Gene Expression Correlates with Lymphocyte Infiltration in Breast Cancer
|
By LabMedica International staff writers Posted on 30 Dec 2014 |
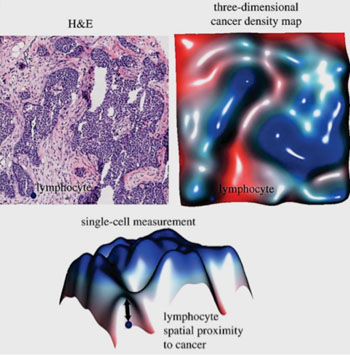
Image: A histology slide stained with hematoxylin and eosin (H&E) and the corresponding three-dimensional cancer density map, which facilitate the measurement of spatial proximity to cancer for every single lymphocyte in the image (Photo courtesy of The Institute of Cancer Research).
Lymphocytic infiltration is associated with a favorable prognosis and predicts response to chemotherapy in many cancer types, including the aggressive triple-negative breast cancer (TNBC).
A novel high-tech system has been developed for measuring the body's immune response to cancer as a way of assessing how rapidly the disease is likely to progress. The system combines computerized imaging of tumor samples with statistical analysis, and is the first objective method to measure the interaction between a patient's immune system and their tumor.
Scientist at The Institute of Cancer Research (London, UK) analyzed 181 samples from women with triple-negative breast cancer. On average, three tumor sections were obtained from different locations of each primary tumor and placed onto the same slide. Tumor materials sandwiched between these sections were sectioned, mixed and used for molecular profiling, thereby maximizing the biological relevance of multiple data types being generated.
The team developed a system, which split lymphocytes into three classes depending on their location within the tumor, and calculated how many of each type were present in each sample, and how many cancer cells were present. Immune infiltration was scored for 112 of the 181 samples by the pathologists into three categories: absent, mild and severe: absent if there were no lymphocytes, mild if there was a light scattering of lymphocytes and severe if there was a prominent lymphocytic infiltrate. Gene expression data were profiled using the human linkage-12 genotyping beadchip (HT-12) platform (Illumina; San Diego, CA, USA).
Women with fewer than around eleven intra-tumor lymphocytes per 1,000 cancer cells had an average five-year survival rate of 49%, compared with an average of 80% in triple-negative breast cancer as a whole. They also found a correlation between immune infiltration of tumors and increased levels of a protein called cytotoxic T-lymphocyte-associated protein 4, (CTLA4) or cluster of differentiation 152 (CD152), suggesting it could be a potential treatment target in this breast cancer type.
Yinyin Yuan, PhD, the team leader of the study, said, “Our test combines imaging technology with computerized analysis of large amounts of data from tumor samples, which typically contain more than 100,000 cells. We found the technique could accurately identify high-risk tumors that were evading the body's immune system in this type of breast cancer, and hope it can be adapted and added to doctors' arsenal against a variety of cancers.” The study was published on December 10, 2014, in the Journal of The Royal Society Interface.
Related Links:
The Institute of Cancer Research
Illumina
A novel high-tech system has been developed for measuring the body's immune response to cancer as a way of assessing how rapidly the disease is likely to progress. The system combines computerized imaging of tumor samples with statistical analysis, and is the first objective method to measure the interaction between a patient's immune system and their tumor.
Scientist at The Institute of Cancer Research (London, UK) analyzed 181 samples from women with triple-negative breast cancer. On average, three tumor sections were obtained from different locations of each primary tumor and placed onto the same slide. Tumor materials sandwiched between these sections were sectioned, mixed and used for molecular profiling, thereby maximizing the biological relevance of multiple data types being generated.
The team developed a system, which split lymphocytes into three classes depending on their location within the tumor, and calculated how many of each type were present in each sample, and how many cancer cells were present. Immune infiltration was scored for 112 of the 181 samples by the pathologists into three categories: absent, mild and severe: absent if there were no lymphocytes, mild if there was a light scattering of lymphocytes and severe if there was a prominent lymphocytic infiltrate. Gene expression data were profiled using the human linkage-12 genotyping beadchip (HT-12) platform (Illumina; San Diego, CA, USA).
