High-Value Practice Reduces Wasteful Blood Transfusions
|
By LabMedica International staff writers Posted on 05 Dec 2017 |
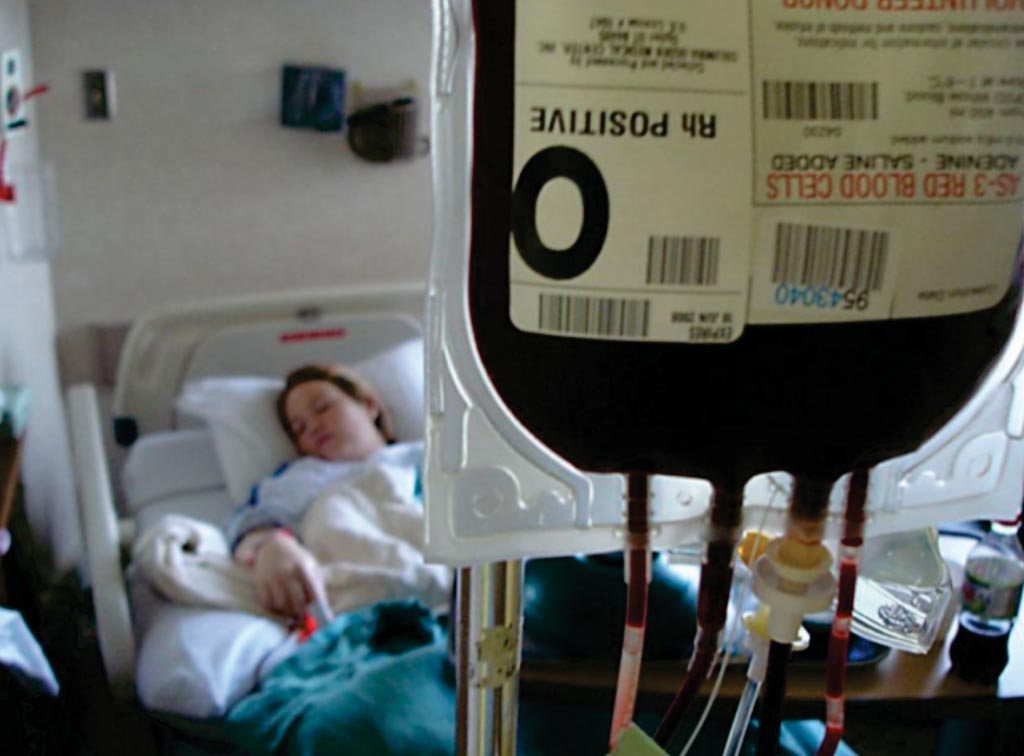
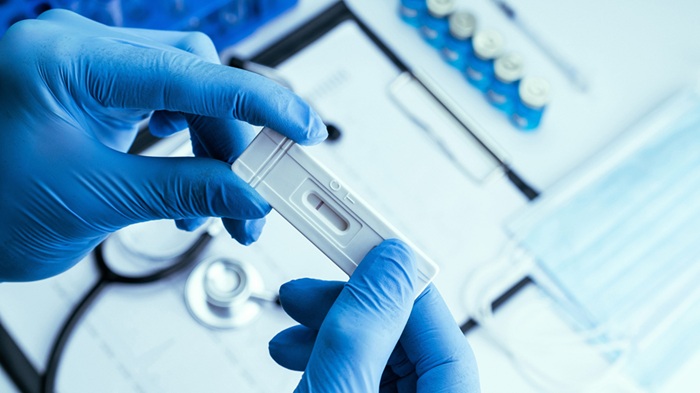
Image: A hospitalized patient receiving a blood transfusion (Photo courtesy of the US National Institute of Health).
Although blood transfusion is a lifesaving therapy for some patients, transfusion has been named one of the top five overused procedures in hospitals in the USA.
As unnecessary transfusions only increase risk and cost without providing benefit, improving transfusion practice is an effective way of promoting high-value care. Most high-quality clinical trials supporting a restrictive transfusion strategy have been published in the past five to 10 years, so the value of a successful patient blood management program has only recently been recognized.
Experts at the Johns Hopkins Medical Institutions (Baltimore, MD, USA) and their colleagues analyzed data from randomized clinical trials comparing blood transfusion approaches and endorse recommendations for blood transfusions that reduce blood use to improve patient safety and outcomes. The clinical trials that were examined compared so-called liberal versus restrictive blood transfusions. Liberal transfusions are those given to patients with hemoglobin values of 9 to 10 g/dL, of blood volume, while restrictive transfusions are those given to patients with 7 to 8 g/dL. Many of the clinical trials examined by this team used the number of patients who died within a 30- to 90-day window post-transfusion as a measure of patient outcome.
