Inflammatory Gene Signature Links Metabolic Disease to Pancreatic Cancer Recurrence
Posted on 07 May 2026
Pancreatic ductal adenocarcinoma (PDAC) is among the deadliest cancers, with late diagnosis, limited treatment options, and frequent relapse. Obesity and type 2 diabetes are established risk factors, yet the biological links to pancreatic cancer outcomes remain unclear. Recurrence after surgery occurs in about 80% of patients, underscoring the need for better risk stratification. A new study shows that shared inflammatory genes connect pancreatic cancer with obesity and diabetes.
At the University of Birmingham, investigators used an integrative, multi-stage approach that combined large human and mouse genetic datasets, single-cell analysis of pancreatic tumors, and laboratory testing of human tissue. The study, published in Cancer Medicine, tested whether genes already tied to pancreatic cancer recurrence also behave differently in metabolic disease. The team consistently found that the same molecular signals were operative across both conditions.
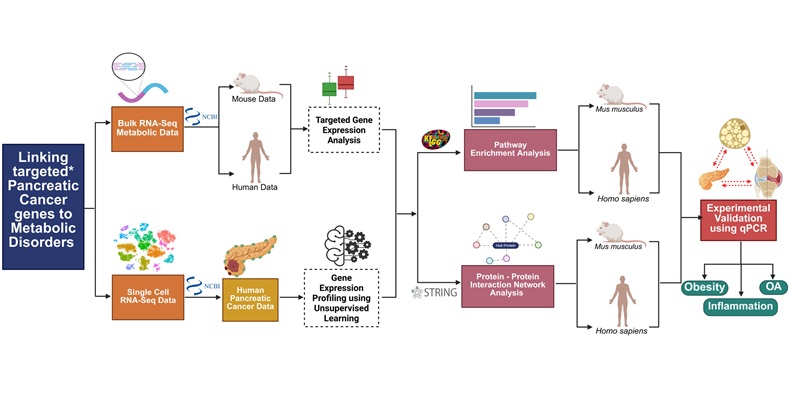
The work identified six genes—ITGAM, PECAM1, CCL5, STAT1, STAT2, and CD44—with increased activity in pancreatic cancer as well as in obesity and diabetes. These targets are involved in inflammatory and immune pathways, indicating a shared biological axis linking metabolic dysfunction to tumor behavior. Analyses of single-cell tumor data revealed a specific immune cell population within the tumor microenvironment where these pathways were particularly active, and subsequent laboratory validation in human tissue confirmed that several of these genes were more active in obesity‑associated contexts.
The article, “Linking Targeted Pancreatic Cancer Genes With Metabolic Disorders: A Cross‑Species Translational Pathway,” is published in Cancer Medicine. The research involved experts supported by the National Institute for Health and Care Research (NIHR) Biomedical Research Center: Birmingham. According to the authors, delineating common inflammatory programs may help explain poorer outcomes among patients with metabolic disease and signal opportunities to identify high‑risk individuals and refine treatment selection.
“We know that people with obesity or diabetes tend to have worse outcomes from pancreatic cancer, but the biological reasons have not been clear. Our study shows that the same genes and inflammatory pathways are active in both metabolic disease and pancreatic cancer, which helps explain this link and points to new opportunities for identifying high‑risk patients and developing more targeted treatments,” said Animesh Acharjee, Associate Professor of Integrative Analytics and AI at the University of Birmingham and senior author of the study.
“This study highlights how chronic inflammation and metabolic dysfunction can intersect with cancer biology. Understanding these shared mechanisms is essential if we are to improve outcomes for patients who are living with multiple long‑term conditions alongside cancer,” stated Simon Jones, Professor of Musculoskeletal Aging at the University of Birmingham and Theme Lead for the NIHR Biomedical Research Center: Birmingham Sarcopenia and Multimorbidity research theme.
Related Links
University of Birmingham