New Risk Factors Identified for Parasitic Infection
By LabMedica International staff writers
Posted on 24 Jul 2013
Recent cases of a parasitic lung infection have been analyzed and new modes of transmission and associated behaviors have identified among different groups of people at risk.Posted on 24 Jul 2013
The index of suspicion among medical professionals should be raised so nontraditional patients and those not exhibiting all symptoms, but who are at risk can be diagnosed and treated to avoid potentially life-threatening lung or brain complications.
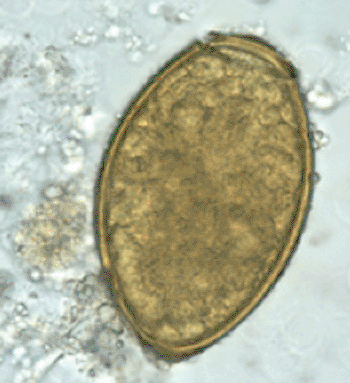
Image: Egg of Paragonimus westermani (Photo courtesy of US Center of Disease Control and Prevention).
A public health professional at the Louisiana State University Health Sciences Center (New Orleans, LA, USA) has reviewed the status of paragonimiasis in the USA, as the epidemiology of this disease has recently changed. The disease is caused by trematode worms, such as Paragonimus westermani, and P. kellicotti. Most cases of infection are reported from Asia or in those who have recently traveled to or emigrated from a region where the parasite is prevalent.
In the laboratory, the diagnosis of paragonimiasis may include the microscopic observation of unembryonated Paragonimus eggs in sputum, feces, bronchoalveolar lavage (BAL) fluid, lung or pleural biopsy specimens, or surgical pleurectomy or lobectomy specimens. A variety of more sensitive immunodiagnostic techniques are available from reference laboratories, including enzyme-linked immunosorbent assays (ELISAs) and immunoblotting developed for the detection of cross-reacting P. westermani antibodies. Some of the newest diagnostic technologies for the rapid detection of food-borne helminthiases, including paragonimiasis, are loop-mediated isothermal amplification (LAMP) assays, DNA pyrosequencing for polymerase chain reaction (PCR) amplicons, and multiplex protein microarray assays.
The parasitic infection can occur when crabs are eaten raw in sushi bars or alcohol-pickled crabs, the so-called drunken crabs, in martinis. The one indigenous Paragonimus species can transmit infection through undercooked mudbugs at a crawfish boil and through exposure while floating, paddling, canoeing, or camping on waterways and in areas where crawfish live. The incubation period can vary from two to six weeks. Although some people can remain asymptomatic for prolonged periods, this parasitic infection can produce symptoms ranging from fever, recurrent cough, and night sweats, mimicking tuberculosis, to bloody cough, pleurisy, and pneumonia. It can cause headaches, seizures, stiff neck, and loss of vision and can be fatal.
James H. Diaz, MD, DrPH, the author of the article, said, “Doctors should consider this infection in vacationers and weekenders returning from areas of the USA where the parasite is endemic and ask about raw or undercooked crawfish in all patients with unexplained fever, cough, high white blood cell count, and fluid around the lungs. Even without microscopic evidence, any patient with a positive history of raw or undercooked freshwater Asian crab or native crawfish and clinical symptoms should be evaluated and treated to prevent serious complications.” The review was published in the July 2013 issue of the journal Clinical Microbiology Reviews.
Related Links:
Louisiana State University Health Sciences Center




.jpg)