Women with fewer than around eleven intra-tumor lymphocytes per 1,000 cancer cells had an average five-year survival rate of 49%, compared with an average of 80% in triple-negative breast cancer as a whole. They also found a correlation between immune infiltration of tumors and increased levels of a protein called cytotoxic T-lymphocyte-associated protein 4, (CTLA4) or cluster of differentiation 152 (CD152), suggesting it could be a potential treatment target in this breast cancer type.
Yinyin Yuan, PhD, the team leader of the study, said, “Our test combines imaging technology with computerized analysis of large amounts of data from tumor samples, which typically contain more than 100,000 cells. We found the technique could accurately identify high-risk tumors that were evading the body's immune system in this type of breast cancer, and hope it can be adapted and added to doctors' arsenal against a variety of cancers.” The study was published on December 10, 2014, in the Journal of The Royal Society Interface.
Related Links:
The Institute of Cancer Research
Illumina
Latest Molecular Diagnostics News
- Blood-Based Epigenetic Signals Enable Osteosarcoma Disease Monitoring
- Host–Virus Genetic Interactions Drive Nasopharyngeal Cancer Risk
- AI-Enabled Biochip Detects microRNA Biomarkers in Minutes
- Blood Test Detects Early Pancreatic Cancer in High-Risk Patients
- Long-Read RNA Sequencing Platform Improves Rare Disease Diagnosis
- Study Confirms Barrett’s Esophagus as Precursor to Esophageal Cancer
- Ultrasensitive Assay Reveals Previously Undetected Tuberculosis in Hospital Patients
- CE-Marked Blood Test Enables Monitoring of Neuroinflammation in Multiple Sclerosis
- Urine-Based Assay Predicts Severe Dengue Risk Early
- Ultrasensitive Assay Tracks Resistance Mutations MRD Monitoring
- FDA Clears At-Home HPV Test with Extended Genotyping for Cervical Screening
- Extracellular Vesicle RNA Biomarkers Enable Noninvasive IBD Diagnosis and Monitoring
- New Gene Signature Reveals Underdiagnosed Lung Cancer Subtype
- Genome Sequencing Identifies Noncoding Variants Causing Neonatal Diabetes
- Genetic Markers Predict GLP-1 Weight-Loss Response and Side Effects
- Noninvasive Urine Test Predicts Recurrence After BCG in Bladder Cancer
Channels
Clinical Chemistry
view channel
Blood Test Predicts Alzheimer Disease Risk Before Imaging Changes and Symptoms
Alzheimer's disease often advances silently for years, making timely risk stratification difficult in routine practice. Current approaches to detect pathology can involve lumbar puncture or positron emission... Read more
