Breast Cancer Risk Variant Type Determines Tumor Aggressiveness
By LabMedica International staff writers
Posted on 14 Nov 2018
Interval breast cancer is a term for tumors detected within a year after a mammographic screening that was determined to be normal and is among the measures used to gauge the efficacy of breast screening programs.Posted on 14 Nov 2018
It has been established that genetic traits contribute to both familial and sporadic breast cancer risks, but the impact of rare variants in breast cancer susceptibility loci on tumor characteristics and survival remains, to date, relatively limited.
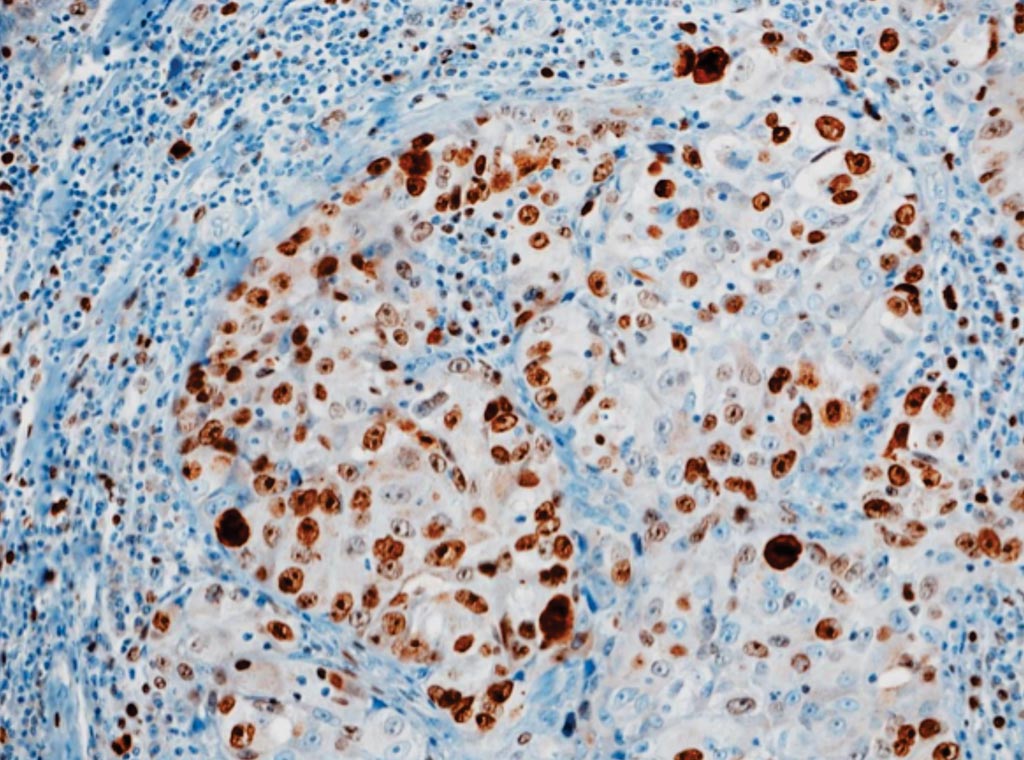
Image: Immunostaining of breast cancer; distribution pattern of the Ki67 labeling index in breast cancer values (Photo courtesy of University of Szeged).
An international team led by those at the Genome Institute of Singapore (Singapore) analyzed data that comprised from 5,099 breast cancer patients from Sweden that passed quality control. The team then analyzed genetic data from the 5,077 women who did not carry BRCA1/2 mutations with the polygenic risk score and found that a higher score was associated with less aggressive tumor phenotypes. Also, there were no significant survival differences linked to increases in polygenic risk scores.
The team also evaluated a subset of 597 women after excluding 92 patients who carried BRCA1/2 mutations, since these are known to be associated with poor prognosis, diagnosis at a younger age, estrogen receptor negativity, and basal-like subtype. HER2 status was dichotomized (positive/negative) in accordance with the Swedish Society of Pathology's guidelines: negative if protein expression showed 0 or 1+, or was higher with no confirmed gene amplification by fluorescence in situ hybridization (FISH), and positive if FISH showed gene amplification. Proliferation marker Ki67 was measured according to contemporary guidelines and reported as percent staining.
The 597 women all carried a rare protein-truncating variant. These women were younger, had more aggressive tumor characteristics, and were at 1.65 times greater risk of dying from breast cancer compared to those who did not have these variants. Women with low breast density who carried protein-truncating mutations in non-BRCA1/2 genes still had a 1.89 times increased risk compared to non-carriers. However, patients with low breast density and a higher polygenic risk score were at 23% lower risk for developing interval breast cancer.
One reason that higher polygenic risk scores in this study were associated with less aggressive disease, which is likely to be detected during routine screening, may be due to the way the algorithm was developed. The authors noted that many of the 172 known SNPs associated with breast cancer, of which they used 162 in their study, were likely identified in large breast cancer cohorts that are enriched for estrogen receptor-positive disease, which is often associated with favorable tumor features and outcomes.
Jingmei Li, PhD, an assistant professor and the lead author of the study, said, “Both rare and common variants can predict breast cancer risk. Our study shows that different variants are associated with different kinds of breast cancer, and those women carrying rare variants have a higher risk of developing interval breast cancers and have worse overall survival compared to women with common mutations.” The study was published in the November 2018 issue of the journal Cancer Research.
Related Links:
Genome Institute of Singapore






.jpg)