Of the more than 8,000 patients included in eight clinical trials that were reviewed, there was no difference in mortality between liberal or restrictive transfusions. One clinical trial found an increased mortality associated with liberal transfusion, and occurrence of blood clots was increased in the liberal cohort in a study that involved traumatic brain injury patients. The team also found that the largest randomized trials reduced the amount of blood used by 40% to 65%. Earlier this year, the results of a four-year project to implement a blood management program across the Johns Hopkins Health System, reducing blood use by 20% and saving more than USD 2 million on costs over a year.
Stable adult patients, including critically ill patients, with hemoglobin levels of 7 g/dL or higher should not be transfused. Patients undergoing orthopedic or cardiac surgery, or patients with underlying heart disease with hemoglobin levels of 8 g/dL or higher should not be transfused. Patients who are stable and not actively bleeding should be transfused with a single unit of blood and then reassessed.
Steven M. Frank, MD, professor of anesthesiology and the lead investigator, said, “In summary, there is no benefit in transfusing more blood than necessary and some clinical trials actually show harm to patients. All this does is increase risks and cost without adding benefit.” The study was published on November 20, 2017, in the journal JAMA Internal Medicine.
Related Links:
Johns Hopkins Medical Institutions
As unnecessary transfusions only increase risk and cost without providing benefit, improving transfusion practice is an effective way of promoting high-value care. Most high-quality clinical trials supporting a restrictive transfusion strategy have been published in the past five to 10 years, so the value of a successful patient blood management program has only recently been recognized.
Experts at the Johns Hopkins Medical Institutions (Baltimore, MD, USA) and their colleagues analyzed data from randomized clinical trials comparing blood transfusion approaches and endorse recommendations for blood transfusions that reduce blood use to improve patient safety and outcomes. The clinical trials that were examined compared so-called liberal versus restrictive blood transfusions. Liberal transfusions are those given to patients with hemoglobin values of 9 to 10 g/dL, of blood volume, while restrictive transfusions are those given to patients with 7 to 8 g/dL. Many of the clinical trials examined by this team used the number of patients who died within a 30- to 90-day window post-transfusion as a measure of patient outcome.
Of the more than 8,000 patients included in eight clinical trials that were reviewed, there was no difference in mortality between liberal or restrictive transfusions. One clinical trial found an increased mortality associated with liberal transfusion, and occurrence of blood clots was increased in the liberal cohort in a study that involved traumatic brain injury patients. The team also found that the largest randomized trials reduced the amount of blood used by 40% to 65%. Earlier this year, the results of a four-year project to implement a blood management program across the Johns Hopkins Health System, reducing blood use by 20% and saving more than USD 2 million on costs over a year.
Stable adult patients, including critically ill patients, with hemoglobin levels of 7 g/dL or higher should not be transfused. Patients undergoing orthopedic or cardiac surgery, or patients with underlying heart disease with hemoglobin levels of 8 g/dL or higher should not be transfused. Patients who are stable and not actively bleeding should be transfused with a single unit of blood and then reassessed.
Steven M. Frank, MD, professor of anesthesiology and the lead investigator, said, “In summary, there is no benefit in transfusing more blood than necessary and some clinical trials actually show harm to patients. All this does is increase risks and cost without adding benefit.” The study was published on November 20, 2017, in the journal JAMA Internal Medicine.
