CSF Liquid Biopsy Sequencing Tracks Glioma Evolution
|
By LabMedica International staff writers Posted on 06 Feb 2019 |

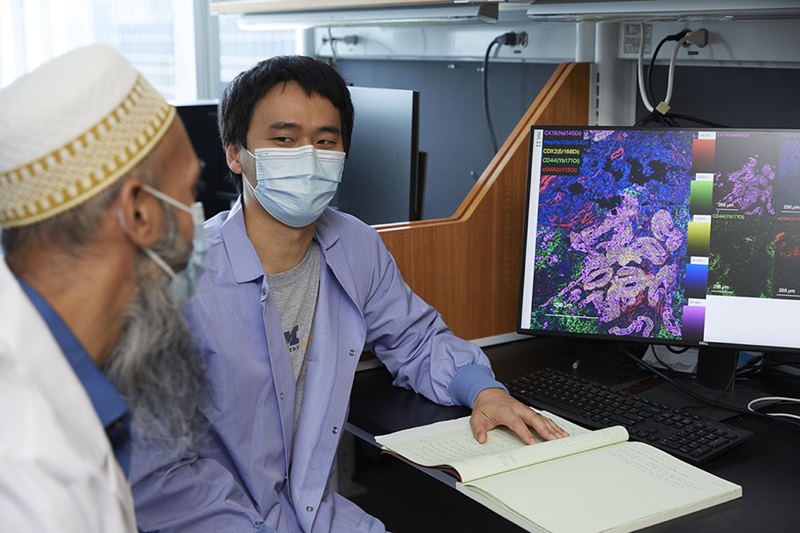
Image: Vials of cerebrospinal fluid that can be sequenced for cell-free DNA in glioma patients (Photo courtesy of James Heilman, MD).
Genetic tumor profiling of gliomas is used to classify disease and guide therapy, but involves brain surgery for tissue collection; repeated tumor biopsies may be necessary for accurate genotyping over the course of the disease.
While the detection of circulating tumor DNA (ctDNA) in the blood of patients with primary brain tumors remains challenging, sequencing of ctDNA from the cerebrospinal fluid (CSF) may provide an alternative way to genotype gliomas with lower morbidity and cost.
A large team of scientists led by the Memorial Sloan Kettering Cancer Center (New York, NY, USA) tracked traces of gliomas in CSF by collecting samples from 85 glioma patients who previously received a lumbar puncture because they showed neurological signs or symptoms of brain tumors. Patient diagnoses included 13 grade II gliomas, 26 grade II gliomas, and 54 grade IV gliomas. All patients had received treatment for glioma before CSF collection, including surgery, radiation, and at least one systemic tumor-directed chemotherapy.
After extracting 3 mL of CSF from each patient through a spinal tap, the team ran the sample on a centrifuge to separate the pellets from supernatant, which contained ctDNA. While normal CSF typically contains a low white blood cell count, the team noted that including pellets dilutes the tumor signature in a sample. The investigators used MSKCC's MSK-IMPACT next-generation sequencing assay to analyze samples for genes relevant to glioma. Afterward, the team ran the results through a bioinformatics analysis pipeline, which included a mutation-calling element that MSKCC developed with the MSK-IMPACT.
The scientists detected tumor-derived DNA in CSF from 42 out of 85 patients and found that the genetic material was linked to disease burden and adverse outcome. They also examined whether combinations of genetic alterations, lower-grade glioma signatures, that they detected in the CSF could be matched to the signature of the original tumor. Sequencing all available tumor biopsies from 36 patients who had positive CSF ctDNA, they found that CSF and tumor samples shared mutations in all 20 patients with wild type glioblastomas (GBMs) that were not hypermutated. The most common alterations in the samples included mutations in the TERT promoter, the protein coding regions of TP53, IDH1, deletions of CDKn2A and CDKN2B, amplifications of EGFR, and EGFR-variant III deletion.
Alterations that occur early during tumorigenesis, such as co-deletion of chromosome arms 1p and 19q (1p/19q codeletion) and mutations in the metabolic genes isocitrate dehydrogenase 1 (IDH1) or IDH2, were shared in all matched ctDNA-positive CSF–tumor pairs, whereas growth factor receptor signaling pathways showed considerable evolution. Michael Berger, PhD, a co-author of the study, said, “Compared to other liquid biopsy applications, cerebrospinal fluid has the potential to enable more sensitive detection of ctDNA because most of the cell-free DNA in CSF is shed from tumor cells. There is very little background DNA from non-cancerous cells, in contrast to plasma where often only a tiny fraction of the cell-free DNA is actually derived from tumor cells.” The study was published on January 23, 2019, in the journal Nature Research.