Study Finds ApoB Testing More Effective Than LDL for Guiding Lipid Therapy
Routine blood tests that measure low-density lipoprotein (LDL), commonly known as “bad” cholesterol, are widely used to guide lipid-lowering therapy, but they do not always provide a complete picture of... Read more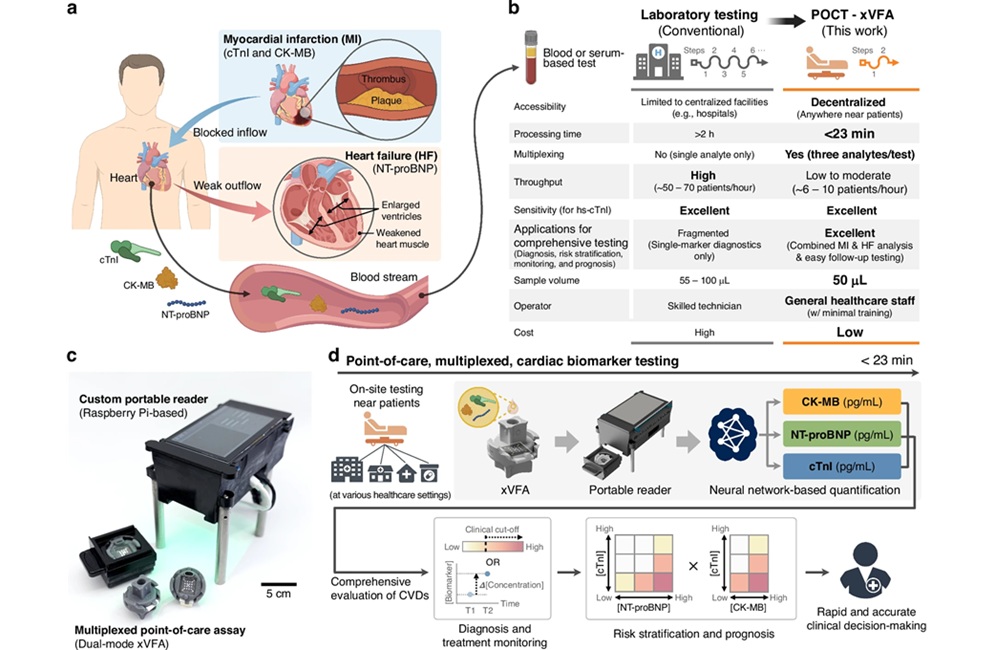
AI-Enabled POC Test Quantifies Multiple Cardiac Biomarkers
Cardiovascular diseases are a leading cause of death, responsible for nearly 20 million deaths each year. Timely triage of myocardial infarction and heart failure hinges on rapid cardiac biomarker measurement,... Read moreNext Generation Automated Analyzers Increase Throughput for Clinical Chemistry and Electrolyte Testing
Clinical laboratories continue to face staffing shortages, limited space, and growing test volumes that pressure chemistry and electrolyte workflows. Maintaining rapid turnaround times increasingly depends... Read moreMolecular Diagnostics
view channel
Blood-Based Epigenetic Signals Enable Osteosarcoma Disease Monitoring
Osteosarcoma is a rare but aggressive pediatric bone cancer where recurrence and metastasis remain difficult to detect early. Imaging-based surveillance can miss small lesions and exposes children to repeated... Read more
Host–Virus Genetic Interactions Drive Nasopharyngeal Cancer Risk
Epstein–Barr virus (EBV) infects more than 95% of adults worldwide, yet only a small fraction develops EBV‑associated cancers such as nasopharyngeal carcinoma. Explaining this divergence requires understanding... Read moreHematology
view channel
Routine Blood Test Parameters Link Anemia to Cancer Risk and Mortality
Anemia detected in routine care can signal underlying pathology and is frequently encountered in adults. Because it is defined by hemoglobin levels below the normal range, it is often evaluated with red... Read more
Prognostic Tool Guides Personalized Treatment in Rare Blood Cancer
Chronic myelomonocytic leukemia (CMML) is a rare blood cancer in which acquired genetic mutations in bone marrow stem cells drive disease. Stem cell transplantation is the only curative option but carries... Read moreImmunology
view channel
Study Finds Influenza Often Undiagnosed in Winter Deaths
Seasonal influenza drives substantial excess mortality, yet its contribution is often obscured when infections go undiagnosed near the time of death. Many deaths occur outside hospitals or in older adults... Read moreCombined Screening Approach Identifies Early Leprosy Cases
