Combined Biopsy Method Improves Prostate Cancer Diagnosis
By LabMedica International staff writers
Posted on 16 Mar 2020
Prostate cancer can vary widely in severity and its potential to spread. Low-grade prostate cancer is associated with a very low risk of cancer-specific death and often does not require treatment, whereas high-grade cancers are much more likely to spread and are responsible for most prostate cancer deaths. This makes the correct assessment of the cancer grade very important for treatment decisions.Posted on 16 Mar 2020
Unlike biopsies for most other types of cancer, which target abnormalities found by imaging, systematic biopsy uses a non-targeted method of taking systematically spaced samples across the prostate gland to find a cancer. Because this method can potentially miss areas of cancer, doctors may then over treat a patient with low-grade disease, fearing there is high-grade disease they missed.
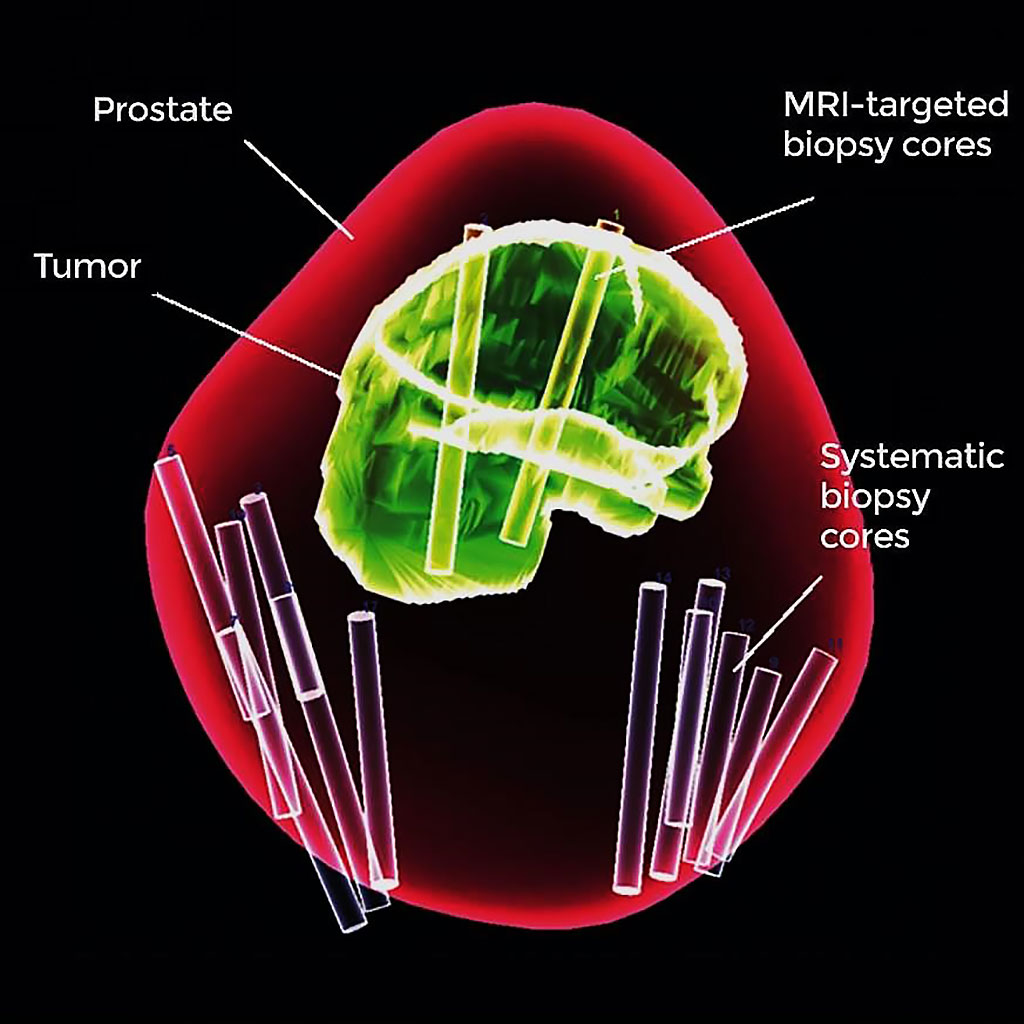
Image: Testing with combined biopsy method improves prostate cancer diagnosis (Photo courtesy of the National Institutes of Health Clinical Center).
A team of medical scientists collaborating with the National Institutes of Health Clinical Center (Bethesda MD, USA) studied 2,103 men who had magnetic resonance imaging (MRI)-visible lesions underwent both MRI-targeted and systematic biopsies. Of these men, 1,312 were diagnosed with cancer and 404 underwent prostatectomy, a full removal of the prostate. By comparing diagnoses from systematic biopsy alone to systematic biopsy plus MRI-targeted biopsy, the team found that adding MRI-targeted biopsy to systematic biopsy led to 208 more cancer diagnoses than systematic biopsy alone. The addition of MRI-targeted biopsy also led to 458 upgrades, or changes in diagnosis to a more aggressive cancer, based on analysis of the biopsy tissue by histopathology.
The team also determined that combined biopsy provided more accurate diagnosis than MRI-targeted biopsies alone. Among the men who underwent prostatectomy, they found that systematic biopsy alone underdiagnosed about 40% and MRI-targeted biopsy alone underdiagnosed about 30% of the cancers, while combined biopsy underdiagnosed 14.4% of the cancers. In addition, while systematic biopsy underdiagnosed 16.8% and MRI-targeted biopsy underdiagnosed 8.7% of the most aggressive cancers, combined biopsy missed only 3.5% of the most aggressive cancers.
Peter Pinto, MD, of the Urologic Oncology Branch in NCI's Center for Cancer Research and senior author of the study, said, “With the addition of MRI-targeted biopsy to systematic biopsy, we can now identify the most lethal cancers within the prostate earlier, providing patients the potential for better treatment before the cancers spread.”
The authors concluded that among patients with MRI-visible lesions, combined biopsy led to more detection of all prostate cancers. However, MRI-targeted biopsy alone underestimated the histologic grade of some tumors. After radical prostatectomy, upgrades to grade group 3 or higher on histopathological analysis were substantially lower after combined biopsy. The study was published on March 5, 2020 in the journal The New England Journal of Medicine.
Related Links:
National Institutes of Health Clinical Center