Related Links:
Memorial Sloan Kettering Cancer Center
While the detection of circulating tumor DNA (ctDNA) in the blood of patients with primary brain tumors remains challenging, sequencing of ctDNA from the cerebrospinal fluid (CSF) may provide an alternative way to genotype gliomas with lower morbidity and cost.
A large team of scientists led by the Memorial Sloan Kettering Cancer Center (New York, NY, USA) tracked traces of gliomas in CSF by collecting samples from 85 glioma patients who previously received a lumbar puncture because they showed neurological signs or symptoms of brain tumors. Patient diagnoses included 13 grade II gliomas, 26 grade II gliomas, and 54 grade IV gliomas. All patients had received treatment for glioma before CSF collection, including surgery, radiation, and at least one systemic tumor-directed chemotherapy.
After extracting 3 mL of CSF from each patient through a spinal tap, the team ran the sample on a centrifuge to separate the pellets from supernatant, which contained ctDNA. While normal CSF typically contains a low white blood cell count, the team noted that including pellets dilutes the tumor signature in a sample. The investigators used MSKCC's MSK-IMPACT next-generation sequencing assay to analyze samples for genes relevant to glioma. Afterward, the team ran the results through a bioinformatics analysis pipeline, which included a mutation-calling element that MSKCC developed with the MSK-IMPACT.
The scientists detected tumor-derived DNA in CSF from 42 out of 85 patients and found that the genetic material was linked to disease burden and adverse outcome. They also examined whether combinations of genetic alterations, lower-grade glioma signatures, that they detected in the CSF could be matched to the signature of the original tumor. Sequencing all available tumor biopsies from 36 patients who had positive CSF ctDNA, they found that CSF and tumor samples shared mutations in all 20 patients with wild type glioblastomas (GBMs) that were not hypermutated. The most common alterations in the samples included mutations in the TERT promoter, the protein coding regions of TP53, IDH1, deletions of CDKn2A and CDKN2B, amplifications of EGFR, and EGFR-variant III deletion.
Alterations that occur early during tumorigenesis, such as co-deletion of chromosome arms 1p and 19q (1p/19q codeletion) and mutations in the metabolic genes isocitrate dehydrogenase 1 (IDH1) or IDH2, were shared in all matched ctDNA-positive CSF–tumor pairs, whereas growth factor receptor signaling pathways showed considerable evolution. Michael Berger, PhD, a co-author of the study, said, “Compared to other liquid biopsy applications, cerebrospinal fluid has the potential to enable more sensitive detection of ctDNA because most of the cell-free DNA in CSF is shed from tumor cells. There is very little background DNA from non-cancerous cells, in contrast to plasma where often only a tiny fraction of the cell-free DNA is actually derived from tumor cells.” The study was published on January 23, 2019, in the journal Nature Research.
Related Links:
Memorial Sloan Kettering Cancer Center
Latest Pathology News
- AI-Powered Digital Imaging System to Revolutionize Cancer Diagnosis
- New Mycobacterium Tuberculosis Panel to Support Real-Time Surveillance and Combat Antimicrobial Resistance
- New Method Offers Sustainable Approach to Universal Metabolic Cancer Diagnosis
- Spatial Tissue Analysis Identifies Patterns Associated With Ovarian Cancer Relapse
- Unique Hand-Warming Technology Supports High-Quality Fingertip Blood Sample Collection
- Image-Based AI Shows Promise for Parasite Detection in Digitized Stool Samples