Leprosy remains a significant public health concern, with more than 200,000 new cases reported globally each year and early disease often escaping routine laboratory detection. In its initial phase, bacterial... Read moreMicrobiology
view channel
Rapid Color Test Stratifies Virulent and Resistant Staph Strains
Staphylococcus aureus (golden staph) remains a leading cause of infection-related mortality worldwide, responsible for more than a million deaths each year. Rapidly distinguishing highly virulent or a... Read more
Syndromic Panel Enables Rapid Identification of Bloodstream Infections
Bloodstream infections require rapid identification of causative pathogens and resistance determinants to guide therapy, yet laboratories often face pressure to deliver clinically relevant results quickly... Read more
RNA-Based Workflow Identifies Active Skin Microbes for Dermatology Research
Human skin carries diverse microbial communities that influence barrier function and inflammation, yet identifying which organisms are metabolically active has been challenging. DNA-based surveys catalog... Read more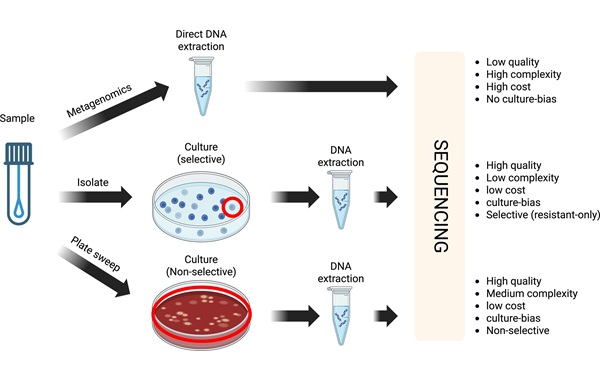
Cost-Effective Sampling and Sequencing Workflow Identifies ICU Infection Hotspots
Intensive care units face persistent threats from hospital-acquired infections, increasingly driven by drug-resistant bacteria. Rapidly pinpointing environmental reservoirs and transmission hotspots remains... Read moreTechnology
view channel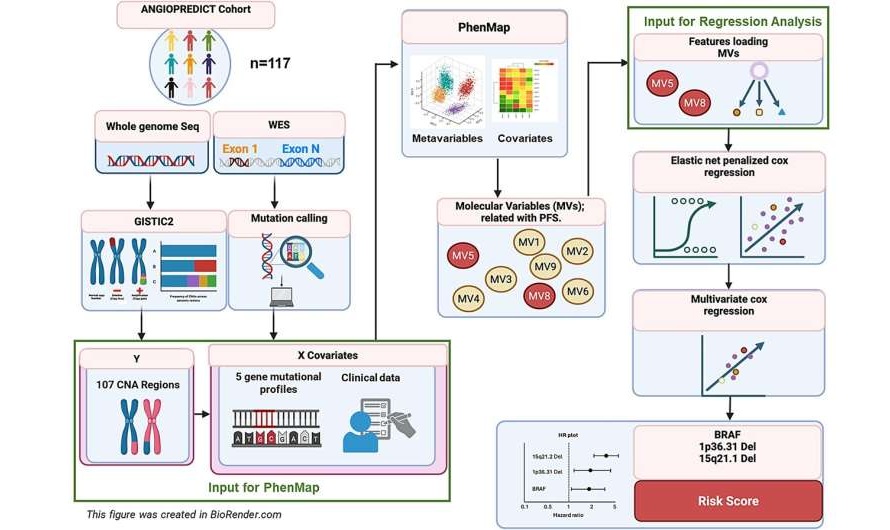
AI Tool Predicts Non-Response to Targeted Therapy in Colorectal Cancer
Advanced bowel cancer remains difficult to treat, and many patients receive targeted therapies that do not help them but still cause harm. Clinicians need reliable ways to identify likely responders before... Read more
Integrated System Streamlines Pre-Analytical Workflow for Molecular Testing
Pre-analytical variation remains a leading source of inconsistent molecular test results and added costs, particularly when laboratories rely on multiple instruments and protocols. Standardizing nucleic... Read moreIndustry
view channel
Partnership Expands Ultrasensitive WGS Assay for for Hematologic Malignancies and MRD Monitoring
Tempus AI and Predicta Biosciences announced the commercial expansion of a co-branded whole‑genome sequencing assay GenoPredicta, which is intended for comprehensive genomic characterization of hematologic... Read more