its heterogeneity complicates measurement and intervention. Clinical laboratories increasingly seek objective... Read more
Study Finds Influenza Often Undiagnosed in Winter Deaths
Seasonal influenza drives substantial excess mortality, yet its contribution is often obscured when infections go undiagnosed near the time of death. Many deaths occur outside hospitals or in older adults... Read moreMicrobiology
view channel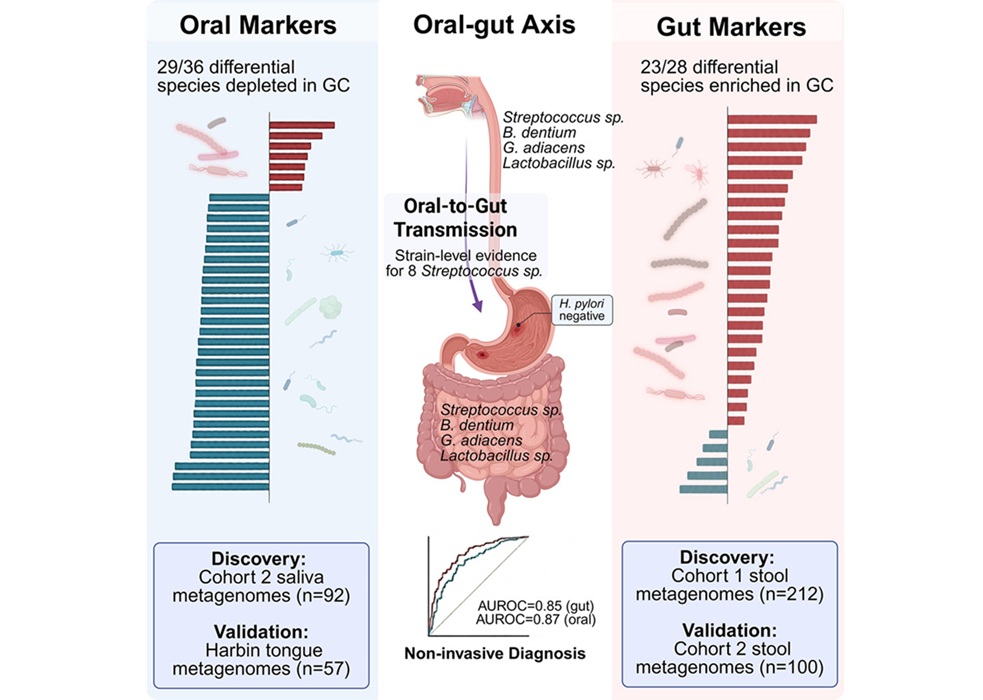
Oral–Gut Microbiome Signatures Identify Early Gastric Cancer
Early detection of gastric cancer could be advanced by scalable screening strategies using minimally invasive sampling. Saliva collection is noninvasive and cost-effective, supporting wider adoption... Read more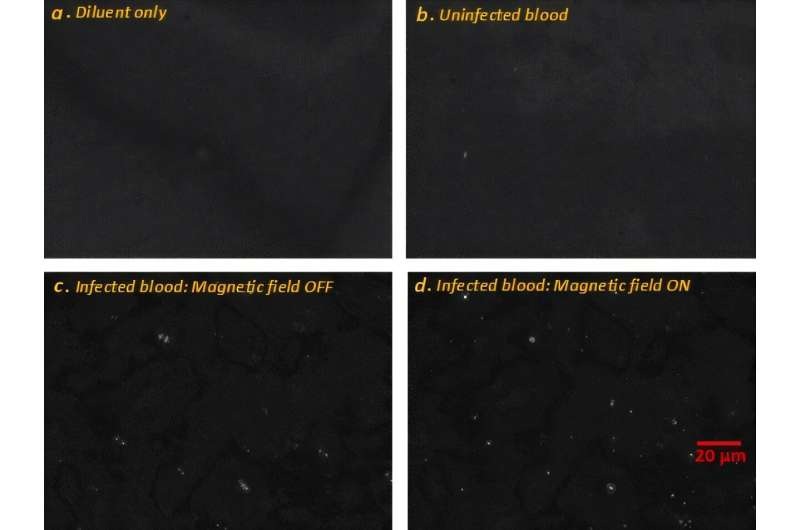
Label-Free Microscopy Methodd Enables Faster, Quantitative Detection of Malaria
Microscopy of blood smears remains a cornerstone for malaria diagnosis but can be slow, stain-dependent, and operator intensive. With more than 200 million infections and over 600,000 deaths annually,... Read more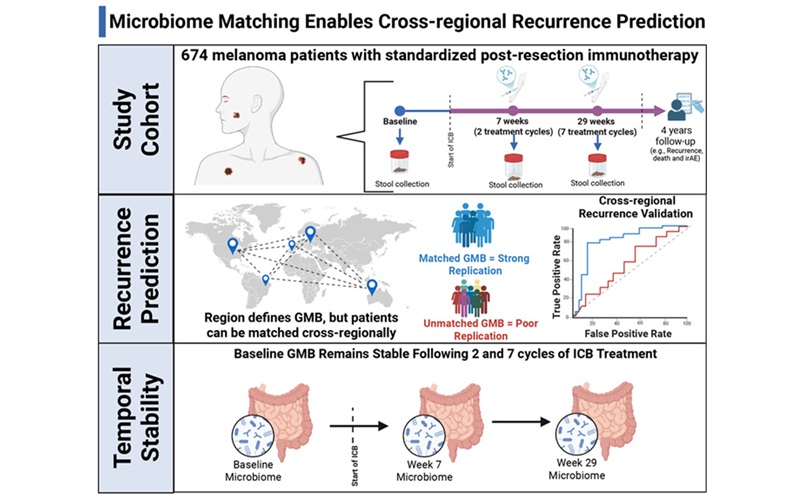
Gut Microbiome Test Predicts Melanoma Recurrence After Surgery
Melanoma remains prone to relapse even after surgery and adjuvant immunotherapy, with 25% to 40% of patients experiencing recurrence. Clinicians lack reliable pre-treatment indicators to identify those... Read more
Rapid Blood-Culture Susceptibility Panel Expands Coverage for Gram-Negative Infections
Gram-negative bloodstream infections and sepsis demand fast, precise antimicrobial therapy, yet conventional susceptibility workflows can delay targeted treatment. Clinical laboratories need platforms... Read morePathology
view channel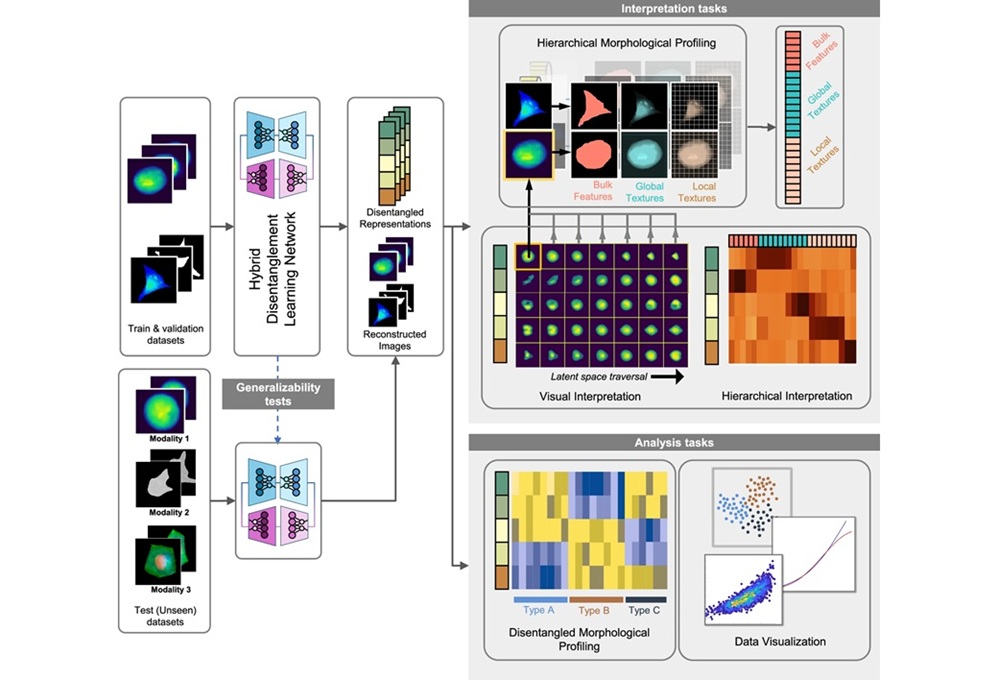
Interpretable AI Reveals Hidden Cellular Features from Microscopy Images