Related Links:
Johns Hopkins Medical Institutions
Latest Hematology News
- Rapid Cartridge-Based Test Aims to Expand Access to Hemoglobin Disorder Diagnosis
- New Guidelines Aim to Improve AL Amyloidosis Diagnosis
- Automated Hemostasis System Helps Labs of All Sizes Optimize Workflow
- Fast and Easy Test Could Revolutionize Blood Transfusions
- High-Sensitivity Blood Test Improves Assessment of Clotting Risk in Heart Disease Patients
- AI Algorithm Effectively Distinguishes Alpha Thalassemia Subtypes
- MRD Tests Could Predict Survival in Leukemia Patients
- Platelet Activity Blood Test in Middle Age Could Identify Early Alzheimer’s Risk
- Microvesicles Measurement Could Detect Vascular Injury in Sickle Cell Disease Patients
- ADLM’s New Coagulation Testing Guidance to Improve Care for Patients on Blood Thinners
- Viscoelastic Testing Could Improve Treatment of Maternal Hemorrhage
- Pioneering Model Measures Radiation Exposure in Blood for Precise Cancer Treatments
- Platelets Could Improve Early and Minimally Invasive Detection of Cancer
- Portable and Disposable Device Obtains Platelet-Rich Plasma Without Complex Equipment
- Disposable Cartridge-Based Test Delivers Rapid and Accurate CBC Results
- First Point-of-Care Heparin Monitoring Test Provides Results in Under 15 Minutes

Channels
Clinical Chemistry
view channel
Blood Test Tracks Transplant Health Using Donor DNA
Organ transplantation offers life-saving treatment for patients with end-stage disease, but complications such as rejection remain a constant risk. Monitoring transplanted organs typically relies on invasive... Read more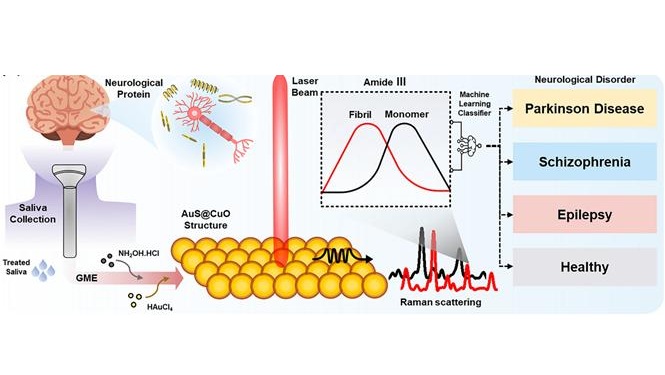
AI Sensor Detects Neurological Disorders Using Single Saliva Drop
Neurological disorders such as Parkinson’s disease and Alzheimer’s disease often develop gradually and present subtle symptoms in their early stages. Because early signs are frequently vague or atypical,... Read moreMolecular Diagnostics
view channel
Blood Test Predicts Dementia in Women 25 Years Before Symptoms Begin