- Deep Learning Powered AI Algorithms Improve Skin Cancer Diagnostic Accuracy
- Microfluidic Device for Cancer Detection Precisely Separates Tumor Entities
- Virtual Skin Biopsy Determines Presence of Cancerous Cells
- AI Detects Viable Tumor Cells for Accurate Bone Cancer Prognoses Post Chemotherapy
- First Ever Technique Identifies Single Cancer Cells in Blood for Targeted Treatments
- Innovative Blood Collection Device Overcomes Common Obstacles Related to Phlebotomy
- Intra-Operative POC Device Distinguishes Between Benign and Malignant Ovarian Cysts within 15 Minutes
- Simple Skin Biopsy Test Detects Parkinson’s and Related Neurodegenerative Diseases
- Bioinformatics Tool to Identify Chromosomal Alterations in Tumor Cells Can Improve Cancer Diagnosis
- Coin-Sized Device Rapidly Isolates Blood Plasma for Quicker and More Precise Clinical Diagnoses
Channels
Clinical Chemistry
view channel
3D Printed Point-Of-Care Mass Spectrometer Outperforms State-Of-The-Art Models
Mass spectrometry is a precise technique for identifying the chemical components of a sample and has significant potential for monitoring chronic illness health states, such as measuring hormone levels... Read more.jpg)
POC Biomedical Test Spins Water Droplet Using Sound Waves for Cancer Detection
Exosomes, tiny cellular bioparticles carrying a specific set of proteins, lipids, and genetic materials, play a crucial role in cell communication and hold promise for non-invasive diagnostics.... Read more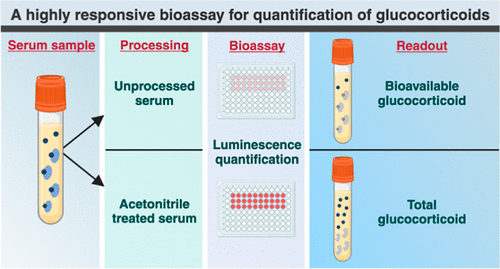
Highly Reliable Cell-Based Assay Enables Accurate Diagnosis of Endocrine Diseases
The conventional methods for measuring free cortisol, the body's stress hormone, from blood or saliva are quite demanding and require sample processing. The most common method, therefore, involves collecting... Read moreHematology
view channel
Next Generation Instrument Screens for Hemoglobin Disorders in Newborns
Hemoglobinopathies, the most widespread inherited conditions globally, affect about 7% of the population as carriers, with 2.7% of newborns being born with these conditions. The spectrum of clinical manifestations... Read more
First 4-in-1 Nucleic Acid Test for Arbovirus Screening to Reduce Risk of Transfusion-Transmitted Infections
Arboviruses represent an emerging global health threat, exacerbated by climate change and increased international travel that is facilitating their spread across new regions. Chikungunya, dengue, West... Read more
POC Finger-Prick Blood Test Determines Risk of Neutropenic Sepsis in Patients Undergoing Chemotherapy
Neutropenia, a decrease in neutrophils (a type of white blood cell crucial for fighting infections), is a frequent side effect of certain cancer treatments. This condition elevates the risk of infections,... Read more
First Affordable and Rapid Test for Beta Thalassemia Demonstrates 99% Diagnostic Accuracy
Hemoglobin disorders rank as some of the most prevalent monogenic diseases globally. Among various hemoglobin disorders, beta thalassemia, a hereditary blood disorder, affects about 1.5% of the world's... Read moreImmunology
view channel
Diagnostic Blood Test for Cellular Rejection after Organ Transplant Could Replace Surgical Biopsies
Transplanted organs constantly face the risk of being rejected by the recipient's immune system which differentiates self from non-self using T cells and B cells. T cells are commonly associated with acute... Read more
AI Tool Precisely Matches Cancer Drugs to Patients Using Information from Each Tumor Cell
Current strategies for matching cancer patients with specific treatments often depend on bulk sequencing of tumor DNA and RNA, which provides an average profile from all cells within a tumor sample.... Read more