Microscopy images contain rich clues about cell health, but many disease-relevant morphological differences are too subtle to see and difficult to quantify consistently. Artificial intelligence (AI) has... Read more
Tumor Immune Structure Predicts Response to Immunotherapy in Melanoma
Many patients with advanced melanoma start on anti-PD-1 immunotherapy, but responses can wane or never develop. Clinicians often turn to anti-CTLA-4 after resistance emerges, yet predicting who will respond... Read moreTechnology
view channel
AI Tool Predicts Non-Response to Targeted Therapy in Colorectal Cancer
Advanced bowel cancer remains difficult to treat, and many patients receive targeted therapies that do not help them but still cause harm. Clinicians need reliable ways to identify likely responders before... Read more
Integrated System Streamlines Pre-Analytical Workflow for Molecular Testing
Pre-analytical variation remains a leading source of inconsistent molecular test results and added costs, particularly when laboratories rely on multiple instruments and protocols. Standardizing nucleic... Read moreIndustry
view channel
QuidelOrtho Adds Ultra-Fast PCR Platform with LEX Acquisition
QuidelOrtho Corporation has completed the acquisition of LEX Diagnostics for approximately USD 100 million in cash. The transaction adds the LEX VELO System to QuidelOrtho’s portfolio. The platform received U.... Read more
Seegene Showcases Real-Time PCR Data Analytics Platform at ESCMID
Seegene introduced STAgora, a real-time data analytics platform built on aggregated statistical testing data, at ESCMID Global 2026 in Munich, where it also presented an enhanced model of its automated... Read more
Roche Affiliate Expands MRD Portfolio with SAGA Acquisition
Foundation Medicine, Inc., an independent affiliate of Roche, announced plans to expand its monitoring portfolio with SAGA Diagnostics’ Pathlight, a personalized, tumor-informed molecular residual disease... Read more






.jpg)