Dementia and Alzheimer’s disease often develop silently over many years before symptoms appear. Detecting risk earlier could allow preventive strategies to begin long before memory problems interfere with... Read more
Serial Liquid Biopsies Reveal Therapy Resistance in Metastatic Prostate Cancer
Metastatic Prostate cancer can rapidly adapt under treatment, making it difficult to detect resistance before clinical progression. Genomic results from archival tumor tissue may no longer reflect the... Read moreImmunology
view channel
Cancer Mutation ‘Fingerprints’ to Improve Prediction of Immunotherapy Response
Cancer cells accumulate thousands of genetic mutations, but not all mutations affect tumors in the same way. Some make cancer cells more visible to the immune system, while others allow tumors to evade... Read more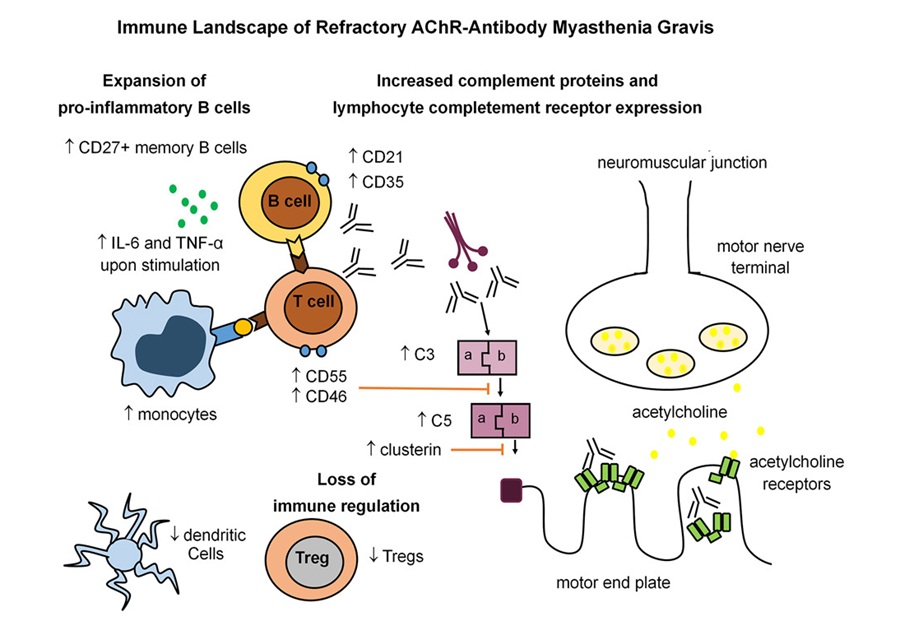
Immune Signature Identified in Treatment-Resistant Myasthenia Gravis
Myasthenia gravis is a rare autoimmune disorder in which immune attack at the neuromuscular junction causes fluctuating weakness that can impair vision, movement, speech, swallowing, and breathing.... Read more
New Biomarker Predicts Chemotherapy Response in Triple-Negative Breast Cancer
Triple-negative breast cancer is an aggressive form of breast cancer in which patients often show widely varying responses to chemotherapy. Predicting who will benefit from treatment remains challenging,... Read moreBlood Test Identifies Lung Cancer Patients Who Can Benefit from Immunotherapy Drug
Small cell lung cancer (SCLC) is an aggressive disease with limited treatment options, and even newly approved immunotherapies do not benefit all patients. While immunotherapy can extend survival for some,... Read moreMicrobiology
view channel
Study Highlights Accuracy Gaps in Consumer Gut Microbiome Kits
Direct-to-consumer gut microbiome kits promise personalized insights by profiling fecal bacteria and generating health readouts, but their analytical accuracy remains uncertain. A new study shows that... Read more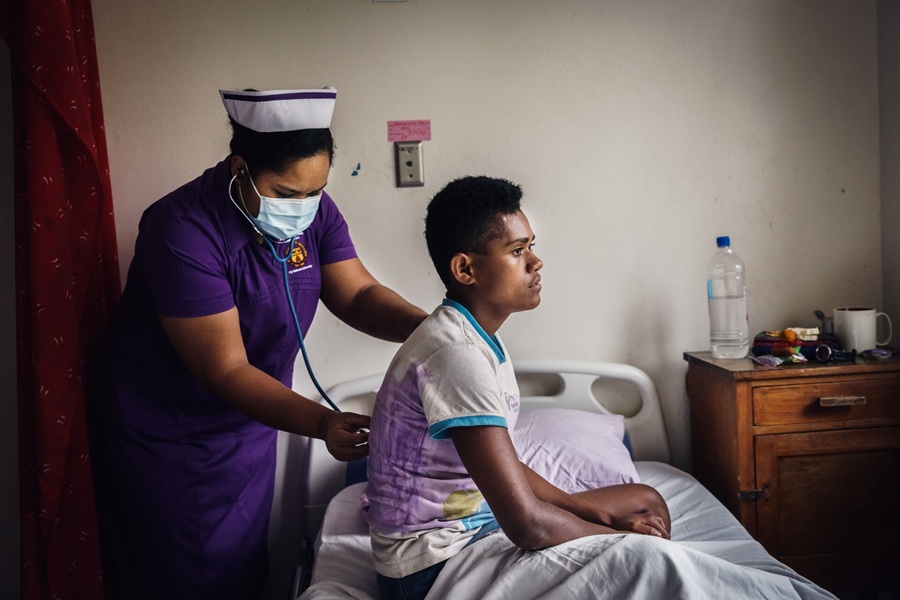
WHO Recommends Near POC Tests, Tongue Swabs and Sputum Pooling for TB Diagnosis