Genetic Testing Combined With Personalized Drug Screening On Tumor Samples to Revolutionize Cancer Treatment
Cancer treatment typically adheres to a standard of care—established, statistically validated regimens that are effective for the majority of patients. However, the disease’s inherent variability means... Read moreMicrobiology
view channel
New CE-Marked Hepatitis Assays to Help Diagnose Infections Earlier
According to the World Health Organization (WHO), an estimated 354 million individuals globally are afflicted with chronic hepatitis B or C. These viruses are the leading causes of liver cirrhosis, liver... Read more
1 Hour, Direct-From-Blood Multiplex PCR Test Identifies 95% of Sepsis-Causing Pathogens
Sepsis contributes to one in every three hospital deaths in the US, and globally, septic shock carries a mortality rate of 30-40%. Diagnosing sepsis early is challenging due to its non-specific symptoms... Read morePathology
view channelAI-Powered Digital Imaging System to Revolutionize Cancer Diagnosis
The process of biopsy is important for confirming the presence of cancer. In the conventional histopathology technique, tissue is excised, sliced, stained, mounted on slides, and examined under a microscope... Read more
New Mycobacterium Tuberculosis Panel to Support Real-Time Surveillance and Combat Antimicrobial Resistance
Tuberculosis (TB), the leading cause of death from an infectious disease globally, is a contagious bacterial infection that primarily spreads through the coughing of patients with active pulmonary TB.... Read moreTechnology
view channel
New Diagnostic System Achieves PCR Testing Accuracy
While PCR tests are the gold standard of accuracy for virology testing, they come with limitations such as complexity, the need for skilled lab operators, and longer result times. They also require complex... Read more
DNA Biosensor Enables Early Diagnosis of Cervical Cancer
Molybdenum disulfide (MoS2), recognized for its potential to form two-dimensional nanosheets like graphene, is a material that's increasingly catching the eye of the scientific community.... Read more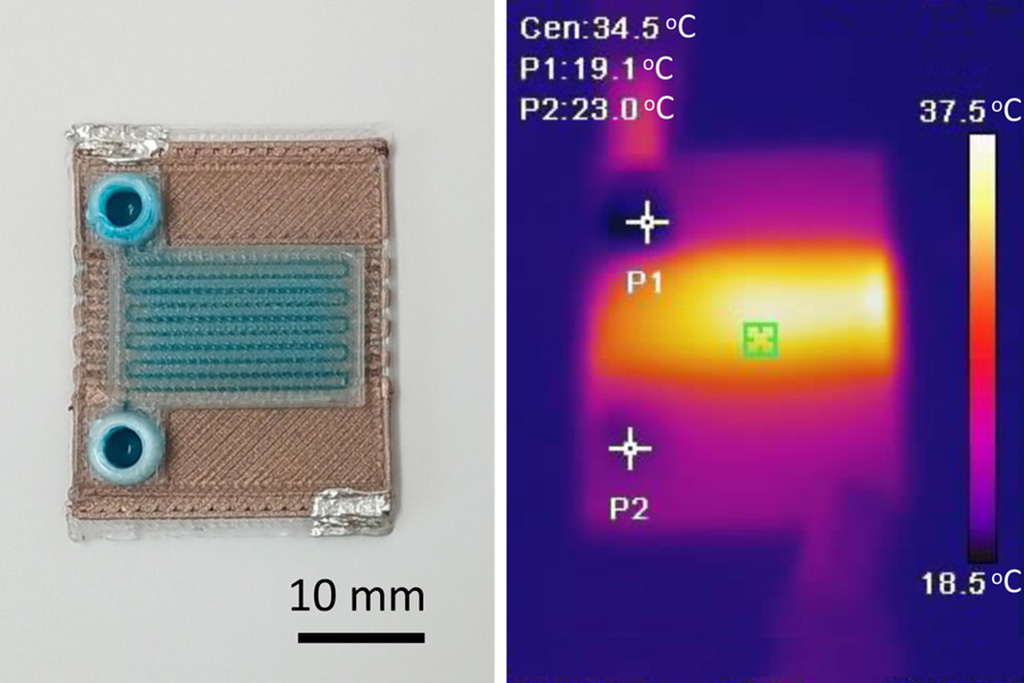
Self-Heating Microfluidic Devices Can Detect Diseases in Tiny Blood or Fluid Samples
Microfluidics, which are miniature devices that control the flow of liquids and facilitate chemical reactions, play a key role in disease detection from small samples of blood or other fluids.... Read more
Breakthrough in Diagnostic Technology Could Make On-The-Spot Testing Widely Accessible
Home testing gained significant importance during the COVID-19 pandemic, yet the availability of rapid tests is limited, and most of them can only drive one liquid across the strip, leading to continued... Read moreIndustry
view channel
ECCMID Congress Name Changes to ESCMID Global
Over the last few years, the European Society of Clinical Microbiology and Infectious Diseases (ESCMID, Basel, Switzerland) has evolved remarkably. The society is now stronger and broader than ever before... Read more
Bosch and Randox Partner to Make Strategic Investment in Vivalytic Analysis Platform
Given the presence of so many diseases, determining whether a patient is presenting the symptoms of a simple cold, the flu, or something as severe as life-threatening meningitis is usually only possible... Read more
Siemens to Close Fast Track Diagnostics Business
Siemens Healthineers (Erlangen, Germany) has announced its intention to close its Fast Track Diagnostics unit, a small collection of polymerase chain reaction (PCR) testing products that is part of the... Read more











.jpg)