Tuberculosis (TB) remains one of the world’s leading infectious disease killers, yet millions of cases go undiagnosed or are detected too late. Barriers such as reliance on sputum samples, limited laboratory... Read morePathology
view channel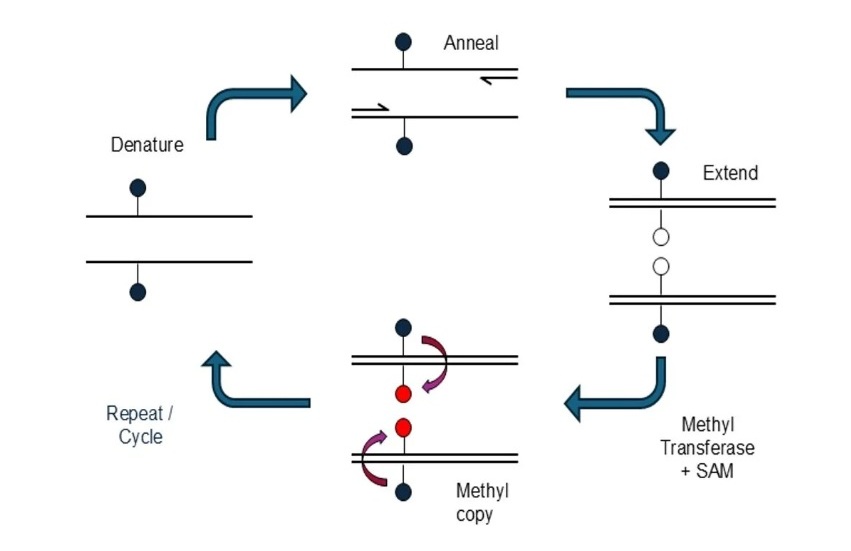
Novel mcPCR Technology to Transform Testing of Clinical Samples
DNA methylation is an important biological marker used in the diagnosis and monitoring of many diseases, including cancer. These chemical modifications to DNA influence gene activity and can reveal early... Read more
Sex Differences in Alzheimer’s Biomarkers Linked to Faster Cognitive Decline
Sex differences in Alzheimer’s disease present ongoing diagnostic challenges, with women often experiencing a disproportionate disease burden even when preclinical amyloid-beta levels are similar to men.... Read moreTechnology
view channel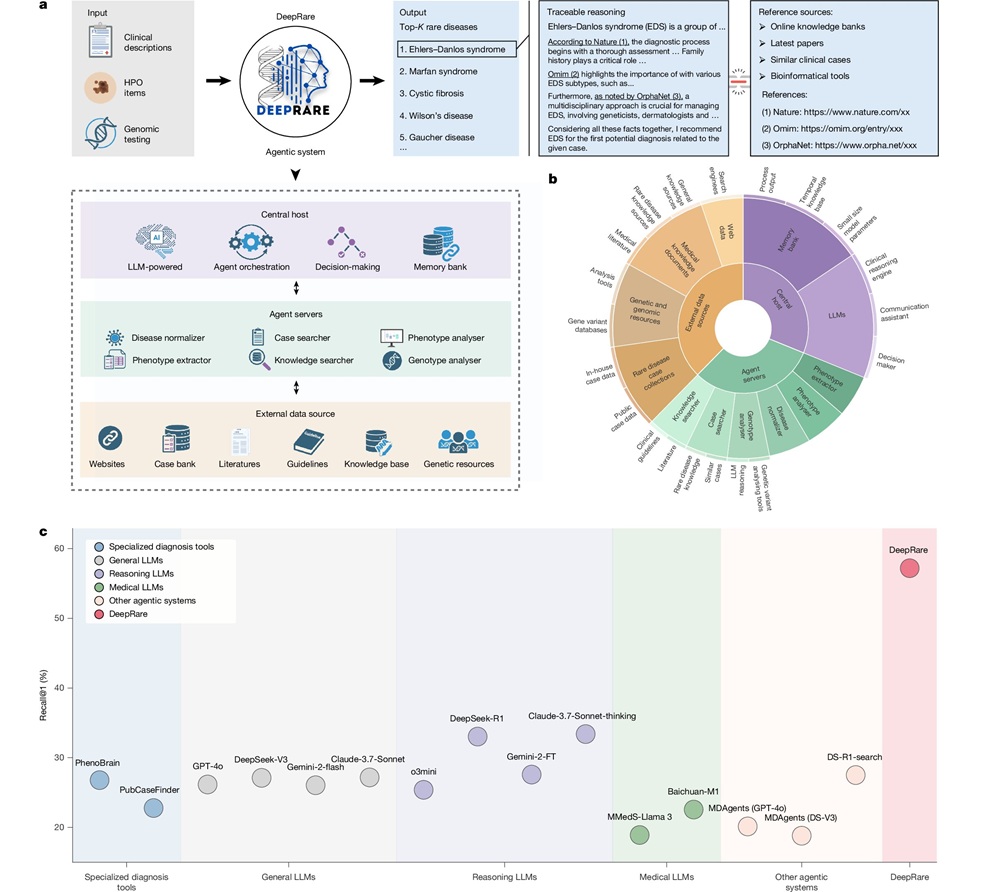
AI Model Outperforms Clinicians in Rare Disease Detection
Rare diseases affect an estimated 300 million people worldwide, yet diagnosis is often protracted and error-prone. Many conditions present with heterogeneous signs that overlap with common disorders, leading... Read more
AI-Driven Diagnostic Demonstrates High Accuracy in Detecting Periprosthetic Joint Infection
Periprosthetic joint infection (PJI) is a rare but serious complication affecting 1% to 2% of primary joint replacement surgeries. The condition occurs when bacteria or fungi infect tissues around an implanted... Read moreIndustry
view channel
MGI Tech Strengthens Sequencing Portfolio with Dual Acquisition
MGI Tech Co., Ltd. (Shenzhen, China) announced the acquisition of STOmics and CycloneSEQ on March 3, 2026, as part of its “SEQALL+GLI+Omics” strategy. According to the company, the combined portfolio spans... Read more
Agilent Technologies Acquires Pathology Diagnostics Company Biocare Medical
Agilent Technologies (Santa Clara, CA, USA) has entered into a definitive agreement to acquire Biocare Medical (Pacheco, CA, USA), expanding its pathology portfolio through the addition of highly complementary... Read more